 Survey of the Use of Massage for Children with Cerebral Palsy
Survey of the Use of Massage for Children with Cerebral Palsy
 Survey of the Use of Massage for Children with Cerebral Palsy
Survey of the Use of Massage for Children with Cerebral Palsy
Gwen Maureen Glew , MD, MPH 1, Ming-Yu Fan , PhD 2, Shawn Hagland , BS 3, Kristie Bjornson , PhD, PT 1, Shay Beider , LMT, MPH 4, John F. McLaughlin , MD 1
1 Division of Developmental Medicine, Department of Pediatrics, University of Washington and Seattle Children’s Hospital, Seattle, WA;, 2 Department of Psychiatry and Behavioral Sciences, University of Washington, Seattle, WA;, 3 Seattle Children’s Hospital, Seattle, WA;, 4 Integrative Touch for Kids, Tucson, AZ, USA.Background
Conventional medicine and complementary and alternative medicine (CAM) are merging into the broader field of “integrative medicine.” Massage is no longer considered complementary or alternative in some conventional medical circles today.
Purpose
We aimed to determine the prevalence of massage use among children with cerebral palsy (CP) in the Pacific Northwest in the United States, the reasons that massage is being used, and the limits of recruitment for a future randomized controlled trial.
Methods
This study, the first step in a three-stage research plan, was conducted at the Neurodevelopmental and Neurology clinics at Seattle Children’s Hospital, a tertiary pediatric hospital that provides service to patients primarily from Washington, Alaska, Montana, and Idaho. As a feasibility study (stage one), it precedes a planned pilot study (stage two), and subsequently, a full-scale randomized controlled trial (stage three) of whether massage can improve the health of children with CP. The study subjects—104 families with a child with CP ranging in age from 17 months to 21 years—were surveyed by the principal investigator and a research assistant in exam rooms at the hospital.
Results
In the families surveyed, 80% of the children had received massage at some point. Massage was currently being used in 51%, and trained professionals were providing the massage in 23%. Most families use massage for musculoskeletal relaxation, to improve quality of life, and to help their children sleep. Lower maternal income was associated with relatives as compared with professional massage therapists providing the massage. Massage therapy use by the mother and more severe CP were significantly associated with current use of massage for the child.
Conclusions
Most children with CP in the Pacific Northwest have used massage. Most parents surveyed believe that massage is helpful to their child. Additional research is needed to determine whether massage should be routinely recommended for children with CP.
KEYWORDS: Massage , cerebral palsy , musculoskeletal pain , quality of life , complementary and alternative medicine , integrative medicine
Conventional medicine and complementary and alternative medicine (CAM) are merging into the broader field of “integrative medicine.” Integrative medicine has been defined as healing-oriented medicine that re-emphasizes the relationship between patient and physician and that integrates the best of CAM with the best of conventional medicine(1). Some therapies traditionally considered to be CAM have been validated and, having become evidence-based, are being embraced by traditional medicine; others are being ignored by conventional medicine because science does not yet support their use.
One intervention that is clearly gaining favor in the conventional medical arena is massage therapy. Today, massage is no longer considered CAM in some conventional medical circles. Numerous rigorous scientific studies of massage have been conducted since 2000, and many of them have shown benefit(2). For example, evidence in support of massage for musculoskeletal back pain in adults is so great that physicians really should at least consider it a potential therapeutic option(3).
Cerebral palsy (CP) describes a group of disorders of the development of movement and posture, which cause activity limitation because of non-progressive disturbances that occur in the developing fetal or infant brain. The motor disorders of CP are often accompanied by disturbances of sensation, cognition, communication, perception, and behavior(4). The condition is marked by musculoskeletal tone abnormality, often spasticity (velocity-dependent tone). Patients with CP have a wide range of symptoms, from severe motor problems with inability to stand or even sit, to a mild form of the disorder in which the motor function of just one of the patient’s limbs is affected.
In the general pediatric population, massage is used significantly more frequently in families in which the mother is well-educated, the father has greater disposable income, and the parents use CAM themselves(5). The literature on the use of massage specifically for children with CP is sparse. However, it does include one study of 213 children with special needs surveyed in a tertiary care center in Michigan. The authors reported that 25% of children with CP received massage on a regular basis(6).
