
Sarah Fogarty , PhD
Massage therapist, Boronia, Victoria, Australia.Objective
To observe the effects of massage aiming to support a mum in her pregnancy after a previous stillbirth. The client’s goal varied over the course of her pregnancy, but her main motivation was to help manage the anxiety and stress of pregnancy after a previous stillbirth.
Methods
A 32-year-old pregnant woman received seven massages over a seven-month period. The Measure Yourself Concerns and Wellbeing (MYCaW) outcome measure was used at each session to identify the client’s concerns at that time point. Written feedback was also sought from the client just prior to her giving birth.
Results
The client’s concerns included anxiety, sciatica, stress, shoulder tension/soreness, and a lack of sleep. The client experienced a decrease in each concern after each treatment over the seven sessions and experienced improved well-being after each session. The client self-reported that the massage helped her cope, saying: “I’m not sure how I would have coped if I didn’t have her sessions.”
Conclusions
Massage is a treatment option for women experiencing pregnancy after stillbirth, which can provide physical and emotional support.
KEYWORDS: Massage, anxiety, stillbirth, grief, stress, support
There are almost six stillbirths a day in Australia.(1,2) Stillbirth is defined as “in-utero death from 20-weeks’ gestation until immediately before birth”.(3) Women who experience a stillbirth have indicated that the prospect of a pregnancy after a stillbirth was daunting, and they were concerned about the mental health impacts of being pregnant again.(4) Additionally, they were concerned about what to expect, the frequency of monitoring, and the types of care they would receive in future pregnancies.( 4) The majority of parents who experience a stillbirth will attempt to conceive again, and 50% of them will fall pregnant within a year of their stillbirth.(5)
Stillbirth profoundly alters the reality of subsequent pregnancies. The mental health of women in the pregnancy following stillbirth has been found to be affected, with women experiencing posttraumatic stress disorder symptoms(6) and significantly more depression and anxiety than pregnant women who had not experienced a stillbirth.(7,8) Research into the lived experience of parents experiencing pregnancy after a stillbirth shows that parents commonly experience conflicted emotions, extreme anxiety, heightened fear and anxiety, isolation, and a lack of trust in a good outcome and that pregnancy is survived or endured.(5) While there are medical guidelines on providing care to pregnant women who have had previous stillbirths, there is little evidence or practical advice on incorporating and providing psychological and/or emotional aspects of care to this population.(5,9) This is highlighted in the 2018 Cochrane review on care prior to and during subsequent pregnancies following stillbirth which found interventions addressing parental anxiety and depression are an urgent priority.( 9) Women experiencing pregnancy after a stillbirth reported that their emotional well-being was enhanced when empathy, support, and being listened to was part of the care provided.(5)
A massage consultation can be a place where empathy, support, and being listened to are part of the treatment experience, as demonstrated in a community program providing women massage after miscarriage, stillbirth or neonatal loss.(10) Massage during pregnancy has also been found to be beneficial for reducing antenatal anxiety and depression,(11) and may provide some psychological and or emotional benefits to women who experience pregnancy after a stillbirth. Pregnancy massage offers a potential option to support women who experience pregnancy after a stillbirth.
A 32-year-old female who works in administration was referred for massage to help her manage the symptoms of grief after experiencing a stillbirth at 37 weeks due to an umbilical cord accident. Just prior to the first anniversary of her child’s death the client informed me she was six weeks pregnant, and the agreed focus of the massage treatments became helping her manage the grief, anxiety and fear associated with a pregnancy after a still-birth. This case study is reporting on the use of massage to support emotional and physical health during her pregnancy after a loss. Her chief symptoms varied over the course of her treatment but included anxiety, sciatica, stress, shoulder tension/soreness, and a lack of sleep. She was connected to and using local stillbirth community support services, and was part of a pregnancy-after-loss online support group.
The client had a history of a previous pregnancy resulting in a live birth, no other history of loss and no issues with her health during her previous pregnancies. Her lifestyle was busy, and at times hectic, with work and raising children (blended family). She had sought and received psychological support after her stillbirth, and she was open to other sources of support. She had a network of support that included family, friends, health-care providers and community organizations. She had no comorbidities and no other relevant past medical history. See Table 1 for a timeline of important dates and times associated with the case.
