Sarah Rostron, RMT
Therapeutic Body Concepts, Edmonton, AB.Background
Migraines involve moderate-to-severe neck and face pain that lasts four to 72 hours, and are followed by fatigue and stiffness. Migraines are treated using medications, massage therapy (MT), and non-pharmacological alternatives. Cervical spondylosis (CS) is characterized by degeneration of the intervertebral discs, neck pain, and involvement of soft tissues in the cervical area. CS is treated using medications and manual therapy, including MT.
Objective
To determine the effects of MT on cervical range of motion and daily function in a patient with migraines and CS.
Case Presentation
The patient was an active 56-year-old female diagnosed with migraines and CS. Initial evaluation included cervical range of motion (ROM), goniometry, reflexes, myotomes, dermatomes, local sensation testing and orthopedic tests. Assessment was followed by five MT treatments. Swedish massage, myofascial trigger point release, and proprioceptive neuromuscular facilitation (PNF) stretching were applied to the back, neck, head, and face. The Headache Disability Index (HDI) was administered on the initial and final visits to evaluate patient function. Cervical ROM was measured pre- and posttreatment using a universal goniometer. Treatment was conducted by a second-year MT student at the MacEwan Massage Therapy Teaching Clinic in Edmonton, Alberta.
Results
All cervical ranges of motion improved. The Headache Disability Index score decreased, but was not considered significant. The patient reported decreased stiffness in the upper back and shoulders, reduced migraines, and better sleeping patterns after the MT intervention.
Conclusion
MT was effective in increasing cervical ROM, but had no significant effect on daily function. Further research is warranted on effects of MT on CS and migraines.
KEYWORDS: cervical spondylosis, massage therapy, migraine
Migraines involve moderate-to-severe head and neck pain. They affect an estimated 11% of the population worldwide, with 1% of that population experiencing chronic migraines.(1,2) Symptoms of migraines include attacks lasting four to 72 hours, with a unilateral location, pulsating quality, and pain which causes avoidance of regular physical activity.(3) Migraines can be preceded by an aura, which consists of visual or auditory disturbances, nausea, and vomiting.(3) Around 60% of patients experience symptoms such as depression, cognitive changes, fatigue, neck pain, and stiffness immediately after migraines.(3)
Migraines are treated using medications, lifestyle changes, trigger management, and complementary alternative medicine.(4,5) Massage therapy (MT), yoga, acupuncture, cognitive therapy, nerve stimulation, and dietary supplements are non-pharmaceutical treatments for migraine.(5,6) MT is effective in reducing the frequency, intensity, and duration of migraine headaches.(7–11) Manual therapies, including reflexology and MT techniques of trigger point therapy and manual lymphatic drainage, are used for the relief of migraine attacks.(7–11) Spinal manipulation techniques have been shown to reduce migraine-associated pain, but are out of the MT scope of practice.(9)
Cervical spondylosis (CS) is characterized by age-related spinal degenerative changes of the spinal intervertebral discs, neck pain, and involvement of cervical soft tissue.(12) The condition is diagnosed based on symptoms and further confirmed by X-ray.(12) Symptoms of CS include: “cervical pain aggravated by movement; referred pain; retro-orbital or temporal pain; cervical stiffness; vague tingling, numbness, or weakness in the upper limbs; dizziness or vertigo; poor balance; [and] rarely can trigger migraine”.(12) CS can present with osteophyte formation, and sometimes results in cervical radiculopathy.(12) CS affects 85% of people over the age of 60.(13)
CS is treated using physiotherapy, chiropractic manipulations, and medications including NSAIDS, opioid analgesics, muscle relaxants, antidepressants, anticonvulsants, and corticosteroids. Alternative treatments include Chinese Herbal Medicine, acupuncture, MT, and surgery.(13,14) Myofascial release, trigger point release, Swedish deep tissue techniques, and cervical traction have been shown to be effective in temporarily relieving pain and dysfunction in CS patients.(14) There is limited research on the effects of massage for individuals with both migraines and CS. The objective of this paper is to determine the effects of MT on cervical range of motion (ROM) and daily function in a patient with migraines and CS.
The patient was a 56-year-old retired female with migraines and CS. She was diagnosed with migraines by her family physician 20–30 years prior to treatment. Two years pre-treatment, her physician diagnosed multi-level CS and degenerative changes involving multiple facet and uncovertebral joints bilaterally. X-rays showed narrowing of the C5–C6 and C6–C7 disc interspaces, mild narrowing of the C4–C5 disc interspace, and multi-level CS.