The only randomized trial of massage for patients with CP involved 20 infants with CP. In the treatment group, 10 children reportedly benefited from massage(7). Specifically, the authors reported that massage was associated with decreased spasticity; improved muscle tone, range of motion, and cognition; improved fine and gross motor skills; and improved social functioning. However, a subsequent review of the pediatric massage literature found only modest support for improvement of muscle tone with massage, and no support for improvement of range of motion, function, or spasticity with massage(2).
One qualitative investigation of massage for a single youth with CP was also favorable. The author reported that the massaged child “smiled more and appeared more relaxed”(8). Another uncontrolled qualitative evaluation of massage by parents trained to massage their children with CP was reported by Powell and colleagues in England in 2006(9). Parents said that their children showed improved calmness, bowel habits, and verbal communication, and increased smiling, eye contact, alertness, and mobility. That study is challenged by its lack of a control group and the possible bias introduced by having parents both perform massage and report the resultant data, because the parents may be especially eager to find positive results. Still, having parents provide massage to their children with CP also has many advantages. This method makes transportation and cost barriers irrelevant. Another distinct advantage is that parents are usually best able to read the child’s cues. For example, a parent can distinguish between a moan of pain and a cry of happiness when the nonverbal child with CP vocalizes. Also, parents are usually adept at positioning the child safely.
Cognitive deficits are not considered part of the definition of CP, but approximately 60% of people with CP also have an intellectual disability. Even if cognition is not impaired, abnormal voice motor function can make speech and communication challenging or even impossible. Cognitively impaired and nonverbal patients with CP may not be able to indicate the severity or the source of their pain. Engel and colleagues at the University of Washington surveyed verbal adults with CP about what worked for their pain(10). Respondents reported that surgical correction of hip dislocation and massage were two of the most effective treatments for pain.
Although the few studies of massage in people with CP have been encouraging, more research in the form of careful randomized controlled trials (RCTs) is needed to determine whether massage is truly beneficial for people with this disorder. One compelling reason to study massage as a treatment modality is that it has biological plausibility. It is well established that massage increases blood flow to the tissues and that enhanced blood flow encourages growth of new tissue and healing of wounds(11,12). In addition, it is possible that massage facilitates removal of lactic acid (an anaerobic respiration byproduct that causes fatigue) from muscle, increases endorphins, and inhibits serotonin reuptake(11–14). Massage may lengthen muscle fibers and reduce the formation of fibrotic tissue, which could potentially inhibit contracture formation(11). Nevertheless, more evidence is needed to determine whether these mechanisms really exist.
The present study was designed as the first stage in a three-stage research plan. It is a feasibility study (stage one), which precedes a pilot study (stage two) and a subsequent full-scale RCT (stage three), with the aim of determining whether massage can improve the health of children with CP. Our feasibility study consisted of a survey with two major goals:
To determine the current prevalence of massage among children with CP
To determine the perceptions of families about the benefits of massage (so as to help chose the outcomes to consider in the planned RCT)
Most massage studies have not used this approach (feasibility–pilot–RCT), and documentation of its use will be a valuable contribution to the field.
The survey was designed in part to teach us more about the current use of massage for children with CP in the northwest United States and to help plan the next phases of the study. It was an opportunity to determine how many subjects our team can expect to recruit for subsequent phases of the project, and to determine potential recruitment barriers. To achieve those ends, we read a description of the planned RTC to patients and their families, soliciting feedback on specific aspects of the methodology and inquiring whether they would be willing to participate in future phases of the project.
The Institutional Review Board of Seattle Children’s Hospital approved the study. Written informed consent and approval to review medical records were obtained from subjects willing to participate in the survey. Informed assent was obtained from the child with CP whenever the child was 14 years of age or older and able to communicate understanding and an opinion.
To identify eligible subjects, we reviewed the list of patients scheduled for the Neurodevelopmental and Neurology clinics each week from January 2007 to August 2007. These inclusion criteria were used:
The patient’s medical record had to contain an entry from a developmental pediatrician or child neurologist specifying that the patient had a diagnosis of CP.
The family had to be fluent in English.
Children with CP who could not speak for themselves had to be accompanied by a parent or legal guardian knowledgeable enough about the child to complete the survey on the child’s behalf.
