

Joel Begin, DPT, PT1*, Luiz Fernando Bertolucci, MD2, Dorothea Blostein, PhD3, Budiman Minasny, PhD4
1Creative Pathways Physical Therapy, Henniker, New Hampshire, USA
2Associação Brasileira de Rolfing, São Paulo, Brazil
3School of Computing, Queen’s University, Kingston, ON, Canada
4School of Life and Environmental Sciences, The University of Sydney, New South Wales, Australia
Our aim is to describe a possible class of nonpathological spontaneous movements that has so far received little attention in the scientific literature. These movements arise spontaneously without an underlying pathology such as Huntington’s, Parkinson’s, cerebral palsy or spinal cord injury. The movements arise in many different contexts including therapeutic, social, religious, and solitary settings. Anecdotal evidence suggests that the movements are related to development and maintenance of form, being part of inherited autoregulatory behaviors and hence bringing an overlooked therapeutic potential. We describe contexts in which they occur, illustrate with case reports, and characterize the movements in terms of their various triggers, movement phenotypes, and conscious and subconscious influences that can occur at both the individual level as well as during collaborative movement relationships between patient and therapist. This description is intended to create a more widespread awareness of the movements, and provide a foundation for future research as to their healing potential.
KEYWORDS: myofascial unwinding, spontaneous movement, beneceptive movement, myofascial induction, tensegrity, subconscious movement, ideomotor action
In this paper we describe a broad class of spontaneous movements that arise in many settings, including manual and movement therapy settings. The movements are nonpathological, meaning that there is no underlying pathology such as Huntington’s, Parkinson’s, cerebral palsy or spinal cord injury. Extensive anecdotal evidence leads us to hypothesize that the inherent movements are health promoting and beneficial. Despite being widespread, this class of spontaneous movements has so far received little attention in the scientific literature. Our goal in describing this phenomenon is to provide a basis for scientific study, describing what occurs as a first step for future scientific investigation of the how and why it occurs. Even though we currently do not have a deep scientific understanding of the causes and mechanisms of these spontaneous movements, we can nevertheless describe strategies that manual and movement therapists have found effective in accessing their possible healing properties and also in assisting people who experience such movements.
Past studies have described spontaneous movements in specific manual therapeutic approaches, such as myofascial unwinding(1) and a form of myofascial release formerly called Muscle Repositioning(2) that enabled a tonic muscle response.(3) Bertolucci(4) proposed that these reflexes are akin to pandiculation, an instinctual soft-tissue stretching that helps maintain the functional integrity of the myofascial system. Others postulated that it is related to ideomotor action and subconscious movement.(1) Massmann(5) surveyed recipients’ experience of myofascial unwinding. Research studies found that the myofascial unwinding treatment improves pain perception over a short-term duration in people with nonspecific lower back pain,(6) decreases pain intensity, and improves neck–shoulder ROM in breast cancer survivors.(7) Blostein(8) hypothesized that these spontaneous movements relate to the maintenance of structural homeostasis.
Traditionally, morphogenetic movement refers to movement that occurs in an embryo and is necessary for normal embryonic development.(9) Perhaps it would be appropriate to use this phrase more broadly to describe spontaneous movements at any stage in life that appear to be related to the adaptation, development, and maintenance of form. However, choosing appropriate nomenclature is difficult at present because the mechanisms underlying these various classes of movements are, as yet, not well-understood. For now, we use the general term spontaneous movements to refer to the broad class of nonpathological movements under discussion.
This paper aims to describe spontaneous movements and their characteristics to help clinicians recognize and respond to this phenomenon. We first describe spontaneous movements that are recognized in manual and movement therapies, as well as in spiritual practices. We then present three types of case reports: self-experienced spontaneous movements, manual therapy induced spontaneous movements, and the use of a clinician’s spontaneous movement experience as a foundation for helping patients who have dyskinesia. Finally, we discuss commonalities of the spontaneous movements and suggest future research directions.
Spontaneous movements arise in a wide variety of manual therapies, movement therapies, and spiritual practices. We summarize these movements based on what we encountered in the literature and anecdotally in Table 1, with video documentation in Appendix A. Criterion for the list in Table 1 is that a person experiencing spontaneous movements does not have the sense of agency that normally accompanies the experience of initiating and controlling action. Braun et al.(10) review experimental paradigms, results, and neurocognitive theories about the senses of agency and ownership. Here we do not include subtle movements induced or occurring in modalities such as osteopathy, cranial therapy, or visceral manipulation.
Table 1 Examples of Contexts in Which Spontaneous Movements Occur