At initial assessment, the patient’s main complaint was severe migraines, occurring six times per month. She rated her migraines on a pain scale from zero to ten, as seven or eight usually, and ten at worst (zero being no pain and ten being the worst pain imaginable). The most severe episodes required hospitalization. She described migraines as sharp and sore, and always located in her right eye. Major shifts in barometric pressure triggered her migraines. She was unaware of other triggers and experienced migraines throughout the year. She reported light, sound, and heat aggravated her symptoms, while ice, Axert® and darkness relieved them. Migraines were sometimes preceded by an aura of sparkly blue lights two hours prior, and occurred most often when the patient was going to sleep. Eighty per cent of her migraines occurred in the evening. She would wake in the middle of the night with sharp, stabbing pain in her right eye. She took 12.5 mg of Axert® as the aura occurred or if she felt a migraine starting, to prevent extreme symptoms. Symptoms normally remained for two days, followed by fatigue, and light and sound sensitivity. The patient reported difficulty reading and performing daily activities depending on the severity of the migraine. The patient had no family history of migraines.
The patient complained of neck and upper back stiffness with occasional pain. Her neck and upper back pain was usually one or two, zero at least and seven at worst. Pain was aggravated by sitting, reading, and sudden neck movements, and relieved by heat, massage, Tylenol®, and lying supine. Neck pain remained constant throughout the day, and she experienced cervical muscle fatigue in the evening. She reported limited ability to check blind spots over her shoulder while driving, occasional tension headaches with a skull-crushing feeling travelling up the posterior neck, and tightness under the skull. The patient perceived the tension headaches and neck pain to be linked, with one often causing the other.
Her past history included right medial epicondylitis in 2014, which resolved with physiotherapy and acupuncture. She experienced carpal tunnel bilaterally, which was resolved surgically in 2013. She practiced yoga three to four times per week, and enjoyed walking and reading. At the time of treatment, she was awaiting a cortisone injection to address tenosynovitis of her right thumb.
The patient’s treatment goals were to reduce migraines, improve cervical ROM, and relieve stiffness in her neck and upper back. She specified that no treatment was to be applied to her thumb; migraines were her main concern.
A cervical scan was performed to determine the origin of the patient’s pathology and rule out other conditions.(15,16) The scan included active cervical ROM with overpressure, myotomes, biceps, triceps, and brachioradialis reflexes, C1–T2 dermatomes, and active movements of all upper extremity peripheral joints. Goniometry measurements revealed limitations of active cervical side flexion and rotation bilaterally. Passive cervical ROM in supine was performed; all ranges were full, with normal end feels. All isometric cervical movements were strong. Local temperature sensation of the neck was normal. Foraminal compression and distraction tests were used to rule out nerve root impingement. Hautant’s and Kemp’s tests were used to rule out vascular and articular problems, respectively; all tests were negative. The patient’s right shoulder was slightly elevated compared to the left in sitting. Hypertonicity of the upper trapezii (right worse than left), levator scapulae, splenius capitus, splenius cervicis, infraspinatus, and upper erector spinae muscles was noted on palpation.
The therapist used a universal goniometer to measure active cervical ROM in sitting at the initial and final assessments, and before and after each treatment.(17) A goniometer has been found to be reliable and valid for measuring active cervical ROM.(17–19) The The Henry Ford Hospital headache disability inventory (HDI) is a questionnaire used to determine disability in terms of function and emotion caused by headaches.(20) It consists of 25 statements—answered with yes, sometimes, or no—to determine how the statement applies to the patient. Answers of yes are given four, sometimes are given two, and no are given zero points. Points are totalled out of 100; higher scores indicate greater disability.(20) A 29-point change is required between initial and final assessment to be considered clinically significant. The HDI was applied at the beginning of the first and sixth visits, and found to be reliable and valid.(20,21)
The therapist was a student in her fifth semester of a six-semester, 2200-hour MT diploma program at MacEwan University. The treatment took place in the Robbins Health Learning Centre in Edmonton, Alberta, in the Massage Therapy Teaching Clinic. It had a receptionist, waiting area, 15 hydraulic adjustable high-low MT tables, linens, pillows, oils, assessment tools, and various hydrotherapy modalities.
