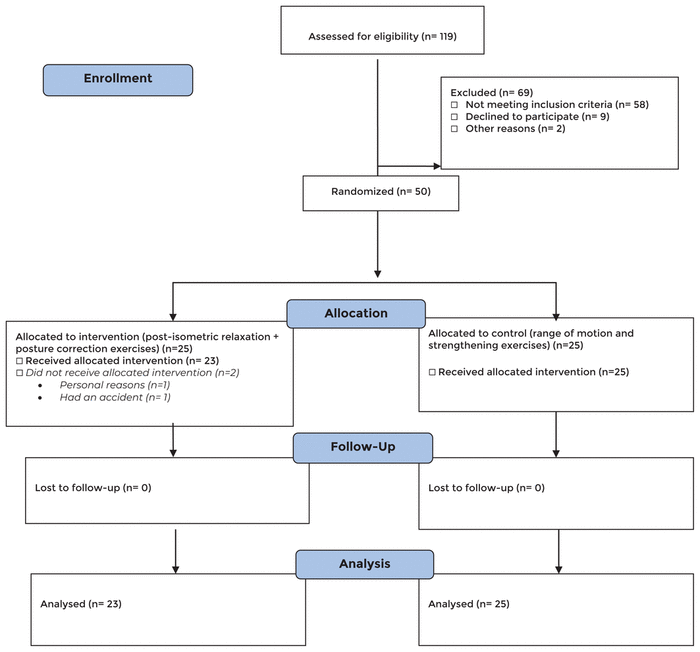
Figure 1 CONSORT flow diagram of study participants.
Reema Joshi, MPT*, Nishita Poojary, BPT
Dr. D.Y. Patil College of Physiotherapy College, Pune, India.Background
Neck pain is a common problem in individuals despite different types of working patterns. Forward head posture is a common identified cause of chronic neck pain in patients. The effect of long-term forward head posture can be loss of function which can limit individuals’ capacity to work or do activities of daily living; hence it becomes necessary to intervene with muscle strengthening to improve neck stability, as well as mobility.
Purpose
To assess effectiveness of muscle energy technique (MET) and posture correction exercises on pain and function in patients with non-specific chronic neck pain having forward head posture.
Study Setting
Outpatient department of Dr. D. Y. Patil College of Physiotherapy, Pune, India.
Participants
Both males and females between the ages of 21–60 years with a cranio-vertebral angle of less than 48° were included in study.
Research Design
A randomized clinical trial.
Methodology
MET group received muscle energy treatment + posture correction exercises, and control group receiving neck range of motion treatment. Outcomes measures were pain (Numerical Pain Rating Scale), function (Neck Disability Index), and cranio-vertebral angle (MB ruler).
Results
Forty-eight subjects were included in the analysis, with 23 participants in Group A (MET) and 25 in Group B (Control). While both groups showed within-group improvements, Group A had significantly greater decreases in neck pain (p < .001), Neck Disability Index scores (p < .001), and significantly greater improvements in cranio-vertebral angles (p < .025) compared to group B.
Conclusion
The combined effect of MET and posture correction exercises provides significantly greater results than neck range of motion treatment, and muscle energy technique should be included in the treatment of non-specific chronic neck pain in individuals with forward head posture.
KEYWORDS: non-specific chronic neck pain, forward head posture, MET
The neck is the most commonly affected site of non-traumatic musculoskeletal pain. Neck pain is defined by Mersky as pain “anywhere within the region bounded superiorly by the superior nuchal line, inferiorly by an imaginary line through the tip of first thoracic spinous process and laterally by a sagittal plane tangential to the lateral borders of the neck.”(1) The worldwide prevalence of neck pain in the adult population ranges from 16.7% to 75.5%.(2) The most common characteristics of neck dysfunction are pain, discomfort or soreness which are experienced in the area between inferior margin of the occipital bone and the T1 vertebrae.(3)
The source of symptoms in mechanical neck pain is not completely understood, but has been purported to be related to various anatomical structures, particularly zygapophyseal or vertebral joints of the cervical spine.(4) Assessment of non-specific neck pain includes the exclusion of any radiculopathy and the consideration of any prognostic factors such as old age or previous history. The confirmation or exclusion of radiculopathy can be done using a combination of the Spurling test, the traction/distraction test, and the upper limb tension test. A commonly used assessment tool for neck pain intensity and disability is the validated self-reported Neck Disability Index.
Non-specific neck pain is categorized using a grading system:(5)
GRADE 1: no signs of pathology and little or no interference with daily activities;
GRADE 2: signs of pathology and interference with daily activities;
GRADE 3: neurologic signs of nerve compression; and
GRADE 4: signs of major pathology.
A study done by Patwardhan et al.(6) in 2018 stated that chronic forward head posture (FHP) can place large stresses on the muscles and connective tissue in the cervical spine (CS) region and may be a contributing factor to non-specific neck pain.
Quek and colleagues(7) and Kim and Kim(8) reported FHP is an abnormality identified by examining the position of the head with respect to the cervical spine (CS). In FHP, the head projects anteriorly over the CS with simultaneous hyperextension of the upper CS occurring from a tilting of the head in a posterior direction. The backward rotation of the head on the CS is a compensation that enables an individual with FHP to look straight ahead instead of towards the ground.
Janda et al.(9) in their description of upper cross syndrome stated that FHP often results in movement dysfunction with some muscles such as the deep neck flexors, cervical erector spinae, lower trapezius, and rhomboids becoming underactive and other muscles becoming overactive such as the upper trapezius, levator scapula, scalene, sternocleidomastoid, and the sub occipitals which are also described by. These muscle imbalances and movement dysfunctions may have a direct effect on joint surfaces, thus causing forward head posture. Neck stabilization is used to correct posture, and helps to elongate the underactive musculature and strengthen overactive muscles.(10)