As is clear from Table 1 and the following case reports, spontaneous movements are a phenomenon that has a wide variety of expressions. Sometimes the movements are familiar to the person (e.g., a familiar arm or leg movement, or a yoga asana), but in other situations, the person experiences the movements as new and unfamiliar. Anecdotal evidence suggests that this class of movements can be labeled as normal and health-promoting.
The communities summarized in Table 1 each have their own intuitive explanation of why the spontaneous movements occur. It seems likely that all of them are dealing with the same phenomenon, or variations of the same phenomenon. All four authors have experienced spontaneous movements themselves, and two (JB and LFB) have frequently observed patients’ spontaneous movements in their manual therapy practices.
Spontaneous movements are illustrated in the following case reports. Even though the experiences in these case reports are quite varied, some commonalities are evident and will be discussed.
We present three groups of case reports: self-described case reports where spontaneous movements occur over an extended period, a case report drawn from Tensegrity Touch manual therapy practice, and case reports for treating dyskinesia using movement collaboration. All subjects in the case reports provided informed consent, signing the form shown in Appendix B. For the Huntington’s case report, the mother of the subject signed on behalf of the deceased subject.
The subjects in the case reports were chosen informally, rather than through a formal recruitment and selection process. For the first group of case reports, we began by contacting the five people we happened to know who experienced vigorous spontaneous movements over an extended time period. These five subjects met us fortuitously. Three of them contacted us via email after finding BM’s publication(1) while searching the internet in an effort to learn more about their unusual and poorly-understood movements. We learned of the other two subjects through informal discussions with therapeutic bodyworkers. Of these five subjects, one was no longer reachable due to outdated contact information and another one did not wish to participate; the remaining three subjects are included in the first group of case reports. For the second group of case reports, LFB chose one representative case from a pool of approximately 50 clients who developed spontaneous movements during a Tensegrity Touch manual therapy session. For the third group of case reports, JB chose one representative case from a pool of approximately 30 clients with dyskinesia that he treated with movement collaboration.
We begin with three case reports of subjects experiencing vigorous spontaneous movements over an extended period of time. We interviewed these subjects in early June 2021, asking them to describe their experience to us by providing a brief health history, a description of how the movements started, and a summary of strategies they have found for dealing with the movements. To address a reviewer’s request for further information regarding aspects of these case reports, we asked the subject follow-up questions in April 2022 via email and zoom.
A 52-year-old man has been experiencing intensive spontaneous movements for almost two years. At nine years old, he had spinal surgery to fuse L4, L5, and S1 because of a congenital structural deformity. He has always been athletic and active; he was a competitive swimmer up to the national level. Throughout his swimming career, he favored breathing on his left side, which often led to tendonitis and other ailments. He smoked for about 30 years. As a teenager and young adult, he had severe back pain whenever he bent over. Eventually, the pain in his lower back became chronic. In his mid-forties, the chronic pain reached debilitating levels and he received pain killers from his doctor. In journaling his pain on a scale of 1 to 10, he recalls a period of 30 consecutive days when his pain level was 10.
His spontaneous movements started almost two years ago, following surgery on his left shoulder due to a fall. Starting roughly eight weeks after that surgery, he has been experiencing spontaneous movements daily. The first movements emanated from his left scapula at an incision point for the shoulder surgery. The area around that incision point started twitching, and the twitching began radiating out. The spontaneous movements are vehement and intensive. He feels movements start at a point of injury and spiral out from there. The spiraling is rapid and can go on for up to 2 min. He can see the tissue vibrating under his skin; sometimes he feels a burn sensation under his skin from the friction. He spontaneously moves in a fluid and undulating manner, almost like a yawning-type movement, trying to alleviate the pain by stretching it out.
The movements are changing over time, and they continue to feel painful. Six months to a year ago, the movements felt superficial. Now they are more penetrating, and he gets a sensation of burning threads that he feels might be collagen filaments. The movements are relentless, they never stop. At times he feels intense unwinding sensations around his SI joint that feel like flowing liquid exiting the joint in a circular motion.
Despite the pain associated with the spontaneous movements, he believes that they are allowing him to slowly heal. There has been a significant reduction in the pain in his back and SI joints. He notices changes in his body structure. A hugely enlarged disc in his lower back has decreased in size. Also, his quadratus lumborum unseized and his lower back stretched out, allowing his back dimples to become visible again. Sometimes he has amazing and intense feelings of his strength coming back in response to the movements. And he has changed from being quite inflexible to having good flexibility.
