Thomas Kopec, PhD, LAT, ATC
Zimmer Biomet Institute, Warsaw, IN, USA.Background
Self-myofascial release has been demonstrated to increase relaxation and improve blood flow, yet it is unknown if it can elicit an acute effect on heart rate variability (HRV).
Purpose
This study aimed to determine if a single-bout of foam rolling could increase parasympathetic activity as measured by HRV.
Methods
Twenty (20) participants volunteered and their baseline HRV was assessed using a finger sensor while lying supine, and then a second measure was recorded with them sitting upright with feet on the ground. This study utilized a practical HRV collection method designed for use in the field settings, and the data is recorded in arbitrary units (A.U.). Participants then oscillated on a closed-cell cylindrical foam roller using their body weight on the triceps surae, hamstrings, quadriceps, lumbar spine, and pectoral muscles each for 60 sec. Participants first massaged the right limb and then repeated on the matching muscle group on the left before continuing to the next region. Follow-up HRV measurements were recorded using the same procedures.
Results
Paired samples t tests assessing pre- and post-foam–rolling HRV measures in supine and seated positions revealed no difference between supine measures (p = .05, d = 0.21), nor the seated measures (p = .27, d = 0.17) among all participants. When sexes were analyzed separately, males showed a significant decrease in HRV in supine positions (p = .03, d = 0.33), but females did not (p = .55, d = 0.09).
Conclusions
The single bout of foam rolling on large muscle groups did not increase parasympathetic activity as hypothesized. Males and females responded differently in supine positions, but no difference was present in seated positions across sexes. The task of self-massage may have prevented the anticipated response from the massage. Further research should investigate if passive massage is more effective on HRV response.
KEYWORDS: foam rolling, heart rate variability, parasympathetic withdrawal
Self-myofascial release (SMR) is a common technique utilized in clinical and field settings for both preparatory and recovery purposes.(1–3) Frequently, SMR is performed via the use of a foam roller (FR), which is a closed-cell dense-foam cylindrical tube that can be oscillated over a target area to relieve spasm,(4) reduce soreness following exercise,(5,6) and increase blood flow.(7) Although evidence for the effectiveness of FR immediately prior to exercise to improve performance is conflicted,(8,9) there is no evidence for FR impeding performance. Therefore, FR may be utilized without fear of decreased performance(10)while still positively affecting blood flow and tissue temperature.(11)
This application is unique from traditional massage because users are able to determine how much of their body weight to apply to a particular area, and can vary that force at will throughout the session.(9) Though FR has been demonstrated to aid in reducing muscle spasm and increase local blood flow, the acute effects on autonomic nervous signaling remains understudied. Recently Lastova et al.(12) demonstrated that a certain FR protocol was effective at decreasing sympathetic influence 10 and 30 min after completion of the protocol. However, their study utilized a traditional 2-lead ECG, which is not a practical method for assessing heart rate variability (HRV) in the field setting. Heart rate variability is a measure of the differences between each heartbeat and the R-waves as visualized on an ECG. More discrepancy between the R-R intervals indicates a greater parasympathetic response, and therefore a higher HRV value. Currently, there have been no valid field assessment tools for measuring HRV. Thus, the immediate effects of an acute bout of FR on HRV remain unclear.
Massage is another technique for treating myofascial pathologies and can also improve cardiovascular performance.(13) The mechanical pushing of blood proximally towards the heart creates a greater parasympathetic neural influence by improving cardiac preload and, therefore, increasing end-diastolic volume, ultimately reducing peripheral blood pooling.(14) Increasing preload and end-diastolic volume has been demonstrated to likewise increase HRV.(14) There are numerous methods for analyzing HRV,(15–19) but one of the most practical and appropriate for field-settings uses the ithlete™ smartphone application with Finger Sensor™.(15,19) This app detects the heart rhythm and can provide an output within 55 sec, utilizing a particular metric of assessing HRV called root mean square of successive RR interval differences (RMSSD) which is a time domain and is not as susceptible to breathing discrepancies as other HRV metrics. Furthermore, the software performs a natural log transformation to the raw value, as well as adds 20 to the output to transform the data into a more intuitive range. This practical method for evaluating HRV is highly applicable to the field setting where time is precious and technical expertise is unnecessary.(15–18,20–22)
In a recent study, Okamoto et al.(7) described how an acute bout of SMR with a FR could decrease arterial stiffness. The increased arterial pliability improved blood flow and consequently improved cardiac preloading and vagal tone. The use of FR to improve blood flow has been proposed(11) and questioned(9,23) in previous literature, yet any effects on HRV are still not understood, most especially immediately after treatment. Increasing parasympathetic influence via SMR and massage may increase venous return, indicating that FR could be a viable method for improving HRV, as HRV is an indicator of overall cardiovascular health. Furthermore, using a finger sensor to detect changes in HRV is an applied technique for quickly determining how FR may affect HRV immediately following treatment and was designed to be used by health-care practitioners in their work settings. Therefore, the purpose of the present study was to investigate the acute effects of a bout of full-body SMR with a FR on HRV in two-positions. It was hypothesized that HRV would improve in both supine and seated positions following a bout of FR as the affected musculature relaxed, arterial stiffness decreased, and venous blood flow to the heart increased. Moreover, it was hypothesized that male and female participants would respond similarly.
An a priori power analysis was used to determine adequate sample size using G-power 3.1.9.6 software (available from: https://www.psychologie.hhu.de/arbeitsgruppen/allgemeine-psychologie-und-arbeitspsychologie/gpower), with parameters analogous to other HRV studies.(15,24) The pre/post study design utilized paired samples t test: d = 0.6, α = 0.05, β = 0.8. Minimum sample size was calculated to be n = 19.
The present study utilized a quasi-experimental, pre/post study design to investigate whether a single-bout of full-body foam rolling could improve parasympathetic neural activity as assessed via HRV. College-aged males and females who participated in at least 150 min of moderate physical activity were recruited to perform a session of whole-body foam rolling. In order to qualify, interested participants were required to be free from upper- or lower-extremity injuries for at least three months. Participants’ HRV was assessed in both supine and seated positions using a validated ultra-short-term technique, then with the closed-cell foam roller systematically massaged their right and then left: calves; hamstrings; quadriceps; lower back; and pectorals for 30 sec each before proceeding to the next segment. Upon completion of the foam-rolling protocol, participants were again assessed for HRV in supine and then seated positions using the ultra-short-term HRV finger sensor and proprietary software. All data were collected in a single session.
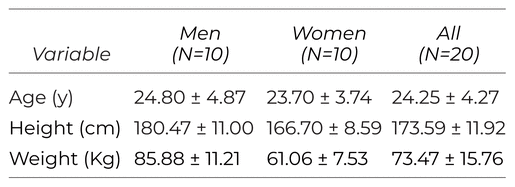
All participants reported to the laboratory to review the informed consent paperwork and consent was obtained from all participants. Additionally, all participants affirmed they met the inclusion criteria. Descriptive statistics on the participants is provided in Table 1. This study recruited physically active populations who exercise at a moderate intensity for at least 150 min per week. Those who were interested in participating proceeded to complete a familiarization trial. Next, they reported back to the lab at least 24 hours later for data collection. Using a pre/post study design, participants first laid supine as the clinicians assessed their HRV using the ithlete™ smartphone application and finger sensor, and then the test was repeated with participants in a seated position. HRV data are reported without units, as the present technique in this study utilized root-mean-square of standard deviations (RMS SD) with a natural log transformation (lnRMSSD), which puts the values on a more easily interpretable range.(18,15)
Table 1 Descriptive Statistics of Participants

