Figure 1
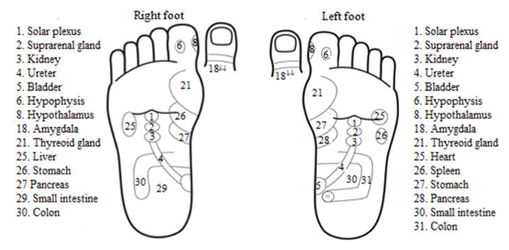
Schematic image of the points/regions of the massage protocol in the plantar area of the right and left feet.
Source: Kuba G, Mogi E. Foot Reflexology Course. São Paulo: Institute of Integrated and Oriental Therapy (ITIO); 2017.
Amanda K.S. Vieira , RN 1*, Marisa T. Nagumo 2, Gisele Kuba , PhD 2, Leonice F.S. Kurebayashi , PhD 2, Ruth N.T. Turrini , PhD 1
1 Department of Medical Surgical Nursing, Nursing School, University of São Paulo, São Paulo
2 Institute of Integrated and Oriental Therapy, São Paulo, Brazil
Background:
Premenstrual syndrome is a highly prevalent cyclical disorder among women of childbearing age which interferes with daily activities, mood, and quality of life.
Purpose:
To evaluate the effects of a foot reflexology protocol on relieving premenstrual syndrome symptoms in nursing students.
Setting:
Nursing School, São Paulo University, Brazil.
Participants:
A convenience sample of 17 nursing students, diagnosed with moderate-to-severe premenstrual syndrome as assessed by the Premenstrual Symptoms Screening Tool (PSST).
Research design:
A pre–post pilot intervention study.
Intervention:
The intervention consisted of eight reflexology sessions lasting 30 minutes for eight weeks.
Main Outcome Measure:
Evaluation of the participants by the PSST applied at the beginning and at the end of the study.
Results:
The participants had an average age of 21.7 (±2.6) years, ranging from 19 to 28 years; all were single, and most were in the third year of the course (58.8%); 75.6% lived with their family; 82.4% do not use contraceptives; 64.7% reported regular menstrual flow with an average duration of 5.1 (±1.1) days, and an average menstrual cycle interval of 29.3 (±4.9) days. The intervention significantly reduced the premenstrual symptoms assessed by the PSST ( p <.017) with a pre–post difference of 10.2 points in the overall score, and the items score decreased between 1.2 to 3.4 for difficulty concentrating, insomnia, hypersomnia, feeling overwhelmed, muscle/ joint pain, bloating, weight gain; and between 3.5 to 5.2 to anger/irritability, anxiety/ tension, tearful, depressed mood, decreased interest in daily activities, fatigue, overeating, and breast tenderness. There was a significant decrease regarding the functional impact of premenstrual symptoms domain in the overall score with a pre–post difference of 10.7, and between 1.7 and 3.0 for all of the items ( p <.04), except for the item “your home responsibilities”.
Conclusion:
Foot reflexology has shown promising results in reducing premenstrual syndrome symptoms.
KEYWORDS: physical therapy modalities , massage , premenstrual syndrome , nursing student
Premenstrual syndrome (PMS) is characterized by a set of physical, emotional, behavioral, cyclical, and recurrent symptoms such as anxiety, mood swings, sleep disorders, fatigue, changes in sexual libido, breast tenderness, weight gain, swelling, headaches and general pains, and changes in appetite,(1) which can vary from one cycle to the next. Menstrual pain may also increase anxiety, tension, sensitivity to rejection by others, and irritability.(2) It is important to differentiate PMS from Premenstrual Dysphoric Disorder (PMDD), which is a more serious subtype with predominantly psychological symptoms.(3)
It is estimated that 5% to 20% of women worldwide have moderate-to-severe premenstrual complaints during their reproductive life, and up to 75% of all women of reproductive age may experience PMS symptoms.(2) A study with a college population in a Turkish university found the prevalence of PMS alone and with dysmenorrhea was 71.3% and 65.9%, respectively; and up to 60% mentioned moderate or severe symptoms of PSM, mainly depression, fatigue, anxiety, irritability, and mood swings.(4) Another study developed in Turkey found a prevalence of 58.1% of PMS among university students in the first year of health faculties.(5)
A comparative study with medical and other health sciences students showed that the prevalence of dysmenorrhea fluctuated around 62%, and only 6% sought medical help for symptom relief; furthermore, 56% self-medicated and 83% used non-pharmacological actions, with a higher prevalence in the group of students in the non-medical field.(6) A cross-sectional survey with students studying health sciences at a state university in Turkey observed a prevalence of 84.5% of PMS among them.(7)
The syndrome has significant consequences on the daily lives of women, their families, and the community which surrounds them, in addition to being one of the factors which makes women more susceptible to depression.(3) PMS symptoms can interfere with the efficiency and/ or productivity of women in their work/ study, as well as in their relationships with co-workers and family, in addition to interfering in their social life activities and responsibilities at home.(8) There are reports that PMS affects students’ academic performance.(2)
Despite divergences in the literature in both the diagnosis and treatment of PMS and in the beginning and end of its symptoms, this study will consider the most comprehensive possible situation in which the symptoms start at the time of ovulation, reach a climax in the last five premenstrual days,(9) and are relieved with the onset of menstrual flow, or a few days after it.