Muscle energy techniques (MET) are a class of soft tissue osteopathic manipulation methods that are directed and controlled patient-initiated isometric or isotonic contractions designed to improve musculoskeletal function and reduce pain. In post-isometric relaxation (PIR), overactive muscles are contracted isometrically for period of time, followed by relaxation for a brief latent period to allow gentle muscle lengthening. According to Chaitow,(11) MET is an active isometric contraction method, along with application of moist heat therapy, that relaxes the muscle and restores the normal blood and lymphatic circulation by altering the interstitial pressure and trans-capillary blood flow that helps in washing out the nociceptive stimulants which relieves pain. MET with PIR helps to increase muscle flexibility due to viscoelastic changes in the muscle and reduce muscle tension. Both muscle energy technique and static stretching are commonly used techniques in the field of physiotherapy. MET is an advanced stretching technique. Studies using these two techniques individually, in symptomatic as well as in asymptomatic individuals, have shown improvement, but fewer studies have compared these techniques in a symptomatic population, where conflicting results are seen.(12)
In this study, muscle energy technique was administered to the overactive muscles along with posture correction exercises, including chin tuck, scapular bracing, and pectoral stretching, to determine the effect in individuals with non-specific neck pain with forward head posture. The aim of the study is to assess the effectiveness of the combined effect of muscle energy techniques and posture correction among individuals with non-specific neck pain.
The study uses a randomized clinical trial study methodology, see Figure 1.
|
| ||
|
Figure 1 CONSORT flow diagram of study participants. | ||
This study was approved by the institutional sub-ethical committee of Dr. D.Y. Patil Vidyapeeth, Pune DYPCPT/ISEC/48/2019.
The treatments were given at the outpatient department of Dr. D.Y. Patil College of Physiotherapy, the Dr. D.Y. Patil Medical College Hospital and Research Institute outpatient department, and the Dr. D.Y. Patil Ayurveda Hospital outpatient department, Pimpri, Pune.
Sample size was calculated using statistical software Primer Version No. 7 (PRIMER-e, Auckland, NZ). Assuming 1.1 as the effect size, with an α-error of 0.05 and power of 0.8, the sample size was 25 in each group.
Eligible participants included males and females between the ages of 21 and 60 years with a cranio-vertebral angle of less than 48°. Subjects with recent cervical spine fracture, radiculopathy in the upper extremity, neck pain with headaches, serious pathology, malignancy, osteoporosis, and disc prolapses were excluded from the study.
Recruitment took place between October 2019 and December 2020 when patients attended the Outpatient Department Dr. D. Y. Patil College of Physiotherapy, Pune. Patients were screened on a regular basis and every second patient who met with the study criteria was invited to participate in the study. The rationale for inviting every second participant was to give an equal chance for participation in the study. The potential participants were informed about the study benefits, risks, and procedures in a regional language that was best understood by them (Hindi or Marathi). Those who consented to participate were randomized into two groups, using a simple lottery random sampling method: Group A (experimental group) and Group B (conventional treatment group/Control group). The second researcher (NP) undertook all the study treatments and assessment according to the study protocols. The primary investigator (RJ) undertook the analysis and was blind to the study group allocation.
Outcomes measures were undertaken pre-treatment and three weeks post-treatment. Primary outcome measures were pain intensity measured by a Numerical Pain Rating Scale (NPRS), and impact of neck pain on the ability to manage in everyday life which was measured by the Neck Disability Index (NDI). Craniovertebral angle (CVA), measured using a MB ruler, was used to assess cervical neck posture.
The NPRS is a subjective pain rating scale using an 11-point scale from 0 to 10, where 0 means ‘no pain’ and 10 means ‘intolerable pain’. Participants select the whole number that best represents their level of pain.
The NDI is a self-reported questionnaire which is formulated to assess pain that restricts the activities of daily living (ADL); it also helps to determine self-assessed disability. NDI has 10 domains covering pain intensity, personal care, lifting, reading, headaches, concentration, work, driving, sleeping, and recreation. Scores range from 0 to 50, with 50 being the greatest levels of dysfunction.
The CVA is measured via drawing an imaginary horizontal line through the C7 spinous process and a line joining the spinous process of C7 vertebra with the tragus of the ear. The Markus Bader ruler (MB ruler) is computer-based objective tool that measure angles and distances. Reflective markers were placed on participants anatomical landmarks and a photograph was taken. The photograph was uploaded to a computer and the MB ruler software was used to calculate the CVA.