As the patient was being checked into an exam room, a medical assistant asked a parent or legal guardian if, while they waited to be seen by their provider, they would be interested in hearing about an opportunity to participate in a study. The medical assistant provided a written description of the study if the family desired, marked a form indicating whether the family wanted to participate, and placed that form on the chart outside the door. Families desiring to hear more about the study were approached by the study’s research assistant shortly thereafter to request consent and to administer the survey.
Surveying by the principal investigator or the research assistant took place in the exam rooms as each subject waited to be seen by the medical provider. The survey, which was written by the principal investigator, took approximately 15 minutes to complete. Table 1 outlines the primary questions on the survey. In some cases, the survey was completed after the patient had been seen by the provider. Those unable to stay in clinic because of time constraints made arrangements to complete the survey later.
Table 1
. Summary of Survey Questionsa
Most of the questions on the survey were read to the family by the research assistant, but the final page of demographic questions was completed by the families in private. This step was intentionally taken to reduce the time spent on the survey and to increase confidentiality for families, especially with regard to income.
Subjects were assigned to either a low-or high-income category based on combined parental income. Combined parental income, reported as “family income,” was calculated by adding the midpoints of the income ranges reported by parents. Any combined income below $40,000 per year was categorized as “low”; any income of $60,000 or more was categorized as “high.”
The data were transferred from an Access spreadsheet (Microsoft Corporation, Redmond, WA, USA) to an Excel database (Microsoft Corporation) and then transferred to the SAS software package (version 9.1: SAS Institute, Cary, NC, USA), which was used to calculate means, medians, standard deviations, and percentages. Simple cross-tabulations, chi-square tests, and analyses of variance were computed to make comparisons between groups. The customary alpha of less than 0.05 was used to determine the significance of the results.
The goal of completing the entire survey with at least 100 families was achieved. Of 106 families approached, 104 agreed to participate in the survey. Four families did not complete the demographic questions. Only 2 families approached about the study declined to participate, yielding a participation rate of 98%. Six families (6%) finished the survey at home and returned it later.
Among the 100 subjects eligible for analysis, ages ranged from 17 months to 21 years. Severity of CP was recorded using the Gross Motor Function Classification System (GMFCS)(15). Most of the children in the families approached and interviewed were at the severe end of the CP spectrum, which was in keeping with the clinic population. The more severe the child’s condition, the more likely the child was to have received massage. Of the analyzed subjects, 20% had never received massage, and 80% had received massage at least once.
The data were analyzed so as to determine the demographic factors associated with the use of massage (ever vs. never). We observed no significant differences between the two groups with regard to parental education, parental ethnicity, parental age, family income, or child’s age.
At the time the survey was conducted, 51% of the surveyed children were receiving massage. Additional questions were asked of those individuals. Massage was given by relatives in 68% of the families, by professional massage therapists in 23%, and by physical therapists in 49%. Children whose mothers had lower incomes were more likely than children whose mothers had higher incomes to receive massage from a relative as compared with a professional. The proportion of girls who received massage from relatives was higher than the proportion of boys who received massage from relatives. Parental age was not associated with whether the children received massage from a licensed massage therapist.
Of surveyed parents who were seeking and using massage for their children with CP, 86% believed that massage helps to relax muscles; 71%, that it improves quality of life; 23%, that it improves sleep; and 30%, that it decreases their child’s pain. In 29% of responding families, massage was used for constipation, and in 29%, for agitation. These are findings that have not, to our knowledge, been reported previously in the United States.
For subjects that had received massage, the children’s care providers were asked if massage had ever been discontinued, and if so, why. Massage had been discontinued at some point in 78% of families. The most common reason for cessation was the time-consuming nature of massage (46%). In 11% of families, massage was stopped for lack of perceived benefit. Cost of massage led to discontinuance in 8%. Massage was stopped for various other reasons in 61%. Among the “other” reasons, the two main ones were illness, surgery, or hospitalization ( n = 12) and a move by the family or the massage provider ( n = 8).
In addition to comparing children who had ever used massage with those who had never used massage, we compared current massage users with current nonusers. Table 2 presents significant findings from that analysis, which revealed that the use of massage by the mother herself was significantly associated with current use of massage by the child. Similarly, a more severe GMFCS level was significantly associated with current use of massage. Neither the age of the child nor the age of the parents was significantly associated with current use or nonuse of massage. Younger children were not significantly more likely to use massage.
