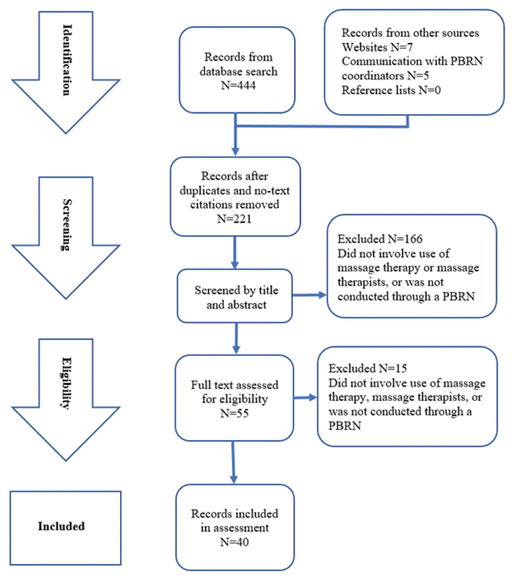
Figure 1 Literature search and eligibility steps.
Samantha Zabel, MA1*, Niki Munk, PhD, LMT1,2
1Department of Health Sciences, Indiana University School of Health and Human Sciences—IUPUI, Indianapolis, IN, USA
2Australian Research Centre in Complementary and Integrative Medicine (ARCCIM), University of Technology Sydney, Ultimo NSW, Australia
Background:
Practice-based research networks (PBRNs) are means to connect practitioners with researchers and increase the body of rigorous research. PBRNs have been used in medicine for decades, but efforts to create PBRNs in massage therapy (MT) are limited.
Purpose:
Examine and describe the amount of and nature of MT-related publications derived from PBRN-supported endeavors.
Publication Selection:
Databases: Scopus, CINAHL, PubMed, ClinicalKey, EMBASE, Google Scholar. Keywords: massage, massage therapy, practice-based research network, PBRN. Key items: publication year, operating PBRN, article type, study design, general theme, massage therapist involvement/MT application. Inclusion Criteria: studies conducted through a PBRN using MT/massage therapists as an investigated factor; articles/editorials focused on PBRN-related MT research.
Results:
Initial database search resulted in 444 records; 40 articles included in analysis from database search, PBRN website access, and PBRN staff contacts. Publication dates ranged from 2005 to 2019, with nearly all published since 2013. Nine PBRNs published 29 articles based on 20 studies and sub-studies as research papers (n=21) or poster/oral presentation abstracts (n=8), and articles discussing the need for PBRNs in MT (n=8). Most research studies were conducted as surveys (n=21), examining practice characteristics (n=9) and patient perspectives/utilization (n=7). Three articles discussing PBRNs in MT were not connected to any specific PBRN.
Conclusion:
The PBRN model holds promise to further the field of MT, but implementation needs significant development. Promoting the creation and growth of massage-specific PBRNs should be a focus of professional associations and research institutions to expand the body of scientific evidence supporting MT. While the United States has had the most PBRN-related research efforts, a sustainable implementation model is not evident as highlighted by inactivity from US-based PBRNs after initial productivity. An Australian PBRN may serve as a needed sustainability model for massage-related PBRNs in the US if their productivity trajectory continues.
KEYWORDS: massage therapy, practice- based research networks, BraveNet, MassageNet, MNO-PBRN, PRACI
Practice-based research networks (PBRNs) have been used to facilitate medical and health care research for decades.(1) Since the beginning of the 21st century, PBRNs have rapidly grown in number and their impact on health-care research is significant.(2–4) The Agency for Healthcare Research and Quality (AHRQ) defines a PBRN as a group of 15 or more practices that have a common goal and mission toward answering research questions and improving the quality of health care, and that utilizes communication and input from its members.(5) As of January 2019, there are 186 PBRNs registered with the AHRQ, operating in all 50 states and in more than 25 countries.(5) The AHRQ provides support and funding for research projects by registered groups, and facilitates educational and outreach programs. Grants are awarded through the National Institutes of Health, prioritizing research in primary care and patient outcomes relating to the opioid crisis, insurance coverage and affordability, patient safety, and more.(6) While originally developed in the 1970s in the United States to support and function within primary care(3) and subsequently joined by related health disciplines such as complementary and integrative medicine (CIM), the PBRN framework provides opportunity to other related disciplines to develop the infrastructure to support an approach to research that is directly relatable to practitioners in the field.
