Massage Therapy Effectiveness in Rehabilitation on Humeral Shaft Fracture in a Child: A Case Study
Hélène
Geoffroy-Legeay
,
BTSM, RMT
Department of Massage, Southern Institute of Technology, Invercargill 9810, New Zealand.
Objectives
This case report aimed to explore the process and outcomes of a seven-week massage therapy treatment on post-surgical intervention to reduce humeral shaft fracture.
Participant
An active 9-year-old girl who recently moved in the region and who underwent two surgeries following a humeral fracture with displacement after a fall at school.
Intervention
The treatment used various techniques such as manual lymphatic drainage (MLD), myofascial release (MFR), therapeutic massage, and neuromuscular techniques (NMT) in conjunction with the physiotherapist rehabilitation programme to help the client recover both physically and emotionally from the trauma. Evaluation of the outcome measures (OM) took place throughout the study and after the four-week interim that followed the intervention period.
Results
The massage therapy intervention indicated improvement regarding range of motion (ROM) and muscular strength. The clients’ progress using the Patient-Specific Functional Scale (PSFS) indicated a gradual evolution to reach almost a 95% gain, and the Upper Extremity Function Index (UEFI) also showed improvement in everyday activities with a 21.5% positive change. The Child Outcome Rating Scale (CORS) and subsequent Child Session Rating Scale (CSRS) monitored therapeutic progress and indicated improvement on biopsychosocial (BPS) aspects throughout the treatment.
Conclusion
The client felt strong and more confident after each massage intervention. A combination of techniques and the child’s empowerment positively affected the client’s overall wellness and confidence to return to activities.
KEYWORDS: child, humeral fracture, massage, rehabilitation
INTRODUCTION
Musculoskeletal conditions and injuries are common throughout one’s lifetime and represent the most significant need for rehabilitation globally.(1) Fracture with a displacement of the bone appears in 20% of fracture cases, and Open Reduction and Internal Fixation (ORIF) surgeries are needed to secure the bone in position.(2) The World Health Organisation noted in 2019 that “between one in three and one in five people (including children) live with a musculoskeletal pain condition.”(1) Nearly 20% of children who present with an injury have a fracture, with an estimated 27% of girls sustaining a fracture during childhood.(3) Fractures occur more often in the paediatric age group than in adults; however, proximal humeral fracture (PHF) is relatively uncommon in children.(2,4)
In New Zealand, the 2016 provisional number of injuries estimated that 194 children under the age of 15 suffered from serious (fatal and non-fatal) fall injuries; falls and motor vehicle crashes are the most frequent causes of fractures.(4,5)
This case study will explore the effects of massage therapy on a child diagnosed with a humeral shaft fracture resulting f rom trauma, presenting with limited range of motion (ROM) and muscle weakness in her left arm. To see the effectiveness of massage therapy post-surgery, the therapist has performed seven 45-minute interventions. The study started with an initial assessment before the hands-on treatment began and ended with a follow-up session four weeks after the final massage therapy intervention.
METHODS
Client Information
The client is a right-handed, 9-year-old girl. Both she and her parents describe herself as having excellent general health. The client is active and usually spends about five hours a week doing various physical activities and helping her parents at home.
In January 2020, she moved from another region before the school year started. She socialised rapidly, and almost started a new activity when the country entered lockdown due to the Covid-19 pandemic.
In May, she fell off the top of a jungle gym, head, and shoulder first. The diagnosis was metaphyseal-diaphyseal fracture with displacement of the left humerus, her non-dominant side. After two surgeries, no further surgical intervention is expected as she ages.
She has never experienced massage therapy before but has received hands-on treatment from a physiotherapist as part of the post-surgery rehabilitation programme. She also mentioned suffering from mild contact eczema.