Until recently, the treatment focus for PMS was pharmacotherapy with the use of selective serotonin reuptake inhibitors, anxiolytic agents, gonadotropin-releasing hormone agonists (GnRH), spironolactone, non-steroidal anti-inflammatory drugs, and/or oral contraceptives. However, clinical research currently suggests that a combination of treatments, including pharmacotherapy with aerobic exercises, homeopathic remedies, reflexology, light therapy, therapeutic massage and/or nutritional modifications, has been more beneficial than single treatments.(3)
Complementary and alternative medicine (CAM) includes several health-related strategies which are outside the conventional medical curriculum,(10) exploring an expansion of the health-disease process and promotion of human care. The popularity of alternative medicine has increased due to the growing search for holistic approaches which emphasize integrating the body, mind, and spirit, along with physical symptoms, in improving health care and well-being.(11)
Reflexotherapy, or reflexology, is a therapy which contributes to pain sedation, eliminates toxins, and promotes relaxation from the reflex points of the body on the feet, hands, and ears.(12) This study focuses on foot reflexology.
The foot reflexology technique consists of applying pressure through the principles of sedation and toning, which respectively aim to circulate stagnant energy in high-energy concentration regions and input energy in low-energy concentration regions. The reflex location points on the foot generally reproduce the human anatomy. The upper part of the hallux corresponds to the head region, and the spine is along the medial border of the feet; similarly, the right foot corresponds to the right side of the body and the left foot corresponds to the left side.(13)
Understanding the foot reflexology action can be related to the Chinese meridians, which are considered different energetic flows responsible for circulating Qi in the human body. Its function is to nourish and guarantee balanced functioning of the human body in the physiological, mental, and emotional spheres.(14) A change in the flow of the meridians can cause discomfort, for example, in the premenstrual phase.
Reflexology can be defined as a technique which is capable of evaluating and treating physical and emotional disorders through stimuli in nervous plexuses related to the organ or to the emotional characteristic being treated.(15) In view of this, foot reflexology appears as an interesting treatment proposal because PMS is a disorder of both physical, behavioral and/or emotional changes, with a negative impact on women’s daily activities, as the therapy proposes pain reduction, and promotes relaxation and homeostasis. In addition, reflexology has a positive effect on stress, anxiety, and quality of life in general.(16)
The first publication of a blinded two-arm clinical trial, placebo and intervention also benefited from reflexology in reducing premenstrual syndrome symptoms by applying it to the microacupuncture reflex systems in the ear, hands, and feet.(17)
Due to the frequent side effects of drugs and, in some cases, a high cost, knowing the effectiveness of a foot reflexology protocol for treating PMS is important for providing women with a non-pharmacological and non-invasive care alternative for their health, and which also can be self-applied.
There are few studies on foot reflexology for premenstrual syndrome applied to college populations, and some of them were written in a foreign language such as Korean(18–19) or Farsi.(20) Only one of them presented a protocol to relieve premenstrual syndrome with images of the points to be pressured, but also including ear and hand points.(17) Thus, this study aimed to evaluate the effects of a foot reflexology protocol on relieving premenstrual syndrome (PMS) symptoms in nursing students.
This pre–post pilot intervention study was conducted at the University of São Paulo Nursing School (EEUSP), as a pre-experimental study for future randomized clinical trials.
The foot reflexology appointments were performed at the Center of Nursing Laboratories in Teaching, Skills, Simulation and Research (CELAB) of the school itself.