Practitioners in many of the various disciplines within CIM generally have insufficient exposure to research methods and literacy.(7–9) Because CIM practitioners often operate within independent solo or group practices,(10) they may not have an association with or support from research-involved institutions such as universities or large hospitals. This lack of experience and support can make involvement in research difficult. As CIM practitioners begin to see value in research and as researchers begin to understand the potential for CIM in health care, CIM-related PBRNs have begun to emerge seeking to connect practitioners and researchers, and to develop CIM research that directly impacts practitioners and patients.(11)
PBRNs that focus on CIM are a recent development. The first PBRN to focus on CIM was BraveNet, organized in 2007 as a part of the Bravewell Collaborative.(12) There are only a few PBRNs that focus on CIM approaches; a search of the AHRQ database identifies four: BraveNet, MassageNet, Massage Northern Ohio PBRN (MNO-PBRN), and Practitioner Research and Collaboration Initiative (PRACI). BraveNet and PRACI focus on CIM in general, and include massage alongside other modalities like chiropractic and yoga. MassageNet and MNO-PBRN focus specifically on massage.
BraveNet was founded with the goals of promoting the growth of integrative medicine alongside allopathic medicine and its health and economic benefits. Through BraveNet, a database of patients—the Patients Receiving Integrative Medicine Interventions Effectiveness Registry (PRIMIER)(13)—was developed to examine the use and effectiveness of different CIM modalities, including massage, acupuncture, and chiropractic. PRIMIER longitudinally tracks medical conditions and use of CIM to evaluate patient-reported outcomes. The main scholarly publication discussing PRIMIER’s preliminary results did not include massage therapy. (13) BraveNet and its parent organization, the Bravewell Collaborative, ended operations in 2015 after achieving its mission of contributing to the advancement of integrative medicine.(14)
PRACI is a PBRN focused on CIM and is located in Australia.(15) PRACI was launched in 2015 and has become the largest PBRN of its kind in the world. PRACI members include practitioners from many different CIM-related fields including acupuncture, herbal medicine, nutrition, naturopathy, yoga, reflexology, and massage therapy. Their goals include supporting communication and collaboration among practitioners and researchers, and developing relevant research that informs patient care.
Two PBRNs registered at ARHQ focus specifically on MT: MNO-PBRN and MassageNet. Massage Northern Ohio PBRN (MNO-PBRN),(16) located in Cleveland, Ohio, seeks to educate the public, health-care providers, and policy makers about MT, as well as conduct research on massage and its effects through practitioner contributions and participation. Additional goals of the group include the promotion of MT as a component of health care through research and education. MassageNet, located in Illinois, was founded in 2009 with funding from the Massage Therapy Foundation.(17) Their goal is to facilitate communication and collaboration between massage therapists, students, educators, and researchers in order to better understand real-world happenings and application of massage in practice and to provide better patient care.
There is great potential for the use of the PBRN model in all areas of health care, including MT. PBRNs in primary care and internal medicine,(18) dental medicine,(19) CIM in general,(11) and other fields are capable and productive, but PBRN research specifically related to the field of massage therapy has not yet been examined. This scoping review explores the state of MT-related literature connected to PBRNs to determine the quantity, type, and characteristics of research and publications, as well as the potential contributions of PBRNs to massage therapy research.
A scoping review is a rigorous method of knowledge synthesis. Unlike other methods of knowledge synthesis, a scoping review does not generally assess the quality of literature. Instead the purpose of a scoping review is to identify key concepts and characteristics of the literature within a topic.(20) This method was selected because a scoping review is well-suited for topics that may be complex or not yet extensively reviewed.(21) Scoping review methods were based on guidelines provided by the Joanna Briggs Institute.(22)
This scoping review intended to examine the literature comprehensively and involved four steps: search for relevant literature, literature selection based on inclusion criteria, data extraction, and results reporting. Scoping review steps are not necessarily consecutive; to ensure comprehensiveness, scoping review steps may be repeated as necessary. The first three steps of the scoping review are described within this Methods section and are followed by the final scoping review step in the Results section.
This scoping review sought to include all peer reviewed and research study report publications related to PRBNs and with a massage therapy focus. Publications could be abstracts, research papers, commentaries, or editorials. Literature that was not peer reviewed or reporting results of a research study such as periodical articles, website information, or online information sources (e.g., blogs, YouTube) were excluded from this scoping review. Included literature must have met one of two key criteria to be included in this scoping review. Either the publication had to derive from a study conducted through a PBRN and use massage therapy or massage therapists as an investigated factors; or the publication had to be an article or editorial in a peer-reviewed publication that commented specifically on the state of or need for PBRNs in MT research. Included literature was not required to have been published in association with an existing PBRN. Literature had to have been available in English.