Clinical Findings
The client was no longer complaining about pain; however, weakness in isometric resisted tests at the glenohumeral joint (GHJ), and tissue stiffness resulting from the surgeries, resulted in reduced active and passive ROM in the left shoulder area (Table 1). The massage therapist used the Defense and Veteran Pain Rating Scale (DVPRS®; The Defense and Veterans Center for Integrative Pain Management, School of Medicine, Uniformed Services University, Bethesda, MD) to identify the progression of pain since the injury and to assess the state of mind of the young client. The client stated her pain was maximal at the time of injury, and described the pain as achy radiating on the entire anterior left arm. After the two surgeries, the pain had gone completely. Continuing with the DVPRS® supplemental questions, the client mentioned being affected by mood, and activities such as putting her jacket on, running, and having trouble writing in class even though she is right-handed (Figure 1). The child and her parents did not mention any predisposing factors about the case.
| |
|
|
|
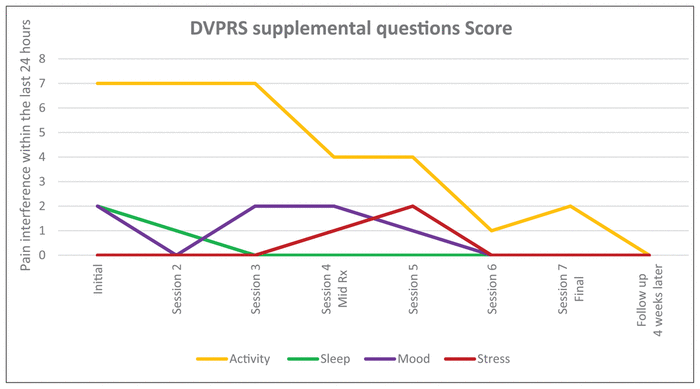
Figure 1
Defense Veteran Pain Rating Scale supplemental questions screening throughout massage therapy interventions and follow-up session. No pain/discomfort is indicated with a 0 on the scale up to 10, where the worst pain/discomfort possible is felt. Rx stands for treatment.
|
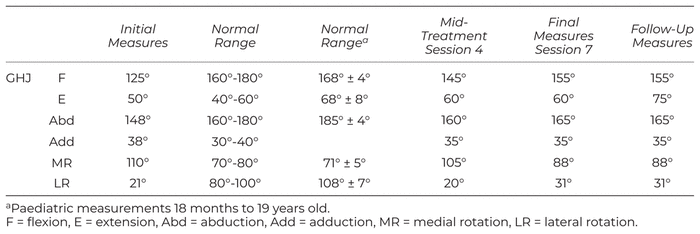
Table 1
Shoulder Joint Goniometry: Active Range of Motion (29,30)
The ROM tests performed at the GHJ, elbow joint, and scapula indicated compensatory patterns. Isometric resisted tests indicated weaknesses at the GHJ in all planes but in extension, and weaknesses in protraction and retraction at the scapula. The physiotherapy exercises noted in Table 2 corroborated these findings. Numbness and tingling were also present in posterior and anterior aspects of the hand, a typical clinical presentation after trauma to the shoulder.(6) However, an assessment for nerve pathologies was performed. The upper limb neurodynamic test of the median nerve, done passively with the shoulder instability technique, showed nerve pain when shoulder was laterally rotated, and forearm supinated. The upper limb neurodynamic test of the radial nerve, done passively, showed nerve pathology when shoulder medially rotated, and forearm pronated (see Table 3).(7)
Table 2
Physiotherapy Rehabilitation Exercises

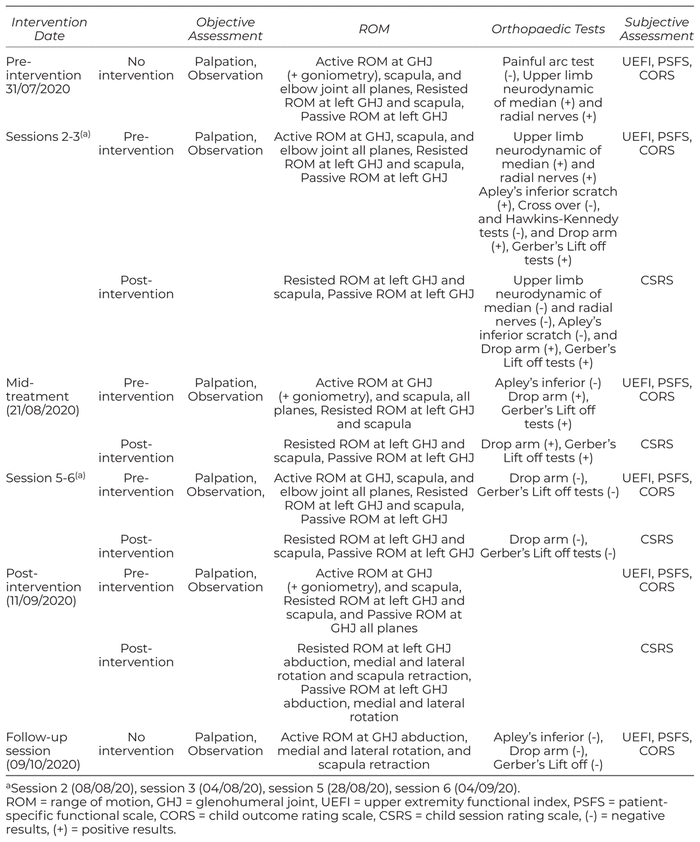
Table 3
Assessment for the Massage Therapy Intervention
Bilateral palpation showed various points of tightness and tenderness on the client’s left arm, left upper chest, and neck (Table 3). Nothing has been found on the client’s dominant side. Interestingly, pain appeared only during palpation, which indicated presence of latent myofascial trigger points.(8)
The child’s skin colour and temperature were standard bilaterally. There were presence of light swelling, redness, and irregular contour of the scars, especially at the site of the humeral shaft. The child also presented with eczema patches located away from the site of injury.