Next, participants completed the foam-rolling protocol, requiring them to roll major muscle groups in the lower extremity, low back, and chest. Finally, participants repeated the HRV measurements in both supine and seated positions, respectively. All experimental procedures were conducted in accordance with the Declaration of Helsinki and approved by the university’s Institutional Review Board.
The pre-foam–rolling HRV (pre-HRV) measures were obtained using the ithlete™ Finger Sensor™, with the right index finger in a finger sensor connected to an electronic tablet and participants positioned supine.(15,21,25) The ithlete™ application collects HRV data in 55 sec and requires participants to follow on-screen prompts to inhale and exhale in rhythm.(15,18,21,25) Once the participants’ heart rhythm has stabilized, the application indicates it is ready and the clinician may begin the data collection. Although the HRV metric utilized by the app is not dependent on respiratory influence, breathing prompts appear on the screen to minimize any deviations in autonomic functioning. This software has been demonstrated to be reliable and valid when compared to ECG (correlation was near perfect at r = 0.99, p < .001, standard error of estimate 1.47, and Bland-Altman plot range 2.57 below to 2.63 above the constant error of −0.03.(21) Following the supine positioning, participants were next placed in a seated position and repeated the ithlete™ with hands resting on their laps.
After pre-HRV data were collected, participants were instructed on the proper form for using the high-density foam roller on the target tissues: triceps surae, hamstrings, quadriceps, lumbar spine, and pectoral group, respectfully. Participants first treated their right side for 60 sec, and then the accompanying left side (where applicable) before moving to the next body segment. The number of oscillations performed at each muscle during the 60-sec treatment was recorded for analysis, but was not prescribed. Following the treatment of the left pectoral group, participants were then immediately placed in a supine position and repeated the procedures for both supine and then seated HRV assessment using the finger sensor (post-HRV).
All results are reported as mean ± standard deviation. A pre/post t test was used to analyze the differences between pre-HRV values and post-HRV values. Furthermore, t tests were also utilized to determine the difference in HRV between sexes, as well as the difference in the number of total oscillations performed. Significance for all analyses was set a priori at p < .05. Effect sizes were calculated using Cohen’s d,(26) where values < 0.2 were considered trivial, 0.2–0.6 were small, 0.6–1.2 were moderate, 1.2–2.0 were large, and > 2.0 were very large.(27) All statistical analyses were performed using IBM® SPSS® statistics software (Version 21.0, IBM Corporation, Armonk, NY ).
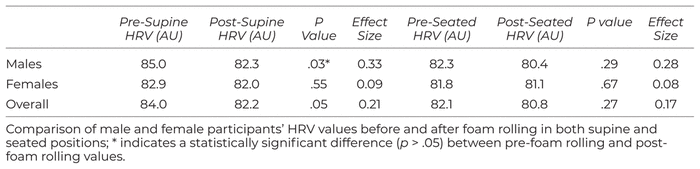
All subjects affirmed they accumulated at least 150 min of physical activity every week for at least three months. There were statistically significant differences in the number of oscillations participants performed at the hamstrings (p > .001, d = 0.20) and pectorals (p = .03, d = 0.11), though the effect sizes are trivial as the average difference of oscillations is less than one from right and left sides, as presented in Table 2. The results for HRV measurements are presented in Table 3. There were no significant differences among the pre-HRV and post-HRV trials in supine (p = .05, d = 0.21) and seated positions among all participants (p = .27, d = 0.17). However, when sexes were assessed separately, males had a significant drop in HRV in supine positions (p = .03, d = 0.33), but females did not (p = .55, d = 0.09). There were no differences in HRV in seated positions for males or females (p = .29, d = 0.28 and p = .67, d = 0.08, respectively). Additionally, when evaluating the total number of oscillations performed, males (128)completed significantly less repetitions than the female (161) participants(p = .03, d = −1.19) (see Figure 1).
Table 2 Aggregate Number of Foam Rolling Oscillations by Body Part across All Participants
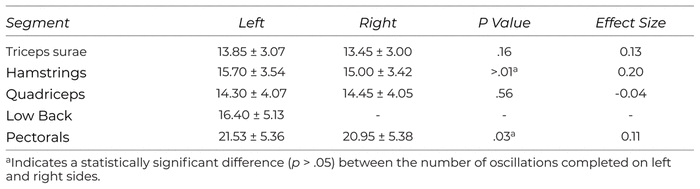
Table 3 Results on HRV and Body Position (recorded in arbitrary units [AU]).
|
| ||
|
Figure 1 Total oscillations on the foam roller by sexa.
| ||
The purpose of this study was to determine the influence of FR on HRV by using a practical assessment tool. There were no significant differences between HRV pre- and post-FR session. These findings indicate that HRV values were not greatly affected immediately following a full-body FR session. The present study rejected the hypothesis that acute follow-up of HRV would be improved immediately following an acute bout of foam rolling. Regardless of supine or seated positions for HRV assessment, no significant differences were found among all participants. There was a significant difference in males when assessing HRV in a supine position; however, these data are novel and need to be repeated in more studies before conclusive interpretations are made, as the difference dissipated when moving the body positions to seated.