He has had some positive results from combining spontaneous movements with manual therapy. He guides his therapist where to put pressure and where to pull away, then the spontaneous movements do their own thing. He has become quite sensitive to touch, with even light touches triggering spontaneous movements. As a result, he doesn’t always like to be touched and instead seeks out quiet environments. He once had to stop an acupuncture session because the needles triggered an overactive response, causing intense rippling sensations all over his body.
The psychological aspects of the movements are difficult. The incessant nature of the movements makes him feel helpless and wears him down. He gets through this by remaining optimistic, one day at a time, and reminding himself of his progress in the form of physical improvements and pain reduction.
A 36-year-old man started experiencing spontaneous movements in early May 2019, a few weeks after receiving nasal surgery. Initially, his spontaneous movements mainly took the form of twitching, with all parts of his body involved. Since then, he has had daily hours-long sessions of spontaneous movements, with many different movement phenotypes. He suffered chronic pain in childhood, as a teenager and as an adult—with bowel pains, neck cramps, constant nasal congestion, and pain on exercising. He also had movement limitations, was bowlegged, could not bend over properly, and could not stand straight. Since no medical cause for his pain could be found, his complaints tended to be ignored. He tried various treatments, such as physiotherapy and exercise, but nothing could relieve his pain.
The movements started after he became increasingly aware that he could not stand up straight, and tried to envision standing like the male figure in da Vinci’s Vitruvian Man. The effort to stand up straight allowed him to perceive increased tension throughout his entire body. He experienced the sensation of what felt like “strings” moving in areas of his neck, back of neck, shoulders, and elsewhere. This was followed by audible pops, cracks, and “things letting go”. He had no idea what to make of these movements and was quite confused and a bit alarmed by them. Later, he discovered the article by Minasny(1) and learned that he wasn’t alone in having these movements, and that the movements have the potential to be health-promoting. He made a conscious choice to explore and discover the spontaneous movements, to allow and encourage them to happen. Because of COVID-19 lockdowns, he was able to work from home, and at that time, his spontaneous movements greatly increased in intensity and duration.
For the past year, he has been spending all free time on the spontaneous movements—often as much as four to five hours a day. He observes the movements, explores new movements, and facilitates the movements by nudging the process along when it gets stuck. He feels that the movements occur at some level all the time, but he can control the movements when he has other tasks to pursue. While the movements are sometimes quite intense and even a bit painful, he has never perceived them as threatening; rather, he experiences them as natural movements that allow his body to heal. He reports that the movements provide him with a feeling of coming to completion and bring him to a greater state of rest.
He has experienced many mental and physical benefits from spontaneous movements. While he continues to experience chronic pain, the pain is less intense and has become more manageable. He no longer feels as tense and clenched, and has had improvements with his cognition, stuttering, tinnitus, peripheral vision, flexibility, strength, and coordination. He feels his body shape is becoming less twisted and more symmetric. He notices changes in his face and neck that make it possible to smile without forcing it, and he feels much better neck mobility. For the first time in his life he is able to do movements like touching his toes and putting his hand behind his back.
A 47-year-old man has been experiencing spontaneous movements for ten years, two to three times per week on average. In infancy, childhood and adulthood, he suffered numerous accidental head impacts, with varying degrees of concussion. For many years he was able to recover from the concussions but, six years ago, started showing fairly severe symptoms from the cumulative head traumas. MRIs show that he has significant scar tissue in his suboccipital area and a void in the cerebellum.
His spontaneous movements started when he was in a massage school, receiving structural integration work from an instructor trained as a Rolfer. The instructor was doing pelvic work targeted at the psoas muscle and this triggered a strong reaction. His legs started shaking and this expanded to his whole body shaking. This response lasted more than 15 min and was disconcerting for the instructor. The subject felt afraid at first and then experienced an emotional release. This was his first adult experience with spontaneous movements; it triggered a memory of a similar leg shaking he experienced as a child, with his mother responding by holding his legs down.
At first, the spontaneous movements arose only when he was on the table receiving bodywork, but eventually the movements became more frequent, occurring 1 to 2 times per week, without a bodywork trigger. He would shake in bed at night. In recent years, he has been experiencing spontaneous movements perhaps once or twice a week, increasing in frequency to 3 to 4 times a week in response to the stress and restrictions of the COVID-19 pandemic. Longer episodes typically last 10 to 15 min, with shorter ones only 5 to 7 min.
