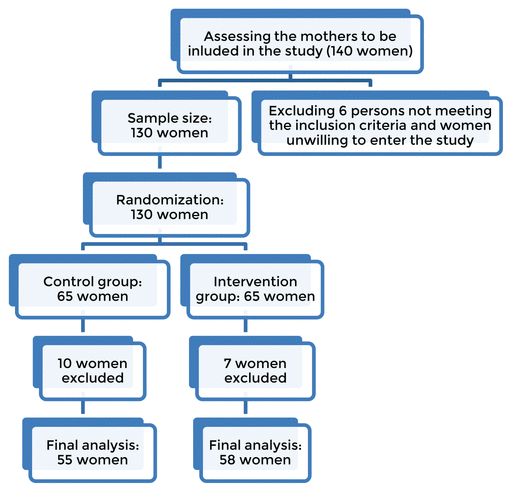
Figure 1 The participants’ selection flowchart.
Maryam Mahdizadeh-Shahri, MSc1, Manijeh Nourian, PhD2, Maryam Varzeshnejad, PhD2, Maliheh Nasiri, PhD3
1Student of Neonatal Intensive Care Nursing, School of Nursing and Midwifery, Shahid Beheshti University of Medical Sciences, Tehran, Iran
2Department of Pediatric Nursing, School of Nursing and Midwifery, Shahid Beheshti University of Medical Sciences, Tehran, Iran
2Department of Pediatric Nursing, School of Nursing and Midwifery, Shahid Beheshti University of Medical Sciences, Thehran, Iran
3Department of Basic Sciences, School of Nursing and Midwifery, Shahid Beheshti University of Medical Sciences, Tehran, Iran
Background
The negative effects of cesarean section on breastfeeding are a major global concern.
Purpose
This study aimed to determine the effect of Oketani breast massage on the maternal need for support during breastfeeding, breastfeeding success, and breastfeeding self-efficacy.
Setting
Three hospitals affiliated to Shahid Beheshti University of Medical Sciences in Tehran, Iran, from April to July 2019.
Study Design
The participants in this experimental study were 113 pregnant women who were candidates for cesarean section. The mothers were selected using convenience sampling and randomly assigned. In addition to routine care, the mothers in the intervention group received Oketani breast massages twice. However, the mothers in the control group received routine care. The data were collected using the Infant Breastfeeding Assessment Tool (IBFAT), LATCH Assessment Score, and the Breastfeeding Self-Efficacy Scale (BSES). The data were analyzed with SPSS 20 software via the independent samples t test, the Mann–Whitney U test, and the chi-square test.
Results
The results of the study suggested that the breastfeeding success rate, which was evaluated with IBFAT in both the first two breastfeeding stages and the last pre-discharge breastfeeding, was significantly higher for the mothers in the intervention group (p < .001). In addition, the mother’s need for support, which was evaluated with LATCH in the first two breastfeeding stages (p = .044) and the last pre-discharge breastfeeding (p < .001) in the intervention group, was less. The total number of breastfeeding sessions from birth to discharge was higher in the intervention group (p = .002). Furthermore, the mothers in the intervention group breastfed their infants in a significantly shorter time interval (p = .002). Breastfeeding self-efficacy, according to the BSES, was significantly higher in the mothers of the intervention group (p < .001).
Conclusion
Oketani massage can be used as a care intervention by nurses to improve breastfeeding in mothers who undergo cesarean sections.
KEYWORDS: Oketani massage, cesarean section, breastfeeding, self-efficacy, breastfeeding support, breastfeeding success
Despite global efforts to promote natural childbirth, the rate of non-emergency cesarean sections is increasing, especially in developing countries.(1) In Iran, the number of cesarean sections is much higher than the world standard(2) to the extent that cesarean sections count for more than 54.8% of deliveries in some regions.(1) However, the rate of cesarean sections in other areas of the world ranges from 10% to 15%.(1) The excessive increase in the number of cesarean sections, and its negative effects on breastfeeding success and duration of breastfeeding, has become a global concern.(1,3)
One of the important complications of cesarean sections is their negative impact on breastfeeding success.(1) Successful breastfeeding means the successful transfer of milk from the mother’s breast to the infant’s mouth. Factors, such as the infant’s desire and the frequency of breastfeeding in 24 hours (which should be between 8 and 12 times), affect its success. Successful breastfeeding indicators are hearing the sound of the baby swallowing and softening of the mother’s breast with wet diapers, and weight loss/gain within normal limits.(4) In cesarean sections, due to the long-term separation of the mother and baby, the lack of skin-to-skin contact, and the surgical pain, there is a delay in starting breastfeeding, and the breastfeeding success and consistency is reduced. As a result, these mothers need more support for breastfeeding, especially during the first hours and days after birth.(5,6,7) Furthermore, mothers who undergo cesarean sections are less interested in breastfeeding their babies and also their babies make less effort to be breastfed early during the first 24 hours of birth. This reduces the mother’s chance for successful breastfeeding(8) and increases the likelihood of milk accumulation and breast congestion.(9)
While the World Health Organization (WHO) and UNICEF emphasize early breastfeeding within one-half to one hour of birth and its exclusive continuation for at least six months,(1) the onset of breastfeeding is delayed for a longer time for neonates born via cesarean sections compared to those born via normal delivery.(3,5,6) This may reduce the baby’s acceptance of the breast and the baby’s sucking reflex, and thus negatively affect the development of the baby’s neurological system.(8) One of the most important factors affecting successful breastfeeding and its self-efficacy is the type of delivery. Cesarean sections delay the first breastfeeding and result in early and long-term separation of mother and baby, and the mother’s greater need for support for breastfeeding and its onset. Thus, cesarean sections reduce the mother’s sense of self-sufficiency and self-esteem, and hinder successful breastfeeding and its continuation.(3,6) Cesarean sections also increase the mother’s need for support during breastfeeding and reduce her breastfeeding self-efficacy.(10)