The study involved an experimental group (Group A), which received muscle energy treatment + posture correction exercises, and a Control group (Group B), which received neck range of motion treatment.
Treatment consisted of a muscle energy technique called post-isometric relaxation (PIR) and posture correction exercises. These techniques were applied to the suboccipital area. In the PIR portion of the treatment, the patient was asked to apply approximately 20% of his strength to protract the shoulder girdle in supine position or asked to match the therapist’s strength. This isometric contraction was maintained for a period of 7 seconds while holding the breath and then the patient was asked to relax and exhale. During the period of relaxation, the therapist stretched the pectoralis minor muscle to its new length and the stretch force was maintained for a period of 10 seconds. The procedure was repeated for a minimum three times per session for a period of three weeks. MET was followed by posture correction exercises which includes chin tuck exercises and scapular bracing pectoral stretch.
Patients received a conventional exercise programme which included strengthening exercises for deep neck flexors, rhomboids, lower trapezius, and serratus anterior because they are weak muscles in the upper crossed syndrome (two sets of 10 repetitions once a day) and stretching exercises for pectoralis muscles (20-second hold with five repetitions each). Each exercise was repeated for a total of 10 times.
Data analysis and interpretation was done using the free online statistical package WinPepi (version 11.65; http://www.brixtonhealth.com/pepi4windows.html) and Primer of Biostatistics version 7.(13) Normality of the data was checked using Shapiro-Wilk Test in WinPepi software and was concluded as normally distributed if p > .05 or not normally distributed if p ≤ .05. Then the pre- and post-reading of each outcome was compared with respective outcome of other group. If the data were normally distributed, the intra-group comparison used an unpaired t-test and the inter-group comparison used a paired t-test. The significance level was set at p ≤ .05 and a 95% CI.
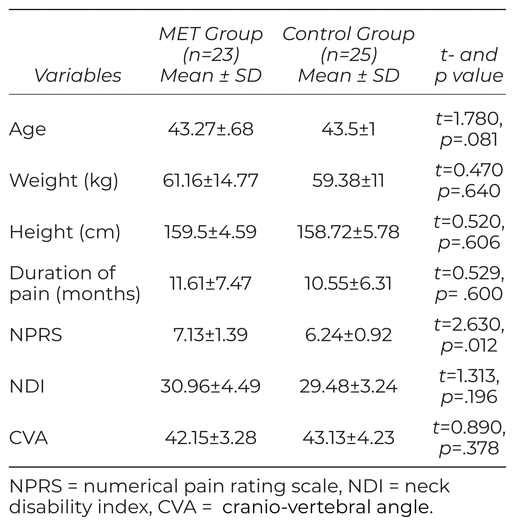
One hundred and nineteen individuals were assessed for eligibility, with 50 individuals meeting the criteria to participate (see Figure 1). Two participants from MET group withdrew prior to receiving any treatment; 48 participants completed the study. The MET group had 23 subjects and the Control group had 25 subjects for statistical analysis. The demographic characteristics for both groups compared using t-test was not statistically significant for age (p = .081), height (p = .606), weight (p = .640), and duration of pain (p = .600). Baseline characteristics were assessed for neck pain, function, and posture using NDI and CVA and were not significantly different at baseline, but NPRS was significantly greater for those in the MET group (p = .012) as presented in Table 1.
Table 1 Baseline Characteristics of the Participants in Both Treatment Groups
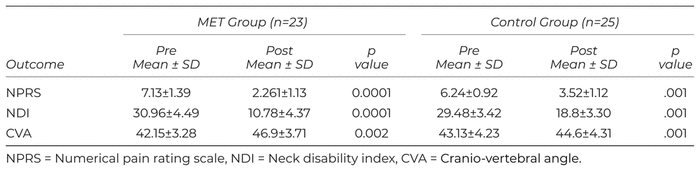
Neck pain decreased significantly pretreatment to post-treatment for both groups (MET group 7.12 to 2.28 and Control group 6.24 to 3.52; p ≤ .05 for both groups). The Neck Disability Index scores decreased significantly pre-treatment to post-treatment for both groups (MET group 30.96 to 10.78 and Control group 29.48 to 18.8; p ≤ .05 for both groups). The cranio-vertebral angle (CVA) improved significantly pre-treatment to post-treatment for MET group (MET group 42.15 to 46.9; p ≤ .02 and Control group 43.13 to 44.6; p = 0.001 (Table 2).
Table 2 Within-Group Change in Outcome Measures for Both ET and Control Groups Using Dependent t-Test
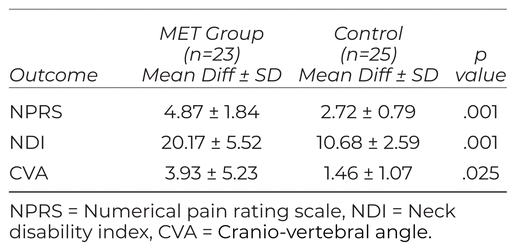
MET group had a significantly greater decrease in neck pain compared to Control group (MET group 4.87 decrease vs. Control group 2.72 decrease; p ≤ .001) (Table 3). MET treatment showed a significantly greater decrease in Neck Disability Index scores compared to Control group (MET group 20.17 decrease vs. Control group 10.68 decrease; p ≤ .001). MET also showed an improvement in cranio-vertebral angles compared to Control group, with a statistically significance of p = .025 (MET group 3.93° improvement vs. Control group 1.46° improvement; Table 3).
Table 3 Between-Group Comparison of Pre-Post Mean Differences (± SD) Between MET and Control Groups Using Independent t-Test
The study was intended to assess the effect of muscle energy technique using PIR and posture correction exercises to alleviate neck pain and enhance function in comparison to a conventional treatment protocol. To avoid selection bias, subjects were allocated into two groups by computerised randomization technique. Baseline characteristics were not statistically different between groups for anthropometric variables or for NDI or CVA, but NPRS was statistically higher in the MET group, which could mark an error in randomization. On comparison, both groups showed significant improvement in NPRS after receiving their respective treatments. MET reduced pain perception by increasing the stretch tolerance; those who received the muscle energy technique (post-isometric relaxation) and posture correction exercises had decreased pain and neck disability, along with greater improvement of their craniovertebral angle compared to the Control group. Table 2 summarizes the effect of MET on patients with non-specific neck pain typically presenting with alterations in cervical proprioception and postural stability. Many studies explain the efficacy of manual therapy and therapeutic exercise for pain reduction and cervical disability.(14,15,16)