Given his history of traumatic brain injury, neurological tests were done. Two MRIs showed a void in the cerebellum that was first considered to be responsible for seizure activity. However, the neurologist observed that he was able to have a conscious conversation while having spontaneous movements. Because of this, the neurologist dismissed seizures as a reason for the symptoms, and follow-up work was not performed. Instead, he was referred to psychiatric or behavioral health.
The subject is able to carry out some voluntary movements when spontaneous movements are occurring. When he feels an episode starts, he positions himself for safety so that if he falls out of bed or off the sofa he will land on something soft. He has experienced powerful undulations in his spine that cause him to repeatedly hit his head, chest, and hip on the floor. When this starts to happen, he usually manages to pull a pillow or other soft object under his head to soften the impact when his head hits the floor. The movements often include incomprehensible vocalizations, yawning, shaking in the legs, and extension of fingers, wrists, and elbows.
He finds it difficult to stop the spontaneous movements voluntarily. If he does stop them in one part of his body, they will typically start up in a different part of his body. Stopping the movements does not feel good and often causes excruciating pain in his head.
The spontaneous movements sometimes feel health-promoting, especially when he is able to manage his environment and set himself up safely either by sitting or lying down. At other times the movements feel scary; for example, when powerful spine undulations cause him to hit his head on the ground. He found several forms of manual and movement therapy to be particularly helpful. One, a technique adapted from Jin Shin Jyutsu, is having someone treat his spine undulations by holding and oscillating his big toes. Another technique is self-applied soft-tissue work to his occipitals with his thumbs. A third technique is to apply vibratory stimulation to his abdominal region and then hum or sing to reduce the intensity of spontaneous movement. He also benefits greatly from working with a movement therapist specializing in head trauma. Together, they use TRX, balance board, and core balance equipment. The therapist provides guidance, feedback, safety, and support while allowing him to move instinctively and intuitively. This allows him to learn to better engage different parts of his body, resulting in better movement coordination.
Here we present a case report drawn from a manual therapy practice (LFB), where the patient develops spontaneous movements in response to an intervention provided by the therapist. The approach was initially called Muscle Repositioning(2,3,22) and is now called Tensegrity Touch. In this approach, a combination of manual forces evokes involuntary muscle activity as detected by EMG.(3)
A 69-year-old female patient had an accident causing acromioclavicular luxation in the left shoulder. She received surgery for reduction and stabilization, then underwent rehabilitation treatment with an improvement of ROM and pain level. Nonetheless, she still experienced dysesthesias: tying sensation over the shoulder and rigidity during movement. Additionally, she reported pain in the left forefoot in a region where Morton’s neuroma had been diagnosed prior to the accident.
The physical examination showed that the scapulothoracic rhythm was altered in the left shoulder, with the scapula being dragged early in the abduction of the left arm. Although ROM was normal, she experienced discomfort raising the arm, reporting a tying sensation at the end of the movement. When shifting weight between the legs, she reported pain in the left forefoot when leaning on the left leg.
She received a series of Tensegrity Touch sessions. The first manual approach was made on the left thoracic area, with the patient lying on her right side. After approximately 5 min of touch, she started to exhibit undulating movements of the torso and pandiculation-like movements of the left arm. Subsequently, the movements spread to other body segments in various patterns, mainly in the upper limbs and trunk. The most intense pattern was a full abduction and external rotation of the left shoulder.
At the end of the first session, the scapulothoracic rhythm was more symmetrical, the movement of the left arm was more fluid, and the discomfort had diminished significantly. The pain in the left foot had vanished and the weight-bearing sensation was more symmetric. The overall sensation was of lightness and well-being.
In subsequent sessions, there were progressively milder symptoms and improved findings in physical examination. The spontaneous movements arose more easily and intensively as the sessions progressed. She recognized that their “intention” was to release felt-tissue restrictions.
She reported that her posture had improved during this process, and that she felt less tired during the day (“I was surprised to realize I was sitting in a good and comfortable posture without effort”). She also reported that she could trigger the spontaneous movements by herself (“lying down and allowing them”), which she currently does whenever she feels the need, in a self-healing practice.
In our (LFB) practice we can observe very consistent therapeutic effects of the spontaneous movements, which seem to be amplified by the manual intervention. These include more fluidity and ease of movement, less mechanical pain, greater postural stability, and overall lightness and well being, suggesting an autoregulatory role of those movements.