Search strategies included database searches, examination of article reference lists, known PBRN websites, and communication with relevant PBRN coordinators. A librarian assisted with the location of literature and identification of databases and keywords. An initial database search was performed between October and December 2018 using the keywords “massage”, “massage therapy”, “practice-based research network”, and “PBRN”, and updated in November 2019 to include all records published through October 2019. Records were drawn from Google Scholar, CINAHL, PubMed, ClinicalKey, EMBASE, and Scopus. Two additional databases, Alt Health Watch and Health Source, were searched, but no relevant results were found.
Figure 1 shows the process of selection of articles for analysis. Database search results were screened by title for initial eligibility, followed by abstract screening for keywords and relevance. Full-text articles were then examined for final selection for inclusion in the analysis.
|
|
||
|
Figure 1 Literature search and eligibility steps. |
||
An Excel spreadsheet was developed to record key article aspects using standardized coding and qualitative statements. Key extracted data included: year of publication, operating PBRN, publication type, purpose, topic, study design (if applicable), field of clinician(s) performing the massage, randomization, interventions involved, number of participants, medical conditions being investigated, measures used, study length, and study results.
Figure 1 is a flow chart of the scoping review’s literature search and article selection. The initial database search in the fall of 2018 resulted in a total of 414 records, of which approximately 6% (n=24) of the publications met inclusion criteria. An additional 12 literature items were included in the scoping review by searching PBRN websites and contacting PBRN staff directly, for a total of 36 included publications. The search was updated in October 2019, resulting in an additional 30 database records, of which four publications met inclusion criteria. All included publications were unique; however, some individual studies have produced more than one paper and some included publications are poster or oral presentation abstracts that then went on to be published as papers. A total of 20 research studies and sub-studies produced 29 articles and presentation abstracts, in addition to 11 commentaries and other non-study publications, all treated as individual publications in this analysis.
An assessment of the articles addressed six components: year of publication, operating PBRN, type of article, type of study design, general theme of article, and active use of massage or massage therapists.
Figure 2 is a graph displaying the distribution of included publications by year. In general, the scoping review found that literature coming out of PBRNs regarding MT is a relatively recent development. The earliest article found was published in 2005,(23) and almost two-thirds were published within the last five years (2015–2019).(11,24–48)
|
|
||
|
Figure 2 Publication by year. |
||
Table 1 shows the distribution of publications among different PBRNs. A total of nine PBRNs have been part of studies involving MT, the most prolific being BraveNet, with eight publications,(27,35,49–54) followed by PRACI with six.(25,37,38,41,45,55) MNO-PBRN has published five works.(28,30,31,36,46) MassageNet(32,44,56,57) and the Australian Chiropractic Research Network (ACORN)(33,34,40,47) have each published four works. The Kentucky Ambulatory Network (KAN)(39,58,59) and the Population Based Palliative Care Research Network (PoPCRN)(23,60,61) have each published three articles. The Osteopathy Research and Innovation Network (ORION) has published two study papers,(42,48) and another study has come out of an unspecified PBRN.(24) Three additional commentaries discuss the need for PBRNs in CIM and MT,(26,29,43) and a literature review assesses CIM-related literature coming out of PBRNs,(11) but these are not connected to any one PBRN.
The two PBRNs that specifically work in MT research, MassageNet and MNO-PBRN, have produced a handful of studies each.(28,30–32,36,44,46,56,57) PRACI has not yet published any studies that involve the application of MT, but their website states that a comparative effectiveness study using MT is currently being performed.(15)
Three general article categories emerged from the scoping review and are arranged in Table 2: commentary or education-focused,(11,23,25,26,29,43,55,58,61) oral presentation or poster presentation abstract,(28,30,32,36,37,49,51–53,56,57) and research study.(24,27,31,33–35,38–42,44–46,48,50,54,59,60,62) Commentary publications did not report on any particular study but, instead, discussed the importance of PBRN research in MT, implementation and development of PBRNs and PBRN research, and how the field can benefit from increased participation in PBRN research, including a critical review of CIM literature from PBRNs.(11) Research studies included surveys, RCTs, and observational studies. Three of the oral and poster presentation abstracts(30,37,49) were later published as papers(46,38,50) which were included in this review as separate entries. Several of the research studies produced multiple papers using data from the same source but for different purposes; specifically, three papers stemmed from PRACI’s practitioner survey.(37,38,45)
