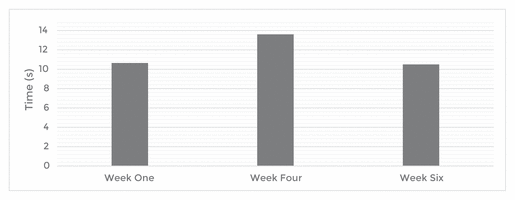
Figure 1 TUG Test Results from Sitting, Walking Three Metres Without a Cane, and Returning to Sitting
Amy Frost-Hunt, RMT
Massage Therapy Program, MacEwan University, Edmonton, AB.Background:
Multiple Sclerosis (MS) is characterized by degeneration of the myelin sheath of an axon resulting in decreased transmission of nerve impulses. It is an autoimmune disease with periods of exacerbation and remission. Types of MS include relapsing-remitting, acute progressive, chronic progressive attack-remitting, and benign. Symptoms vary from patient to patient. Common symptoms include fatigue, spasticity, swelling, and altered gait. MS is commonly treated with medications that help relieve symptoms and prolong disease progression. Massage Therapy (MT), specifically Swedish techniques, have been effective in treating MS.
Objective:
To examine the effects of MT on mobility, fatigue, and edema in a patient with MS.
Methods:
An MT student from MacEwan University’s 2,200-hour Massage Therapy program administered five MT treatments over a six-week period to a 58-year-old female diagnosed with MS 11 years earlier. She presented with symptoms of decreased mobility, fatigue, and left ankle edema. Assessment included active and passive range of motion (ROM), myotomes, dermatomes, reflexes, and orthopedic tests. Goals for the treatment sessions were to increase mobility, decrease fatigue, and decrease edema. Assessment measures included the Timed-Up-and-Go (TUG) test for mobility, the Modified Fatigue Impact Scale (MFIS) to measure fatigue, and Figure-8 ankle measurement to measure edema. Techniques used included Swedish massage, passive ROM, manual lymphatic drainage (MLD), and home-care exercises.
Results:
Little change was noted in mobility. The patient’s fatigue level and left ankle edema decreased.
Conclusion:
The results suggest that MT is effective in reducing fatigue and edema in a patient with MS. Future studies are needed to evaluate the correlation between mobility and massage.
KEYWORDS: Multiple Sclerosis, massage therapy, fatigue, mobility, edema
Multiple Sclerosis (MS) is a progressive, inflammatory, autoimmune disease marked by periods of exacerbation and remission, resulting in demyelination of nerve axons throughout the brain and spinal cord.(1–3) Myelin sheaths surround axons providing insulation and increasing speed of transmission.(1) With demyelination, a sclerotic plaque forms which causes nerve transmissions to be slowed, interrupted, or blocked; the more plaque, the worse the symptoms.(1) During early phases, regeneration of myelin occurs from oligodendrocytes. Over time these fatigue, reducing regeneration.(1) With disease progression, symptoms worsen, periods of remission become shorter, and lesions appear along the spinal cord.(3) Most individuals affected are between the ages of 20 and 45.(2) Women are affected twice as often as men.(2) MS is multifactorial with a wide variety of genetic, environmental, viral, and immunological influences.(1) Patients with MS often present with cognitive impairment correlated with muscle atrophy.(4,5) There is an increased risk for intracranial hemorrhage.(6)
There are various forms of MS: relapsing-remitting, acute progressive, chronic progressive, and benign. The most common form, relapsing-remitting, involves repeated periods of exacerbation and remission. Acute progressive MS involves continuous worsening and rapid progression of symptoms without remission. Chronic progressive MS is characterized by an initial period of exacerbation and remission and then continuous progression of symptoms without further remissions. The remission periods become less frequent resulting in greater disability. Benign MS is a mild form of MS characterized by few exacerbations and complete recovery.(1)
The signs and symptoms of MS vary and may include tingling, numbness, blurred vision, and slurred speech.(1) Fatigue is common and can increase these symptoms.(1) Spasticity, paresthesia, cold extremities, sweating, and mood swings are also common.(1) Other symptoms include cardiomyopathy, pulmonary edema, swelling, and orthostasis.(1,7) Altered posture and gait often occur due to muscle imbalances, weakness, and spasticity.(8) Patients with MS often have slower walking speeds and longer periods of double limb support, and these deficits increase with disease progression.(8)
Prescription medication is most commonly used to treat symptoms and delay disease progression.(9–14) Intravenous immunoglobulin treatments have been effective.(15) Non-pharmacological treatment includes reflexology, hydrotherapy, and transcutaneous electrical nerve stimulation.(16) MT, particularly Swedish techniques, has been effective in reducing deficits associated with MS, including gait speed—both alone and with exercise programs.(17–19)
There is limited research on the effects of MT on edema, fatigue, and mobility in patients with MS. Further research is needed to help therapists provide more effective and comprehensive treatments. The objective of this case report was to examine the effects of MT on mobility, fatigue, and edema in a patient with MS.
