Wray Barraclough, BSc, RMT1, Amanda Baskwill, PhD, RMT2, Colin Higgs, PhD3, Stacey Neilson, BA(Hons), RMT1, Debbie Wilcox, BEd, RMT1
1Centennial College, Toronto, ON, Canada
2Loyalist College, Belleville, ON, Canada
3Memorial University, St. John’s, NL, Canada
An investigation into the work-related pain (WRP) experienced by Massage Therapists (MTs) in Ontario, Canada was undertaken using voluntary completion of an online questionnaire following broad distribution of requests to take part in this study. Data from respondents were included for analysis if they provided informed consent and were a currently or previously registered MT in the region. With voluntary participation, self-selection respondent bias must be considered in evaluating reported results. Valid questionnaires (n=1103) were analyzed both quantitatively and qualitatively. Massage therapists ranged in age from 20 to 73 years, and 85% of respondents were female.
The overwhelming majority (85%) of MTs had experienced, or were experiencing, WRP at one or more of five pre-identified, primary locations with the hand/wrist, the most common site (65.5%); followed by the fingers/thumb (60.3%), shoulder (55.0%), lower back (50.1%), and neck (49.2%). Females were significantly more likely to report neck and shoulder pain than males, and were significantly more likely to report WRP at a higher number of body locations, with approximately one in five female MTs reporting WRP at all (5) primary sites. On a 10-point pain-severity scale, females reported significantly higher perceived pain than males.
Work-related pain was attributed to the gradual onset of musculoskeletal conditions by 60.3% of respondents, with no other choice of cause being reported by more than 11.1%. There was clear indication of WRP impacting the lives of MTs, with 48% reporting an impact on activities of daily living, 31% reporting a loss of income, 54.6% working in pain, and 30.5% considering changing (or having changed) their profession. Various work adjustments to WRP were reported, including altered biomechanics and greater rest between patient treatments.
The reported data suggested that WRP was a limiting factor for MTs’ work capacity.
KEYWORDS: work-related pain, massage therapist, hand pain, therapist pain, Ontario, career longevity
Success as a massage therapist (MT) is partially dependent on individual physical capacity and ongoing good health. A study from Statistics Canada reports that the hand accounts for 28% of reported work injury locations and that healthcare workers make up 3% of all reported injuries.(1) This rate of injury was the sixth highest of listed professions and, as a result, investigation into work-related pain (WRP) or injury in health professionals is of great importance.
A professional earnings survey by the Registered Massage Therapists’ Association of Ontario (RMTAO) reported that 51% of practitioners would like to work more hours per week; however, 40.3% of those who wished to work more hours chose not to, due to the physically demanding nature of the work, and a further 13.4% did not take on more work because they feared physical burn-out.(2) Massage therapy publications(3–5) and projects(6) address ergonomics and self-care strategies for the purpose of career longevity, suggesting that physical limitations and the risk of injury are primary concerns for members of the massage therapy profession.
Currently, research regarding WRP within the massage therapy profession is limited, leading the profession to draw upon findings from other relevant health care research. Studies within the nursing,(7,8) physical therapy,(9,10) and occupational therapy(11) professions identified common areas of WRP and provided location comparisons for this study. Massage therapy specific investigations have also explored WRP and found the main location of WRP to be fingers and thumbs.(12,13) Of note is the identification of manual techniques as causative and perpetuating factors of WRP for physical therapists.(9,14,15,16) Research in the field of manual therapy provided background information related to WRP management strategies,(17) job strain(18) of physical therapists, as well as injury-forced work reductions of MTs.(19)
Although the body of massage therapy specific research is growing and the overlap of technique delivery between physical therapy and massage therapy provides a credible degree of transferability between the professions, a deepened understanding of WRP of MTs is required. Massage therapy is regulated in the province of Ontario, Canada, which is the location of approximately 70% of Canada’s MTs, creating a large standardized pool of potential survey respondents. This cross-sectional study explores self-reported WRP of MTs in Ontario, Canada. It examines the experience of, contributors to, and impact of MTs’ WRP within a framework from existing research,(12,13,19) which suggest that the nature of manual techniques, compounded by repetition and other biomechanical factors, create conditions for WRP in MTs. This study also challenges data in order to understand whether the variables of sex, age, years in practice, and hours of work per week are related to WRP. Additionally, this study examines beliefs and concerns of MTs related to the sources and prevention of WRP.
Approval for this study, number 193, was granted by the Research Ethics Board at Centennial College.
Consent was provided by participants via the questionnaire. The consent statement was presented as the initial screen, and the reader was invited to proceed to the questionnaire if they agreed to participate in the study.