Table 3 delineates the applicable publications included in the scoping review into study design categorizations. The majority of PBRN-derived research publications including a MT component were survey studies. Of the 40 articles included in this review, only two involved randomized trials(31,60) and one was a repeated measures cohort study.(39) The remainder were reported as using survey format, with cross-sectional (n=14),(24,27,33–36,40,41,44,47,48,54,56,57) observational (n=6),(30,46,49,50,52,53) or descriptive (n=6)(32,37,38,42,45,51) study designs. Ten articles were written in narrative format (and thus not categorized as studies) discussed some aspect of a PBRN study with MT or the need for more MT research through PBRNs (n=10).(23,25,26,28,29,43,55,58,59,61) There was one critical review published that examined MT as a part of CIM research through PBRNs.(11)
Included publications aligned with seven general thematic categorizations established by investigators through an iterative process: treatment, practice characteristics, patient perspectives, patient utilization, state of the field, PBRN development and design, and other (Table 4). Most included publications of the studies that considered the use of massage as treatment investigated how practitioners apply massage for pain and its potential effectiveness. Practice characteristic surveys asked PBRN members about demographics, health promotion activities, referrals and professional relationships, and care approaches, among other items.(32,33,37,38,41,42,44,45,48,57) Patient perspectives surveys asked about reasons for seeking CIM interventions, perception of MT or CIM, and barriers to access to CIM.(30,36,46,56) Patient utilization studies examined patients’ reasons for seeking MT and CIM.(34,35,51,54) State-of-the-field category articles were commentaries about using PBRNs in CIM, along with a critical review of CIM literature from PBRNs.(11,23,25,29,43) The two PBRN development and design articles discussed the implementation of MNO-PBRN and PRACI.(28,55) Articles in the “Other” category covered topics that were not discussed in detail in more than two articles, and examined things like challenges in practice,(61) cost,(52) the application of the Pragmatic Explanatory Continuum Indicator Summary (PRECIS) model to PBRN research,(58) a call to action,(26) identifying intervention potential,(27) and massage therapists in research.(59)
Table 4 General Theme of Article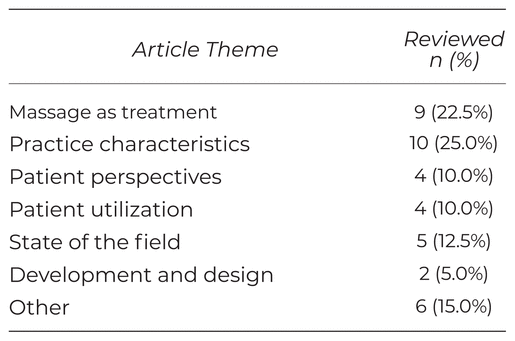
The majority of the articles discussed characteristics or perceptions regarding massage, but did not involve the actual application of massage (Table 5). Eight articles did not directly involve MT or massage therapists,(33,34,41,42,47,48,51,54) but rather discussed perceptions or practitioner relationships with massage therapists from the perspective of practitioners from other CIM fields, or patient perspectives, or use of CIM and MT. Eight articles discussed involving massage therapists to perform MT,(31,39,46,49,50,53,56,58) and three discussed the use of MT by non-massage therapist practitioners.(24,40,60) The remaining articles were commentaries and did not apply to this category.
Table 5 Active Application of MT and Involvement of Massage Therapists
This scoping review is the first formal synthesis of all PBRN-related literature focused on or involving MT specifically. The assessment indicates that there is an increasing amount of literature coming out of PBRNs that involve MT, although as with most areas of CIM research, PBRN-produced research in MT is still somewhat sparse. Few PBRNs involve CIM and/or are specifically working with or including MT, and those that are, tend to be investigating it as a part of CIM in general rather than as its own field. These broader-scope studies tend to be surveys of practice characteristics and general interventions. It is important to take into consideration that, because CIM-focused PBRNs are so new, they are still growing, developing, and assessing themselves. Practitioner surveys are an important first step to determine the needs and interests of network members, as well as clarify the potential research contributions of the PBRN as a whole. Data regarding patient conditions and perceptions can be used to guide future research projects within the PBRNs and in outside research institutions. Understanding what medical conditions have high prevalence and/or high relevance for practitioners and patients will allow researchers to develop projects that directly impact the lives of the people they aim to help. The body of PBRN research in CIM and MT is bound to grow as PBRNs like PRACI, MassageNet, and MNO-PBRN continue their work and, as more medical professionals from all fields begin to take notice, perhaps more collaborative networks will be implemented. The general trend of yearly publications is increasing, and judging from information found on PBRN websites (i.e., PRACI(15)), there will be more available in the coming years.
In 2015, the Academic Consortium for Complementary and Alternative Health Care (ACCAHC) gave its recommendations to the NCCIH for the advancement of research in CIM disciplines.(26) Among these recommendations was the proposal to encourage and expand the operations of PBRNs specific to CIM through increased funding and informational resources. Previous PBRN efforts had focused on encouraging more generalized PBRNs, such as those in primary care, to develop CIM-related research projects. This new recommendation of the PBRN model as a mechanism for specialized CIM research will hopefully impact the number of MT-related PBRNs and the amount of PBRN-produced literature involving MT in the near future.