Foam rolling has been repeatedly demonstrated to be effective for increasing flexibility,(5) reducing soreness,(3) and improving muscle recovery,(8) and improving localized blood flow,(11) all without negatively impacting physical performance,(10) yet very few studies have investigated the effects of FR on autonomic functioning.(12) Though this is a novel area of research, the present study was unable to wholly support the use of FR to affect HRV response. In a related study by Okamoto et al.,(7) FR was effective for reducing arterial stiffness and increasing plasma nitric oxide concentrations. These physiological responses are related to sympathetic withdrawal and increased vagal tone,(28) and therefore it was theorized that the muscle relaxation following myofascial release would reduce arterial stiffness, increase plasma NO concentration, release tension in the treated myofascia, and ultimately improve parasympathetic output. The present study did not evaluate arterial stiffness, nor examine blood concentration compositions, as the goal was to evaluate a practical method for clinicians to use in the field. It may be that the FR protocol in the present study was inadequate for eliciting increased parasympathetic activity.
These findings conflict with recent studies that found FR to be impactful for improving HRV by increasing the parasympathetic output. In the Lastova et al. study, HRV was significantly increased between 10 and 30 min after FR treatment, though no acute effects were reported.(12) Delaney et al.(13) demonstrated an increase in parasympathetic activity at 5-min follow-up after a session of myofascial trigger-point massage, demonstrating a clear acute effect. It is proposed that the current FR protocol was ineffective for initiating an acute parasympathetic response, and it is unknown if the protocol was effective for causing a change by 10 or 30 min after treatment as the present study only collected HRV data immediately following completion of the FR protocol. The significant difference seen in males in the supine position from this current study indicate there may be a factor that was not considered in the present study design and warrants further investigation to determine if biological sex influences parasympathetic response to mechanical pressure via SMR.
The confounding results may be most easily explained as full-body FR being more metabolically demanding than originally theorized. Delaney et al.(13) reported acute changes in parasympathetic functioning; however, they utilized a protocol with a clinician performing myofascial trigger-point massage, where the participants were passive recipients of the treatment. Further, Lastova et al.(12) assessed HRV at 10- and 30-min follow-ups after the FR protocol, but did not assess HRV immediately post-FR protocol. Although the present study seems to fit in between these, the lack of significant findings indicates that immediate follow-up to self-myofascial release is not indicated for assessing parasympathetic response. It is possible, therefore, that a time delay of at least 10 min is appropriate for assessing parasympathetic response to self-myofascial release with a foam roller. These findings provide a greater depth to the scientific community’s understanding of massage techniques and acute autonomic responses.
Although seemingly innocuous and non-fatiguing, full-body FR appears to be more strenuous than originally believed. The FR oscillations technique involves periods of isometric holds, mixed with short bursts of muscle contractions, that may be shunting blood to the peripheral working tissues(29) and occluding capillary beds, and reducing the venous return, ultimately decreasing parasympathetic neural activity (and consequently increasing sympathetic activity). Massage has been demonstrated to improve venous return to the heart,(14) and encourage a return to parasympathetic neural dominance.(13) As a specific technique for myofascial release, FR compresses the superficial neurovascular vessels,(7) stimulating superficial A-β nerves to diminish noxious transmission.(30,31) This gate-control mechanism(30,31) effectively blocks pain stimulus from reaching the CNS and can, therefore, have the secondary effect of improving relaxation and decreasing pain sensitivity in the targeted areas. It was theorized in the present study that the relaxation of the large muscle groups that were treated, in combination with the vessel compression from the participants’ body weight, would further improve vagal tone as blood in the periphery would be directed back towards the heart.(7,32) Further investigations are needed to determine the threshold for muscle relaxation, decreased vessel rigidity, and parasympathetic neural activity.