A convenience sample of 30 volunteers graduating in Nursing from EEUSP was assessed for eligibility criteria. The inclusion criteria were defined as: enrolled in EEUSP graduation course; diagnosis of PMS according to the Premenstrual Symptoms Screening Tool (PSST) version validated in Brazilian Portuguese: the presence of at least five of the physical and psychological symptoms (first domain of the instrument), classified as moderate or severe; the presence of at least one of the first four symptoms of the first domain (anger/ irritation, anxiety/tension, desire to cry/increased sensitivity to rejection, depressed mood) classified as moderate or severe; the presence of at least one item of symptoms which evaluates the impact of PMS on the woman’s life (according to the instrument’s domain) classified as moderate or severe.(8) The exclusion criteria were: amenorrhea or pregnancy, endometriosis, presence of myoma with profuse bleeding, metrorrhagia, suspected uterus/ovarian tumors, chemotherapy or radiotherapy treatment in the last six months, diagnosis of depression or other psychiatric disorders, insensitivity in the lower limbs, decompensated diabetes, thrombosis, or performing some other complementary practice during the research period.
The clinical outcome was a reduction in premenstrual symptoms measured by the PSST. It presents a list of 19 items divided into two domains: 14 items on premenstrual symptoms which measure the intensity of symptoms according to criteria for PMDD of the 4th edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV), while the other domain contains five items on the functional impact of premenstrual symptoms.(21) Validation for Portuguese found a Cronbach’s alpha coefficient of 0.91 overall, 0.87 for the first domain and 0.84 for the second domain, content validity ratio of 0.61, content validity index of 0.94, and test–retest reliability of 0.867.(8) In this study, physical symptoms grouped into one item on the original scale were separated into five items so that each item corresponded to only one physical symptom.
Each participant received a weekly foot reflexology session lasting 30 minutes for eight weeks to follow two menstrual cycles. The protocol was developed by three authors of this study who teach courses in foot reflexology at the Institute of Integrated and Oriental Therapy (ITIO). The intervention was applied by a nursing student, who had completed the foot reflexology course, using the Sokutei technique which sedates hyperactive regions through slow and deep movements, or tones hypoactive regions with rapid and superficial movements. The need for sedation and toning varied throughout the sessions and from participant to participant. The points corresponding to the symptoms and their consequences (present in the first and second domains of the PSST) were worked on respectively. According to the principles of foot reflexology, the selected points contribute to regulating sleep, emotional balance, the ability to concentrate, the flow of body fluids, and menstruation regulation. An intervention protocol was used respecting the need for toning or sedation of each participant.
Preparing the feet: Clean the feet with cotton soaked in 70% alcohol, wrapping one foot with one hand while the other performs cleaning.
Relaxation: (1st) Hold the foot by the heel and perform dorsiflexion and plantar flexion movements to stretch the anterior and posterior leg muscles. Repeat the movement three times; (2nd) Press the instep with your thumbs. Repeat the movement three times; (3rd) Press the back of the feet with the palm of the hand, making circular movements. Repeat the movement three times; (4th) Hold the foot with both hands and perform twisting movements, sliding your hands through it. Repeat the movement three times; (5th) Press the plantar area of the feet with your thumbs. Repeat the movement three times; (6th) Press the plantar region with the palm of your hand, making circular movements. Repeat the movement three times.
Work the points corresponding to the symptoms present in the PSST, respecting the following order: (1st) Right foot: points 1, 2, 3, 4, 5, 6, 8, 18, 21, 25, 26, 27, 29, and 30 (Figure 1); (2nd) Left foot: points 1, 2, 3, 4, 5, 6, 8, 18, 21, 25, 26, 27, 28, 30, and 31 (Figure 1); (3rd) Medial region: Uterus (point 4) (Figure 2A); (4th) Lateral region: Menstruation (point 1) and Ovaries (point 4) (Figure 2B); (5th) Frontal region: Equilibrium and discouragement (point 3) and head problems (Figure 2C).
Finish the massage as described in Step 2 (relaxation).
|
|
||
|
Figure 1
Schematic image of the points/regions of the massage protocol in the plantar area of the right and left feet.
|
||
|
|
||
|
Figure 2
Uterus point (2A), points of ovaries and menstruation (2B), points of discouragement and balance and head problems (2C).
|
||
The study was advertised in the student space via WhatsApp groups, and the PSST instrument and the biosociodemographic questionnaire were sent electronically to students who showed interest in participating in order to identify students who met the eligibility criteria. The biosociodemographic questionnaire collected information on age, marital status, year of graduation, work/occupation, living companions, presence of other people in the family who suffer from PMS, clinical and surgical history, weight, date of last menstruation, regularity and flow intensity, use of hormonal contraceptives, and usual treatments for symptom control.