PBRNs that focus specifically on MT research have the potential to make great contributions to the field of massage. The nature of PBRNs—that of connecting researchers and practitioners in the field—can allow practitioners to have a say in what kind of research projects are developed, leading to research that relates directly to what practitioners do every day. Relatable research is more likely to be used by practitioners to inform their practice,(63) leading to the advancement of real-life practice, as well as research literature. The involvement of professional organizations in encouraging the development of, and participation in, PBRNs may be a crucial push for the advancement of the field.
A major limitation of this review was its time frame. Only literature published before October 2019 was included, so the number of articles published in 2019 may not reflect the entirety of the literature published in that year. The requirements of a broad search and limited existing MT-related PBRNs made it impossible to remain solely within the field of MT research, and necessitated the inclusion of other CIM-related fields that incorporated MT in their research.
A clear gap in the current MT research coming out of PBRNs is that of clinical trials, or even simply hands-on research. Randomized controlled trials are possible to implement in MT,(64) and PBRNs are an excellent way to implement pragmatic approaches to clinical trials that reflect real-world practice.(65) Massage therapists tend to have limited research literacy skills(66) and may be hesitant to accept evidence with which they are unfamiliar;(67) so, offering information that is pertinent to their everyday practice may be more readily accepted than laboratory-based research. Involving more practitioners in the production and implementation of research may help spark interest from other practitioners, educators, and the public, and allow MT to become more accepted as an integral part of health care.
The future of CIM and MT does not rest solely in the hands of PBRNs. However, a more fully developed research system that includes PBRNs would likely improve the quality and quantity of practical research. Facilitating the connection of networks such as MassageNet and MNO-PBRN with larger primary care PBRNs in a variety of allied health fields including medicine, chiropractic, and physical therapy, may help increase visibility of these networks, add resources, and allow for more projects to be implemented. PBRNs in other fields should recognize the potential for massage therapist contributions to their projects. MT professional organizations should reach out to existing PBRNs in all areas of health care to bring the wide variety of fields together and create valuable research connections. The strong base already put in place by networks like PRACI and BraveNet can be used as a guide to build other PBRNs, and their databases will be useful in executing new projects and realizing the potential of PBRNs.
PBRNs can also be used as a tool to provide education for practitioners. Through the connections and resources of the network, there is the potential to develop programs that benefit massage schools to improve research literacy from the ground up, as well as for impacting the development of continuing education courses in research literacy and participation. Better understanding of the importance of research in practice may encourage more massage therapists to become involved, furthering the growth of the massage therapy field.(68)
This scoping review examined the quantity and characteristics of literature published through PBRNs that used massage therapy or massage therapists as a factor of consideration. Currently, MT research using PBRNs is dominated by studies that describe the characteristics of practitioners and patients, and there is limited published work in testing the effectiveness of MT through PBRNs. As existing CIM PBRNs grow and new ones are founded, the massage therapy literature base is bound to increase both in quantity and quality with regard to massage practitioner involvement and engagement in research.
The authors would like to extend a sincere thank you to University librarian Rachel Hinrichs, who played an important role in preparing the database search. No funding was obtained for the completion of this project.
The authors declare there are no conflicts of interest.
1 Green LA, Hickner J. A short history of primary care practice-based research networks: from concept to essential research laboratories. J Am Board Fam Med. 2006;19(1):1–10.
2 Lanier D. Primary care practice-based research comes of age in the United States. Ann Fam Med. 2005;3(Suppl 1):s2–s4.
3 Hickner J, Green LA. Practice-based research networks (PBRNs) in the United States: growing and still going after all these years. J Am Board Fam Med. 2015;28(5):541–545.
4 Rhyne RL, Fagnan LJ. Practice-based research network (PBRN) engagement: 20+ years and counting. J Am Board Fam Med. 2018;31(6):833–839.
5 US Department of Health and Human Services. Agency for Healthcare Research and Quality. Practice-based research networks. Bethesda, MD: the Agency; 2019. Available from: https://pbrn.ahrq.gov/ Accessed 13 November, 2019.
6 US Department of Health and Human Services. Agency for Healthcare Research and Quality. AHRQ research funding priorities & special emphasis notices. Bethesda, MD: the Agency; 2019. Available from: https://www.ahrq.gov/funding/priorities-contacts/special-emphasis-notices/index.html Accessed 26 November, 2019.
7 Kania-Richmond A, Menard MB, Barberree B, Mohring M. “Dancing on the edge of research” — What is needed to build and sustain research capacity within the massage therapy profession? A formative evaluation. J Bodywk Move Ther. 2017;21(2):274–283.