A final consideration for the findings in the present study was the utilization of a clinician-friendly assessment tool using a smartphone and finger sensor, whereas previous studies have utilized traditional ECG-techniques.(12) This non-invasive and clinician-friendly HRV assessment technique has been previously validated against traditional ECG (r = 0.99, p < .001)(21,25) and so can be considered acceptable for determining HRV. Therefore, it is unlikely that the equipment bears any substantial influence on the measured outcomes, and more likely the protocol and timing of assessment are responsible for the lack of significant findings.
There are multiple limitations to note in the present study. Firstly, the participant population came from a moderately homogenous population, as a convenience sample was taken from the host institution. The inclusion and exclusion criteria help to offset this bias, however, as participants were required to maintain a minimum level of physical activity while also being free from major orthopedic injury in the immediate preceding three months. Additionally, the direct role that sex has on autonomic functioning, as measured via HRV, has not been well-established. Previous research has favored using only the same sex for participants or standardizing when female participants begin the data collection based on their status in the menstrual cycle. It should be noted that the phase of menstrual cycles for the female participants in this study were not considered, as a clear link in discrepancy for HRV in men and women has not been established. Furthermore, limiting female participation to only a specific timing window in their cycle limits the external validity of the study, as females will utilize self-myofascial release treatments regardless of their menstrual cycle phase. A final limitation for this study may have been the FR protocol. There are currently no published standardized FR protocols for a given therapeutic outcome, and so researchers should be thoughtful when selecting a protocol that is appropriate for their anticipated therapeutic goal. This study utilized a protocol that allowed participants to oscillate at a comfortable rhythm, and the differences in the number of oscillations between left and right triceps surae and quadriceps were not statistically significant (p = .163 and p = .562, respectively); yet hamstrings and pectorals were both statistically significant (p < .001, d = 0.20 and p = .033, d = 0.11, respectively). However, the number of oscillations was practically insignificant (right-to-left triceps surae 13.45 to 13.85; right-to-left hamstrings 15.00 to 15.70; right-to-left quadriceps 14.45 to 14.30; right-to-left pectorals 20.95 to 21.53), as there was less than one-oscillation difference between right and left sides where a difference existed, and the effect sizes reflect that interpretation as both were “trivial”.(27) Though the present protocol was selected because it targeted numerous large muscle groups, it was not effective in eliciting an immediate change in HRV. Also, oscillations were utilized to avoid blood pooling caused by isometric holds, as the goal was to initiate effects comparable to myofascial release massage; though the lack of significant findings may indicate the use of isometric holds to imitate pressure release therapy. The effects of oscillations versus isometric holds have not been established, and therefore researchers and clinicians need to be aware of this dearth in foam-rolling application prescription. Future research should consider taking follow-up HRV assessments in small time increments while extending the follow-up until at least 30 min after treatment. Moreover, future research may benefit from altering the FR technique they employ to discern which protocol is most effective.
The present findings indicate that a single bout of FR is not effective at eliciting an acute change in parasympathetic activity. The results from the present study failed to initiate an immediate parasympathetic physiological response overall with all participants, despite other reported benefits of FR following a single bout of full-body FR. Clinicians should be aware that, although FR has been established to be safe and beneficial for a myriad of applications, it may not be appropriate for altering autonomic cardiovascular influence.
I would like to acknowledge Rebecca Rogers for her help in the data collection process and thank all who volunteered for this study. This project was partially funded by an internal “Faculty Development Grant” from the Faculty Committee on Academic Affairs by Samford University.
The author declares there are no conflicts of interest.
1 Weerapong P, Hume P, Kolt G. The mechanisms of massage and effects on performance, muscle recovery and injury prevention. Sports Med. 2005;35(3):235–256.