A total of 26 of the 30 undergraduate students interested in participating in the study were considered eligible and were subsequently contacted via WhatsApp or e-mail to continue the study. The selected participants received the intervention with the foot reflexology application and filled out the PSST instrument again at the end of the study. The participants were evaluated in each foot reflexology session according to the Evolution Instrument (changes perceived in the new menstrual cycles, uncomfortable/painful points during massage and evaluation of the session).
Descriptive statistics were used to characterize the participants, and the paired student’s t test or Wilcoxon signed-rank test according to the normality of data were used to assess the effect of the intervention, with an alpha of 5%. The effect size was calculated by Cohen’s d with 0.2 < d < 0.5 considered as a small effect, 0.5 ≤ d < 0.8 medium effect, and d ≥ 0.8 as a large effect.(22) Some speeches from the participants were also used to present their perceptions about the intervention. The letter P for the participant and a numerical sequence randomly assigned to the participants is used to present their reports.
In compliance with the legislation on research with human beings, the project was submitted to, and approved by, the Research Ethics Committee of the School of Nursing (no. 2,968,728) and the Research Commission, to authorize its development with school students. The participants signed the Informed Consent Form.
Of the 26 volunteers who met the eligibility criteria, seven did not respond to messages to continue the study and two failed to meet the inclusion criteria during data collection. Thus, 56.7% (17/30) completed the study (Figure 3).
|
|
||
|
Figure 3 Flow diagram of the study. |
||
The participants had an average age of 21.7 (± 2.6) years, ranging from 19 to 28 years; all were single, most were in the third year of the course (58.8%), and 75.6% lived with their family; 82.4% did not use contraceptives; 64.7% reported regular menstrual flow, with an average duration of 5.1 (± 1.1) days, range from 3 to 7 days and an average menstrual cycle interval of 29.3 (± 4.9) days, range from 21 to 40 days.
The intervention significantly reduced the premenstrual symptoms assessed by the PSST ( p <.017) (Table 1), with a pre–post difference of 10.2 points in the overall score. The items scores decreased between 1.2 to 3.4 for the symptoms difficulty concentrating, insomnia, hypersomnia, feeling overwhelmed, muscle/joint pain, bloating, and weight gain, and between 3.5 to 5.2 for anger/irritability, anxiety/tension, tearful, depressed mood, decreased interest in daily activities, fatigue, overeating, and breast tenderness.
Table 1
Descriptive Analysis of the Premenstrual Symptoms Domain of the PSST and P Value of the Comparison Before and After
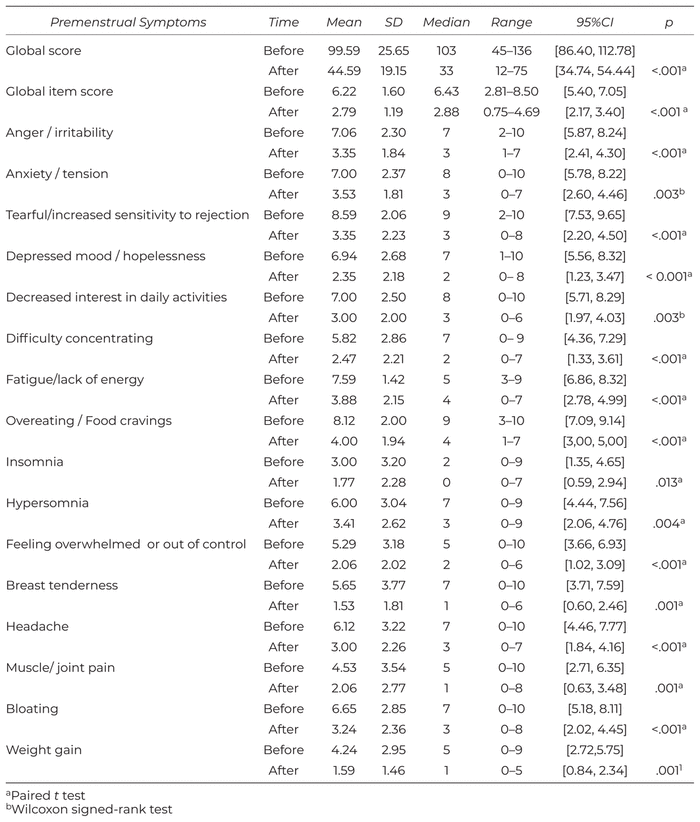
There was a significant decrease regarding the functional impact of the premenstrual symptoms domain in the overall score, with a pre–post difference of 10.7 and between 1.7 and 3.0 for all of the items, except for the item ‘your home responsibilities’, which did not achieve a statistically significant reduction (Table 2).