A physical assessment noted some observations about postural behaviour, with bilateral elevation of shoulders, increased lordosis, and kyphosis, and anteriorly rotated left GHJ.
The client presented with no pain and the DVPRS® assessment tool showed only significant impact on the activity aspect (Figure 1). The therapist identified areas of weakness, and reduced ROM at the GHJ, elbow joint, and at the scapular level.
Orthopaedic testing of the client’s ability to perform movements and assessing the possibility of glenohumeral pathologies came back negative.(9,10) However, the Drop Arm test was positive indicating a possible supraspinatus tear. It could also show myofascial trigger point referrals limiting the child to hold the arm in the abducted position; however, the child was able to sustain the abducted position with the Full Can test. The Gerber’s Lift-Off sign indicated weakness for the subscapularis tendon, the child being unable to resist the therapist’s pressure by extending the elbow. Also, the Apley’s inferior scratch test indicated limitations in shoulder medial rotation and adduction and highlighted a winging scapula.(7)
Thus, a treatment plan for rehabilitation following left PHF was sought, focusing on reducing the compensating pattern imposed on the scapula and helping increase the ROM at the GHJ. Having the young client’s full attention throughout the entire intervention determined the massage treatment choices and the duration of sessions.(9,11)
Informed Consent
The child and her parents received information about the case study and gave informed consent to participate. It provided a detailed explanation of what a massage intervention entails, how pressure is used, and how different techniques can be applied. A parent attended all interventions.(11)
Practitioner Descriptor
The practitioner is a qualified remedial massage therapist who qualified in 2019. She continues professional development pursuing studies to obtain a bachelor’s degree in therapeutic and sports massage. The qualifications programme and additional training covered the techniques used. Although the therapist has previous experiences in sports and remedial massage treatments with many people, this is the first experience with a child.
Therapeutic Intervention
The massage intervention happened 19 days after the sling was no longer necessary, and the massage practitioner had received the physiotherapist consent to participate in the child’s rehabilitation.(12)
The massage therapist was aware of the physiotherapy treatments, and the strengthening exercises prescribed (Table 2). The physiotherapist was not involved in the decision-making regarding the massage therapy intervention; however, the massage intervention was designed not to impact or interfere with the physiotherapist’s interventions, and considered the evolution of the strengthening exercises prescribed (Table 2).