Table 2
. Comparison of Children Who Currently Do and Do Not Receive Massagea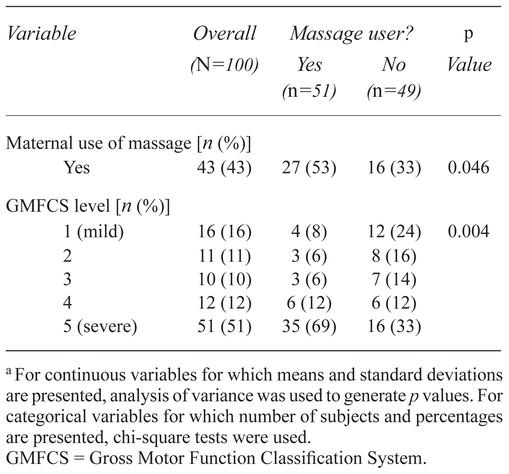
The type of person engaged to perform massage did appear to depend on maternal income. If maternal income was less than $20,000 annually, the child was significantly more likely to receive massage from a relative. The sex of the child mattered too: female children were more likely than male children to receive massage from a relative.
Of the subjects surveyed, 99% were willing to participate in the planned RCT. The only unwilling person cited lack of interest and inability to commit to the time required.
Subjects and their caregivers were asked if they would prefer a particular geographic location for receiving massage if they were to be assigned to the treatment arm in a future RCT. Response options included “at home,” “in a hospital room,” “at a spa,” “at a massage therapist’s office,” and “other.” Most respondents (87%) said that they preferred to receive massage therapy at home. They preferred a schedule of massages twice weekly for 5 weeks rather than once weekly for 10 weeks.
We collected comments from the subjects and their families to capture their ideas about a future RCT of massage for CP. There was enthusiasm from most parents for testing massage. Some of the parents saw a future study of massage as a potential opportunity for additional insurance coverage, for the child’s relief from discomfort and pain, and for their own education. Many of the parents already believe that massage is an effective modality. Almost all survey respondents expressed a clear desire to know the results of the planned trial so as to help their child.
Our study was designed as the beginning of a larger research plan to address the question “Is massage a useful modality for children with CP?” The fact that 80% of our surveyed CP patients in Seattle are already using massage suggests that the modality is at least perceived as useful, that it may in fact be underutilized, and that further research is needed.
Pain and sleep disturbances in children with CP are especially challenging and pressing problems. Of the surveyed parents who are seeking and using massage for their child with CP, 86% believed that massage helps to relax muscles, and 71% believed that it improves quality of life. This information will be valuable for the design of future studies of massage for children with CP.
Our results suggest that, compared with children having mild disease, those more severely affected are massaged more often. There are many possible reasons that use of massage might vary with symptom severity. Complications of CP are often a result of chronic overstimulation of muscle and lack of normal movement. Children with more severe CP are more likely to look and feel worse. More severely affected patients are more likely to suffer from constipation, sleep problems, agitation, and muscle spasms—all the reasons for which parents say massage is performed.
Based on training time, depth of concentration, practice, and focus, experienced licensed massage therapists and physical therapists may be superior to untrained professionals in providing massage to children with CP, but this supposition has not been proven. Parental massage (after training) may have other advantages. Many past pediatric massage studies have used volunteers, parents, or massage therapy students as the primary providers of treatment(2). More research is needed to determine whether the massage provider makes any difference with regard to specific health outcomes.
Insurance coverage for massage and other CAM therapies varies widely from state to state. The reimbursement policy in Washington State is that only evidence-supported modalities of massage are covered(16). Currently, massage is seldom covered by insurance for children with CP, and only a subset of therapists are able to perform massage when coverage is available. More research in this area is clearly needed so that, if massage is helpful, it will be accessible to children from all socioeconomic groups.
Our study has four main limitations. First, limited funding prevented us from surveying non-English speakers. More work is especially needed in ethnically diverse populations. Second, because this study used a convenience sample of patients presenting for specialty care in an outpatient setting and because the patients surveyed generally had more severe CP, the results may not be generalizable to the entire population of children with CP. Third, to keep the survey brief and to minimize the time burden on families, we obtained maternal and paternal income, but no information on insurance type (Medicaid, none, etc.) or family size. Finally, the type of massage therapy used by each family and the duration of a typical massage were not explored. An increasing number of massage modalities fall under the general heading of “massage therapy.” These therapies use varying pressure, pacing, and site restrictions. This variation may influence perceived benefit. Family members might massage for a shorter time than do professional massage therapists, possibly influencing actual and perceived benefit.