Study participants were recruited through (a) an email sent directly to MTs listed in the College of Massage Therapists of Ontario (CMTO) public registry; (b) a news briefing and link to the questionnaire on the CMTO website; (c) an article and link on the Massage Therapy Canada website; and (d) a posting on the Registered Massage Therapist Association of Ontario website. Eligibility criteria were provision of informed consent and current or former registration with the CMTO.
A 42-item questionnaire was developed for this study, based on an earlier instrument by Albert et al.(13) that explored the musculoskeletal injuries of Canadian MTs. Items not related to sex, age, years in practice, and amount of work were removed (e.g., body mass index), and questions regarding specific episode(s) of pain were added. Input from additional sources(20–22) further contributed to the development of the questionnaire and focused on three key areas: experience of, contributors to, and impact of WRP. Documenting what MTs experience was identified as a necessary step to informing the profession of possible obstacles to success and the potential risks of WRP. The initial section of the survey gathered demographic information (sex, age, years in practice, and number of hours worked) which allowed us to draw a picture of the MT at risk of experiencing WRP. The next section was optional and focused on specific episode(s) of WRP which provided information related to impact and management of the WRP. A variety of response options were offered throughout all portions of the survey: yes or no, Likert scale, and open-ended. For the purpose of this study, WRP was defined by investigators as “pain that you have had that you feel was caused by or aggravated by your work as a massage therapist”. The draft questionnaire was reviewed by four experts in the field of massage therapy or musculoskeletal pain/injury. A pilot study was conducted with MTs (n=10) who completed the questionnaire and provided recommendations to improve questionnaire face-validity and question clarity. The revised questionnaire included 42 closed and open-ended items and was delivered online via SurveyMonkey™ (Momentive, San Mateo, CA). The inclusion of open-ended questions, limited access to the survey (direct email and three professional-focused website offerings), and allowance of a single response only from an IP address helped to ensure that the survey was completed by a person.
Raw data were cleaned using manual inspection and IBM SPSS Data Preparation and Missing Data software (IBM SPSS v 27, IBM SPSS Statistics, Armonk, NY) prior to analysis. Descriptive statistics were generated for demographic variables, and group differences in interval or ratio variables were analyzed using analysis of variance (ANOVA) to identify statistically significant between-group differences. Chi-squared tests were also utilized. Statistical significance was set at p < .05.
Respondents selected from six possible areas of WRP: low back, neck, shoulder, hand/wrist, finger/thumb, and other. Quantitative analysis was restricted to the five pre-determined choices of WRP location; data from “other” locations of pain were not analyzed. Age groupings were as follows (20–29, 30–39, 40–49, 50–59, 60–69, 70+ years of age), years in practice were grouped to reflect early versus established therapists (0–5 and greater than five years in practice), and hours worked per week were separated into part-time and full-time. For the purpose of this study, investigators defined part-time as 20 hours or less per week and full-time as greater than 20 hours per week. There was no specific definition of what constituted ‘work’.
Analysis of responses to open-ended questions was undertaken using steps outlined by Auerbach and Silverstein,(23) as well as Morse and Field.(24) The data were examined to formulate an understanding of how MTs viewed their experience within the framework related to risk factors of WRP (manual techniques, repetition, and biomechanics). Initially, two research assistants working in communication with one of the co-investigators explored the qualitative data to identify common concepts related to the framework. Using Excel spreadsheets, and tables to track occurrences of similar words or ideas, these initial discussions identified dominant concepts from the collected data, as responses frequently consisted of a single word or short statement.
A total of 1172 respondents opened the online questionnaire, of whom 50 did not provide informed consent and were eliminated from consideration. A further 19 respondents indicated that they were not, and had not been, registered as MTs in Ontario and, as a result, 1103 responses met the inclusion criteria and were analyzed.
Of 1103 valid responses, 84.6% (933) were female and 15.4% (170) male. Respondents ranged from 20 to 74 years of age, with an average age of 40.7 years (SD 10.9). The average number of years in practice was 10.42 years (SD 7.4), and the average number of hours worked per week was 19.05 hours (SD 9.28).
Respondents indicated whether or not they had experienced WRP and, if they had, were asked to provide details related to a single specific episode. Work-related pain was reported to have been experienced previously, or was being experienced currently, by 84.9% (929) of massage therapists. The prevalence of reported WRP did not differ significantly by sex (χ21 = 1.4, p = .24), age (χ25 = .2, p = .99), or years in practice (χ21 = 2.4, p = .12). Part-time MTs (defined as working 20 hours or fewer per week) were significantly more likely to report WRP than those working full-time (χ21 = 3.8, p = .05).
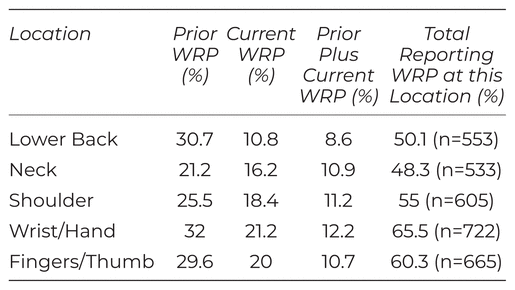
Body location of WRP, currently or previously experienced, is reported in Table 1. Figure 1 shows the percentage of respondents reporting WRP at 1, 2, 3, 4, or 5 different body locations.
Table 1 Percentage of Massage Therapists Reporting WRP at Five Researcher Identified Body Locations