Table 2
Descriptive Analysis of the Functional Impact of Premenstrual Symptoms Domain of the PSST and The P Value Result of the Comparison Before and After.
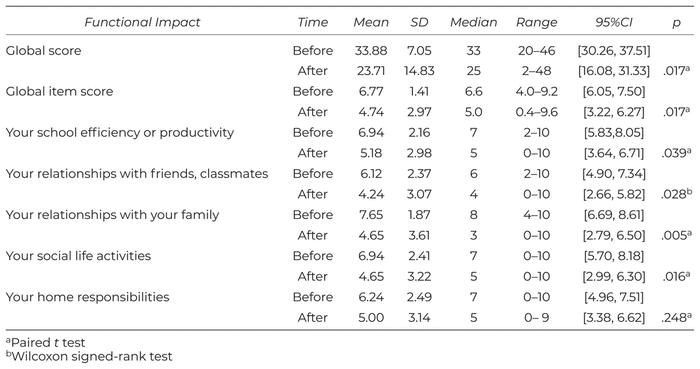
Considering the confidence interval, the effect on the symptoms of insomnia, hypersomnia, and feeling overwhelmed is questionable. The same was observed for the functional impact of premenstrual symptoms domain, except for the item ‘your relationships with your family’.
A large effect size measured by Cohen’s d was observed in the premenstrual symptoms for the overall score (2.50), and higher than 0.9 for all the items except insomnia (0.46) and muscle/join pain (0.80). Although classified as large, the effect size in the functional impact of premenstrual symptoms domain presented smaller values (range from 1.08 to 0.83), except for the items ‘your school efficiency or productivity’ ( d = 0.70), ‘your relationships with friends, classmates’ ( d = 0.71), and ‘your home responsibilities’ ( d = 0.45).
Other results in addition to the findings obtained with PSST were noticed during the sessions regarding the therapeutic evolution. Of the participants, 88.2% (n = 15) did not need to use medication or other treatment to reduce premenstrual symptoms during the intervention period; 41.2% (n = 7) noticed a reduction in the menstrual flow intensity, a fact they claimed to be positive for them.
Among the answers recorded in the open question “session evaluation”, some also mentioned the effect of foot reflexology for relieving acute pain, and reducing anxiety and stress, as seen in the following responses:
I arrived with a headache and after the session the pain passed (P1 and P2).
I felt more willing this week. The sessions help me a lot to relax from the stress of the week (P3).
I feel less and less stressed; I feel a difference in the stress relief and tiredness from day to day (P4).
It has helped me far beyond PMS issues. It makes me less anxious (P5).
Some responses when filling out the instruments presented very positive feedback about reflexology regarding the relief of symptoms involving the menstrual period:
At the end of the sessions, I realize that in addition to not only reducing stress during the premenstrual period, there is also a noticeable decrease in pain intensity. For the first time in many years, I didn’t need to take any medication for cramps (P4).
I feel calmer and more concentrated than I usually do during the premenstrual period” (P3).
For the first time, I didn’t feel nauseous or vomit during PMS. Amazing! (P6)
Social and cultural factors affect the way a woman perceives PMS and its consequences;(23) in addition, a Turkish study found 56% of the college students reported lower academic performance during menstruation.(4) However, a large part of the studies on the subject show that a significant portion of women suffer from at least one premenstrual symptom during their reproductive life.
The results of this study showed that foot reflexology can be an important therapy for women who suffer from PMS and who are looking for an alternative to the use of medications. A significant reduction in premenstrual symptoms and their functional impacts were observed using the protocol proposed with a large effect size, and more than 80% of the participants did not take medication during the intervention period.
The first published clinical trial with reflexology applied the technique for 30 minutes once a week for eight weeks at the solar plexus, ovary, uterus, pituitary, supra-renal (or adrenal) gland, and kidney points (the same as in the present study), in addition to the sympathetic nervous system.(17) The protocol created for this study expanded the areas of pressure in the plantar region to follow the trajectory of the Liver, Kidney and Spleen meridians (Chinese medicine), which are closely associated with the menstrual cycle.