8 Schneider MJ, Evans R, Haas M, Leach M, Hawk C, Long C, et al. US chiropractors’ attitudes, skills and use of evidence-based practice: a cross-sectional national survey. Chirop Man Ther. 2015;23(1):16.
9 Moonaz S, Jeter P, Schmalzl L. The importance of research literacy for yoga therapists. Int J Yoga Ther. 2017;27(1):131–133.
10 Floden L, Howerter A, Matthews E, Nichter M, Cunningham JK, Ritenbaugh C, et al. Considerations for practice-based research: a cross-sectional survey of chiropractic, acupuncture and massage practices. BMC Complem Altern Med. 2015;15:140.
11 Lee H, Peng W, Steel A, Reid R, Sibbritt D, Adams J. Complementary and alternative medicine research in practice-based research networks: a critical review. Complem Ther Med. 2019;43:7–19.
12 Bravewell Collaboratives. BraveNet, the practice-based research network. 2010. Available from: http://www.bravewell.org/transforming_health-care/models_for_change/bravenet_research/
13 Dusek JA, Abrams DI, Roberts R, Griffin KH, Trebesch D, Dolor RJ, et al. Patients Receiving Integrative Medicine Effectiveness Registry (PRIMIER) of the BraveNet practice-based research network: study protocol. BMC Complem Altern Med. 2016;16(1):1–9.
14 “The Bravewell Story: How a small community of philanthropists made a big difference in healthcare”. Minneapolis, MN: George Family Foundation; 2016. Available from: http://www.georgefamilyfoundation.org/news/the-bravewell-story-how-a-small-community-of-philanthropists-made-a-big-difference-in-healthcare Accessed 26 November, 2019.
15 Australian College of Natural Medicine. Practitioner research and collaboration initiative. Fortitude Valley, Australia: the College; 2018. Available from: https://praci.com.au/
16 Massage Northern Ohio Practice-Based Research Network [website]. Cleveland, OH: MNOPBRN; n.d. Available from: http://mnopbrn.weebly.com/
17 MassageNet [website]. Lombard, IL: MassageNet; n.d. Available from: https://www.massagenet.org
18 Green LA, Dovey SM. Practice based primary care research networks. They work and are ready for full development and support. BMJ. 2001;322(7286):567–568.

19 Gilbert GH, Williams OD, Korelitz JJ, Fellows JL, Gordan VV, Makhija SK, et al. Purpose, structure, and function of the United States National Dental Practice-Based Research Network. J Dent. 2013;41(11):1051–1059.

20 Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32.
21 Pham MT, Rajić A, Greig JD, Sargeant JM, Papadopoulos A, McEwen SA. A scoping review of scoping reviews: advancing the approach and enhancing the consistency. Res Synthesis Meth. 2014;5(4):371–385.
22 Peters M, Godfrey C, Khalil H, McInerney P, Parker D, Soares C. Guidance for conducting systematic scoping reviews. Int J Evid-Based Healthcare. 2015;13(3):141–146.
23 Kutner JS, Main DS, Westfall JM, Pace W. The practice-based research network as a model for end-of-life care research: challenges and opportunities. Cancer Control. 2005;12(3):186–195.
24 Woggon AJ, Woggon DA. Patient-reported side effects immediately after chiropractic scoliosis treatment: a cross-sectional survey utilizing a practicebased research network. Scoliosis. 2015;10(1):1–6.
25 Reid R, Steel A. The importance of the PRACI project for grass roots complementary medicine practice: a call for practitioner involvement. Aust J Herbal Med. 2015;27(3):101–104.
26 Menard MB, Weeks J, Anderson B, Meeker W, Calabrese C, O’Bryon D, et al. Consensus recommendations to NCCIH from research faculty in a transdisciplinary academic consortium for complementary and integrative health and medicine. J Altern Complem Med. 2015;21(7):368–394.
27 Wolever RQ, Goel NS, Roberts RS, Caldwell K, Kligler B, Dusek JA, et al. Integrative medicine patients have high stress, pain, and psychological symptoms. Explore. 2015;11(4):296–303.
28 Muellner J, Mastnardo D, Ross A. P42 Establishing a non-traditional PBRN: a massage therapy practice-based research network. Paper presented at: NAPGRG Annual Meeting 2015; Bethesda, MD.
29 Hunter J, Wardle J, Kotsirilos V, Molodysky E, Ewer T. The case for establishing an Australasian integrative medicine practice-based research network. Aust Fam Physician. 2016;45(12):925–927.
30 Mastnardo D, Rose J. P42 Provider recommendation for massage card study. Paper presented at: NAPCRG Annual Meeting 2016; Colorado Springs, CO.