|
| ||
|
Figure 1 Percentage of respondents reporting WRP at 1, 2, 3, 4, or 5 different body locations. | ||
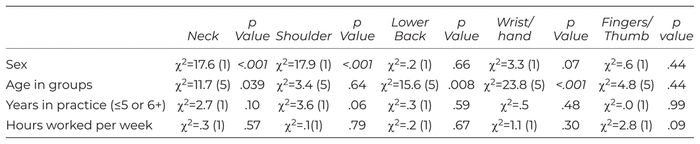
Of the five researcher-determined body locations, highly significant differences in prevalence between male and female respondents were reported for neck pain and shoulder pain, with females reporting higher prevalence than males for both locations. Table 2 presents results where it can be seen that there were no significant differences between sexes in prevalence for lower back, wrist/hand, or fingers/thumb WRP. Age presented some significant results related to the neck, lower back, and wrist/hand, which showed a decrease in occurrence as MTs grew older. Body location of WRP was not significant in relation to hours worked per week.
Table 2 Location of Pain Comparisons with Sex, Age, Years in Practice, and Hours Worked per Week (chi square analysis)
In addition to reporting on researcher-identified sites of MTs’ WRP, respondents identified other body locations at which they experienced WRP. Of those reporting other body locations, 29% identified the elbow, followed by mid-back (10%), hip, feet and forearm (9% each), and knee (7%).
When considering the number of different body locations for WRP, males were significantly (F1, 1101 = 13.6, p = .007) more likely to report no WRP or a single body location (mean 2.23, SD 1.74), while females were more likely to report WRP at two or more locations (mean 2.77, SD 1.76), with more than 20% of females reporting current or previous WRP at all five primary locations investigated (lower back, neck, shoulder, wrist/hand, and fingers/thumb). The reported number of locations of WRP did not differ between age groups (F5, 1095 = 5.6, p = .06), by years in practice (F1, 1799 = 1.9, p = .17), or by hours worked per week (F1, 990) = 0.8, p = .37.
On the 10-point self-reported pain scale (1 = low pain to 10 = severe pain), the mean reported severity of pain was 6.45 (SD 2.02). Further analysis showed females reported significantly higher levels of perceived pain than males (F1 = 14.6, p < .001), and that MTs in practice more than five years also reported more severe pain (F1 = 12, p < .001). Reported pain severity was not significantly related to age (F5 = 0.4, p = .84), or hours worked per week (F1 = 1.2, p = .27).
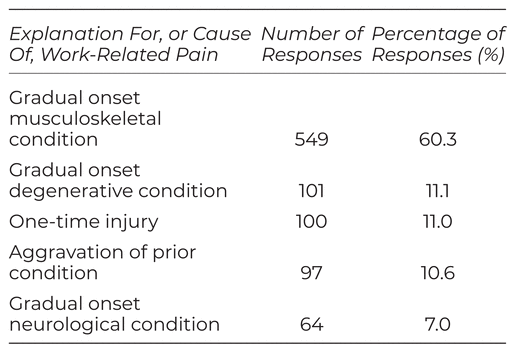
Respondents reported their perceived explanation for, or cause of, WRP, with responses shown in Table 3.
Table 3 Explanation For, or Cause Of, WRP in Those Reporting Pain
The perceived cause of WRP seems to be random and was not significantly related to respondents’ sex (χ24 = 4.6, p = .34), or age (χ220 = 28.1, p = .11), years in practice (χ24 = 3.1, p = .55) or hours worked per week (χ24 = .9, p = .93).
Following WRP, 400 (42.9%) MTs temporarily reduced their workload. Workload reduction was more common in those in practice more than five years than those in practice five years or less (χ21 = 5.2, p = .02). Reduction in workload was unrelated to sex (χ21 = .4, p = .54), age (χ25 = 7.6, p = .18, or hours worked per week (χ21 = .02, p = .9).
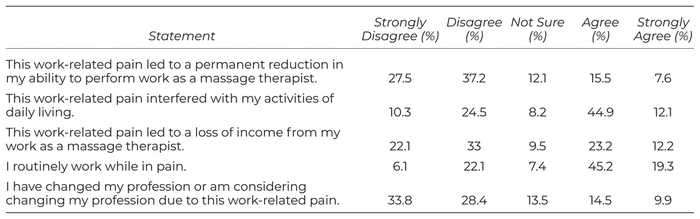
Respondents reported on the impact of WRP by rating a number of statements related to work (found in Table 4), using a five-point Likert scale ranging from ‘strongly agree’ to ‘strongly disagree’.
Table 4 Percentage of MTs Reporting Degrees of Agreement with Various Statements on the Impact of a Specific Episode of Work-Related Pain
Additionally, 64.8% of MTs reporting on a specific episode of WRP reported that, as a result, they had changed the way they do their job, and 90.1% reported that they had sought professional help in treatment.
Open-ended responses to concerns about WRP were categorized into four themes: (a) biomechanics and body usage, (b) the need for alternative modalities, (c) hours of hands-on practice, and (d) self-care regimens and physical limits. Many MTs admitted they did not initially comprehend the impact that the work of the profession might have on their bodies, and expressed frustration that the resulting WRP or injury could compromise their financial security. Therapists urged this knowledge gap be addressed in MT training.