Dyskinesia refers to involuntary movements arising from conditions such as Huntington’s, Parkinson’s, cerebral palsy or spinal cord injury.(23) Since medical treatment options cannot eliminate dyskinesia, any relief provided by manual therapy is helpful. The following case reports provide anecdotal evidence for a treatment approach that the therapist (JB) devised based on prior experience with his own nonpathological spontaneous movements.
The following case report illustrates an experimental treatment approach for Huntington’s disease in which a movement collaboration is established between therapist and patient, with the therapist providing rhythmic and responsive mechanical forces that serve to dampen the dyskinesia and provide a “mirror-like” experience to the patient.(24)
A 19-year-old woman with Huntington’s disease had been suffering from several years of vigorous and disorganized chorea, powerful enough to make it difficult for her to maintain her balance in standing. There was enormous energy expenditure; she consumed about 6000 calories per day while maintaining low body weight.
In this treatment approach, the therapist and patient join to cooperatively and responsively form a single prestressed system that incorporates the dyskinetic movements (on the part of the patient) and spontaneous movement responses (on the part of the therapist). During the first of three treatment sessions, the therapist and patient interlocked hands while standing. The therapist instructed her to “stay with me”, thus beginning a movement collaboration where both worked together to keep re-establishing an agreed-upon light, but perceivable, pre-stressed tension between their interlocked hands. Due to the unpredictable timing and direction of the patient’s dyskinesia movements, the therapist did not have time to select and apply any one specific treatment before having to reconfigure his own posture while simultaneously maintaining pre-stressed tension. Instead, following each dyskinesia episode, both responded instinctively in whatever way seemed appropriate to make progress toward restoring a constant pressure at the interlocked hands while also maintaining balance. Each postural reconfiguration was done quickly and intuitively using the therapist’s entire fascial system, in order to provide the powerful mechanical forces needed to help slow down or dampen the movements arising from the patient’s episodes of spontaneous chorea. Every time the patient had a few seconds of voluntary muscle control between bouts of chorea, regardless of what new or “abnormal” posture the patient or therapist was in, the patient was encouraged to move purposefully.
After 10 to 15 min of this work together, the patient’s chorea stopped for about half a minute. This was the first period of pause and stillness that she had experienced in several years. She reported increased appetite and improved sleep following this treatment. During two subsequent sessions, the therapist used a similar treatment approach to again help guide her to a point of stillness.
Before her illness, she had been an accomplished gymnast and she felt deep joy at being able to access and perform gymnastics motor patterns during chorea-free periods while interlocking hands with the therapist. The support and resultant dampening of forces by the therapist did not appear to hinder her ability to access these older motor patterns; rather, it appeared to offer her improved rhythmic control, coordination, and ease while accessing these motor patterns. Sadly, she passed away three years later due to the fast degeneration caused by this disease.
The application of similar methods by JB has yielded good results with other patients with dyskinesia. An elderly patient with Parkinson’s disease had continuous cog-wheel movement in the right arm, which the therapist was able to bring to a still point by holding the moving arm, joining in with the movement, and looking for opportunities to apply light amounts of mechanical forces in appropriate directions while respecting the rhythmic nature of the autonomous movement.
An Alzheimer’s patient who walked with difficulty and rigidity had treatment through movement collaboration (establishing constant light hand-to-hand pressure while standing) and afterward walked more fluidly, with less rigidity, increased stride, and greater voluntary control. A man with complete C7 spinal cord injury had extremely severe spasticity in his legs,(23) which the therapist was able to reduce by intuitively creating rhythmic movement patterns in whatever directions the spastic leg would allow. Similarly, spasticity was reduced for a woman with Restless Legs Syndrome, improving her ability to lift her foot and walk with ease.
Even though a patient’s spontaneous movements are clearly arising from a disease condition, it is possible for a manual therapist to incorporate appropriate intuitive responses, while using principles that would be used with an individual of nondisease status.
There are commonalities in the descriptions of spontaneous movements in the manual therapy, movement therapy, and spiritual settings summarized in Table 1, as well as in the case reports. Generally, spontaneous movements are seen as beneficial experiences with positive therapeutic effects.
We summarize common characteristics of the movements in Table 2. These characteristics are usually present, but individuals with spontaneous movements do not display all of these characteristics all of the time. The descriptions in Table 2 are based on many years of observation by the authors. We group the characteristics into triggering factors, types of movement, health-promoting, and subconscious and conscious influences.
Table 2 Characteristics of Nonpathological Spontaneous Movements
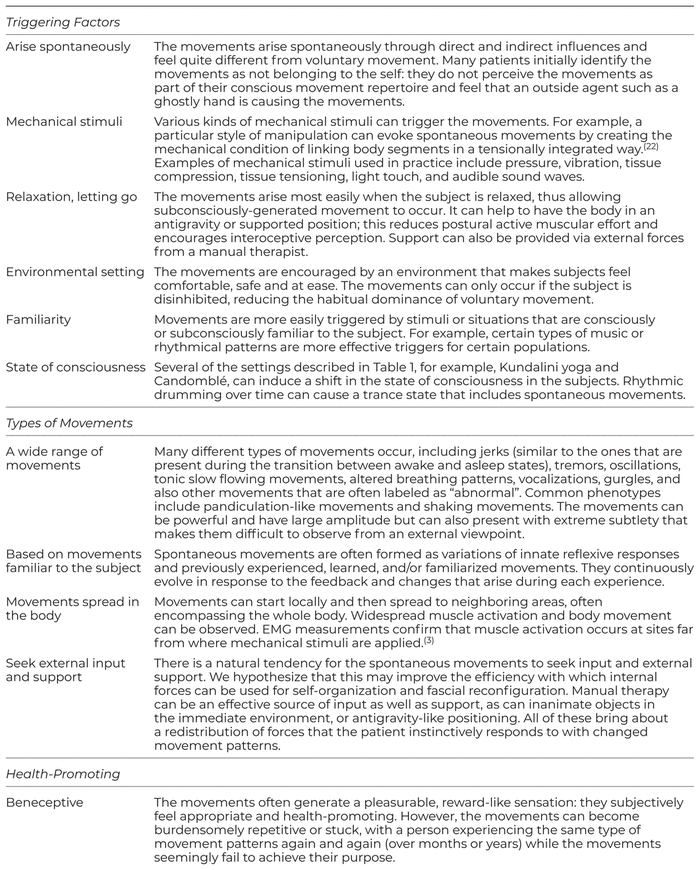