According to Chinese medicine, the proper functioning and homeostasis of the human body is due to the efficient absorption, circulation, and distribution of the Qi (energy) through the organism. Chinese medicine divides the organs into two categories: the storing ( Zhang ) and the transforming ( Fu ) organs.(14) Some of the various functions attributed to organs and viscera by the Zang Fu theory for these three organs with regard to the menstrual cycle stand out. The Kidney stores the Essence, ancestral energy responsible for providing the energy base which controls this phase, and its dysfunction can appear as pain in the lower back, tiredness, and fatigue.(24) The Spleen is responsible for energetically screening the food and liquid intake and for Blood production ( Xue ). When in an unbalanced state it can cause fatigue, edema in the lower limbs (also associated with renal energy), and a desire to eat sweet foods (representative flavor of this organ).(25) And finally the Liver, which is an organ responsible for circulating Qi (Energy) in the body, is capable of expelling the blood produced by the Spleen and Kidneys. Some symptoms appear when the energy of this meridian becomes unbalanced, such as headache, irritability, colic/cramping, and irregular sleep.(26)
The protocol application from this first study(17) aimed to balance the energy flow in the body with the objective of restoring the functions of the organs related to the menstrual cycle. The improvement in symptoms, as observed in the students reports, shows the positive effect of this intervention on Qi circulation in these meridians and their interrelationships.
A meta-analysis on the effects of reflexology on PMS showed that there is a reduction in the severity of the physical and psychological symptoms related to PMS; the session length has an impact on the severity of premenstrual symptoms; and no side effects have been reported.(27) However, the study did not discuss the relationship of the effects from the reflex points used in the treatment.
Another study with voluntary health students to compare the effect of foot reflexology with olive oil applied three times a week and of connective tissue massage for five days a week for treating dysmenorrhea concluded that both techniques were effective for reduction of pain, use of analgesics, and premenstrual symptoms.(28) The intervention protocol in this referenced study for foot reflexology application contained several common points with those in the protocol of the present study, namely: solar plexus, hypothalamus and pituitary gland, thyroid, spleen, small and large intestines, uterus and ovary. The first point to be massaged in both protocols was the solar plexus point, which aims to stimulate the whole body. Another similarity between the two intervention protocols was the reflexology application time of thirty minutes in duration.
There are reports of the influence of foot reflexology in reducing stress or anger/ irritation, frequent symptoms in PMS, in undergraduate students,(29) in pre-menopausal women,(30) and also in reducing fatigue and cortisol levels in the urine of women with postpartum depression.(31) These three studies showed the effectiveness of the technique for improving fatigue/lack of energy, a symptom which can have an impact on other items evaluated by the PSST instrument, such as: lack of interest in daily activities, difficulty concentrating, and excessive sleep.
Regarding the effect of reflexology on fatigue, sleep, and pain, a literature review with a meta-analysis concluded that reflexology is an effective intervention for reducing fatigue and for treating sleep disorders.(7) Excluding eight (18.2%) studies with an interval between sessions of a few days, the median duration of the intervention was three weeks (1 to 6), with a median of six sessions (2 to 14) and 30 minutes of foot reflexology (20 to 60). The authors suggest in their conclusions that the session duration should be at least 30 minutes due to the Chinese meridian theory(11) upon which reflexology practice is based.
The effectiveness of foot reflexology for treating insomnia was also confirmed in another investigation(32) which showed a significant reduction in insomnia in the group that received intervention when compared to the control group.
Increased intake of caloric foods during the premenstrual period or overeating/desire to eat may be related to stress or anger/ irritation, given that cyclical fluctuations in estrogen and progesterone increase the stress response, and fluctuations are responsible for the increased desire for food.(33) Thus, reduced stress after applying foot reflexology may also explain the reduction in excessive desire for caloric foods and, consequently, a reduction in weight gain.
Weight gain may also be related to premenstrual swelling, which is a symptom present in the first domain of PSST in which its reduction was evidenced after applying foot reflexology. The swelling, which is also perceived by increased breast sensitivity, is due to progesterone, and impairs drainage by generating damage in the blood vessels, leading to fluid retention.(34)
The set of symptoms found in the first domain of the PSST directly or indirectly impact the lives of women suffering from PMS and, therefore, a reduction in these impacts after applying reflexology is confirmed by the reduced symptoms. The impacts are listed in the second domain of the instrument, and include: efficiency and productivity in university, relationships with fellow students, family relationships, activities and social life, and responsibilities at home. The benefit of the reflexology was perceived by the students and the reports showed improvement of the quality of life.