Both groups had significant decrease in pain, but the muscle energy technique (post-isometric relaxation) with posture correction exercises group demonstrated significantly better results than those receiving conventional exercises. This could be due to the isometric contraction of the muscles which stimulates the muscle and joint mechanoreceptors and proprioceptors which, in turn, reduces the sensation of pain, making the consecutive stretch easier and more tolerable.
The results of the present study obtained for pain reduction in the MET group is similar to the previous studies where pain intensity was found to be reduced following MET over the neck area. The mechanism behind this MET application to the sub-occipital muscles is that it helps to decrease hyper activation and tightness of the shortened muscles via the neurophysiological mechanism activated by the Golgi tendon reflex which inhibits the alpha motor neuron and results in reflex relaxation of muscles and decreases pain. Results of this study help to draw attention to postural input, which also helps in correction of forward head posture among the individuals with non-specific neck pain in comparison to static stretching.(17,18,19)
A study by Gupta et al.(12) on the effects of post-isometric relaxation versus isometric exercises in non-specific neck pain also concluded that MET showed a significant improvement in pain and functional status. Our results for Group A are also supported by a study by Abha and Angusamy(20) which compared postisometric relaxation with an integrated neuromuscular inhibition technique on the upper trapezius trigger points and concluded that MET is effective in improving pain and functional status. Results of a study by Sharmila(21) on the effects of MET versus conventional exercises in non-specific neck pain in secondary school teachers are in accordance with our results for MET group, which concluded that post-isometric relaxation had better reductions in pain and disability. Muscle energy technique combined with posture correction exercise helps to improve posture by recruiting muscles and stimulating the muscle and joint mechanoreceptors and proprioceptors, as well as giving positive feedback to the spinal musculature to maintain erect position; thus the results mentioned in Table 3 helps to provide evidence that MET with posture correction exercise can be considered together in the treatment of non-specific neck pain to improve neck disability over conventional exercises.
The therapist-guided neck range of motion group was observed to have significant within-group decreases in pain. According to a study published by EI Laithy and Fouda,(22) the mechanism behind the reducing in pain for this group is that the isometric neck exercises cause the activation of the muscle stretch receptors which occur during strong isometric contraction of muscle and this leads to the release of beta endorphins from the pituitary gland, thereby decreasing the pain. This hypothesis is supported by research study by Rupesh et al.(23) on the effects of sitting posture modification and exercises in school going children with neck pain in a rural area where subjects were given sitting posture modification, isometric neck exercises, and home exercises and were a reduction in pain and neck disability after posture correction exercises was observed.
The small sample size, which leads to reduced statistical power, was a limitation. Long-term effects of the treatment were not studied because of loss of follow-up. The study groups were not matched for age and gender. The outcome assessor was not blinded, which might have led to measurement bias.
The present study concluded that both MET and conventional treatments are effective in relieving pain and reducing disability in patients with non-specific neck pain. However, muscle energy technique and posture correction exercises have shown a statistically significant improvement in pain and functional status in patients with non-specific chronic neck pain having forward head posture compared to the conventional treatment group. Thus, MET is recommended over conventional treatment when treating patients with non-specific chronic neck pain having forward head posture.
We thank our institute for providing all support during the study. We also extend warm regards to Dr Sarah Fogarty, PhD, for her valuable guidance in process of scientific manuscript writing. This study is a self-funded project.
The authors declare there are no conflicts of interest.
1 Treede RD, Rief W, Barke A, Aziz Q, Bennett MI, Benoliel R, et al. A classification of chronic pain for ICD-11. Pain. 2015;156(6):1003–1007.