The patient did not present with osteophytes, which sometimes occur with CS, so there were no contraindications to passive stretching and cervical traction.(12,22) Treatment of acute migraine headaches is contraindicated if there are severe symptoms.(23) The use of heat hydrotherapy is contraindicated during an acute migraine attack.(23) Medical attention is required for patients experiencing sudden onset of headache with no cause, headache with fever and neck rigidity, headache after head trauma, or other symptoms of severe pathology.(23)
Treatment consisted of six weekly sessions; the first session was for assessment and the remainder for treatment. Each treatment consisted of 5 min of reassessment followed by 55 min of massage. The same treatment plan was followed for all sessions. Subjective input from the patient was obtained regarding the number of migraines, severity of symptoms, and the presence of stiffness before and after treatments.
Treatment began with the patient in prone for 35 min. Longitudinal palmar gliding strokes and palmar, fingertip, and thumb kneading were applied for 10 min across the entire back to prepare the tissues for deeper work, and reduce hypertonicity and pain.(24,25) Muscle stripping, myofascial skin rolling, and ischemic compression trigger point (TrP) release were utilized to reduce pain, tissue restrictions, and hypertonicity of the upper back and neck muscles.(26–28) There was a focus on upper erector spinae muscles, levator scapulae, upper and middle trapezii, splenius capitus, and splenius cervicis. Myofascial TrP release has been found to reduce headache symptoms and neck pain, and improve cervical ROM.(29–32) Therefore, TrPs in the upper trapezii and levator scapulae were treated for 24 min. Longitudinal palmar gliding strokes were applied for 1 min to the entire back to flush out fluid and metabolites mobilized during the previous techniques, and reduce posttreatment soreness.(25,33)
For the remaining 20 min, the patient was treated in supine. Massage techniques were applied to the upper trapezius, splenius capitus, splenius cervicis, sternocleidomastoid, suboccipital group, and temporalis muscles. Longitudinal palmar gliding strokes were applied for the initial 5 min with the goal of decreasing stiffness, pain, and hypertonicity.(24,25) Fingertip and knuckle kneading were applied to the posterior neck with the same goals as the initial strokes. Myofascial release was applied to the scalp and forehead to reduce restrictions and pain, and to relieve headache symptoms.(29–3233) Tension in the suboccipital group was released using fingertip kneading. Hypertonicity in this region can contribute to headaches.(26,27) Manual neck traction was held for 30 sec to reduce pain and increase cervical ROM.(21,22,34,35)
PNF stretching was applied to the upper trapezii, using the hold–relax technique. The patient was asked to elevate her shoulder for 6 sec against therapist resistance, then relax as the therapist passively laterally flexed the neck on exhalation. Three cycles of 6-second contractions with 6 sec in between contractions were used to increase ROM and flexibility.(36) PNF promotes reflexive relaxation of the target muscle as the antagonist contracts, due to reciprocal inhibition.(36) This allows the therapist to reach a deeper stretch and produces more significant increases in ROM than passive stretching. Longitudinal flushing strokes were used for the final minute of treatment, with the same goals as when the patient was in prone.(25,33)
For home care, the patient was advised to drink an extra glass of water after the massage, and perform a stretch to target the upper trapezii and scalene muscles for 30 sec on each side, one to two times per day. The patient was instructed to sit and use one hand on her head to laterally flex the neck away from her other hand which was placed underneath the buttock.
Written and verbal informed consent were obtained on initial assessment, and verbal consent was obtained prior to each treatment. Informed consent included discussion of risks and benefits of treatment, and the right to refuse treatment or disclose information, ask questions, request changes, or revoke consent. The therapist discussed findings and treatment options before obtaining consent. The aims of treatment were aligned with the patient’s goals to increase cervical ROM, decrease upper back and neck stiffness, and decrease migraines. Written consent to participate in the case report was also obtained.