Breastfeeding self-efficacy is defined as the mother’s perceived breastfeeding ability and her self-confidence in her ability to breastfeed the baby successfully.(3,11) Low levels of breastfeeding self-efficacy are associated with an increased probability of early cessation of exclusive breastfeeding.(12) Nevertheless, breastfeeding self-efficacy has been shown to have a significant and positive relationship with increasing the breastfeeding time,(6,10) and is considered as one of the important indicators influencing breastfeeding outcomes.(13,14) In general, cesarean delivery has a negative effect on breastfeeding and can affect all three factors: the mother’s need for breastfeeding, breastfeeding success, and breastfeeding self-efficacy.(1,10,11) Therefore, given the numerous problems suffered by cesarean section mothers as detailed above, it is necessary to take intervention measures to reduce these problems and improve breastfeeding.
One of the standard nursing interventions mentioned in the Nursing Interventions Classification (NIC) is massage therapy.(15) Breast massage is a treatment technique used throughout the world and aims to relieve breastfeeding problems. There is a variety of breast massage techniques that may be used to treat breastfeeding problems. Some of these techniques include the Oketani breast massage, Gua Sha therapy, and general massage of breast tissue.(16,17)
One of the reasons for using a formula instead of breast milk is the negative effect of cesarean delivery on early breastfeeding. Using a formula also increases family expenses. Lack of breastfeeding increases the risk of the baby developing chronic diseases, which are associated with increased costs for the family and the hospital.(6,14,18) Oketani breast massage is an efficient, cost-effective, and easy method(9,19,20) that was first introduced as a massage technique in 1981 in Japan by Sotomi Oketani.(20,21) Some studies have addressed the effects of Oketani breast massage on breastfeeding, but its effect on breastfeeding success and the mother’s need for support during breastfeeding are still unknown. Studies have underlined its effect on reducing breast pain, increasing the speed of infant sucking,(19,22) improving the quality of breast milk by increasing pH,(19) increasing lipids at the end of feeding,(23) reducing sodium in breast milk,(19) increasing infant weight gain,(9) and reducing breast congestion in different communities.(24) While mothers who are candidates for cesarean sections are more prone to breastfeeding problems, there is no specific study on how to solve lactation problems caused by cesarean section, and studies addressing Oketani breast massage have focused on both groups of mothers with cesarean section and vaginal delivery.(9,19,22,24) The most important factor for the survival and health of infants is breastfeeding, and the first environment in which to start breastfeeding is the hospital.(25,26) Given the importance of the role played by nurses in supporting, educating, and promoting breastfeeding, and considering that Oketani massage is a low-cost, independent nursing intervention, and finally concerning the breastfeeding problems faced by cesarean section mothers,(9,26,16) the present study explored the effect of Oketani breast massage on the need for support during breastfeeding, breastfeeding success, and breastfeeding self-efficacy among mothers undergoing cesarean section.
This study was conducted using an experimental design with a control group. The research population included all pregnant women who were candidates for cesarean sections and referred to Mahdiyeh, Taleghani and Imam Hossein hospitals affiliated with Shahid Beheshti University of Medical Sciences in Tehran, Iran.
The inclusion criteria included: mothers aged between 18 to 35 years; singleton pregnancy; absence of physical and mental illness that prevented breastfeeding based on the available medical records; gestational age of 38 to 42 weeks; no history of breast surgery and breast tumor; the absence of disorders such as placental abruption, placenta previa, heart, and respiratory diseases during pregnancy; lack of hepatitis and AIDS during pregnancy and afterward; the birth of a healthy and mature baby weighing more than 2500 grams; the first- and fifth-minute Apgar score of above 7; the absence of the need for any postnatal medical intervention based on the medical records; and the absence of any cleft palate and cleft lip in the infant.
The exclusion criteria were as follows: infants in need of intensive care at birth or admitted to the neonatal intensive care unit; severe bleeding; atony or uterine inertia during cesarean sections; use of any drug that stopped breastfeeding; the existence of any reason that led to a ban on breastfeeding; the unwillingness to breastfeed the baby or participate in the study; and mothers who were discharged 24 hours before starting the study upon their consent and did not receive any massage treatment.