The initial session aimed to discuss the purpose of the massage intervention and the treatment plan. It also included a thorough explanation regarding the findings and the results from the outcome measurement (OM) tools: Patient-Specific Functional Scale (PSFS), Upper Extremity Function Index (UEFI) adapted to the client’s age, and Child Outcome Rating Scale (CORS) to capture therapeutic progress and the client’s state of mind (Table 3).
Treatment consisting of seven sessions of 45 minutes each has included OM tools to aid in tracking progress, along with the Child Session Rating Scale (CSRS) to assess the client-therapist relationship (Table 3). Through the treatment, techniques have evolved to follow assessments findings, including study of the physiotherapy exercises prescriptions which evolved overtime to build strength (Table 2). The treatment also considered tissue changes, from the client’s responses to previous massage sessions, and the client’s confidence and trust gained through the massage experience with the therapist. The client adopted a seated position in sessions 2 and 3 to manage the stress related to her first experience with massage therapy, and gave consent for the treatment to continue using the massage table once she felt more comfortable (Table 4). There was a minimum five-day interval between massage therapy sessions to allow for tissues to heal and adapt to the treatment in conjunction with physiotherapy work.(9,11)
Table 4
Treatment Plan

RESULTS
Treatment Outcomes
The treatment has helped in the process of muscle balance awareness and coordination, especially at the scapular level.
The treatment relieved the child from the neural discomfort mid-intervention. The intervention benefits appeared to plateau regarding the active range of motion at the GHJ even though there were continuous postural adjustments throughout the sessions (Table 3). The passive ROM improved dramatically, with only signs of apprehension in GHJ medial rotation. The resisted isometric ROM progressed, but weakness was present in GHJ abduction, and GHJ medial and lateral rotation.
The Drop Arm, Apley’s inferior and Gerber’s lift off tests improved with time; however, a sign of a winging scapula persisted.
The scars’ shapes and colour evolved positively in both humeral shaft and anatomic neck of humerus areas.
Follow-Up & Outcomes
Four weeks post-massage therapy intervention, the new measurements taken at the GHJ indicated improved active ROM on extension (Table 1). The passive and resisted isometric ROM evolved positively; however, some neck and scapular adaptations appeared during GHJ abduction and medial rotation.
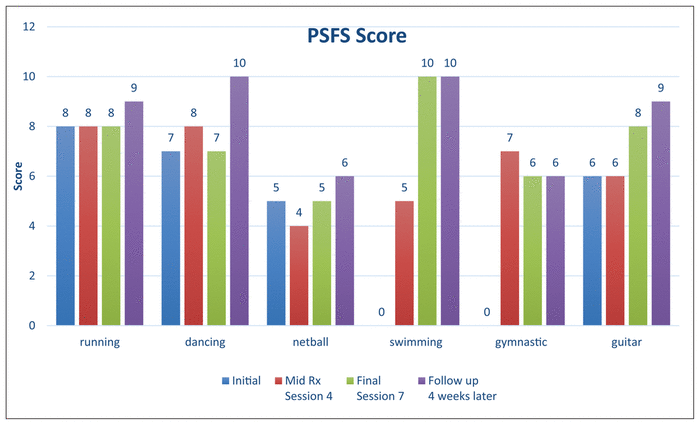
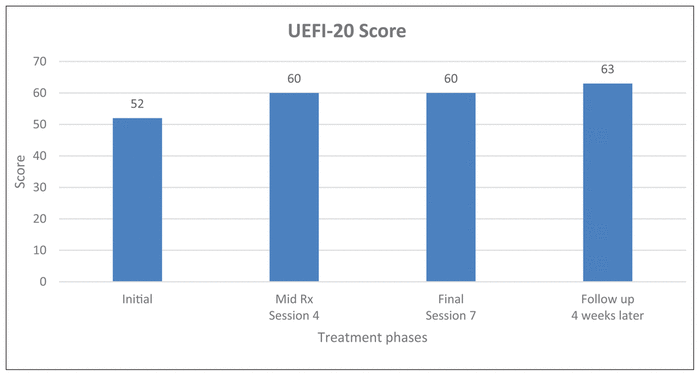
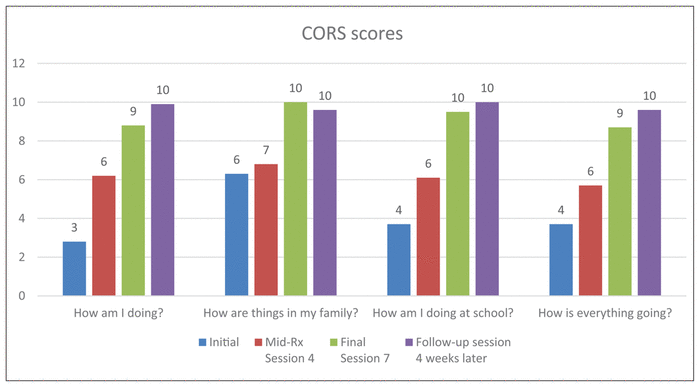
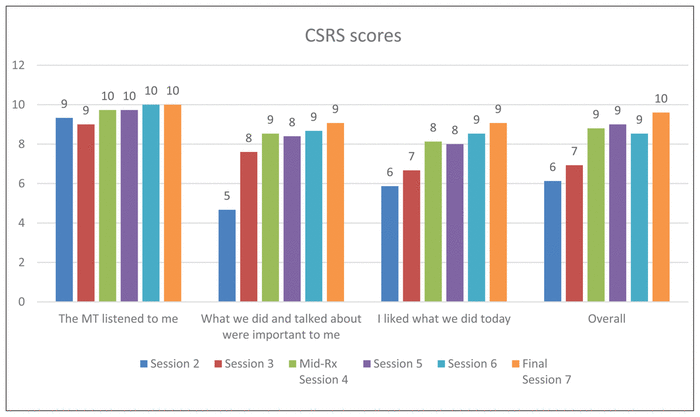