Massage therapists described making changes to the biomechanics of their work, and changing body usage to avoid or reduce physical pain and remain effective in their practice. There were frequent references to acquiring adjustable tables and chairs to optimize body mechanics.
Respondents believed that some WRP stemmed from what they considered to be “bad habits” developed early in their careers, and that improving techniques reduced WRP. Therapists referred to “hiking shoulders”, “torquing wrists”, or overusing thumbs/fingers as undesirable, and frequently reported reducing time spent using thumbs for techniques.
There was notable concern by MTs regarding the physically demanding and repetitive nature of what would be considered traditional Swedish massage techniques. In addition, 36% of respondents indicated they had modified their work, including taking on management roles to reduce pain. In addition, 42% of respondents reported that they incorporated physical aids to prevent, or as a result of, WRP. They also reported varying techniques to avoid repetition. Multiple comments were noted regarding the importance of post-graduate skills training to introduce techniques and modalities that did not involve deep pressure and could be interspersed with other treatments; the most common being acupuncture, manual lymph drainage, craniosacral therapy, and hydrotherapy.
Therapists frequently reported reducing their hours of hands-on work. Many MTs indicated that they had additional part-time jobs (often teaching) or worked in other areas within the profession. Another strategy used by MTs was to increase the time between scheduled appointments.
A common response was the need to preserve professional viability by identifying personal limits and avoiding excessive work. Therapists reported that committing to a regular self-care regimen helped them to function better in day-to-day tasks.
The overwhelming majority of MT respondents (84.2%), reported WRP at some point in their career, indicating that WRP is a concern for the profession. The most commonly reported location of WRP was the hand/wrist complex, reported by 65.5% of respondents, closely followed by fingers/thumb at 60.3%. Additionally, WRP in the neck and shoulder was reported more often by women than men. Women reported WRP of greater severity and at more locations than men. Of note is that the frequency of reporting at a location decreased with years in practice; MTs in practice more than five years reported less often, which introduces the possibility that MTs experiencing WRP may have left the profession. We saw an increase in workload reductions for MTs in practice greater than five years and they also tended to have WRP of greater severity.
Congruent with the stated framework, respondents attribute biomechanics, repetition, and the high usage of manual techniques for their WRP and, because of their pain, often seek other part-time work.
Although the reporting of low-back pain has classically been high in other health care professions such as nursing, paramedicine, and physiotherapy,(25,26) often due to ergonomics and patient transfers,(27,28) it was less prevalent in our study or as reported by Jang et al.(12) This may be due to the infrequency with which MTs perform patient transfers.
Aligning with existing research on pain perception, we found that women reported their WRP as more severe than men when measured by the pain scale.(29)
Chronicity can be explained by the cumulative impact of regular manual work and the progression of degeneration over time.(30) While a high percentage of MTs identified the perceived mechanism of their pain as being of a “gradual onset musculoskeletal condition”, it was also noted that, although fewer MTs in practice more than five years reported pain at most locations, they did report pain of greater severity, aligning with King et al.(31)