Table 1
Timeline of Important Dates and Times Associated with the Case

There are no formal diagnoses available to quantify the specific effects of a stillbirth on a subsequent pregnancy. The client was attending psychological treatment and no mental health diagnosis was given prior or during her treatment period.
Limited physical assessment was undertaken due to the supportive nature of the treatment. Palpation was undertaken to determine the location of tender areas when applicable. Primarily, information was sought via verbal communication obtained during the consultation. The consultation time allocated for each session was 15 minutes to allow the client to share their experiences and updates on what was happening at each stage of their pregnancy journey. This included practical updates, such as when they were seeing their obstetrician and updates to the birth plan, as well as spiritual and emotional updates, such as how they were feeling and how they felt they were coping (or not), and physical updates on what areas of the body they felt needed attention either due to being pregnant and or as symptoms of stress, anxiety and/or grief.
The Measure Yourself Concerns and Wellbeing (MYCaW) outcome measure was used at each session to identify the client’s concerns at that time point. The MYCaW allows clients to choose their own concerns and write them down in their own words, and is completed before and after treatment.(12) The MYCaW collects both quantitative data (a seven-point Likard scale) and allows for written qualitative data.(12) The client lists one or two concerns they would like addressed in the treatment and they are also asked about their well-being.
Written feedback was also sought from the client just prior to her giving birth, to reflect on her experiences with massage including her reasons for seeking massage, the benefits she felt she received, and the needs she felt were meet from the massage. Written feedback included two visual analogue scales measuring perceived physical benefits and perceived psychological/ emotional benefits. The visual analogue scales were a straight horizontal line of 100 mm. The left end was no benefit and the right end was extremely beneficial. The client marked the line with a cross to indicate her response.
Treatment was undertaken in a multidisciplinary clinic (allied health and fitness professionals) that had a focus on pregnancy, postnatal, and family care. The room where the treatments occurred was shared by other therapists and was sparsely furnished.
The intervention was provided by the author, holding massage association membership as a remedial massage therapist. At the time of the treatments the therapist had over 20 years of experience as a remedial massage therapist including working predominately with pregnant women for last three years, and had experience working with parents who experienced miscarriage, stillbirth and/or neonatal death. The therapist had undertaken postgraduate pregnancy and postnatal massage training five years prior to providing these treatments. In the last two years, the therapist had undertaken grief massage courses through The Grief Institute, and had completed Holding Space for Pregnancy Loss via The Institute for the Study of Birth, Breath, and Death.
Based on research on massage during pregnancy, the massage applied was Swedish massage which included the following massage strokes: longitudinal gliding, transverse gliding, digital ischemic pressure, transverse frictions, and transverse gliding.(13,14) Massage was applied from the cervical to the lumbar area including the shoulders. Lighter pressure Swedish massage was performed initially with the intent of relaxing the client and warming her muscles and, depending on the purpose of the massage, specific deeper work in the lower back, shoulders, and gluteal area was applied. The conceptual approach utilized was based on a vulnerability-to-stress concept which acknowledges the impact of stress on a pregnant woman based on a biopsychosocial model (see Figure 1).
|
|
||
|
Figure 1 Conceptual framework for stress vulnerability and pregnancy massage after a stillbirth (image by Tanya Antusenok/Shutterstock). |
||
The role of massage was to provide support via symptom relief, such as reduction in pain via the gate control theory of pain(15) or an increase in serotonin levels,(16) a reduction in muscle tightness, improved mood state via increased vagal activity, and higher heart rate variability(15,17,18) and emotional support via relational continuity, the development of a good therapeutic relationship, and the collaborative model of care.(19)
This involved prior research on the experiences of having a stillbirth from a medical perspective and the perspective of a mother, as well as researching what it is like for women to be pregnant after a stillbirth. This allowed me to better understand what my client may have experienced and what her needs might be. Along with my training, this helped provide me with the terminology and context to ask questions during the consultations so that my client felt I understood what she was going through and what experiences were important to her. Time was allocated each session prior to the hands-on treatment to converse, including communication about negative emotions and experiences, where I used therapeutic listening and responding with empathy and curiosity to help strengthen the therapeutic alliance.(20) The client received seven treatments that were 60 minutes in length, with 45 minutes of treatment and 15 minutes of consultation time. The seven treatments were administered over seven months, with two cancelled appointments (see Table 1). The collaborative and flexible nature of the intervention never changed over the duration of the treatment. The frequency of the treatments was flexible based on the client’s needs, with the plan always being to support the client as they needed over the gestation of her pregnancy. At each of the seven appointments, the therapist checked in with her to see how she was going and if she felt she needed any other support. She was aware of, and was using, other support services as she felt she needed to. Informed consent was obtained verbally at each session.