The PSFS showed an increase in the client’s perception of her ability to go back to activities by 93% (Figure 2). The UEFI (adapted) score of the client’s overall ability to perform usual activities of daily living (ADL) increased from 52 to 63 (scale up to 68 to correlate client’s age), which equates to a 21.1% increase (Figure 3). Four weeks post-intervention, the client reported no pain and no change regarding the impact of the shoulder rehabilitation in the mood, sleep, and stress aspects of the DVPRS® biopsychosocial (BPS) questions since the last massage treatment. However, the child-specific OM, CORS, and CSRS indicated an improvement from the initial session and highlighted benefits after each session (Figure 4, Figure 5).
| |
|
|
|
Figure 2
Patient-Specific Functional Scale (PSFS) progress throughout massage therapy interventions and follow-up session. The higher the score the easier to perform activity at the same level than before injury (scale up to 10).
|
| |
|
|
|
Figure 3
Upper Extremity Functional Index (UEFI-20) improvement (score=68). The greater the score the higher the functional status. UEFI adapted to child’s activity of daily living (ADL).
|
| |
|
|
|
Figure 4
Child Outcome Rating Scale (CORS): Wellbeing self-assessment. The greater the score the better the state of mind.
|
| |
|
|
|
Figure 5
Child Session Rating Scale (CSRS): How was our time together today? The greater the score the better the experience. MT stands for massage therapist.
|
The parents also saw progress in the child’s sleep pattern and confidence regained in playing again.
DISCUSSION
A PHF typically happens after a fall, followed by pain in the related arm or shoulder in children. About 5% of all fractures are humeral shaft fractures.(13) Despite humeral shaft fractures occurring in all age groups, researchers identified a bi-modal distribution in children with humeral shaft fractures primarily occurring in children younger than three or older than twelve.(13,14) The client, who was a 9-year-old, represented an exception to the latter. However, the client presented with a mechanism of injury and a PHF, representing 30% of cases in this site of injury.(13) The rehabilitation programme, including massage therapy intervention, should be done carefully and as soon as possible to avoid potential disturbance on the developing skeleton even if the children often respond well to treatment and make a remarkable recovery.(4,11)
A Child Is Different
There are significant differences in the type of injuries sustained by children compared to adults.(15,16) These are due to the physiology of growing bone that is less stable and manages to bow rather than break in response to trauma, leading to fracture types not seen in adults.(4,13) Even though the child bones are not yet fused or ossified, the massage intervention is not much different from providing massage for adults.(9) The therapist employed a gentle approach to reduce stress from being touched on the trauma’s site, and to develop connection and trust with the young client.