Limitations of this study could be related to low numbers of participants who volunteered which decreases the power, increases risk of a Type I error, and the possibility of a finding by chance. In addition, other limitations include the absence of a control group and the randomness of the participants.
However, the importance of the study is due to the evidence so that the proposed protocol can be applied in a future clinical trial. The detailed steps of the intervention applied allow for reproducibility of the study, and make the procedure accessible to people who wish to take care of themselves.
The foot reflexology protocol implemented herein was not only effective in reducing symptoms and their impact on the lives of women with PMS, but also in maintaining the well-being of participants, thus constituting an important tool for promoting the quality of life of these women and/or people who are looking for a way to better manage the stress, anxiety, and fatigue accumulated in their daily lives.
Additionally, the use of protocols respecting the individuality of the participants in relation to the need for sedation or toning of the points is important for the reproducibility of the studies and for a better understanding of the differences in results obtained in research with different signs and symptoms and different population groups.
The authors thank the Nursing School of University of São Paulo for making this study possible, as well as the participants of this study.
The authors declare there are no conflicts of interest.
1 Sammon JC, Nazareth I, Petersen I. Recording and treatment of premenstrual syndrome in UK general practice: a retrospective cohort study. BMJ Open. 2016;6(3):e010244.

2 Minichil W, Skindir E, Demilew D, Mirkena Y. Magnitude of premenstrual dysphoric disorders and its correlation with academic performance among female medical and health science students at University of Gondar Ethiopia, 2019: a cross-sectional study. BMJ Open. 2020;10(7):e034166.

3 Tolossa FW, Bekele ML. Prevalence, impacts and medical managements of premenstrual syndrome among female students: cross-sectional study in college of health sciences, Mekelle University, Mekelle, Northern Ethiopia. BMC Women’s Health. 2014;14(1):1–9.
4 Bilir E, Yildiz Ş, Yakin K, Ata B. The impact of dysmenorrhea and premenstrual syndrome on academic performance of college students, and their willingness to seek help. J Turk Obstet Gynecol. 2020;17(3):196–201.
5 Acikgoz A, Dayi A, Binbay T. Prevalence of premenstrual syndrome and its relationships to depressive symptoms in first-year university students. Saudi Med J. 2017;38(11):1125–1131.

6 Chia CF, Lai JHY, Cheung PK, Kwong LT, Lau FPM, Leung KH, et al. Dysmenorrhoea among Hong Kong university students: Prevalence, impact, and management. Hong Kong Med J. 2013;19(3): 222–228
7 Işik H, Ergöl Ş, Aynioğlu Ö, Şahbaz A, Kuzu A, Uzun M. Premenstrual syndrome and life quality in Turkish health science students. Turk J Med Sci. 2016;46(3):695–701.
8 Câmara RA, Kohler CA, Frey BN, Hyphants TN, Carvalho AF. Validation of the Brazilian Portuguese version of the Premenstrual Symptoms Screening Tool (PSST) and association of PSST scores with health-related quality of life. Braz J Psychiatry. 2016;39(2):140–146.

9 Nevatte T, O’Brien PMS, Backstrom T, Brown C, Dennerstein L, Endicott J, et al. ISPMD consensus on the management of premenstrual disorders. Arch Womens Ment Health. 2013;16(4):279–291.

10 Fisher C, Adams J, Hickman L, Sibbritt D. The use of complementary and alternative medicine by 7427 Australian women with cyclic perimenstrual pain and discomfort: a cross-sectional study. BMC Complementary Altern Med. 2016;16(1):129.
11 Lee J, Han M, Chung Y, Kim J, Choi J. Effects of foot reflexology on fatigue, sleep and pain: a systematic review and meta-analysis. J Korean Acad Nurs. 2011;41(6):821–833.
12 Embong NH, Soh YC, Ming LC, Wong TW. Revisiting refleoxology: concept, evidence, current practice, and practitioner training. J Tradit Complement Med. 2015;5(4):197–206.