The MYVCaW allows the client to list up to two concerns they would like addressed at each appointment. Table 2 shows the concerns listed by the client for each treatment session. The client experienced a decrease in each concern after each treatment over the seven sessions (see Table 3). Lower scores indicate fewer issues having concern. Scoring was from 0 to 6 with 0 being ‘not bothering me at all’ and 6 being ‘bothers me greatly’.
Table 2
MYCaW Concerns at Each Treatment
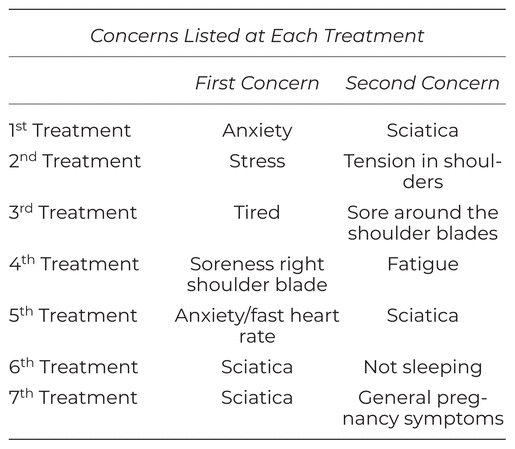
Table 3
MYCaW Pre- and Post-Treatment First and Second Concerns Scores
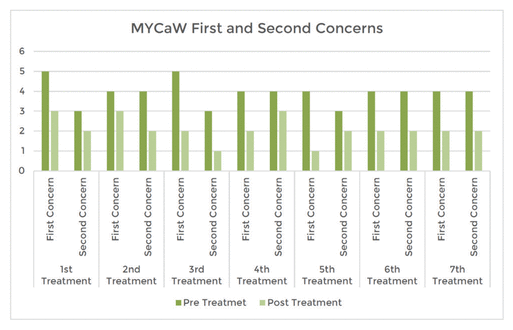
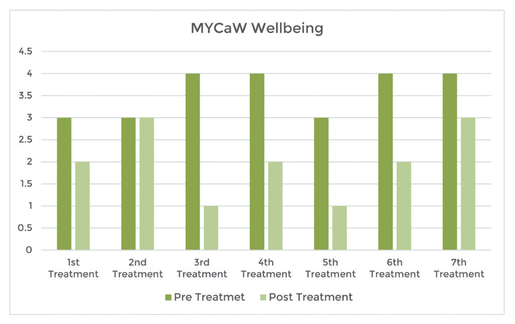
The client rated their well-being as being better after each massage compared to before the massage (see Table 4). A lower score indicated better well-being. Scoring was from 0 to 6 with 0 being ‘as good as it could be and 6 being ‘as bad as it could be’.
Table 4
MYCaW Pre- and Post-Treatment Wellbeing Scores
Written feedback provided by the client indicated that her reasons for using massage for her pregnancy after stillbirth was a mixture of physical needs (muscle stiffness and/or tightness and sleeplessness) and emotional/spiritual needs (stress relief, time out, help with depressive symptoms, help with anxiety symptoms, better overall mental health, and help to manage the grief of her loss). She experienced “reduced shoulder stiffness and sciatica” symptoms and felt that she was “better able to manage my overall anxiety and depressive symptoms” and that she “developed tactics and strategies to get through”. She indicated that the treatments were very beneficial with a score of 90/100 on the physical visual analogue scale and a score of 90/100 on the phycological/emotional visual analogue scale.
What she liked best was having “someone to talk to about what is going on, and the amazing relaxation massage”. The client felt that that massage meet a number of other needs, such as being listened to and being acknowledged (see Table 5).
Table 5
Other Needs Met by Massage for the Client

It was very important to the client that her therapist found out about her history and asked about some of her journey, had experience working with pregnant clients, and had experience working with bereavement.