There are many different triggers of spontaneous movements, such as mechanical and sensory stimuli, clinical setting, the environment, and expectations. Spontaneous movements can be triggered in the practices listed in Table 1, or can arise on their own as in the self-described case reports. While the conditions in therapeutic settings have been described,(5) spontaneous self-experiences have not been well-documented. In our case reports, two cases reported that they were confused and felt alone with their experience. They also reported that people did not understand or believe their spontaneous movements and, instead, interpreted them as “faking” or “acting up”.
Some of the disciplines in Table 1 use specific mechanical stimuli to interact with spontaneous movements, whereas others use a broader range of stimuli. For example, tension and trauma-releasing exercises uses stretching and “fatiguing” of specific muscles to evoke spontaneous tremors, whereas Tensegrity Touch uses a much more sustained pressure stimulus to bring about a wide variety of spontaneous movements. Both of these can be contrasted with Candomblé, which uses a trance state to create spontaneous movements. Even though these triggers are different from one another, they all lead to the facilitation of spontaneous movements.
A reduction of postural tension can trigger spontaneous movements. Antigravity positions—such as suspension from the ceiling as in aerial yoga, being supported by a therapist during a myofascial unwinding technique—or other positions that promote floating-like sensations, may reduce the effects of postural tension, making spontaneous movements more easily accessible and easier to perceive.
Massmann(5) lists preconditions for myofascial unwinding in a clinical setting. These include feeling safe and trusting the practitioner, oneself, and the practitioner-recipient relationship. Patient “letting go” is the general condition for spontaneous movements.
There are many phenotypes of movement. Appendix A lists some examples of spontaneous movements documented in videos, which include parts of the body or the whole body.
Pandiculation-type movements are one common phenotype of spontaneous movements, which have benefits of restoring the structural and functional equilibrium of the myofascial system.(4) Like yawn reflexes, we believe spontaneous movements can arise due to bodily state needs, or can be influenced and encouraged by other external triggering agents that involve mirror neuron systems and promote disinhibition. Clinical experiences by LFB and JB confirm that patients agree that the movements feel similar to pandiculation, especially when the phenotype of the movements matches.
EMG measurements confirm that movements are not localized. A myofascial technique application to the right side of the thorax evoked tonic reflexes that were synchronically measured at lumbar and cervical regions with EMG.(3)
The practitioner-recipient (clinician-patient) relationship influences the experience of spontaneous movements.(5) Supportive environments, as well as support being provided by another person, benefits and enhances spontaneous movements.
Anecdotal evidence suggests that spontaneous movements have health-promoting potential. Engaging with the movements may be viewed as a heuristic, trial-and-error process where a person is likely to discover and learn health-promoting movements and behaviors directly from experience. Over time, this can lead to the discovery of movement strategies that offer higher accuracy as well as lower effort. In addition, through unpredictable reconfiguration, spontaneous movements can provide stress reduction, and improved functionality and mobility.
Spontaneous movements are usually beneceptive, generating a pleasurable or positive motivational feeling. A person experiencing them feels that the movements are appropriate and health-promoting. Case reports indicate that while engaging with spontaneous movements, unexplored movements (e.g., moving beyond their normal range of motion) or pain arising from the movement are still felt as appropriate. The subjects have the feeling that this pain is OK, and often a part of healing. Experiencing the spontaneous movements increases the set of familiar/safe body positions, sensations, and movements.
There is anecdotal evidence of spontaneous movements being used constructively in a bodywork setting. Manual therapy, such as myofascial unwinding, results in patients reporting a “sense of returning to the body” and “increased physiological awareness”.(5) Clinical observations (LFB and JB) are that spontaneous movements result in patients feeling calmer, having less pain, having increased range of motion and better movement control. During the application of myofascial unwinding techniques, clinicians report that they can feel a reduction in tissue tension in restricted areas, warmth, and a “melting” sense in the tissues.(11)
Spontaneous movements can become “stuck” or difficult to manage, and clinical intervention can help with this. Our case reports, especially Self-Described Case Report 3, illustrate that a clinician can observe the movements to see which body parts are not moving and then offer an intervention that helps the movements spread into the surrounding tissue. Indeed in myofascial unwinding, the therapist is advised to move a patient away from “fulcrumless”, since that would be unlikely to produce a therapeutic effect.(6,11)
Movements can have adverse effects, although this is rare. Self-Described Case Report 3 reported that the patient experienced powerful undulations in his spine, which could cause him to repeatedly hit his head, chest, and hips on the floor. LFB experienced that some wild movements can have adverse effects, such as a strong jerk of the leg causing a temporary weakening of the fibular muscles. In another case, strong mandibular movements caused a small tooth crack.
Spontaneous movements can usually be stopped voluntarily. The ability to control the movements distinguishes these nonpathological spontaneous movements from movement disorders. Disease-induced or drug-induced movement disorders create uncontrolled movements such as tremor, tic, myoclonic jerk, chorea, athetosis, dystonia, or hemiballismus.
Engaging with spontaneous movements is a learning process. The first experiences are memorable because the person is quite surprised by the unusual feeling of moving spontaneously, rather than in the accustomed consciously controlled manner. In the longer term, as months and years of experience with spontaneous movements are acquired, the subject develops personalized ways of interacting with the movements.
This description of a broad class of nonpathological spontaneous movements is intended to provide a basis for further research. There are many avenues of investigation related to clarifying the mechanisms underlying the movements. Spontaneous movements seem to be associated with a shift toward greater activation of the parasympathetic system. We have clinically observed signs of parasympathetic activation, such as changes in breathing patterns, ease in mobility, and other bodily responses that demonstrate reduction of arousal levels, and many of the triggers in Table 2 can help facilitate this shift. Tozzi(11) reviews several proposed theories regarding underlying mechanisms, including stimulation of mechanoreceptors followed by a parasympathetic response, ideomotor action, alterations in HRMT (human resting myofascial tone), and anandamide-mediated fibroblast remodeling and fascial reorganization. In addition to these theories, studies could focus on the role of adaptive reactions of the autonomic nervous system and social engagement, the role of the insula, the relationship of spontaneous movements to primitive and postural reflexes, and co-regulation processes between subject and therapist.
Other avenues of investigation relate to clinical application, studying how clinicians can support and exploit the health-promoting potential of spontaneous movements. Topics to be investigated include triggers of spontaneous movements (bodywork techniques and clinical setting), strategies for integrating a patient’s spontaneous movements with other bodywork techniques, and the use of movement collaboration as described in the section on treating dyskinesia. What is most important is that clinicians learn to educate patients on responding to spontaneous movements that arise in nonclinical settings, thus helping patients who are having difficulties, such as managing intense or overly-repetitive movements.
Nonpathological spontaneous movements are a common phenomenon, with people observing and using such movements in many different situations (Table 1). However, the phenomenon is not well documented, and we are in the early stages of understanding the mechanisms, purpose, and potential of this possible class of spontaneous movements. To establish that they indeed constitute a class of movements, it is necessary to demonstrate that the various instances of these movements are caused by the same underlying mechanisms. Investigation of this subject can be based on a variety of hypotheses and research approaches. Research techniques used in LFB’s ongoing investigation include TMS (transcranial magnetic stimulation) and heart rate variability, to be followed by fNIRS (functional near-infrared spectroscopy), fMRI (functional magnetic resonance imaging), and cinematics (to study the patterns of movements). This is just a small sampling of the research techniques that could be used in scientific investigation of this possible class of spontaneous movements.
We hypothesize that the movements are health-promoting, based on our clinical experience, as well as extensive anecdotal reports that the movements can be perceived as beneceptive. Large-scale case studies are required to scientifically investigate this topic. Our small set of case reports illustrate that subjects’ relationship with the spontaneous movements changes over time. When spontaneous movements first arise, the subjects respond with confusion and perhaps fear, because the movements feel strange and unexpected. As the subjects become more familiar and comfortable with the movements, they learn to safely interact with them in ways that anecdotally appear to be health-promoting. Because this class of spontaneous movements has so far received little attention in the scientific literature, the subjects in our case reports did not receive much help or understanding from the medical establishment. Our hope is that this article helps to make bodyworkers and movement therapists aware of the widespread existence of these types of movements, thus allowing them to support and reassure patients who exhibit spontaneous movements.
The authors declare there are no conflicts of interest.
1 Minasny B. Understanding the process of fascial unwinding. Int J Ther Massage Bodyw. 2009;2(3):10–17.
2 Bertolucci LF. Muscle repositioning: a new verifiable approach to neuro-myofascial release? J Bodyw Mov Ther. 2008;12(3):213–224.