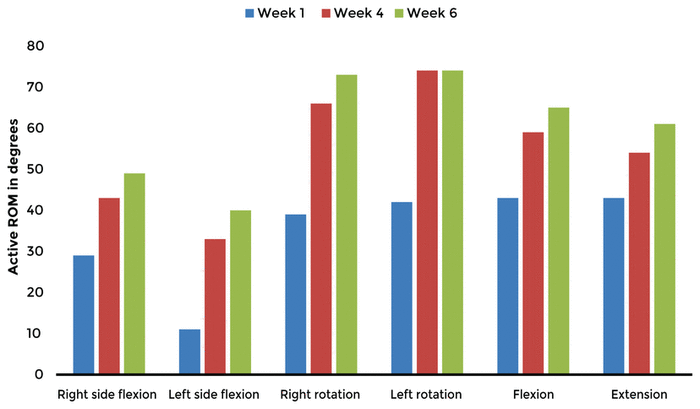
The patient’s active cervical ROM increased in all movements from initial to f inal visits (Table 1). The HDI results decreased by 18 points, while a decrease of 29 points is considered clinically significant (Table 2).
Table 1 Cervical Goniometry of Active ROM Following Treatmenta
Table 2 Headache Disability Index Scorea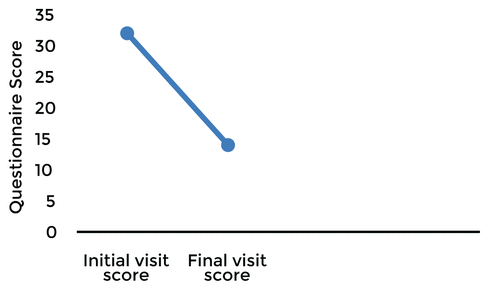
The patient indicated the frequency of migraines decreased by 30%–40% throughout treatment, and no longer affected her reading ability. She reported decreased stiffness in her upper back and neck, and reduced soreness in her shoulders. Hypertonicity and myofascial TrPs were decreased on final assessment. The patient did her prescribed stretch two to three times per day. After each treatment, she reported less tossing and turning at night, and also feeling rested in the morning. She reported increased cervical ROM and improvement in her ability to shoulder check. She experienced no tension headaches over the course of the sessions, and was pleased with her results.
Treatment of TrPs, myofascial restrictions, and hypertonic tissues effectively reduced stiffness and improved cervical ROM. Treatment was partially effective in reducing migraines. It has been hypothesized that the presence of myofascial TrPs and hypomobility of upper facet joints often found in CS are associated with migraines.(11) In this instance, the patient demonstrated increased ROM and improved function following MT treatment, possibly due to PNF stretching. The results of this study support those of previous studies; when TrPs were released and cervical ROM improved, migraines decreased.(11,27,29–32,36)
It is possible that the techniques applied in this study increased tissue extensibility by reducing fascial restrictions, improving tissue blood flow, and mechanical releasing of hypertonic muscles, which improved cervical ROM.(33,37) This supports the findings of other studies, which saw improvements in ROM following massage.(38,39)
Reduced subjective stiffness following MT supports the results of other studies.(40,41) It is feasible MT reduced myofascial restrictions, hypertonicity and TrPs, thus decreasing stiffness.(40,41) Based on the hypertonicity found at initial assessment, the MT used in this case report focused primarily on the upper trapezius, levator scapulae, posterior cervicals, and suboccipitals. Additional MT to other muscles implicated in cervicogenic headaches, such as the sternocleidomastoid and temporalis muscles, may have produced different results.
The frequency of migraines decreased over the course of treatment, but not by a clinically significant amount according to the HDI. Results may have been negatively affected by fluctuating weather conditions prevalent in the region during the winter.
This study was limited by a short duration and lack of follow-up. A follow-up two to three months after the study would help determine if results were sustained after treatment was discontinued. Chronic conditions can take longer to show improvements with manual therapy; the patient had migraines for decades before the study, which could have negatively affected results.(25) Another limitation was the absence of a pain scale recording at final assessment. Results cannot be generalized from this case report to a larger population. A larger sample size would provide more data for interpretation.
Future studies should utilize a longer duration with more measurement tools to evaluate frequency and duration of headaches; a Visual Analog Scale (VAS) is frequently utilized to measure migraine intensity. The VAS has been used extensively and found to be reliable and valid.(42) Further research should be directed at the effects of MT on CS so it can be utilized as a non-pharmacological alternative. The MT profession would benefit from larger scale research involving patients experiencing CS in combination with migraines. Research would allow for more comprehensive understanding of the effects of specific massage techniques, like myofascial release, TrP release, and PNF stretching, on these conditions.
This study suggests that MT can have positive effects on improving ROM, decreasing subjective stiffness, and reducing reported migraine frequency in a patient with both CS and migraines. Further research is needed to support the potential benefits of massage in this population. MT should be considered as a treatment option for patients with CS and migraines.