The sample size was calculated as equal to 44 women per group, following a similar study,(27) and according to the equation presented below with 95% confidence and 80% power. At least 50 mothers were selected as the members of each group (intervention group (n = 55) and the control group (n = 58).
The mothers were selected using convenience sampling and randomly assigned to the intervention and control groups. At each hospital, the researcher determined the group the mothers would be assigned to by simple lottery. To prevent contact between mothers in the two groups, sampling was performed in each hospital every other week. For example, by drawing lots, all eligible mothers in the first week were placed into the intervention group, and then in the second week, the mothers were assigned to the control group. This process was repeated until all mothers were assigned to one of the two groups. The sampling procedure was performed from April to July 21, 2019.
|
|
||
|
Figure 1 The participants’ selection flowchart. |
||
The mothers in the control group received routine care including measuring the baby’s height and chest circumference, dressing the baby with the help of an attendant who transferred the infant to the mother’s room under the supervision of a nurse, and teaching breastfeeding verbally, as well as the nurse’s emphasis on timely breastfeeding and instructions on how to care for the baby while breastfeeding. The mothers in the intervention group, in addition to receiving routine care, underwent Oketani breast massage by the researcher twice before the mother entered the operating room and once before the mother’s first breastfeeding in the recovery room or the ward. Before starting the intervention in both stages, the researcher did her best to maintain the participants’ privacy and protect their territory and space, according to the requirements of the hospital and the ward. To this end, she pulled the curtains in the room and performed Oketani massage on the massage site using a cotton towel. She also gave the mothers a package containing a cotton towel (to cover the massage site), a training brochure about Oketani massage and its benefits, and gloves. In addition, comprehensive explanations were given to the mothers orally on how to perform the massage. The mothers were also told that the massage would be done only by the researcher during the hospitalization period, and the mothers were forbidden to do the massage themselves during this period.
Oketani breast massage was performed using eight different manual techniques. Steps 1 to 7 are called “course of treatment” and Step 8, “expressing or milking”. A set of operations and expressing are completed within one minute and this is repeated for 15 to 20 minutes. Pushing and pulling away Steps 1, 2, and 3 involve manipulations to separate the hard portion of the breast from the fascia of the pectoralis major with very gentle pressure and without causing discomfort to mothers. Steps 4 to 6 involved pulling the whole breast with two thumbs down and to both sides by both hands. In Step 4, the whole breast is pushed down towards the umbilicus. Steps 5 and 6 are techniques to isolate the hard base portions of the breast. Additionally, Step 7 involves rotating the breast gently clockwise with stretching of its base and, in the Step 8, expression is done in four different directions for the outside surface, lower part, inside of the breast and inside of the upper periphery of the right breast and inside, lower part, outside surface, and inside of the upper periphery of the left breast. Manual operations are performed rhythmically and very gently.
The researcher performed Oketani massage on both right and left breasts. The massage therapy was performed on all mothers by the researcher after gaining the necessary training and skills under the supervision of a complementary medicine physician.
The breastfeeding success rate and mother’s need for support during breastfeeding were measured and recorded once in the first breastfeeding and once during the last breastfeeding (22 to 28 hours after the cesarean sections) for all mothers in both intervention and control groups before discharge. The Breastfeeding Self-Efficacy Scale (BSES) was completed by the mothers themselves once after the last breastfeeding. The number of breastfeeding times from birth to the last breastfeeding before discharge was recorded by the researcher.
This study was extracted from a master’s thesis approved by Shahid Beheshti University of Medical Sciences under the code of ethics IR.SBMU.PHARMACY. REC.1397.223. The objectives of the study were explained to all participants and written consent was obtained from them. The participants were reassured that their information would be kept confidential, and that they had the right to leave the study at any time they wished.
The following instruments were used to collect the data.
The Demographic Characteristics Questionnaire: The questionnaire contained two maternal and neonatal sections. The maternal information section was completed by the researcher according to the answers provided by the mother and the information in her medical file. The infant section was completed after birth by referring to the medical file documentation.
The LATCH Assessment Score: This tool was elaborated in 1994 in the USA by a nurse called Deborah Jensen and her group, to document the assessment of breastfeeding,(5,6,28) The total score gained by administering this tool varies from zero to ten, and getting a score of less than ten shows the mother’s need for more support during breastfeeding. The letters of the acronym LATCH designate separate areas of assessment: L (Latch) for how well the infant latches onto the breast; A (Audible swallowing) refers to the amount of audible swallowing noted while nursing the baby; T (Type of nipple) for the mother’s nipple type; C (Comfort) for the mother’s level of comfort related to the breast and nipple; and H (Hold) refers to whether or not the mother needs help in positioning the child. The system assigns a numerical score, 0, 1, or 2, to five key statements.(28) The validity and reliability of this tool have been reviewed and confirmed in several studies.(5,28–30) Karimi et al.(31) assessed the reliability of the tool using the Cronbach’s alpha coefficient, and the corresponding value was reported as 0.711. The reliability of this tool was evaluated in the present study using concurrent observation of 15 mothers and its Cronbach’s alpha coefficient was calculated to be 0.98.