Frequently, throughout the qualitative portion of this study, respondents named the repetitive nature of their work as a contributor to their WRP. This was also reported in a study by Glover et al.(32) which identified “performing the same task over and over” as the activity physiotherapists believed factored most in their work-related musculoskeletal disorders. Magee and colleagues state that “hand-intensive tasks that are highly repetitive or forceful (or both) in awkward or sustained postures” (p. 747) can lead to musculoskeletal disorders of the upper limb.(30) These phrases could accurately describe the delivery of massage therapy techniques and support our findings.
When exploring modifications, the communication by respondents of the problematic nature of excessive use of fingers and/or thumbs and the need for modifications was notable; this aligned with the study by Rossettini et al.(33) The necessity for these modifications seems apparent as the hands are typically the point of contact with the patient and are under high degrees of forces, as demonstrated by Snodgrass et al.(34) Modifications reported by MTs included utilization of a hydraulic or electric table, using forearms and elbows instead of thumbs/fingers or using different modalities altogether.
Anecdotal responses from our study describe ways MTs adapted to working in pain: reducing clinic hours, changing patient demographics or treatment modalities. Similar adaptations to WRP are seen in the study on work productivity by Campo and Darragh.(35)
Additionally, our study found that 24% of respondents reporting that they had changed or were considering changing professions due to their WRP. Cromie et al.(36) similarly observed physical therapists leaving or switching areas within the profession at a rate of 1 in 6 (17%).
The clear definition of our subject pool, the anonymous method of recruiting respondents, and the resultant large sample size were strengths of the study. Also strengthening the study were the consultations with subject specialists, and the pilot study completed in the development of the questionnaire. The analysis of qualitative data by different members of the research team, the neutral nature of open-ended questions, and the fact that qualitative results supported previous findings(9,12,14,15) further bolstered trustworthiness, as outlined by Morse and Field.(24)
Caution interpreting the results of this study should be exercised, given the potential of responder bias from self-selection of respondents. It is possible that MTs with experience of WRP may have been more likely to voluntarily complete the survey or that MTs never experiencing WRP were less likely to complete the questionnaire, thus potentially skewing the results. Other weaknesses include the possibility of survey fatigue due to the length of the questionnaire (42 items in total). Additionally, although the sample size was substantial (n=1103) the fact that this represented only 8.6% of the provincial membership is a concern. An unexplained difference in male/female proportional representation between the study (15%/85%) and regional male/female MT profile (21.7%/78.3%)(37) is another concern and may potentially have introduced a specific self-selection bias in results. The fact that many MTs are self-employed reduces the possibility of comparative data generated by the Workplace Safety and Insurance Board of Canada. Increased specificity of the questionnaire would have strengthened results, such as identifying an objective diagnosis of WRP, defining ‘work’ (it is unclear whether respondents identified the amount that they worked as hands-on time solely or time taken with all work-related responsibilities). Additionally, the perceived mechanism of pain results depended on subjective reporting, although due to regional standards, respondents could be considered informed.