A 58-year-old retired female presented to the MacEwan Massage Therapy Clinic with decreased mobility, fatigue, left ankle edema, and occasional left lower leg muscle spasms due to MS. The patient’s history included: left ankle fracture, torn left knee meniscus, kidney stones, and a cholecystectomy. She reported depression, bladder leakage, and high cholesterol; all managed with medications. She was diagnosed with MS 11 years before the initial assessment; the type was unknown.
Previously, the patient used reflexology, MT, and yoga to manage MS. Although she experienced relief with these treatments, she did not use them in addition to her home care. The patient self-regulated activity based on fatigue level.(17)
The patient’s major complaints were low energy and limited control of her left leg, causing frustration. The patient occasionally experienced aching in her low back. Her goals for treatment were to increase well-being and energy.
The therapist performed a lumbar scan which included active and passive range of motion (ROM), myotomes, dermatomes, reflexes, and peripheral joint active movements.(20) The patient had an antalgic gait and used a cane in her right hand. Postural analysis revealed pes planus bilaterally, elevation of her right hip, an anterior pelvic tilt, a depressed right shoulder, and a head tilt to the right. Her left foot was ahead of the right in standing. There was slight lumbar pain with overpressure on flexion.(20) The therapist was unable to test myotomes on the left because of generalized marked weakness. Sensation was altered along the L5 dermatome.(20) Special tests performed on the knee included Anterior and Posterior Drawer Signs to rule out cruciate ligament sprains or tears, Clarke’s test to rule out patellofemoral dysfunction, and McMurray’s test to rule out meniscal injuries.(20) Bilateral figure-8 measurements revealed left ankle edema. Tinel’s sign was used to rule out tarsal tunnel syndrome.(20) Anterior Drawer sign was used to rule out deltoid, tibionavicuar, anterior talofibular, posterior talofibular, and calcaneofibular ligament injuries.(20) Morton’s test was used to rule out neuroma and metatarsal stress fractures.(20) All knee and ankle special tests were negative. Varus and Valgus stress tests on the left knee, and Homan’s sign and Talar Tilt test on the left ankle were not performed due to decreased ROM and general weakness. The patient was unable to actively move her left ankle, and passive dorsiflexion was drastically limited. Palpation revealed hypertonicity of the patient’s iliotibial bands and quadratus lumborum bilaterally, the left hamstrings and quadriceps, and the right gastrocnemius.
Assessment and MT treatments were conducted by a MacEwan University student in her fifth of six semesters of a 2,200-hour Massage Therapy Program.
The main goals for the treatments were to increase mobility and decrease fatigue and left ankle edema, which would help reach the patient’s goals of increased well-being and energy. Due to the patient’s complaints of occasional low back aching, the therapist included treatment on her back. The first session was used primarily for assessment. The following five sessions held at the same day, time, and place, consisted of 50-minute treatments, plus 10 minutes for assessment and evaluation of previous treatment. The patient’s progress was monitored using the Timed-Up-and-Go (TUG) test,(21–23) Modified Fatigue Impact Scale (MFIS),(24–26) and Figure-8 ankle measurements.(27–29) The use of vigorous techniques and heat was contraindicated due to the possibility of increasing fatigue.(1,30) Deep techniques were contraindicated in areas of altered sensation.(1) Cold hydrotherapy was contraindicated due to the patient’s sensitivity to cold. No hydrotherapy was used due to these contraindications.(1,30)
The therapist began treatment on the patient’s back with the patient in prone with a pillow under the ankles. Working bilaterally, the therapist used longitudinal palmar stroking for 15 seconds to spread lotion and prepare the tissue for further massage, followed by wringing bilaterally for 15 seconds.(1,31) Unilaterally, open c-kneading, palmar and specific fingertip kneading were used for two minutes on each side to decrease aching, flush tissues, and promote relaxation.(1,31,32) Wringing and longitudinal palmar stroking were used bilaterally for 30 seconds to flush out the tissues, preventing longstanding hyperemia.(31) The therapist moved onto the legs, always treating the unaffected leg first, working proximal to distal to proximal to aid in circulation towards the heart.