The Infant Breastfeeding Assessment Tool (IBFAT): The IBFAT contains four scored items assessing the infant state: (1) infant readiness to feed/arousability, (2) rooting, (3) fixing (the time needed to latch to the breast), and (4) the sucking pattern. Each item is scored on a scale of 0–3, with the minimum and maximum scores of 0 to 12, respectively. A score of 10–12 indicates completely successful breastfeeding, a score of 7–9 suggests relatively successful breastfeeding, and a score of 0–6 shows unsuccessful breastfeeding. (32,33) This tool has been used in various studies in Iran, and its validity and reliability have been confirmed.(34–36) In the present study, the reliability of this tool was calculated to be 0.97 by concurrent observation of 15 participating mothers. The LATCH tool, which is a system for the documentation of lactation, identifies areas where intervention is required to support latency and focuses on the mother’s role in the process of breastfeeding, whereas the IBFAT scale focuses on the baby during feeding.(37)
The Breastfeeding Self-Efficacy Scale-Short Form (BSES-SF): This scale was developed by Dennis et al.(38) and contains 14 statements(10,38) that are scored on a 5-point Likert scale ranging from very confident (score 5) to never confident (score 1). The minimum and maximum possible scores on this scale are 14 and 70, respectively. In a study conducted in Iran by Araban et al.,(39) Cronbach’s alpha coefficient of the scale was reported to be higher than 0.7.(39) In various other studies, the Cronbach’s alpha coefficient of this instrument was reported from 0.86 to 0.94.(6,40) The internal consistency of the scale was estimated to be 0.94 in the present study.
The collected data were analyzed using SPSS software (version 20) via descriptive statistics (mean, standard deviation, frequency, and percentage) and inferential statistics including the independent samples t test, the Mann–Whitney U test, and the chi-square test.
In this study, Oketani massage was taken as the independent variable, and the breastfeeding success rate, the mother’s need for support during breastfeeding, and the mother’s breastfeeding self-efficacy were manipulated as the dependent variables. To accurately assess the breastfeeding success rate, the number of breastfeeding times and the onset time of the first breastfeeding were recorded and evaluated. The results showed that the mean age of the participants in the intervention and control groups was 29.85 ± 4.43 and 28.95 ± 5.33 years, respectively. There was no statistically significant difference between the two groups in terms of the mothers’ and infants’ demographic characteristics (Table 1). It was also shown that, in both breastfeeding rounds (the first and last breastfeeding before discharge), the number of mothers with completely successful breastfeeding according to the IBFAT in the intervention group was significantly higher than those in the control group (p < .001) (Table 2). Furthermore, it was noted that the mean scores for all dimensions of breastfeeding success, including readiness to feed, rooting, fixing (latching on), and sucking, in the breastfeeding mothers in the intervention group in both stages were significantly higher than those of the participants in the control group (p < .001).
Table 1 A Comparison of the Demographic Characteristics of the Participants in the Two Groups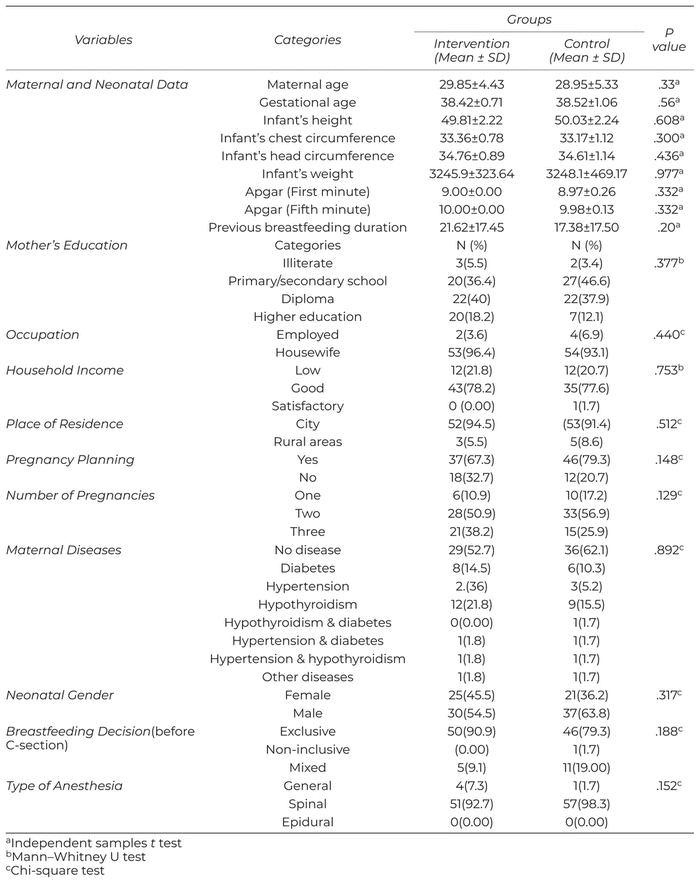
Table 2 A Comparison of the Two Groups According to the Mother’s Need for Breastfeeding Support and Breastfeeding Success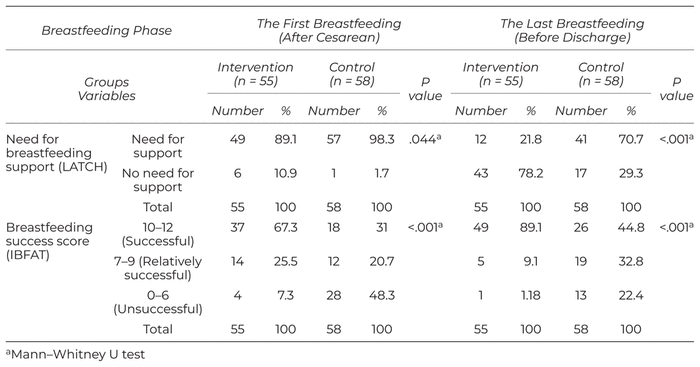
The results of the study suggested a significant difference between the two groups in terms of the need for breastfeeding support in both breastfeeding rounds. The mothers in the intervention groups, according to the LATCH, needed less support compared to the participants in the control group (p < .001) (Table 2). It was also shown that the number of breastfeeding times for the participants in the intervention group from the time of entry to the recovery room to discharge was higher compared to that of the participants in the control group (p < .001). In addition, the mothers in the intervention group breastfed their infants within less than one hour after entering the recovery room, showing a significant difference in comparison with the participants in the control group (p < .002) (Table 3). According to the hospital protocol, after the cesarean section, the infant was placed next to the mother (in both groups) and there was no prohibition on breastfeeding for one hour at birth. The results also indicated that the breastfeeding self-efficacy of the mothers in the intervention group according to the BSES was significantly higher than those in the control group (p < .001) (Table 4)