The open-ended feedback the client gave about her treatments reported that the therapist
Was amazing, she took the time every session to make sure that I was coping and was great at listening. She didn’t judge (no matter how outrageous my comments), I’m not sure how I would have coped if I didn’t have her sessions… to look forward to. Her massages were always related to where I was feeling tension or pain and she always made sure I was comfortable and relaxed.
The treatment intervention used a collaborative approach and was very much client-led regarding frequency and timing of treatments. A loose plan was provided at her initial appointment suggesting that she might need fewer appointments at the beginning of her pregnancy and appointments spaced closer together as she got closer to giving birth. It was unknown how the client would manage and cope with her pregnancy after stillbirth and what she would need, thus the plan was fluid to accommodate this. The client did end up keeping to the loose plan regarding frequency of treatments. The client tolerated the treatment well and the timing was flexible enough to meet her needs. No adverse or unexpected events were experienced by the client over the course of her treatments.
No self-care recommendations or referrals to other practitioners were made during the duration of her treatment. Information was sought during the consultations about what support she was utilizing and strategies she was using to cope. The client used distraction and keeping busy as her main coping mechanisms, but as mentioned above, she had multiple support options including friends and community support groups.
The suggested rationale for why this client experienced the outcomes she did was that the conceptual model used to develop a treatment for this client included both physical and emotional care. This was achieved by providing symptom relief such as reduction in pain or muscle tightness and supporting emotional health via relational continuity, and by the development of a good therapeutic relationship and a collaborative care model. Whilst the massage treatments were able to meet several of her needs, she received other supportive care, such as an excellent obstetrician (the same obstetrician who delivered her still-born daughter), and the integrative care she received supported her health during her pregnancy after stillbirth. This highlights the importance of a client-centred treatment approach and important non-massage–related treatment effects such as the therapeutic relationship and feelings of safety.
A strength of the intervention provided is that massage can address both physical and emotional symptoms associated with pregnancy after stillbirth. The massage room can be a safe place where clients feel comfortable to share what they are feeling and provide an option for emotional support. Massage therapists can provide referral pathways to clients if they recognize that more help and support is needed. A limitation of the intervention is a lack of knowledge about the role massage might play in supporting women during pregnancy after stillbirth. Women who have experienced a stillbirth may not be aware that massage therapy is an option they can use to for support during subsequent pregnancies. Massage therapists may also not be aware of the role they can play supporting women in a pregnancy after a stillbirth. An understanding and/or knowledge about pregnancy and stillbirth are required to treat women experiencing pregnancy after loss safely and to decrease the risk of traumatization. Lower socio-economic families have twice the risk of delivering a stillborn baby(21) and these are the parents who are less likely to be able to afford massage treatment during subsequent pregnancies and who have a greater need for support.
This case study is a snapshot of a ‘real world’ experience of a woman experiencing pregnancy after a stillbirth. The results highlight potential benefits for woman experiencing pregnancy after a stillbirth and research into the role of massage to support women at this time is needed. The dissemination of this case study to bereavement health professionals and obstetric professionals might provide options for clinicians whose patients need, or are looking for, additional support in a pregnancy after stillbirth. Providing a pathway of care for women who have experienced a loss and are thinking they might like to have another child may ease some of the fear and anxiety about the types of care they would receive in future pregnancies. Stillbirth and grief are sensitive topics, and it is important that massage therapists who want to work in this area have the skills and knowledge to do so safely, as well as structure in their practice and private life to decrease the risk of compassion fatigue.
Stillbirth profoundly alters the reality of subsequent pregnancies, resulting in women experiencing extreme anxiety, heightened fear and anxiety, and isolation. A patient-centred massage treatment and consultation can provide support options for women experiencing a pregnancy after stillbirth and assist with coping during that stressful time. Increasing knowledge about the role massage may play in supporting women experiencing pregnancy after a stillbirth may ease some of the fear and anxiety about care options available to these women in future pregnancies.
The author would like to thank the amazing woman in this case study and acknowledge her generosity for allowing me to share her experience with others.
The author declares there are no conflicts of interest.
1 Australian Institute of Health & Welfare. Mothers & Babies—2018. Canberra, Australia: Australian Government, The Institute; 2018. Available from: https://www.aihw.gov.au/reports-statistics/population-groups/mothers-babies/about. Accessed 7 February 2018.