The author would like to thank Lois Wihlidal for her continued support and advice over the course of the case report, and Jeff Moggach for his guidance and assistance in planning and conducting the treatment sessions.
The author declares there are no conflicts of interest.
1 Stovner L, Hagen K, Jensen R, Katsarava Z, Lipton RB, Scher RB, et al. The global burden of headache: a documentation of headache prevalence and disability worldwide. Cephalalgia. 2007;27(3):193–210.
2 Natoli J, Manack A, Dean B, Butler Q, Turkel CC, Stovner, et al. Global prevalence of chronic migraine: a systematic review. Cephalalgia. 2010;30(5):599–609.
3 Weatherall M. The diagnosis and treatment of chronic migraine. Ther Adv Chronic Dis. 2015;6(3):115–123.
4 Rizzoli P, Mullally W. Headache. Am J Med. 2018;131(1):17–24.
5 Goskel BK. The use of complementary and alternative medicine in patients with migraine. Noro Psikiyatr Ars. 2013;50(Suppl 1):S41–S46.
6 Puledda F, Shields K. Non-pharmacological approaches for migraine. Neurotherapeutics. 2018;15(2):336–345.
7 Yedikardachian D, Quasthoff S, Lechner AT, Guilani A, Fazekas F. Migraine prophylaxis with trigger point therapy and lymphatic drainage: a pilot study. Wien Med Wochenscher. 2017;167(15–16):359–367.
8 Kobza W, Lizis P, Zieba HR. Effects of feet reflexology versus segmental massage in reducing pain and its intensity, frequency and duration of the attacks in females with migraines: a pilot study. J Tradit Chin Med. 2017;37(2):214–219.
9 Noudeh YJ, Vatankhah N, Baradaran HR. Reduction of current migraine headache pain following neck massage and spinal manipulation. Int J Ther Massage Bodywork. 2012;5(1):5–13.
10 Hernandez-Reif M, Dieter J, Field T, Swerdlow B, Diego M. Migraine headaches are reduced by massage therapy. Int J Psychol Neurosci. 1998;96 (1–2):1–11.
11 Tali D, Menahem I, Vered E, Kalichman L. Upper cervical mobility, posture and myofascial trigger points in subjects with episodic migraine: case-control study. J Bodyw Mov Ther. 2014;18(4): 569–575.
12 Binder A. Cervical spondylosis and neck pain. BMJ. 2007;334(7592):527–531.
13 Hirpara K, Butler J, Dolan R, O’Byrne J, Poynton A. Nonoperative modalities to treat cervical spondylosis. Adv Orthop. 2012:1–12.
14 Cheng Y, Huang G. Efficacy of massage therapy on pain and dysfunction in patients with neck pain: a systematic review and meta-analysis. Evid Based Compl Alt Med. 2014:1–13.
15 Wihlidal L. MTST 155: Assessment for Massage Therapists I. Edmonton, AB: MacEwan University; 2018:47–58.
16 Magee DJ. Orthopedic Physical Assessment, 6th ed. St. Louis, MO: Elsevier; 2014.
17 Farooq M, Banpei M, Ali M, Khan G. Reliability of the universal goniometer for assessing active cervical range of motion in asymptomatic healthy persons. Pak J Med Sci. 2016;32(2):457–461.
18 de Koning CH, Van den Huevel SP, Staal JB, Smits-Engelsman BC, Hendriks EJ. Clinimetric evaluation of active range of motion in patients with non-specific neck pain: a systematic review. Eur J Spine. 2008;17(7):905–921.
19 Asha S, Pryor R. Validation of a method to assess range of motion of the cervical spine using a tape measure. J Manip Physiol Ther. 2013;36(8):538–545.
20 Jacobson G, Ramadan N, Aggarwal S, Newman C. The Henry Ford Hospital headache disability inventory. Neurology. 1994;44(5):837–842.
21 Haywood KL, Mars TS, Potter R, Patel S, Matharu M, Underwood M. Assessing the impact of headaches and the outcomes of treatment: a systematic review of patient-reported outcome measures (PROMs). Cephalalgia. 2018;38(7):1374–1386.
22 Edmond S. Joint Mobilization/Manipulation: Extremity and Spinal Techniques, 3rd ed. St. Louis, MO: Elsevier; 2017:231–235.