Table 3 A Comparison of the Two Groups in Terms of the Frequency of Breastfeeding, Time of First Breastfeeding, and Mother’s Breastfeeding Self-Efficacy
Table 4 Mean and Standard Deviation for Mothers’ Breastfeeding Self-Efficacy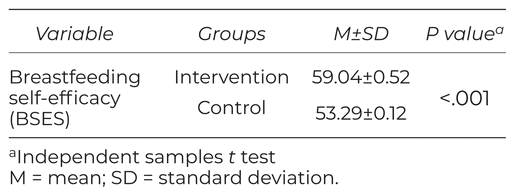
This study explored the effects of Oketani massage on breastfeeding success, the need for breastfeeding support, and breastfeeding self-efficacy among the mothers of term infants born via cesarean sections. The results of the current study suggested that Oketani massage has positive effects on the mother’s breastfeeding success and can improve it in different respects, including readiness to feed, rooting, fixing (latching on), and sucking, as evident in various earlier studies.(9,19,22,24,41) Cho et al.(19) found that Oketani breast massage, in addition to reducing breast pain and increasing the pH of breast milk, increased the sucking speed and breast milk volume and, consequently, an improvement in breastfeeding success. In the Cho study, the authors studied the mothers with any type of delivery and with breastfeeding problems and breast pain, and they did not focus on the problems of cesarean section mothers. Postoperative pain after cesarean sections is one of the reasons for a delay in starting breastfeeding,(1) which makes mothers experience more pain in the breast and the breasts are more prone to congestion.(24,42)
Massage can be used as an effective intervention to control mothers’ postoperative pain.(19,41,43) However, each massage therapy intervention, in addition to its positive effects, brings about some complications and side effects including muscle pain, fatigue, and damage to muscle tissue and peripheral nerves.(44,45,46) Nevertheless, since Oketani massage is based on massaging all breast muscles—the base, as well as the areola—it affects blood and lymph flows, and can also reduce milk stasis in the breast without any unwanted side effects. It can even reduce the pain of breast congestion and increase the breastfeeding success by stimulating the oxytocin/milk ejection reflex.(9,21,24)
The present study showed that Oketani massage had a positive effect on the frequency of breastfeeding, so that the average number of breastfeeding times from the first breastfeeding to discharge in mothers who received Oketani massage was significantly higher than the participants in the control group who received only the routine care. The duration of breastfeeding indicates breastfeeding success and, as an interactive process, will be followed by maternal satisfaction and meeting the baby’s needs.(6)
The results of the present study suggested that Oketani massage can facilitate early breastfeeding after cesarean sections. Early initiation of breastfeeding is especially important for mothers undergoing a cesarean section, and can play an important role in exclusive feeding and increasing the duration of breastfeeding.(5)
This study also indicated that the average duration of breastfeeding after the mother was transferred to the recovery room was significantly shorter among the participants in the Oketani massage group compared to the members of the control group. This study also showed that the duration of the first postoperative breastfeeding in the mothers who underwent cesarean sections was approximately three times greater compared to mothers with normal delivery,(47) and this can negatively affect the acceptance of the mother’s breast by the baby and the baby’s sucking reflex.(8)
The results of the study suggested a statistically significant difference between the two groups in terms of the need for breastfeeding support in both breastfeeding rounds, as the mothers in the intervention groups needed less support in the first and last breastfeeding before discharge compared to the participants in the control group. Oketani massage reduced the mother’s need for support by influencing the way the infant latched onto the breast, the amount of audible swallowing noted, the mother’s nipple type, and the mother’s position of holding the infant while breastfeeding. However, previous studies have suggested that mothers who undergo cesarean sections need more support to start and continue breastfeeding, and the cesarean section is one of the most important risk factors for breastfeeding problems.(5,6,7,48)
It seems that, since postpartum breast congestion can be a barrier to timely breastfeeding and mothers with breast congestion will need more support, Oketani breast massage can reduce breast congestion in mothers and thus diminish their need for breastfeeding support. Furthermore, Jamzuri et al.(41) and Kraleti et al.(49) showed that Oketani massage increased the secretion of oxytocin and prolactin, increased blood circulation in the breasts, facilitated the exit of milk from the breast, and increased milk volume which, in general, can reduce the mother’s need for support in breastfeeding.