(31) Starting on the posterior aspect of the upper leg, the therapist used longitudinal palmar stroking and wringing for one minute to prepare the tissues for further massage.(31) Open c-kneading and knuckle kneading were then used for two minutes to promote relaxation.(1,31,32) The therapist proceeded with knuckle kneading on the gluteal muscles for one minute to relieve aching in the low back.(31) The therapist moved onto the lower legs using the same techniques used on the upper legs, as well as specific fingertip kneading for three minutes to promote relaxation.(1,31,32) The therapist spent one minute on the foot using kneading and stroking techniques to further promote relaxation.(31,32) Two minutes were spent flushing out the entire posterior aspect of the leg using wringing and longitudinal palmar stroking.(1,31,32) This sequence was repeated on the posterior aspect of the left leg with the addition of Golgi Tendon Organ (GTO) technique performed on gastrocnemius to reduce spasticity. The GTO technique is performed by applying a direct compression on the tendon near the musculotendinous junction for a minimum of 30 seconds.(1) Pain free passive ROM of the knee and ankle to promote blood flow and nutrition of the joints was also used on the left leg.(1,17,31)
The patient was moved into supine with a pillow placed under her knees. The same techniques used to promote relaxation were repeated on the anterior aspect of each leg for ten minutes per leg.(1,31,32) Lastly, manual lymphatic drainage (MLD) was used for three minutes. The therapist started by stimulating the lymph nodes bilaterally with gentle pressure, from the clavicular to the superficial inguinal.(33) MLD was performed using gentle, non-gliding, rhythmical strokes in an upwards direction from the left inguinal pump down to the left ankle to decrease edema.(33–36)
This treatment plan was used during every treatment session.
During the fifth session, MLD was also used as outlined above on the right leg to decrease swelling in her right ankle due to a reported increase in salt intake the night before.(33) During the fifth week, the patient’s husband was admitted to the hospital, resulting in increased stress. To reduce stress, the therapist focused on relaxation and instructed the patient to practice diaphragmatic breathing.(1) These were the only changes to the treatment plan.
The patient was given a home-care sheet at the end of the second session and the therapist inquired about home care every session. Home care included drinking one or two extra glasses of water post-treatment, using self-assisted ankle ROM, and self-MLD. The patient was instructed to use a towel wrapped around her left foot and bring her ankle through all ranges by pulling on different areas of the towel. The patient was instructed to do two repetitions, twice daily, without increasing her fatigue level. Self-assisted ROM was used to promote movement of her ankle and increase joint nutrition.(37) For self-MLD the patient was instructed to elevate her ankle to promote drainage and to stimulate the superficial inguinal lymph nodes, and to use gentle, short, non-gliding strokes towards the pump as she moved from the pump down to her ankle, once daily.(31,33–36) Self-MLD was used to manage or reduce edema outside of the treatment sessions.(34–36)
Mobility was measured using the TUG test due to its reliability and validity.(21–23) The patient was timed as she stood from sitting, walked three meters without her cane, and returned to sitting. This test was administered at the beginning of the first, fourth, and last sessions. A score of 14 seconds or more indicates a risk of falling.(38) The MFIS is a reliable and valid 21-item questionnaire which assesses fatigue in individuals with MS.(24–26) It is scored out of 84 points; the higher the score the greater the impact of fatigue on daily activities.(24) It was administered at the end of the initial and final sessions. The figure-8 ankle measurement has been reported to be reliable and valid and was used to measure left ankle edema.(20,27–29) Her right ankle was measured for comparison. Figure-8 measurements were taken pre- and post-treatment during the second through sixth sessions. An average of three measurements was recorded each time.(20)
Verbal and written consent were obtained during the initial assessment and included therapist qualifications, confidentiality, risks and benefits, clinical findings, positioning, types and purposes of techniques, and treatment plan. The patient was encouraged to ask questions and informed she could alter or stop treatments at any time. Informed consent was obtained every session and when the therapist altered treatment.