2 Fejer R, Kyvik KO, Hartvigsen J. The prevalence of neck pain in the world population: a systematic critical review of the literature. Eur Spine J. 2006;15(6):834–848.

3 Genebra CV, Maciel NM, Bento TP, Simeão SF, De Vitta A. Prevalence and factors associated with neck pain: a population based study. Brazil J Phys Ther. 2017;21(4):274–80

4 Cavanaugh JM, Lu Y, Chen C, Kallakuri S. Pain generation in lumbar and cervical facet joints. J Bone Joint Surg Am. 2006;88(Suppl 2):63–67. doi:10.2106/JBJS.E.01411
5 Tsakitzidis G. Remmen R, Peremans L, Van Royen P, Duchesnes C, Paulus D, et al. Nonspecific Neck Pain: Diagnosis and Treatment. KCE Reports 119C. Brussels: Belgian Health Care Knowledge Centre (KCE); 2009.
6 Patwardhan AG, Havey RM, Khayatzadeh S, Muriuki MG, Voronov LI, Carandang G, et al. Postural consequences of cervical sagittal imbalance: a novel laboratory model. Spine. 2015;40(11): 783–792.

7 Quek J, Pua YH, Clark RA, Bryant AL. Effects of thoracic kyphosis and forward head posture on cervical range of motion in older adults. Man Therap. 2013;18(1):65–71.