A study by Dehghani et al.(24) showed that Oketani massage has a greater relieving effect on the severity of breast congestion than routine care. A systematic review study by Zakarija-Grkovic and Stewart (17) and a study by Dehghani et al.(24) indicated that lower breast engorgement scores in women who had received Oketani massage than those who had received routine care; but the true effect is unclear because, in the Dehghani study, the data were reported per breast instead of per woman, so the data could not be included in the analysis. Thus, it is uncertain if Oketani breast massage is more effective than routine care for breast engorgement, and it cannot be ensured that the results of this study were in line with the results of our study.
The results of the present study indicated that the self-efficacy of mothers in the intervention group was significantly higher than those in the control group. Self-efficacy is one of the predictors and effective variables of exclusive breastfeeding and its continuation,(39,40) and refers to a person’s belief in their ability to perform a specific task.(50) Since the evidence shows that a mother’s self-efficacy is related to the frequency, amount, and duration of breastfeeding,(51,52) Oketani massage may positively affect the frequency and duration of breastfeeding by increasing the self-efficacy of the mother—a claim that requires further attestation and research. One of the limitations of the present study was the use of self-report questionnaires to measure the mothers’ self-efficacy. In addition, mothers’ characteristics, their mental status, and the level of spousal support were factors that could affect the success of breastfeeding, and which were not addressed in this study.
The present study showed that Oketani massage has a positive effect on the breastfeeding success rate and can increase the number of breastfeeding times in addition to the number of breastfeeding times during the hospital stay. It also reduces the breastfeeding onset time and facilitates early breastfeeding, reducing the mother’s need for further support and improving her self-efficacy. Oketani massage can be performed as an independent and routine prophylactic intervention for all cesarean section mothers by nurses who have completed a short training course. Therefore, it is recommended to teach this massaging technique to nurses and midwives who are in contact with the mother immediately before and after delivery to promote breastfeeding efficacy and reduce breastfeeding problems.
We are thankful to all the mothers who participated and made this study feasible, and to the hospitals involved in the study for the support provided during the conduction of this study.
1 Chen H, Tan D. Cesarean section or natural childbirth? A cesarean birth may damage your health. Front Psychol. 2019;10:351.
2 Hejazi M. Comparison of personality characteristics and anxiety in pregnant women based on choosing the type of delivery. Sci J Rehab Med. 2018;7(1):51–58.
3 Kirca N, Adibelli D. Effects of the delivery type on the breastfeeding self-efficacy perception. Int J Caring Sci. 2020;13(1):698.
4 Ladewig PW, London ML, Davidson MC. Contemporary Maternal-Newborn Nursing, 8th edition. London, UK: Pearson; 2013.
5 Isik Y, Dag ZO, Tulmac OB, Pek E. Early postpartum breastfeeding effects of cesarean and vaginal birth. Ginekologia Polska. 2016;87(6):426–30.
6 Kocaöz FŞ, Destegül D, Kocaöz S. Comparison of the breastfeeding outcomes and self-efficacy in the early postpartum period of women who had given birth by cesarean under general or spinal anesthesia. J Maternal-Fetal Neonatal Med. 2019;34(10):1545–1549.
7 Chang YS, Glaria AA, Davie P, Beake S, Bick D. Breastfeeding experiences and support for women who are overweight or obese: a mixed-methods systematic review. Matern Child Nutr. 2020;16(1):e12865.
8 Hobbs AJ, Mannion CA, McDonald SW, Brockway M, Tough SC. The impact of cesarean section on breastfeeding initiation, duration, and difficulties in the first four months postpartum. BMC Pregnancy Childb. 2016;16(1):1–9.