2 Cheatham SW, Kolber MJ, Cain M, Lee M. The effects of self-myofascial release using a foam roll or roller massage on joint range of motion, muscle recovery, and performance: a systematic review. Int J Sports Phys Ther. 2015;10(6):827–838.

3 Pearcey G, Bradbury-Squires D, Kawamoto J-E, Drinkwater E, Behm D, Button D. Foam rolling for delayed-onset muscle soreness and recovery of dynamic performance measures. J Athl Train. 2015;50(1):5–13.


4 Romero-Moraleda B, González-García J, Cuéllar-Rayo Á, Balsalobre-Fernández C, Muñoz-García D, Morencos-Martinez E. Effects of vibration and non-vibration foam rolling on recovery after exercise with induced muscle damage. J Sports Sci Med. 2019;18(1):172–180.

5 Madoni S, Costa P, Coburn J, Galpin A. Effects of foam rolling on range of motion, peak torque, muscle activation, and the hamstrings-to-quadriceps strength ratios. J Strength Cond Res. 2018;32(7):1821–1830.

6 Macdonald G, Button D, Drinkwater E, Behm D. Foam rolling as a recovery tool after an intense bout of physical activity. Med Sci Sports Exerc. 2014;46(1):131–142.

7 Okamoto T, Masuhara M, Ikuta K. Acute effects of self-myofascial release using a foam roller on arterial function. J Strength Cond Res. Jan 2014;28(1):69–73.

8 Peacock C, Krein D, Silver T, Sanders G, von Carlowitz K. An acute bout of self-myofascial release in the form of foam rolling improves performance testing. Int J Exerc Sci. 2014;7(3):202.
9 Wiewelhove T, Döweling A, Schneider C, Hottenrott L, Meyer T, Kellmann M, et al. A meta-analysis of the effects of foam rolling on performance and recovery. Front Physiol. 2019;10:376.


10 Kopec T, Bishop P, Esco M. Influence of dynamic stretching and foam rolling on vertical jump. Athl Train Sports Health Care. 2017;9(1):33–38.