23 Rattray F, Ludwig L. Clinical Massage Therapy: Understanding, Assessing and Treating Over 70 Conditions. Elora, ON: Talus Incorporated; 2000:497–509.
24 Adams R, White B, Beckett C. The effects of massage therapy on pain management in the acute care setting. Int J Ther Massage Bodywork. 2010;3(1):4–11.
25 Andrade C. Outcome Based Massage: Putting Evidence into Practice, 3rd. ed. Philadelphia, PA: Wolters Kluwer; 2014.
26 Cubick EE, Quezada VY, Schumer AD, Davis CM. Sustained release myofascial release as treatment for a patient with complications of rheumatoid arthritis and collagenous colitis: a case report. Int J Ther Massage Bodywork. 2011;4(3).
27 Arab AM, Ramezani E. Suboccipital myofascial release technique for the treatment of cervicogenic headache. J Bodyw Mov Ther. 2018;22(4):859.
28 Simons DG, Travell J, Simons D. Myofascial Pain and Dysfunction: The Trigger Point Manual, 2nd ed. Baltimore, MD: Williams and Wilkins; 1999.
29 Chatchawan U, Eungpinichpong W, Sooktho S, Tiamkao S, Yamauchi J. Effects of Thai traditional massage on pressure pain threshold and headache intensity in patients with chronic tension-type headaches and migraine headaches. J Altern Compl Med. 2014;20(6):486–492.
30 Quinn C, Chandler C, Moraska A. Massage therapy and frequency of chronic tension headaches. Am J Public Health. 2002;90(10):1657–1661.
31 Moraska A, Chandler C. Changes in clinical parameters in patients with tension-type headache following massage therapy: a pilot study. J Man Manip Ther. 2008;16(2):106–112.
32 Moraska F, Stenerson L, Butryn N, Krutsch JP, Schmiege SJ, Mann JD. Myofascial trigger point-focused head and neck massage for recurrent tension-type headache: a randomized, placebo-controlled clinical trial. Clin J Pain. 2015;31(2): 159–168.
33 Gasibat Q, Suwehli W. Determining the benefits of massage mechanisms: a review of literature. Rehabil Sci. 2017;2(3):58–67.
34 Peake N, Harte A. The effectiveness of cervical traction. Physical Ther Rev. 2005;10(4):217–229.
35 Avery RM. Massage therapy for cervical degenerative disc disease: alleviating a pain in the neck? Int J Ther Massage Bodywork. 2012;5(3):41–46.
36 Hindle K, Whitcomb T, Briggs W, Hong J. Proprioceptive neuromuscular facilitation (PNF): its mechanisms and effects on range of motion and muscular function. J Hum Kinet. 2012;31:105–113.
37 Backus D, Manella C, Bender A, Sweatman M. Impact of massage therapy on fatigue, pain, and spasticity in people with multiple sclerosis: a pilot study. Int J Ther Massage Bodywork. 2016;9(4):4–13.
38 Sobeck C, Lenk L, Knipper S, Rhoda A, Stickler L, Stephenson P. The effectiveness of functional massage on pain and range of motion measurements in patients with orthopedic impairments of the extremities. Int Musculoskelet Med. 2016;38(1):21–25.
39 Brummitt J. The role of massage in sports performance and rehabilitation: current evidence and future direction. N Am J Sports Phys Ther. 2008;3(1):7–21. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2953308/. Accessed February 2019.
40 Chunco R. The effects of massage on pain, stiffness, and fatigue levels associated with ankylosing spondylitis: a case study. Int J Ther Massage Bodywork. 2011;4(1):12–17.
41 Imtiyaz S, Vegar Z, Shareef MY. To compare the effect of vibration therapy and massage in prevention of delayed onset muscle soreness (DOMS). J Clin Diagn Res. 2014;8(1):133–136.
42 Hawker GA, Mian S, Kendzerska T, French M. Measures of adult pain: Visual Analog Scale for Pain (VAS Pain), Numeric Rating Scale for Pain (NRS Pain), McGill Pain Questionnaire (MPQ), Short-Form McGill Pain Questionnaire (SF-MPQ), Chronic Pain Grade Scale (CPGS), Short Form-36 Bodily Pain Scale (SF-36 BPS), and Measure of Intermittent and Constant Osteoarthritis Pain (ICOAP). Arthritis Care Res. 2011;63(S11):S240–S252.
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 14, NUMBER 3, September 2021