9 Dehghani M, Babazadeh R, Khadivzadeh T, Pourhoseini SA, Esmaeili H. Effect of breast oketani-massage on neonatal weight gain: a randomized controlled clinical trial. Evidence-Based Care. 2018;8(3):57–63.
10 Awaliyah SN, Rachmawati IN, Rahmah H. Breastfeeding self-efficacy as a dominant factor affecting maternal breastfeeding satisfaction. BMC Nurs. 2019;18(1):30.
11 Guimarães CM, Conde RG, Gomes-Sponholz FA, Oriá MOB, Monteiro JC. [Factors related with breastfeeding self-efficacy immediate after birth in puerperal adolescents] [in Portuguese]. Acta Paulista de Enfermagem. 2017;30(1):109–15.
12 Rahmatnejad L, Bastani F. Factors associated with discontinuation of exclusive breastfeeding by first-time mothers. Iran J Nurs. 2011;24(71):42–53.
13 Boateng GO, Martin SL, Tuthill EL, Collins SM, Dennis CL, Natamba BK, et al. Adaptation and psychometric evaluation of the breastfeeding self-efficacy scale to assess exclusive breastfeeding. BMC Pregnancy Childb. 2019;19(1):73.
14 Soti-Ulberg C, Hromi-Fiedler A, Hawley NL, Naseri T, Manuele-Magele A, Ah-Ching J, et al. Scaling up breastfeeding policy and programs in Samoa: application of the Becoming Breastfeeding Friendly initiative. Int Breastfeeding J. 2020;15(1):Article No. 1.
15 Butcher HK, Bulechek GM, Dochterman JMM, Wagner CM. Nursing Interventions Classification (NIC)-E-Book on Vital Source, 7th edition. New York, NY: Elsevier Health Sciences; 2018.
16 Anderson L, Kynoch K, Kildea S. Effectiveness of breast massage in the treatment of women with breastfeeding problems: a systematic review protocol. JBI Evid Synthesis. 2016;14(8):19–25.
17 Zakarija-Grkovic I, Stewart F. Treatments for breast engorgement during lactation. Cochrane Database System Rev. 2020(9).
18 Lagerberg D, Wallby T, Magnusson M. Differences in breastfeeding rate between mothers delivering by caesarean section and those delivering vaginally. Scand J Pub Health. May 2020:140349482091178.
19 Cho J, Ahn HY, Ahn S, Lee MS, Hur MH. Effects of oketani breast massage on breast pain, the breast milk pH of mothers, and the sucking speed of neonates. Korean J Women Health Nurs. 2012;18(2):149–58.
20 Oketani S. Oketani’s Breast Massage Therapy. Tokyo, Japan: Bong Hwang Dang Press; 1991.
21 Kabir N, Tasnim S. Oketani lactation management: a new method to augment breast milk. J Bangladesh Coll Phys Surg. 2009;27(3):155–159.
22 Ahn S, Kim J, Cho J. Effects of breast massage on breast pain, breast-milk sodium, and newborn suckling in early postpartum mothers. J Korean Acad Nurs. 2011;41(4).
23 Foda MI, Kawashima T, Nakamura S, Kobayashi M, Oku T. Composition of milk obtained from unmassaged versus massaged breasts of lactating mothers. J Pediatr Gastroenterol Nutr. 2004;38(5): 484–487.
24 Dehghani M, Babazadeh R, Khadivzadeh T, Azam Pourhosseini S, Esmaeili H. Effect of breast oketani-massage on the severity of breast engorgement. Iran J Obstetr Gynecol Infertil. 2017;20(5):30–38.
25 WHO & UNICEF. Implementation guidance. Protecting, promoting, and supporting breastfeeding in facilities providing maternity and newborn services: the revised Baby-Friendly Hospital Initiative. Geneva, Switzerland: World Health Organization; 2018.
26 Zhang F, Yang Y, Bai T, Sun L, Sun M, Shi X, et al. Effect of pumping pressure on the onset of breastfeeding after cesarean section: a randomized controlled study. Matern Child Nutr. 2018;14(1):e12486.
27 Srivastava S, Gupta A, Bhatnagar A, Dutta S. Effect of very early skin to skin contact on success at breastfeeding and preventing early hypothermia in neonates. Indian J Pub Health. 2014;58(1):22–26.
28 Jensen D, Wallace S, Kelsay P. LATCH: a breastfeeding charting system and documentation tool. J Obstetr Gynecol Neonat Nurs. 1994;23(1):27–32.
29 Chapman DJ, Doughty K, Mullin EM, Pérez-Escamilla R. Reliability of breastfeeding assessment tools applied to overweight and obese women. J Human Lactat. 2016;32(2):269–276.
30 Altuntas N, Turkyilmaz C, Yildiz H, Kulali F, Hirfanoglu I, Onal E, et al. Validity and reliability of the infant breastfeeding assessment tool, the mother-baby assessment tool, and the LATCH scoring system. Breastfeeding Med. 2014;9(4):191–195.