The results from this project suggest that use of massage in children with CP is prevalent among patients of the Seattle Children’s Hospital in the Pacific Northwest. Economics likely plays a role in the choice of massage provider. We do not yet know whether the type of provider (physical therapist vs. massage therapist vs. parent) affects the quality of massage given. Systematic examination of massage as a treatment modality for musculoskeletal relaxation, quality of life, pain, sleep, and other outcomes for people with CP is needed. Massage looks promising as a treatment modality for all people with CP, but for families and clinicians to make scientific decisions about its usefulness, more evidence, including our planned RCT, is necessary.
1
. Maizes V, Schneider C, Bell I, Weil A. Integrative medical education: development and implementation of a comprehensive curriculum at the University of Arizona. Acad Med. 2002;77(9):851–860.
2
. Beider S, Moyer CA. Randomized controlled trials of pediatric massage: a review. Evid Based Complement Alternat Med. 2007;4(1):23–34.

3
. Cherkin DC, Eisenberg D, Sherman KJ, Barlow W, Kaptchuk TJ, Street J, et al. Randomized trial comparing traditional Chinese medical acupuncture, therapeutic massage, and self-care education for chronic low back pain. Arch Intern Med. 2001;161(8):1081–1088.
4
. Bax M, Goldstein M, Rosenbaum P, Leviton A, Paneth N, Dan B, et al. for the Executive Committee for the Definition of Cerebral Palsy. Proposed definition and classification of cerebral palsy, April 2005. Dev Med Child Neurol. 2005;47(8):571–576.
5 . Spigelblatt L, Laîné-Ammara G, Pless IB, Guyver A. The use of alternative medicine by children. Pediatrics. 1994;94 (6 Pt 1):811–814.
6
. Hurvitz EA, Leonard C, Ayyangar R, Nelson VS. Complementary and alternative medicine use in families of children with cerebral palsy. Dev Med Child Neurol. 2003;45(6):364–370.
7
. Hernandez-Reif M, Field T, Largie S, Diego M, Manigat N, Seoanes M, et al. Cerebral palsy symptoms in children decreased following massage therapy. Early Child Dev Care. 2005;175:445–456.
8 . Stewart K. Massage for children with cerebral palsy. Nurs Times. 2000;96(1):50–51.
9
. Powell L, Barlow J, Cheshire A. The Training and Support Programme for parents of children with cerebral palsy: a process evaluation. Complement Ther Clin Pract. 2006;12(3):192–199.
10
. Engel JM, Kartin D, Jensen MP. Pain treatment in persons with cerebral palsy: frequency and helpfulness. Am J Phys Med Rehabil. 2002;81(4):291–296.
11 . Vickers, Andrew Van Toller S, Stevensen C. Massage and Aromatherapy: A Guide for Health Professionals. London, UK: Chapman and Hall; 1996: 311.
12 . Hovind H, Nielsen SL. Effect of massage on blood flow in skeletal muscle. Scand J Rehabil Med. 1974;6(2):74–77.
13
. Engel JM, Kartin D. Pain in youth: a primer for current practice. Crit Rev Phys Rehabil Med. 2004;16(1):53–76.
14
. Field T, Hernandez-Reif M, Diego M, Schanberg S, Kuhn C. Cortisol decreases and serotonin and dopamine increase following massage therapy. Int J Neurosci. 2005;115(10):1397–1413.
15
. Palisano R, Rosenbaum P, Walter S, Russell D, Wood E, Galuppi B. Development and reliability of a system to classify gross motor function in children with cerebral palsy. Dev Med Child Neurol. 1997;39(4):214–223.
16
. Watts CA, Lafferty WE, Baden AC. The effect of mandating complementary and alternative medicine services on insurance benefits in Washington State. J Altern Complement Med. 2004;10(6):1001–1008.
CONFLICT OF INTEREST NOTIFICATION
The authors declare that there are no conflicts of interest.
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK , VOLUME 3 , NUMBER 4 , 2010