Clarification of the WRP experienced by MTs based on sex is needed. While it seems that hands and wrists are at risk, a continued exploration of risk factors associated with hands-on modalities is urgently indicated. As well, a full understanding of how MTs manage their WRP and the impact on chronicity would be useful.
This study begins to identify that MTs are at a high risk of experiencing WRP at some point during their career, with impact greater the longer an MT is in practice. Further to this, we see a greater percentage of women reporting multiple locations for WRP and higher levels of pain. In general, hand pain that may involve areas from fingers to wrist predominates the experience of therapists. Subjective reporting shows that MTs modify working conditions and hours of work per week to keep WRP under an individually set threshold, with chronic pain above this threshold triggering actual or contemplated change of profession.
The large response to this survey illustrates that MTs are concerned and want to communicate their experience related to WRP. The results generated by this study identify the necessity for effective technique delivery, good ergonomics, and therapist-care management. This may help to inform existing and future MTs, as well as educational institutions, of the possible risks of WRP. Considering that WRP is leading MTs to consider leaving the profession and becomes more severe over time, research looking closely at best practices of all available modalities could inform future massage therapy practices to the benefit of the health of MTs, and may lead to an ideological shift in the delivery of care toward efficacy and away from the classically based delivery of manual techniques.
Many thanks to Centennial College School of Community and Health Studies which released the principal investigator from academic responsibilities via professional development leave to complete this project. Thanks to the Centre for Applied Research and Innovation for an Applied Research and Innovation Fund grant. Thank you also to Lilian Barraclough who was always willing to help and provided tremendous support to the principal investigator.
The grant from Centennial College’s Applied Research and Innovation Centre (ARIC) allowed for release time for Stacey Neilson and an hourly remuneration for Debbie Wilcox. Two student assistants were also hired briefly to organize the qualitative data. The School of Community and Health Studies (SCHS) of Centennial College provided release time for the principal investigator, Wray Barraclough. Neither ARIC nor SCHS had any involvement nor influence on this study.
1 Wilkins K, Mackenzie, S. Work Injuries. Health Reports, Statistics Canada, Vol. 18. No.3, August 2007. https://www150.statcan.gc.ca/n1/pub/82-003-x/2006007/article/injuries-blessures/4149017-eng.htm#a5
2 Registered Massage Therapists’ Association of Ontario. 2013 Registered massage therapist earnings survey: results snapshot [cited 2014 Jan 15]. Available at: https://www.rmtao.com/Media/Default/Surveys/2013%20Registered%20Massage%20Therapists%20Earning%20Survey.pdf. Retrieved May 18, 2022.
3 Benjamin B, Greene L, Goggins R, Peterson J. Save Your Hands!: The Complete Guide to Injury Prevention and Ergonomics for Manual Therapists, 2nd ed. Coconut Creek, FL: Gilded Age Press; 2008.
4 Frye, B. Body Mechanics for Manual Therapists A Functional Approach to Self-Care, 3rd ed. Baltimore, MD: Lippincott Williams & Wilkins; 2010.
5 Benjamin P. Pearson’s Massage Therapy: Blending Art with Science, 6th ed. Boston, MA: Pearson; 2015.
6 Anderson R. All about the MTF ergonomics project. Evanston, IL: Massage Therapy Foundation; 2021. Available from: https://massagetherapyfoundation.org/mtf-ergo-project/. Accessed March 12, 2022.
7 Karahan A, Kav S, Abbasoglu A, Dogan N. Low back pain: prevalence and associated risk factors among hospital staff. J Adv Nurs. 2009;65(3):516–524.