31 Karimi S, Najafi Kalyani M, Naghizadeh MM, Nekoee F, Kamali M. Comparison of breastfeeding patterns in women with normal vaginal delivery and cesarean section. Iran J Obstetr Gynecol Infertil. 2011;14(6):46–53.
32 Matthews MK. Developing an instrument to assess infant breastfeeding behavior in the early neonatal period. Midwifery. 1988;4(4):154–165.
33 Walker M. Breastfeeding Management for the Clinician: Using the Evidence, 2nd ed. Sudbury, MA: Jones & Bartlett Learning; 2011.
34 Adeli M, Alirezaei S, Kabiriyan M, Rafiei F. A comparison of the effect of short abdominal skin-to-skin contact and kangaroo skin contact on the initiation of successful breastfeeding. J Babol Univ Med Sci. 2018;20(2):70–76.
35 Beiranvand S, Valizadeh F, Hosseinabadi R, Pournia Y. The effects of skin-to-skin contact on temperature and breastfeeding successfulness in full-term newborns after cesarean section. Int J Pediatr. 2014;2014: Article ID 846486.
36 Ahamd Y, Shariffar S, Pishgooie SA, Teymori F, Hoseyni MS, Yari M. Comparison of the quality of breastfeeding in postpartum mothers undergone cesarean and vaginal delivery in selected military hospitals of Tehran. Military Car Sci J. 2017;4(1):70–79.
37 Agudelo S, Gamboa O, Rodríguez F, Cala S, Gualdrón N, Obando E, et al. The effect of skin-to-skin contact at birth, early versus immediate, on the duration of exclusive human lactancy in full-term newborns treated at the Clínica Universidad de La Sabana: study protocol for a randomized clinical trial. Trials. 2016;17(1):1–9.
38 Dennis C-L, Heaman M, Mossman M. Psychometric testing of the breastfeeding self-efficacy scale-short form among adolescents. J Adolesc Health. 2011;49(3):265–271.
39 Araban M, Mehrjardi FF, Shahry P, Montazeri A. The Persian version of breastfeeding self-efficacy scale-short form (BSES-SF): translation and psychometric assessment. Payesh (Health Monitor). 2016;15(1):87–93.
40 Moafi F, H Hajnasiri H, Hosseini T, Alimoradi Z, Bajalan Z. Breastfeeding self-efficacy and its associated factors in women who gave birth in Kosar Hospital of Qazvin in 2016–2017: a descriptive study. J Rafsanjan Univ Med Sci. 2019;17(11):1003–1016.
41 Jamzuri M, Khayati N, Widodo S, Hapsari ED, Haryanti F. Increasing oxytocin hormone levels in postpartum mothers receiving oketani massage and pressure in the gb-21 acupressure point. Int J Adv Life Sci Res. 2019;2(1):22–27.
42 Lim AR, Song JA, Hur MH, Lee MK, Lee MS. Cabbage compression early breast care on breast engorgement in primiparous women after cesarean birth: a controlled clinical trial. Int J Clin Experiment Med. 2015;8(11):21335.
43 Saatsaz S, Rezaei R, Alipour A, Beheshti Z. Massage as adjuvant therapy in the management of post-cesarean pain and anxiety: a randomized clinical trial. Complement Ther Clin Pract. 2016;24:92–98.
44 Cambron JA, Dexheimer J, Coe P, Swenson R. Side-effects of massage therapy: a cross-sectional study of 100 clients. J Altern Complem Med. 2007;13(8):793–796.
45 Fogarty S, McInerney C, Stuart C, Hay P. The side effects and mother or child-related physical harm from massage during pregnancy and the postpartum period: an observational study. Complem Ther Med. 2019;42:89–94.
46 Yin P, Gao N, Wu J, Litscher G, Xu S. Adverse events of massage therapy in pain-related conditions: a systematic review. Evid-Based Complem Altern Med. 2014:Article ID 480956.
47 Permatasari TAE, Syafruddin A. Early initiation of breastfeeding related to exclusive breastfeeding and breastfeeding duration in rural and urban areas in Subang, West Java, Indonesia. J Health Res. 2016;30(5):337–345.
48 Wood NK. Home-based interventions in a case of first latch at 27 days. Nurs Women’s Health. 2019;23(2):135–140.
49 Kraleti SK, Lingaldinna S, Kalvala S, Anjum S, Singh H. To study the impact of unilateral breast massage on milk volume among postnatal mothers—a quasi-experimental study. Indian J Child Health. 2018;5(12):731–734.
50 Bandura A. Self-efficacy: toward a unifying theory of behavioral change. Psychol Rev. 1977;84(2):191.
51 Ngo LTH, Chou HF, Gau ML, Liu CY. Breastfeeding self-efficacy and related factors in postpartum Vietnamese women. Midwifery. 2019;70:84–91.
52 Brockway M, Benzies K, Hayden KA. Interventions to improve breastfeeding self-efficacy and resultant breastfeeding rates: a systematic review and meta-analysis. J Human Lact. 2017;33(3):486–499.
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 14, NUMBER 3, September 2021