8 Kim EK, Kim JS. Correlation between rounded shoulder posture neck, disability indices, and degree of forward head posture. J Phys Ther Sci. 2016;28(10):2929–32.


9 Janda V. Muscles and motor control in cervicogenic disorders. In: Grant R, ed. Physical Therapy of the Cervical and Thoracic Spine. New York: Churchill Livingstone; 1988. p.182–199.
10 Singla D, Veqar Z. Association between forward head, rounded shoulders and increased thoracic kyphosis: a review of the literature. J Chiropract Med. 2017;16(3):220–29.

11 Chaitow L. Muscle Energy Techniques, 3rd ed. Edinburgh: Churchill Livingstone; 2008. p. 59, 125, 128, 176–80, 185–87.
12 Gupta S, Jaiswal P, Chhabra D. A comparative study between post isometric relaxation and isometric exercises in nonspecific neck pain. J Exerc Sci Physiother. 2008;4(2):88–94.
13 Glantz, ST. Primer of Biostatistics, 7th ed. New York: McGraw Hill Medical; 2012.
14 Vincent K, Maigne J, Fischhoff C, Lanlo O, Dagenais S. Systematic review of manual therapies for nonspecific neck pain. Joint Bone Spine. 2013;80(5):508–15.

15 Gross AR, Paquin JP, Dupont G, Blanchette S, Lalonde P, Cristie T, et al. Exercises for mechanical neck disorders: a Cochrane review update. Man Ther. 2016;24:25–45.

16 Miller J, Gross A, D’Sylva J, Burnie SJ, Goldsmith CH, Graham N, et al. Manual therapy and exercise for neck pain: a systematic review. Man Ther. 2010;15(4):334–54.

17 Contractor ES, Shah S, Dave P. To study the immediate effect of suboccipital muscle energy technique on craniovertebral angle and cranihorizontal angle on subjects with forward head posture. Int J Health Sci Res. 2019;9(3):83.
18 Fathollahnejad K, Letafatkar A, Hadadnezhad M. The effect of manual therapy and stabilizing exercises on forward head and rounded shoulder postures: a six-week intervention with one-month follow-up study. BMC Musculoskelet Disord. 2019;20(1):1–8.

19 Lynch S, Thigpen CA, Mihalik JP, Prentice WE, Padua D. Forward head and rounded shoulder postures in elite swimmers. The effects of an exercise intervention on forward head and rounded shoulder postures in elite swimmers. Br J Sports Med. 2010;44:376–81.

20 Abha S, Angusamy R. Efficacy of post-isometric relaxation versus integrated neuromuscular ischemic technique in the treatment of upper trapezius trigger points. Ind J Physiother Occup Ther. 2010;4:1e5.
21 Sharmila, B. Isometric muscle energy technique and non-specific neck pain in secondary school teachers—results of an experimental study. Ind J Physiother Occup Ther. 2014;8(2):58–62.

22 El Laithy M, Fouda KZ. Effect of post isometric relaxation technique in the treatment of mechanical neck pain. Phys Ther Rehabil. 2018;5:20.

23 Rupesh P, Malarvilzhi D, Prasanth D, Sivakumar VP. Effects of sitting modification and exercises in school going children with neck pain in rural area in Tamil Nadu. Int J Clin Skills. 2016;10(2):22–25

Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 15, NUMBER 2, May 2022