8 Tinubu BM, Mbada CE, Oyeyemi AL, Fabunmi AA. Work-related musculoskeletal disorders among nurses in Ibadan, south-west Nigeria: a cross-sectional survey. BMC Musculoskel Dis. 2010;11(1):1–8.

9 Rozenfeld V, Ribak J, Danziger J, Tsamir J, Carmeli E. Prevalence, risk factors and preventive strategies in work-related musculoskeletal disorders among Israeli physical therapists. Physiother Res Int. 2010;15(3):176–184.

10 Wajon A, Ada L, Refshauge K. Work-related thumb pain in physiotherapists is associated with thumb alignment during performance of PA pressures. Manual Ther. 2007;12(1):12–16.

11 Anyfantis ID, Psychouli P, Varianou-Mikelidou C, Boustras G. Cross-sectional survey on burnout and musculoskeletal disorders in Greek and Cypriot occupational therapists. Occup Ther Mental Health. 2020;36(3):291–302.

12 Jang Y, Chi CF, Tsauo JY, Wang JD. Prevalence and risk factors of work-related musculoskeletal disorders in massage practitioners. J Occup Rehab. 2006;16(3):416–429.

13 Albert WJ, Currie-Jackson N, Duncan CA. A survey of musculoskeletal injuries amongst Canadian massage therapists. J Bodywk Move Ther. 2008;12(1):86–93.

14 Darragh AR, Campo M, King P. Work-related activities associated with injury in occupational and physical therapists. Work. 2012;42(3):373–384.


15 Snodgrass SJ, Rivett DA. Thumb pain in physiotherapists: potential risk factors and proposed prevention strategies. J Manual Manip Ther. 2002;10(4):206–217.

16 Cornwell L, Doyle H, Stohner M, Hazle C. Workrelated musculoskeletal disorders in physical therapists attributable to manual therapy. J Manual Manip Ther. 2021;29(2):92–98.

17 Passier L, McPhail S. Work related musculoskeletal disorders amongst therapists in physically demanding roles: qualitative analysis of risk factors and strategies for prevention. BMC Musculoskel Dis. 2011;12(1):1–9.

18 Campo MA, Weiser S, Koenig KL. Job strain in physical therapists. Phys Ther. 2009;89(9):946–956.


19 Blau G, Monos C, Boyer E, Flanagan R, Lopez A, Tatum DS. Correlates of injury-forced work reduction for massage therapists and bodywork practitioners. Int J Therapeut Massage Bodywk. 2013;6(3):6.
20 Campo M, Darragh AR. Impact of work-related pain on physical therapists and occupational therapists. Phys Ther. 2010;90(6):905–920.