31 Mastnardo D, Lewis JM, Hall K, Sullivan CM, Cain K, Theurer J, et al. Intradialytic massage for leg cramps among hemodialysis patients: a pilot randomized controlled trial. Int J Therapeut Massage Bodywk. 2016;9(2):3–8.
32 Madigan D, Cambron J, Kennedy AB, Burns K, Dexheimer J. Volunteerism of Massage Therapists: a MassageNet study. Int J Therap Massage Bodywk. 2016;9(4):14–21.
33 Adams J, Lauche R, Peng W, Steel A, Moore C, Amorin-Woods LG, et al. A workforce survey of Australian chiropractic: the profile and practice features of a nationally representative sample of 2,005 chiropractors. BMC Complem Altern Med. 2017;17(1):14.
34 Adams J, Peng W, Steel A, Lauche R, Moore C, Amorin-Woods L, et al. A cross-sectional examination of the profile of chiropractors recruited to the Australian Chiropractic Research Network (ACORN): a sustainable resource for future chiropractic research. BMJ open. 2017;7(9):e015830–e015830.

35 Yang N, Wolever RQ, Roberts R, Perlman A, Dolor RJ, Abrams DI, et al. Integrative health care services utilization as a function of body mass index: a BraveNet practice-based research network study. Adv Integrat Med. 2017;4(1):14–21.
36 Mastnardo D, Dolata J, Pike E, Thornton J. P483 Barriers to access and perceptions of massage therapy among patients receiving services at a public hospital system in Northeast Ohio. Abstracts from the 2019 Research Poster Session of the American Massage Therapy Association Annual Convention, Indianapolis, IN. http://www.napcrg.org/Conferences/AnnualMeeting/EducationEvents/SearchEducationalSessions?language=en-US&m=1&s=Mastnardo&p=0
37 Steel A, Adams J, Sibbritt D, et al. The Practitioner Research and Collaboration Initiative: establishment and baseline data for the world’s largest practice-based research network in complementary healthcare. BMC Complem Altern Med. 2017;17(Suppl 1):D4. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5498855/ (p.24).
38 Steel A, Sibbritt D, Schloss J, Wardle J, Leach M, Diezel H, et al. An overview of the Practitioner Research and Collaboration Initiative (PRACI): a practice- based research network for complementary medicine. BMC Complem Altern Med. 2017;17:87.
39 Elder WG, Munk N, Love MM, Bruckner GG, Stewart KE, Pearce K. Real-world massage therapy produces meaningful effectiveness signal for primary care patients with chronic low back pain: results of a repeated measures cohort study. Pain Med. 2017;18(7):1394–1405.

40 Moore C, Leaver A, Sibbritt D, Adams J. The management of common recurrent headaches by chiropractors: a descriptive analysis of a nationally representative survey. BMC Neurol. 2018;18(1):171.

41 Yang L, Peng W, Adams J, Sibbritt D. Treating people with arthritis with traditional Chinese medicine (TCM): an examination of the perception of TCM practitioners. Acupuncture Med. 2018;36(4):228–239.
42 Adams J, Sibbritt D, Steel A, Peng W. A workforce survey of Australian osteopathy: analysis of a nationally-representative sample of osteopaths from the Osteopathy Research and Innovation Network (ORION) project. BMC Health Serv Res. 2018;18(1):352.

43 Ooi SL, McLean L, Pak SC. Naturopathy in Australia: Where are we now? Where are we heading? Complem Therap Clin Pract. 2018;33:27–35.
44 Kennedy AB, Cambron JA, Dexheimer JM, Trilk JL, Saunders RP. Advancing health promotion through massage therapy practice: a cross-sectional survey study. Prevent Med Rep. 2018;11:49–55.
45 Steel A, Leach M, Wardle J, Sibbritt D, Schloss J, Diezel H, et al. The Australian complementary medicine workforce: a profile of 1,306 practitioners from the PRACI study. J Altern Complem Med. 2018;24(4):385–394.
46 Mastnardo D, Rose JC, Dolata J, Werner JJ. Medical provider recommendations to massage therapy: a card study. Int J Therapeut Massage Bodywk. 2019;12(3):9–15.
47 Moore C, de Luca K, Wong AYL, Fernandez M, Swain M, Hartvigsen J, et al. Characteristics of chiropractors who manage people aged 65 and older: a nationally representative sample of 1903 chiropractors. Australas J Ageing. 2019;18(4):249–257.
48 Steel A, Vaughan B, Orrock P, Peng W, Fleischmann M, Grace S, et al. Prevalence and profile of Australian osteopaths treating older people. Complem Ther Med. 2019;43:125–130.