3 Bertolucci LF, Kozasa EH. Sustained manual loading of the fascial system can evoke tonic reactions: preliminary results. Int J. Ther. Massage Bodyw. 2010;3(1):12–14.
4 Bertolucci LF. Pandiculation: nature’s way of maintaining the functional integrity of the myofascial system? J Bodyw Mov Ther. 2011;15(3):268–280.

5 Massmann RS. A Descriptive Study of the Myofascial Unwinding Experience. [Master’s Thesis]. Oakland, CA: Saybrook University; 2015.
6 Tozzi P, Bongiorno D, Vitturini C. Fascial release effects on patients with non-specific cervical or lumbar pain. J Bodyw Mov Ther. 2011;15(4):405–416.

7 Castro-Martín E, Galiano-Castillo N, Ortiz-Comino L, Cantarero-Villanueva I, Lozano-Lozano M, Arroyo-Morales M, et al. Effects of a single myofascial induction session on neural mechanosensitivity in breast cancer survivors: a secondary analysis of a crossover study. J Manip Phys Ther. 2020;43(4): 394–404.

8 Blostein D. Simulation of abstract models of structural homeostasis. J Bodyw Mov Ther. 2016;20(2):373–376.

9 Perez-Vale KZ, Peifer M. Orchestrating morphogenesis: building the body plan by cell shape changes and movements. Development. 2020;147(17):dev191049.


10 Braun N, Debener S, Spychala N, Bongartz E, Sörös P, Müller H, et al. The senses of agency and ownership: a review. Front Psychol. 2018;9:535.