The clinical approach to the child will require greater attention on first establishing rapport with the child.(15) The feeling of empowerment is beneficial for the recovery process. The treatment may therefore be more valuable, as the therapist addressed the questions directly to the young client with comprehensive vocabulary and later clarified any point with the parents especially considering the child was receiving her first massage.(17,18)
The therapist decided on a 45-minute appointment to keep the child’s attention.(9,11) However, the client was encouraged in the recovery process to be motivated to return to play. The child’s willingness to participate in the case also presented an advantage in the rapid evolution of the recovery.(19)
The hands-on intervention considered the age of the client entering a transitional phase to puberty, dealing with emotions and physical changes. The therapist used a draping method not different from that used with an adult.(9)
Skin
The progressive approach of techniques used allowed the therapist to address the physical discomfort related to the injury and tackle skin sensitivity issues the child may have had. Massage interventions were performed outside the areas of eczema to prevent aggravation of contact dermatitis.
(20)
The choice of lubricant helps lower the chance of skin irritation, and the risk of absorption of toxic agents is influenced largely by the barrier properties of the child’s skin.(21) The therapist used a natural beeswax to minimize contamination from allergens, and to allow a better drag and a firmer grip for the remedial work.
Assessments & Results
The fracture has impacted the surrounding soft tissues, involving imbalanced patterns. A rehabilitation done appropriately should correct the compensations and increase coordination of muscles’ activation around the joint.(11,22) Even though the pain was no longer a factor, the physical assessment indicated the main muscles at the GHJ and neck were involved in the compensating patterns. Other muscles were identified as problematic due to the postural adaptation to protect her arm while wearing the sling. The ROM did plateau with minimal change at lateral rotation, but there was a significant improvement on the GHJ extension. Passive ROM did not indicate a joint restriction of the GHJ, but some limitations in the quality and the quantity of movement augmented with signs of apprehension particularly in the sagittal plane. The resisted isometric ROM improved, but there were some postural adaptations involving the neck and scapula. Thus, maintaining a strengthening programme of the shoulder girdle which follows the child’s progress seems inevitable to correct the new posture adopted in addition to increasing ROM.(12)
The DVPRS® showed some limitations regarding the client’s absence of pain and very slight BPS disturbances. Nevertheless, the use of the CORS and CSRS allowed integration of a deeper understanding of the BPS issues with an adapted language for the client age, giving enough information on the course and the results of the sessions.(23,24) The child sometimes had difficulties with concentration during assessments and wanted to receive massage as soon as possible; this could reflect the scores in the CSRS. The UEFI assessment tool presented challenges because of its design to assess the client’s dominant hand and items related to adults’ ADL; thus, the UEFI scale was reduced from 80 to 68 items to correlate with the client’s age. The PSFS has excellent validity; the tool was easy to conduct and indicated to the child the progress made.(25,26) After the study, the young client felt more confident and fearless in her short-term return to play.
Techniques
The therapist chose at first to use manual lymphatic drainage (MLD) to approach the child within the new massage therapy environment, and reduce swelling and promote bone regrowth.(9,27) It had been an effective technique initially; however, it was of limited use in the remaining treatment sessions. The myofascial release technique (MFR) had shown positive outcomes regarding the scars’ adhesion, the improved range at GHJ, and the gentle touch to build up a trust relationship with the young client.(9,11) MLD and MFR techniques were both appropriate for addressing the young client’s discomfort, preventing fear of touch at the shoulder, and did not present any contraindication to the case.(11) Later in the treatment, the therapist incorporated neuromuscular techniques (NMT) to correct future imbalances, especially around the neck area and at the anterior aspect of the chest.(9,28)
While the implementation of the physiotherapy exercises showed improvements in ROM by strengthening, massage therapy delivered ease of movement by relaxing and lengthening the muscles and minimize scar adhesions from the surgeries.(9) Massage intervention allowed the tissue to be more pliable from tissue being hypertonic from a shortened position with the immobilization, and the strengthening exercises resulted in a more effective rehabilitation programme than physiotherapy as a unique intervention.