2 Australian Institute of Health & Welfare. Mothers & Babies: Stillbirths and Neonatal Deaths in Australia. Canberra, Australia: Australian Government, The Institute; 2020. Available from: https://www.aihw.gov.au/reports/mothers-babies/stillbirths-and-neonatal-deaths-in-australia/contents/overview-of-perinatal-deaths. Accessed 15 November 2020.
3 Stillbirth Foundation Australia. The Economic Impacts of Stillbirth in Australia. North Sydney, NSW: The Foundation; 2016.
4 Meaney S, Everard CM, Gallagher S, O’Donoghue K. Parents’ concerns about future pregnancy after stillbirth: a qualitative study. Health Expect. 2017;20(4):555–562.

5 Ellis A, Chebsey C, Storey C, Bradley S, Jackson S, Flenady V, et al. Systematic review to understand and improve care after stillbirth: a review of parents’ and healthcare professionals’ experiences. BMC Pregnancy Childbirth. 2016;16(1):16.
6 Turton P, Hughes P, Evans CD, Fainman D. Incidence, correlates and predictors of post-traumatic stress disorder in the pregnancy after stillbirth. Br J Psychiatry. 2001;178(6):556–560.
7 Gravensteen IK, Jacobsen EM, Sandset PM, Helgadottir LB, Rådestad I, Sandvik L, et al. Anxiety, depression and relationship satisfaction in the pregnancy following stillbirth and after the birth of a live-born baby: a prospective study. BMC Pregnancy Childbirth. 2018;18(1):41.

8 Hughes PM, Turton P, Evans CD. Stillbirth as risk factor for depression and anxiety in the subsequent pregnancy: cohort study. BMJ. 1999;318(7200):1721–1724.

9 Wojcieszek AM, Shepherd E, Middleton P, Lassi ZS, Wilson T, Murphy MM, et al. Care prior to and during subsequent pregnancies following stillbirth for improving outcomes. The Cochrane Database System Rev. 2018;12(12):CD012203.
10 Fogarty S. A role for massage after antenatal or neonatal loss: evaluations from a community program. Adv Integrat Med. 2021;8(2):129–135.
11 Hall HG, Cant R, Munk N, Carr B, Tremayne A, Weller C, et al. The effectiveness of massage for reducing pregnant women’s anxiety and depression; systematic review and meta-analysis. Midwifery. 2020;90:102818.
12 Paterson C, Thomas K, Manasse A, Cooke H, Peace G. Measure Yourself Concerns and Wellbeing (MYCaW): an individualised questionnaire for evaluating outcome in cancer support care that includes complementary therapies. Complement Ther Med. 2007;15(1):38–45.
13 Osborne C, Kolakowski M, Lobenstine D. Pre- and Perinatal Massage Therapy, 3rd ed. Pencaitland, Scotland: Handsrping Publishing; 2021.
14 Yates S. Pregnancy and Childbirth: a Holistic Approach to Massage and Bodywork, 1st ed. Edinburgh, Scotland: Churchill Livingstone; 2010.
15 Field T. Touch for socioemotional and physical well-being: a review. Development Rev. 2010;30(4): 367–383.
16 Field T, Hernandez-Reif M, Diego M, Schanberg S, Kuhn C. Cortisol decreases and serotonin and dopamine increase following massage therapy. Int J Neurosci. 2005;115(10):1397–1413.
17 Diego MA, Field T. Moderate pressure massage elicits a parasympathetic nervous system response. Int J Neurosci. 2009;119(5):630–638.
18 Edwards DJ, Young H, Curtis A, Johnston R. The immediate effect of therapeutic touch and deep touch pressure on range of motion, interoceptive accuracy and heart rate variability: a randomized controlled trial with moderation analysis. Front Integr Neurosci. 2018;12:41.

19 Evans K, Spiby H, Morrell CJ. Developing a complex intervention to support pregnant women with mild to moderate anxiety: application of the Medical Research Council framework. BMC Pregnancy Childb. 2020;20(1):777.
20 Kornhaber R, Walsh K, Duff J, Walker K. Enhancing adult therapeutic interpersonal relationships in the acute health care setting: an integrative review. J Multidiscip Healthc. 2016;9:537–546.

21 Flenady V, Wojcieszek AM, Middleton P, Ellwood D, Erwich JJ, Coory M, et al. Stillbirths: recall to action in high-income countries. The Lancet. 2016;387(10019):691–702.
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 15, NUMBER 1, March 2022