There was an increase in the time for the patient to complete the TUG test during the fourth session; however, the patient’s mobility remained the same between the first and last treatments overall (see Figure 1). The timing to complete the TUG test was within normal range in the first and last sessions, but below normal during the fourth sessions.(21,22) There was a slight decrease in fatigue (see Figure 2). The patient reported increased energy throughout the treatments. Other than a slight increase from Week Four to Week Five, overall there was a decrease in left ankle edema. Edema decreased pre- to post-treatment. Little variation was seen in the measurements of the right ankle, except for slight swelling during the fifth week (see Figure 3).
|
|
||
|
Figure 1 TUG Test Results from Sitting, Walking Three Metres Without a Cane, and Returning to Sitting |
||
|
|
||
|
Figure 2 MFIS Total Scores |
||
|
|
||
|
Figure 3 Figure-8 Measurements of Anklesa |
||
The patient stated her spasms completely stopped over the course of treatment. The patient attended all appointments, was diligent with performing home care, and massage. and reported home care improved her function and decreased her left ankle edema. She expressed gratitude in meeting her treatment goals.
MT did not improve this patient’s mobility. In one study of 48 participants with MS, TUG test scores improved following MT, which differs from the results in this case report.(18) In the cited study, participants received MT, exercise therapy, or both. The participants in all three treatment groups improved, and the participants who received MT without exercise therapy had the best results. The finding suggests that MT can have positive effects in increasing mobility.(18) The lack of improvement in the mobility of the patient in this case report could be due to the chronicity of the condition. It is feasible that, as MS progresses, walking speed becomes slower and periods of double limb support become longer. The study of 48 participants by Negahban et al.(18) focused on relapsing-remitting MS. The patient in this case report was unsure about her type of MS which could have affected the results. The Negahban study measured 2-minute walk test (2MWT) times as well as TUG scores, whereas this case study only measured TUG scores. It is possible that, had the therapist also used the 2MWT as an assessment measure, a change in mobility could have been seen. At the beginning of the fourth session, the patient indicated she felt unusually tired, sluggish, and fatigued, which could explain the increase in TUG time.
Fatigue decreased with the use of MT, supported by the MFIS.(24–26) A study of MT treatment including 28 participants with MS revealed reduced MFIS scores from the first to the last treatments.(17) The decrease in fatigue seen could be due to the relaxation experienced during a Swedish massage.(31)
With MT, edema decreased as supported by Figure-8 measurements of the ankle.(27–29) There is limited research on edema reduction using MT in patients with MS; however, multiple studies have shown that MLD is effective in reducing edema.(39,40) A study with 47 participants compared the effectiveness of postural drainage to MLD in reducing lower limb edema after bariatric surgery.(34) Results showed MLD to be more effective than postural drainage and supports that MLD is effective in reducing lower limb edema.(34) The increase in the patient’s left ankle edema and swelling in the right ankle in the fifth week could have been due to the patient’s reported ingestion of salty foods the night before treatment. Studies have shown salt intake can affect the lymphatic system, resulting in swelling.(41)
Patient compliance with home care likely contributed to the positive outcome in this case report; these results may not have been seen had the patient been non-compliant.
There were a number of limitations in this case report. This case report involved one patient; having more participants in this case study would have produced more information for analysis. Longer treatment durations are shown to be more effective in chronic conditions.(31) It is feasible that a longer study period would provide more positive results. The previously-mentioned study that showed MT could improve TUG scores used 15 treatment sessions, compared to the 5 treatment sessions in this case report.(18) There was no follow-up with the patient after the treatment sessions; therefore, long-term effects of treatment could not be determined. External factors, such as cold weather and visiting her husband in the hospital, may have increased the patient’s fatigue and decreased her mobility, altering the results of the MFIS and TUG test.
There is limited research on the effectiveness of MT in treating MS. Most studies focus on Swedish techniques; further research is needed to evaluate the effects of other massage techniques.(17–19) Further research on the effects of MT on mobility and walking speed in MS patients, and the correlation between MT and exercise, would help massage therapists develop a greater understanding of and ability to design appropriate and effective treatment protocols.(18) Despite limitations in this study, MT appeared to be effective in managing this patient’s symptoms associated with MS.
This study suggests that MT is effective in reducing fatigue and edema in a patient with MS. Future studies are needed to evaluate the correlation between mobility
The author would like to extend the sincerest form of gratitude to the staff and faculty of MacEwan University’s Massage Therapy Program for their ongoing support and encouragement. A special thank you to Lois Wihlidal for her continuous support and guidance throughout this case report, and for always going above and beyond.
The author declares there are no conflicts of interest.
1 Rattray F, Ludwig L. Clinical Massage Therapy: Understanding, Assessing and Treating Over 70 Conditions. Elora, ON: Talus Incorporated; 2009.