11 Tozzi P. Fascial unwinding technique. In: Liem T, Tozzi P, Chila A, eds. Fascia in the Osteopathic Field. London, UK: Handspring Publishing; 2017:Chapter 40.
12 Fernández-Pérez AM, Peralta-Ramírez MI, Pilat A, Villaverde C. Effects of myofascial induction techniques on physiologic and psychologic parameters: a randomized controlled trial. J Altern Complement Med. 2008;14(7):807–811.

13 Dorko BL. The analgesia of movement: ideomotor activity and manual care. J Osteopath Med. 2003;6(2):93–95.

14 Berceli D, Salmon M, Bonifas R, Ndefo N. Effects of self-induced unclassified therapeutic tremors on quality of life among non-professional caregivers: a pilot study. Glob Adv Health Med. 2014;3(5):45–48.

15 Berceli D. Shake it Off Naturally: Reduce Stress, Anxiety, and Tension with [TRE]. Scotts Valley, CA: CreateSpace Publishers; 2015.
16 Payne P, Levine PA, Crane-Godreau M. Somatic experiencing: using interoception and proprioception as core elements of trauma therapy. Front Psych. 2015;6:93.
17 Stromsted T. Authentic movement: a dance with the divine. Body Mov Dance Psychother J. 2009;4(3):201–213.

18 García-Díaz S. The effect of the practice of Authentic Movement on the emotional state. Arts Psychother. 2018;58:17–26.

19 Shannahoff-Khalsa DS. An introduction to Kundalini yoga meditation techniques that are specific for the treatment of psychiatric disorders. J Alt Compl Med. 2004;10(1):91–101.

20 Andrews E. The Gift to be Simple: Songs, Dances and Rituals of the American Shakers. New York, NY: Dover Publications; 1940.
21 Melcher MF. The Shaker Adventure. Princeton, NJ: Princeton University Press; 1941.
22 Bertolucci LF. Muscle repositioning: combining subjective and objective feedbacks in the teaching and practice of a reflex-based myofascial release technique. Int J Ther Massage Bodyw. 2010;3(1):26–35.
23 McKay W, Ovechkin A, Vitaz TW, Terson de Paleville MS, Harkema SJ. Long-lasting involuntary motor activity after spinal cord injury. Spinal Cord. 2011;49(1):87–93.

24 Senna I, Russo C, Parise CV, Ferrario I, Bolognini N. Altered visual feedback modulates cortical excitability in a mirror-box-like paradigm. Exp Brain Res. 2015;233(6):1921–1929.

Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
The following videos illustrate spontaneous movements in a variety of settings.
Myofascial unwinding: John Barnes https://youtu.be/1QM-8_DwArU; without therapist present https://youtu.be/-8FI7kHOSiE
Simple contact: Barrett Dorko https://youtu.be/F8tvipt_-3Y
Tensegrity Touch: https://www.youtube.com/user/FernandoBertolucci/videos
TRE: partners https://youtu.be/uIy7saco04k; parent and child https://youtu.be/VeXeBe300mo
Somatic experiencing: https://youtu.be/nmJDkzDMllc?t=1250 (at 20:50)
Authentic movement: group setting https://youtu.be/fcZGUTy5wYk
Continuum movement: https://youtu.be/o3KBPqbPd-8; https://youtu.be/enWQoYRl_TM; https://youtu.be/1AF_ZCJ9lPk
Qi Gong: spontaneous Qi https://youtu.be/efu5vjdzAfc
Kundalini yoga: https://youtu.be/FILB4muyBX8?t=278; https://youtu.be/W6gZfKGVsw8; https://youtu.be/bUtqGjSaLh0; https://youtu.be/63WGG1r9s9U
Candomblé: https://youtu.be/dr3zQRXzuvY?t=62
I [PRINT FULL NAME]
give my consent for the Material about me/the patient to appear in a Journal publication.
I confirm that I:
have seen text or other material about me/the patient
have read the article to be submitted to a Journal
am legally entitled to give this consent.
I understand the following:
(1) The Material will be published without my/the patient’s name attached, however I understand that complete anonymity cannot be guaranteed. It is possible that somebody somewhere - for example, somebody who looked after me/the patient or a relative - may recognize me/the patient.
(2) The Material may show or include details of my/the patient’s medical condition or injury and any prognosis, treatment or surgery that I have/the patient has, had or may have in the future.
(3) The article may be published in a journal which is distributed worldwide. Once published, the article will be placed on the journal’s website and may also be available on other websites.
(4) The text of the article will be edited for style, grammar and consistency before publication.
(5) I/the patient will not receive any financial benefit from publication of the article.
(6) The article may also be used in full or in part in other publications and products published by the journal and/or by other publishers.
(8) This consent form will be retained securely and in confidence in accordance with the law, for no longer than necessary.
Signed:
[Signature]
Print name:
[Name]
Address:
[Address]
Email address:
[Email]
If signing on behalf of the patient, please give the reason why the patient can’t consent for themselves.
[Reason if not patient]
Date:
[Date]
If you are signing for a family or other group, please confirm that all relevant members of the family or group have been informed.
[Yes, informed]
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 15, NUMBER 3, SEPTEMBER 2022