Client Perspective
It was complicated to gain a clear answer from the client. Her parents and the CORS measurements tool exposed the actual benefits of the treatment. The future looks promising, since children heal faster than adults and their bodies have not yet reached their full development. Considering the voluntary participation and application to her recovery, the client has a limited chance of significant issues related to the humeral fracture.
CONCLUSION
This case study looked at the effectiveness of massage therapy for the rehabilitation of a 9-year-old girl with a humeral shaft fracture after a fall. The progression of discomfort with daily and sporting activities, sleep patterns, and the positive increase in ROM at the GHJ justified that massage therapy was beneficial when used in conjunction with physiotherapy intervention. Additionally, the massage therapy experience and assessment tools indicated improvement in the biopsychosocial aspects of the client’s life and her empowerment in the rehabilitation process.
ACKNOWLEDGMENTS
Thanks to Dr Joanna Smith, programme manager and tutor, for encouraging me to having a go at publishing the case report and her confidence in doing so, and to my young client and her parents for their participation and trust in conducting the study.
CONFLICT OF INTEREST NOTIFICATION
The author declares there are no conflicts of interest.
REFERENCES
1 World Health Organization. Musculoskeletal conditions [fact sheet]. Geneva: World Health Organization. Published November 26, 2019. Accessed September 3, 2020. https://www.who.int/news-room/fact-sheets/detail/musculoskeletal-conditions
2 Byram I. Treating a proximal humerus fracture. Sports Health [online newsletter]. Veritas Health, Deerfield, IL. Published February 17, 2017. Accessed August 12, 2020. https://www.sports-health.com/sports-injuries/shoulder-injuries/treating-proximal-humerus-fracture
3 Eiff MP, Hatch RL. Boning up on common pediatric fractures. Contemp Pediatr [MJH Life Sciences, Cranbury, NJ]. November 2003. Accessed August 2020. https://www.contemporarypediatrics.com/view/boning-common-pediatric-fractures-0.
4 Lefèvre Y, Journeau P, Angelliaume A, Bouty A, Dobremez E. Proximal humerus fractures in children and adolescents. Orthop Traumatol Surg Res. 2014;100(1 Suppl.): S149–S156. Accessed August 2, 2020.

5 Serious injuries outcome indicators: 2000–18. Stats NZ. Published October 2, 2019. Accessed September 2020. https://www.stats.govt.nz/information-releases/serious-injury-outcome-indicators-200018.
6 Kraus R, Wessel L. The treatment of upper limb fractures in children and adolescents. Dtsch Arztebl Int. 2010;107(51–52):903–910. Accessed August 12, 2020. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3023154/.
7 Lowe W. Orthopedic Assessment in Massage Therapy. Sisters, OR: David Scott; 2006.
8 Travell JG, Simon DG. Myofascial pain and dysfunction. Vol 1. Baltimore, MD: Williams & Wilkins; 1983.
9 Fritz S. Mosby’s Fundamentals of Therapeutic Massage, 4th ed. St. Louis, MO: Mosby Elsevier; 2009.
10 Vizniak NA. Orthopedic Conditions, 3rd ed. Vancouver, BC: Prohealthsys; 2015.
11 Grace S, Deal M. Textbook of Remedial Massage, 1st ed. New York: Elsevier; 2012.
12 Crall T, White B. Rehabilitation guidelines for proximal humerus fracture—ORIF. Mammorth Lakes, CA: Mammoth Orthopedic Institute. Published March 2016. Accessed August 14, 2020. https://www.mammothortho.com/pdf/proximal-humerus-fracture-orif-crall.pdf.
13 Gaillard F, Weerakkody Y. Proximal humeral fracture. Radiopaedia. Accessed Jan 12, 2022. https://radiopaedia.org/articles/proximal-humeral-fracture-1?lang=us.