13 Foot Reflexology Course. São Paulo: Institute of Integrated and Oriental Therapy (ITIO); 2017.
14 Lemonnier N, Zhou GB, Prasher B, Mukerji M, Chen Z, Brahmachari SK, et al. Traditional knowledge-based medicine: a review of history, principles, and relevance in the present context of P4 systems medicine. Prog Prev Med. 2017;2(7):e0011.
15 Lourenço OT. Reflexologia Podal: sua saúde através dos pés. São Paulo, BR: Ground; 2011.
16 McCullough JE, Liddle SD, Sinclair M, Close C, Hughes CM. The physiological and biochemical outcomes associated with a reflexology treatment: a systematic review. Evid Based Complement Alternat Med. 2014(2014).

17 Oleson T, Flocco W. Randomized controlled study of premenstrual syndrome treated with ear, hand and foot reflexology. Obstet Gynecol. 1993;82(6):906–911
18 Kim YH, Cho SH. [The effect of foot reflexology on premenstrual syndrome and dysmenorrhea in female college students.] Korean J Women Health Nurs. 2002;8(2):212–21.
19 Kim YS, Kim MZ, Jeong IS. The effect of self-foot reflexology on the relief of premenstrual syndrome and dysmenorrhea in high school girls. J Korean Acad Nurs. 2004;34(5):801–808.
20 Shafaie FS, Shirazi HD, Kamalifard M, Ghojazadeh M. The effect of foot medical zone-therapy reflex on the intensity of PMS symptoms in students (double-blind random controlled clinical trial). Iranian J Obstetr Gynecol Infert. 2018;21(7):10–19.
21 Steiner M, Macdougall M, Brown E. The premenstrual symptoms screening tool (PSST) for clinicians. Arch Womens Ment Health. 2003;6(3): 203–209.
22 Cohen J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed. Hillsdale, NJ: Lawrence Erlbaum; 1988.
23 Mendes DE, de Souza AP. Alterações fisiológicas relacionadas à Síndrome da Tensão Pré-Menstrual na Vida da Mulher [in Portuguese]. Rev Psic. 2017;10(33).
24 Ling S, Dang Y, Ni R, Xu J. The connotation of kidney stores essence theory and kidney endocrine substance. In: Li XT, editor. Chinese Medical Therapies for Diabetes, Infertility, Silicosis and the Theoretical Basis. Rijeka, Croatia: Intech Open; 2017.
25 Chung VC, Wu X, Lu P, Hui EP, Zhang Y, Zhang AL, et al. Chinese herbal medicine for symptom management in cancer palliative care: systematic review and meta-analysis. Medicine. 2016;95(7):e2793.

26 Liu ZW, Shu J, Tu JY, Zhang CH, Hong J. Liver in the Chinese and Western medicine. Integr Med Inter. 2017;4(1–2):39–45.
27 Hasanpour M, Mohammadi MM, Shareinia H. Effects of reflexology on premenstrual syndrome: a systematic review and metanalysis. BioPsycoSoc Med. 2019;13(1):25.
28 Demirtürk F, Erkek ZY, Alparslan Ö, Demirtürk F, Demir O, Inanir A. Comparison of reflexology and connective tissue manipulation in participants with primary dysmenorrhea. J Altern Complement Med. 2016;22(1):38–44.
29 Lee YM. Effects of self-foot reflexology on stress, fatigue, skin temperature and immune response in female undergraduate students. J Korean Acad Nurs. 2011;41(1):110–118.
30 Jang SH, Kim KH. Effects of self-foot reflexology on stress, fatigue and blood circulation in premenopausal middle-aged women. J Korean Acad Nurs. 2009;39(5):662–672.
31 Choi MS, Lee EJ. Effects of foot-reflexology massage on fatigue, stress and postpartum depression in postpartum women. J Korean Acad Nurs. 2015;45(4):587–594.
32 Lee YM, Shong KY. The effects of foot reflexology on fatigue and insomnia in patients suffering from coal workers’ pneumoconiosis. J Korean Acad Nurs. 2005;35(7):1221–1228.
33 Barreiros FF. Alimentação, estresse e ciclo menstrual. Porto, Portugal: Faculdade de Ciências da Saúde da Universidade de Fernando Pessoa; 2015.
34 Ferreira JJ, Machado AF, Tacani R, Saldanha ME, Tacani PM, Liebano RE. [Manual lymphatic drainage for premenstrual syndrome symptoms: a pilot study.] Fisioter Pesq. 2010;17(1):75–80.
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 14, NUMBER 4, December 2021