2 Damjanov I. Pathology for the Health Professions, 5th ed. St. Louis, Missouri: Elsevier; 2017.
3 Myers T, Vora S, Patterson J, Willard JM, Catalano P. Mosby’s Dictionary of Medicine, Nursing, and Health Professions, 10th ed. St. Louis, MO: Elsevier; 2017.
4 Fenu G, Fronza M, Lorefice L, Arru M, Coghe G, Frau J, et al. Performance in daily activities, cognitive impairment and perception in multiple sclerosis patients and their caregivers. BMC Neurol. 2018; 18(1):212.

5 Eijlers A, Meijer K, van Geest Q, Geurts J, Schoonheim M. Determinants of cognitive impairment in patients with multiple sclerosis with and without atrophy. Radiology. 2018; 288(2):544–551.
6 Zulfiqar M, Qeadan F, Ikram A, Farooqui M, Richardson SP, Calder CS, et al. Intracerebral hemorrhage in multiple sclerosis: a retrospective cohort study. J Stroke Cerebrovasc Dis. 2019;28(2):267–275.
7 Bayer AD, Cahill JF, Rizvi SA. Multiple sclerosis relapse presenting as an acute cardiomyopathy. Mult Scler Relat Disord. 2019;27:7–8. doi:10.1016/j.msard.2018.09.021.
8 Storm FA, Nair KP, Clarke AJ, van der Meulen JM, Mazzà C. Free-living and laboratory gait characteristics in patients with multiple sclerosis. PLoS One. 2018;13(5):e0196463.

9 Miller A. Handbook of Relapsing-Remitting Multiple Sclerosis. New York City, NY: Springer International Publishing; 2017.
10 Pakdaman H, Abbasi M, Gharagozli K, Ashrafi F, Kasmaei HD, Harandi AA. A randomized double-blind trial of comparative efficacy and safety of Avonex and CinnoVex for treatment of relapsing-remitting multiple sclerosis. Neurol Sci. 2018;39(12): 2107–2113.
11 Diaz GM, Hupperts R, Fraussen J, Somers V. Dimethyl fumarate treatment in multiple sclerosis: Recent advances in clinical and immunological studies. Autoimmun Rev. 2018;17(12):1240–1250.
12 Rasche L, Paul F. Ozanimod for the treatment of relapsing remitting multiple sclerosis. Expert Opin Pharmacother. 2018;19(18):20173–20186.
13 Dumitrescu L, Constantinescu CS, Tanasescu R. Siponimod for the treatment of secondary progressive multiple sclerosis. Expert Opin Pharmacother. 2019;20(2):143–150.
14 Ceronie B, Jacobs BM, Baker D, Dubuisson N, Mao Z, Ammoscato F, et al. Cladribine treatment of multiple sclerosis is associated with depletion of memory B cells. J Neurol. 2018;265(5):1199–1209.

15 Berkovich R. Treatment of acute relapses in multiple sclerosis. In: Aron R, Miller A, eds. Translational Neuroimmunology in Multiple Sclerosis. 2016:307–326.
16 Amatya B, Young J, Khan F. Non-pharmacological interventions for symptoms of Multiple Sclerosis. Cochrane Database Syst Rev. 2018;12.
17 Backus D, Manella C, Bender A, Sweatman M. Impact of massage therapy on fatigue, pain, and spasticity in people with multiple sclerosis: a pilot study. Int J Ther Massage Bodywork. 2016;9 (4):4.

18 Negahban H, Rezaie S, Goharpey S. Massage therapy and exercise therapy in patients with multiple sclerosis: a randomized controlled pilot study. Clin Rehabil. 2013;27(12):1126–1136.
19 Schroeder B, Doig J, Premkumar K. The effects of massage therapy on multiple sclerosis patients’ quality of life and leg function. Evid Based Complement Alt Med. 2014;2014:1–8.
20 Wihlidal L. MTST 156: Assessment for Massage Therapists II [course description]. Edmonton, AB: MacEwan University; 2018. p.47–55.
21 Lyders Johansen K, Derby Stistrup R, Skibdal Schjøtt C, Madsen J, Vinther A. Absolute and relative reliability of the Timed ‘Up & Go’ test and ’30 second Chair-Stand’ test in hospitalized patients with stroke. PLoS One. 2016;11(10).

22 Chan PP, Tou JIS, Tse MM, Ng SS. Reliability and validity of the timed up and go test with a motor task in people with chronic stroke. Arch Phys Med Rehab. 2017;98(11):2213–2220.