21 Dawson AP, Steele EJ, Hodges PW, Stewart S. Development and test–retest reliability of an extended version of the Nordic Musculoskeletal Questionnaire (NMQ-E): a screening instrument for musculoskeletal pain. J Pain. 2009;10(5): 517–526.

22 Magee D. Orthopedic Physical Assessment, 6th ed. Philadelphia, PA: Saunders Elsevier; 2014.
23 Auerbach C, Silverstein L. Qualitative Data: an Introduction to Coding and Analysis, Chapters 5–7. NY: New York University Press; 2003.
24 Morse J, Field P. Qualitative Research Methods for Health Professionals, 2nd ed., Chapter 6. Thousand Oaks, CA: Sage Publications; 1995.
25 Mroczek B, Łubkowska W, Jarno W, Jaraczewska E, Mierzecki A. Occurrence and impact of back pain on the quality of life of healthcare workers. Ann Agr Enviro Med. Published December 30, 2019; accessed March 22, 2022.
26 Milhem M, Kalichman L, Ezra D, Alperovitch-Najenson D. Work-related musculoskeletaldisorders among physical therapists: a comprehensive narrative review. Int J Occup Med Enviro Health. 2016;29(5):735–747.

27 Nordin NA, Leonard JH, Thye NC. Work-related injuries among physiotherapists in public hospitals: a Southeast Asia picture. Clinics. 2011;66(3):373–378.

28 Alrowayeh HN, Alshatti TA, Aljadi SH, Fares M, Alshamire MM, Alwazan SS. Prevalence, characteristics, and impacts of work-related musculoskeletal disorders: a survey among physical therapists in the State of Kuwait. BMC Musculoskel Dis. 2010;11(1).

29 Racine M, Tousignant-Laflamme Y, Kloda LA, Dion D, Dupuis G, Choinière M. A systematic literature review of 10 years of research on sex/gender and experimental pain perception—Part 1: Are there really differences between women and men? Pain. 2012;153(3):602–618.

30 Magee DJ, Zachazewski JE, Quillen WS. Pathology and Intervention in Musculoskeletal Rehabilitation. Philadelphia, PA: Saunders Elsevier; 2009.
31 King P, Huddleston W, Darragh A. Work-related musculoskeletal disorders and injuries: differences among older and younger occupational and physical therapists. J Occup Rehab. 2009;19(3):274–283.

32 Glover W, McGregor A, Sullivan C, Hague J. Work-related musculoskeletal disorders affecting members of the Chartered Society of Physiotherapy. Physiotherapy. 2005;91(3):138–147.

33 Rossettini G, Rondoni A, Schiavetti I, Tezza S, Testa M. Prevalence and risk factors of thumb pain in Italian manual therapists: an observational cross-sectional study. Work. 2016;54(1):159–169.

34 Snodgrass SJ, Rivett DA, Chiarelli P, Bates AM, Rowe LJ. Factors related to thumb pain in physiotherapists. Austral J Physiother. 2003;49(4):243–250.

35 Campo M, Darragh AR. Work-related musculoskeletal disorders are associated with impaired presenteeism in allied health care professionals. J Occup Enviro Med. 2012;54(1):64–70.

36 Cromie JE, Robertson VJ, Best MO. Work-related musculoskeletal disorders in physical therapists: prevalence, severity, risks, and responses. Phys Ther. 2000;80(4):336–351.

37 College of Massage Therapists of Ontario. TouchPoint: Keeping You in Touch with Massage Therapy Regulations in Ontario. Did You Know [regular series]. Spring/Summer 2015; 22(1):17–18. Available from: http://www.cmto.com/assets/TouchPoint_2015spring-en.pdf
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 15, NUMBER 3, SEPTEMBER 2022