11 Healey K, Hatfield D, Blanpied P, Dorfman L, Riebe D. The effects of myofascial release with foam rolling on performance. J Strength Cond Res. 2014;28(1):61–68.

12 Lastova K, Nordvall M, Walters-Edwards M, Allnutt A, Wong A. Cardiac autonomic and blood pressure responses to an acute foam rolling session. J Strength Cond Res. Oct 2018;32(10):2825–2830.

13 Delaney JP, Leong KS, Watkins A, Brodie D. The short-term effects of myofascial trigger point massage therapy on cardiac autonomic tone in healthy subjects. J Adv Nurs. 2002;37(4):364–371.

14 Mori H, Saito I, Eguchi E, Maruyama K, Kato T, Tanigawa T. Heart rate variability and blood pressure among Japanese men and women: a community-based cross-sectional study. Hypertens Res. 2014;37(8):779–784.

15 Nakamura FY, Flatt AA, Pereira LA, Ramirez-Campillo R, Loturco I, Esco MR. Ultra-short-term heart rate variability is sensitive to training effects in team sports players. J Sports Sci Med. 2015;14(3):602–605.

16 Flatt AA, Esco MR. Smartphone-derived heart-rate variability and training load in a women’s soccer team. Int J Sports Physiol Perform. 2015;10(8): 994–1000.

17 Flatt AA, Esco MR. Heart rate variability stabilization in athletes: towards more convenient data acquisition. Clin Physiol Func Imag. 2016;36(5):331–336.

18 Esco MR, Flatt AA. Ultra-short-term heart rate variability indexes at rest and post-exercise in athletes: evaluating the agreement with accepted recommendations. J Sports Sci Med. 2014;13(3):535–541.

19 Boos CJ, Bakker-Dyos J, Watchorn J, Woods DR, O’Hara JP, Macconnachie L, et al. A comparison of two methods of heart rate variability assessment at high altitude. Clin Physiol Funct Imaging. 2017;37(6):582–587.

20 Esco MR, Flatt AA, Nakamura FY. Initial weekly HRV response is related to the prospective change in VO2max in female soccer players. Int J Sports Med. 2016;37(6):436–441.

21 Flatt AA, Esco MR. Validity of the ithlete(TM) smartphone application for determining ultra-short term heart rate variability. J Hum Kinet. 2013;39: 85–92.

22 Flatt AA, Esco MR, Nakamura FY. Association between subjective indicators of recovery status and heart rate variability among divison-1 sprint-swimmers. Sports. 2018;6(3):93.


23 Jo E, Juache GA, Saralegui DE, Weng D, Falatoonzadeh S. The acute effects of foam rolling on fatigue-related impairments of muscular performance. Sports. 2018;6(4):112.


24 Williams TD, Esco MR, Fedewa MV, Bishop PA. Inter- and intra-day comparisons of smartphone-derived heart rate variability across resistance training overload and taper microcycles. Int J Environ Res Public Health. 2021;18(1):177.


25 Sagarra-Romero L, Peña MR, Antón AM, Morales SC. ithlete Heart Rate Variability app: knowing when to train. Br J Sports Med. 2017;51(18): 1373–1374.

26 Cohen J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed. Mahwah, NJ: Lawrence Erlbaum; 1988.
27 Hopkins WG, Marshall SW, Batterham AM, Hanin J. Progressive statistics for studies in sports medicine and exercise science. Med Sci Sports Exercise. 2009;41(1):3–13.

28 Kalra P, Yeragani VK, Kumar KP. Cardiac autonomic function and vascular profile in subclinical hypothyroidism: Increased beat-to-beat QT variability. Indian J Endocrinol Metab. 2016;20(5):605–611.


29 Drew RC, Bell MP, White MJ. Modulation of spontaneous baroreflex control of heart rate and indexes of vagal tone by passive calf muscle stretch during graded metaboreflex activation in humans. J Appl Physiol. 2008;104(3):716–723.

30 Melzack R, Wall PD. Pain mechanisms: a new theory. Science. 1965;150(3699):971–979.

31 Handwerker HO. Pain and allodynia, itch and alloknesis: an alternative hypothesis [Commentary]. APS J. 1992;1(2):135–138.

32 Ramalho ES, Souza-Junior EL, Magnani M, Braga VA. Gender differences in heart rate variability among individuals undergoing regular resistance training preliminary observations. Sultan Qaboos Univ Med J. 2017;5(2):e209–e212.

Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 15, NUMBER 4, DECEMBER 2022