23 Dobson F. Timed Up and Go test in musculoskeletal conditions. J Physiother. 2015;61(1):47.
24 Mathiowetz V. Test-retest reliability and convergent validity of the Fatigue Impact Scale for persons with multiple sclerosis. Am J Occupat Ther. 2003;57(4):389–395.
25 Kos D, Kerckhofs E, Nagels G, D’Hooghe Bd, Duquet W, Duportail M, et al. Assessing fatigue in multiple sclerosis: Dutch modified fatigue impact scale. Acta Neurol Belg. 2003;103(4)105–191.
26 Learmonth Y, Dlugonski D, Pilutti L, Sandroff B, Klaren R, Motl R. Psychometric properties of the fatigue severity scale and the modified fatigue impact scale. J Neurol Sci. 2013;331(1–2):102–107.
27 Petersen EJ, Irish SM, Lyons CL, Miklaski SF, Bryan JM, Henderson NE, et al. Reliability of water volumetry and the figure of eight method on subjects with ankle joint swelling. J Orthop Sports Phys Ther. 1999;29(10):609–615.
28 Mawdsley RH, Hoy DK, Erwin PM. Criterion-related validity of the figure-of-eight method of measuring ankle edema. J Orthop Sports Phys Ther. 2000;30(3):149–153.
29 Reis F, Ribeiro EA, Carvalho P, Belchior AC, Arakaki JC, Vasconcelos RA. Analysis of the figure-of-eight method and volumetry reliability for ankle edema measurement. Rev Bras Med Esporte. 2004;10(6):468–471.
30 Bol Y, Smolders J, Duits A, Lange IMJ, Romberg-Camps M, Hupperts R. Fatigue and heat sensitivity in patients with multiple sclerosis. Acta Neurol Scand. 2012;126(6):384–389.
31 Andrade CK. Outcome Based Massage: Putting Evidence into Practice, 3rd ed. Baltimore, MD: Lippincott Williams & Wilkins; 2014.
32 Jane S-W, Chen S-L, Wilkie DJ, Lin YC, Foreman SW, Beaton RD, et al. Effects of massage on pain, mood status, relaxation, and sleep in Taiwanese patients with metastatic bone pain: a randomized clinical trial. ISRN Pain. 2011;152(10):2432–2442.
33 Chikly B. Silent Waves: Theory and Practice of Lymph Drainage Therapy: an Osteopathic Lymphatic Technique, 3rd ed. Scottsdale, AZ: The Chikly Health Institute; 2017.
34 Bertelli DF, Oliveira PD, Gimenes AS, Moreno MA. Postural drainage and manual lymphatic drainage for lower limb edema in women with morbid obesity after bariatric surgery: a randomized controlled trial. Am J Phys Med Rehabil. 2013;92(8):697–703.
35 Duman I, Ozdemir A, Tan AK, Dincer K. The efficacy of manual lymphatic drainage therapy in the management of limb edema secondary to reflex sympathetic dystrophy. Rheumatol Int. 2009;29(7):759–763.
36 Bongi SM, Rosso AD, Passalacqua M, Miccio S, Cerinic MM. Manual lymph drainage improving upper extremity edema and hand function in patients with systemic sclerosis in edematous phase. Arthritis Care Res. 2011;63(8):1134–1141.
37 Kisner C, Colby LA. Therapeutic Exercise: Foundations and Techniques, 6th ed. Philadelphia, PA: F. A. Davis; 2012.
38 Shumway-Cook A, Brauer S, Woollacott M. Predicting the probability for falls in community-dwelling older adults using the Timed Up & Go test. Phys Ther. 2000;80(9):896–903.
39 Pinto e Silva MP, Bassani MA, Miquelutti MA, Marques Ade A, do Amarai MT, de Oliveira MM, et al. Manual lymphatic drainage and multilayer compression therapy for vulvar edema: a case series. Physiother Theory Pract. 2015;31(7):527–531.
40 Reiss M, Reiss G. [Manual lymph drainage as therapy of edema in the head and neck area.] [in German] Praxis. 2003;92(7):271–274.
41 Kanbay M, Chen Y, Solak Y, Sanders PW. Mechanisms and consequences of salt sensitivity and dietary salt intake. Curr Opin Nephrol Hypertens. 2011;20(1):37–43.

COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
INTERNATIONAL JOURNAL OF OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 13, NUMBER 4, December 2020