49 Abrams D. P02.05. Clinical practice outcomes of an individualized integrative intervention for chronic pain: results from the BraveNet PBRN [poster presentation]. BMC Complem Altern Med. 2012;12(Suppl 1):P61.
50 Abrams DI, Dolor R, Roberts R, Pechura C, Dusek J, Amoils S, et al. The BraveNet prospective observational study on integrative medicine treatment approaches for pain. BMC Complem Altern Med. 2013;13(1):146.
51 Abrams D, Horrigan B, Lewis S, Acree M, Pechura C, P04.16. Integrative medicine practice patterns across the US: results from a survey of 29 centers [poster presentation]. BMC Complem Altern Med. 2012;12(Suppl1):P286.
52 Dinan M, Roberts R, Reed S, Wolever R, Abrams D, Dolor R. P04.68. Costs associated with integrative medicine interventions on chronic pain [poster presentation]. BMC Complem Altern Med. 2012;12(Suppl 1):P338.
53 Dusek J, Abrams D. OA16.02. Longitudinal collection of patient-related outcomes in integrative medicine clinics: a pilot study from the BraveNet Practice Based Research Network [oral presentation]. BMC Complem Altern Med. 2012;12(Suppl 1):O63.
54 Wolever RQ, Abrams DI, Kligler B, Dusek JA, Roberts R, Frye J, et al. Patients seek integrative medicine for preventive approach to optimize health. Explore. 2012;8(6):348–352.
55 Steel A, Adams J, Sibbritt D. Developing a multi-modality complementary medicine practice-based research network: the PRACI project. Adv Integrat Med. 2014;1(3):113–118.
56 Cambron J, Dexheimer J, Madigan D, Brod N. Client perceptions of massage effects: a MassageNet study. Evanston, IL: Massage Therapy Federation; 2011. Available from: http://massagetherapyfoundation.org/recipient/client-perceptions-massage-effects-massagenet-study/
57 Cambron J, Dexheimer J, Madigan D, Brod N, Walton T. Massage therapists’ collection of health history and client conditions encountered: a MassageNet survey. Evanston, IL: Massage Therapy Federation; 2011. Available from: http://massagetherapyfoundation.org/recipient/massage-therapists-collection-health-history-client-conditionsencountered-massagenet-survey/
58 Elder WG, Munk N. Using the Pragmatic-Explanatory Continuum Indicator Summary (PRECIS) model in clinical research: application to refine a practice-based research network (PBRN) study. J Am Board Fam Med. 2014;27(6):846–854.
59 Munk N, Stewart K, Love MM, Carter E, Elder WG. The intersection of massage practice and research: community massage therapists as research personnel on an NIH-funded effectiveness study. Int J Therapeut Massage Bodywk. 2014;7(2):10–19.
60 Kutner JS, Smith MC, Corbin L, Hemphill L, Benton K, Mellis BK, et al. Massage therapy versus simple touch to improve pain and mood in patients with advanced cancer: a randomized trial. Ann Intern Med. 2008;149(6):369–379.

61 Kutner J, Smith M, Mellis K, Felton S, Yamashita T, Corbin L. Methodological challenges in conducting a multi-site randomized clinical trial of massage therapy in hospice. J Palliat Med. 2010;13(6): 739–744.

62 Moore C, Leaver A, Sibbritt D, Adams J. Prevalence and factors associated with the use of primary headache diagnostic criteria by chiropractors. Chiropr Man Ther. 2019;27(1):33.
63 Cordingley P. Research and evidence-informed practice: focusing on practice and practitioners. Cambridge J Edu. 2008;38(1):37–52.
64 Baskwill A. A commentary on the role of randomized controlled trials in massage therapy. Int J Therapeut Massage Bodywk. 2017;10(4):13–16.
65 Dolor RJ, Schmit KM, Graham DG, Fox CH, Baldwin LM. Guidance for researchers developing and conducting clinical trials in practice-based research networks (PBRNs). J Am Board Fam Med. 2014;27(6):750–758.

66 Gowan-Moody D. Research perceptions and utilization among massage therapists in Saskatchewan, Canada (Master’s thesis). Saskatoon, SK: Department of Community Health & Epidemiology, University of Saskatchewan; 2010.
67 Baskwill A. Changing the culture of clinical education in massage therapy. Int J Therapeut Massage Bodywk. 2011;4(4):33–36.
68 Baskwill A, Dore K. Exploring the awareness of research among registered massage therapists in Ontario. J Complem Integrat Med. 2016;13(1):41–49.
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
INTERNATIONAL JOURNAL OF OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 13, NUMBER 4, December 2020