14 Rush J. Humeral shaft fracture [webpage]. Accessed October 13, 2020. https://posna.org/Physician-Education/Study-Guide/Humeral-Shaft-Fractures. Publication date unavailable.
15 Popovic N, Bukva B, Maffuli N, Caine D. The younger athlete, Chap. 44. In: Brukner P, Khan K, eds. Clinical Sports Medicine: Vol 1–Injuries, 5th ed. New York: McGraw-Hill Education; 2018: 974–989.
16 The Royal Children’s Hospital Melbourne. How are children different. Accessed September 10, 2020. https://www.rch.org.au/trauma-service/manual/how-are-children-different/.
17 Bell J, Condren M. Communication strategies for empowering and protecting children. J Pediatr Pharmacol Ther. 2016;21(2):176–184.

18 Brown K, Fitzmaurice L, Milne K, Provoost D. Engaging children and young people in the policy process: Lessons learned from the development of the Child and Youth Wellbeing strategy. Policy Q. 2020;16(1):3–9.

19 Coyne I, Amory A, Kiernan G, Gibson F. Children’s participation in shared decision-making: children, adolescents, parents and healthcare professionals’ perspectives and experiences. Eur J Oncol Nurs. 2014;18(3):273–280.

20 Blume-Peytavi U, Tan J, Tennstedt D, Boralevi F, Fabbrocini G, Torrelo A, et al. Fragility of epidermis in newborns, children and adolescents. J Eur Acad Dermatol Venereol. 2016;30(4):3–56. Accessed August 25, 2020.

21 Mancini AJ. Skins. Pediatrics. 2004;113(3): 1114–1119. Accessed September 12, 2020. https://publications.aap.org/pediatrics/article-abstract/113/Supplement_3/1114/66814.

22 Kobesova A, Davidek P, Morris CE, Andel R, Maxwell M, Oplatkova L, et al. Functional postural-stabilization tests according to Dynamic Neuromuscular Stabilization approach: Proposal of novel examination protocol. J Bodyw Mov Ther. 2020;24(3):84–95.

23 Casey P, Patalay P, Deighton J, Miller SD, Wolpert M. The Child Outcome Rating scale: Validating a four-item measure of psychosocial functioning in community and clinic samples of children aged 10–15. Eur Child Adolesc Psychiatry. 2020;29(8):1089–1102.

24 Duncan BL, Miller SD, Sparks J, Claud D, Reynolds L, Brown J, et al. The session rating scale: Preliminary psychometric properties of a “working” alliance measure. J Brief Ther. 2003;3(1):3–12.
25 Hefford C, Haxby Abbott J, Arnold R, Baxter GD. The Patient-Specific Functional scale: Validity, reliability, and responsiveness in patients with upper extremity musculoskeletal problems. J Orthop Sports Phys Ther. 2012;42(2):56–65. https://pubmed.ncbi.nlm.nih.gov/22333510/.

26 Patient-Specific Functional scale. Physiopedia [website for health professionals]. Publication date unavailable. Accessed October 17, 2020. https://www.physio-pedia.com/Patient_Specific_Functional_Scale.
27 Fujiura T, Nagasawa H, Wakabayashi H. Effect of manual lymphatic drainage for up to 10 days after total knee arthroplasty: a randomized controlled trial. Phys Ther Res. 2020;23(1):39–46.


28 Chaitow L, DeLany J. Clinical Application of Neuromuscular Techniques. Vol 1: The Upper Body, 2nd ed. London, UK: Churchill Livingstone Elsevier; 2008.
29 Musculoskeletal Key. Pediatric range of motion. Published August 10, 2016. Accessed October 2020. https://musculoskeletalkey.com/pediatric-range-of-motion/.
30 Vizniak NA. Muscle Manual, 2nd ed. Vancouver, BC: Prohealthsys; 2018.
Corresponding author: Hélène Geoffroy-Legeay, BTSM, RMT, Department of Massage, Southern Institute of Technology, Invercargill 9810, New Zealand, E-mail:
hln.legeay@gmail.com
(Return to Top)
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 15, NUMBER 1, March 2022