
Robin B. Thomas, LMT, DrPH
Departments of Human Services and Health Promotion Sciences, University of Arizona, Tucson, AZ, USA.Background
Women worldwide experience perinatal mood, anxiety, and pain contributing to pregnancy and birth challenges, maternal and infant bonding, and childhood development. Perinatal women seek massage therapy for relaxation, pain management, and emotional support, but may encounter socioeconomic barriers. Prior studies demonstrated improved perinatal health by teaching partners of pregnant women a side-lying massage.
Purpose
This study examined health effects to perinatal mood, anxiety, and pain, by teaching partners of pregnant (PG) women a chair massage.
Setting
Participant’s homes in Tucson, Arizona, USA.
Participants
Twelve PG women with minor mood, anxiety, and pain: 67% white, 33% Hispanic, college educated, married, aged 32 years (± 3.86 SD), 67% expecting a first child, annual incomes ≤ $50,000 (33%), > $50,000 (67%).
Research Design
A pre/postintervention pilot study in a single group for eight weeks.
Intervention
Twice weekly partner-delivered chair massage and its relation to perinatal mood, anxiety, and pain.
Main Outcome Measures
Pre/poststudy perinatal massage effects were measured with the Edinburgh Depression Scale (mood), the STAI-AD (anxiety), and the VAS (pain). Weekly text messaging tracked dose and frequency, follow-up surveys measured sustainability, and birth outcomes were acquired by texting.
Results
Study retention was 86%, protocol compliance 94%, with couples averaging 10-minute, twice weekly chair massage over the eight-week study period. Paired-sample t tests indicated statistically significant improvements to perinatal mood and anxiety, Cohen’s d, a large strength of effect size (p = .012, d = 0.87; p = .004, d = 1.03). A trend was observed for reduced pain, with a medium strength of effect size (p = .071; d = 0.58). Follow-up surveys indicated most couples were sustaining at least weekly massage. Birth outcomes showed healthy infants with no complications, mean birth weight of 7.26 pounds, and mean gestation of 39 weeks.
Conclusion
This is the first evidence of partner chair massage as safe and effective complementary home management of perinatal mood, anxiety, and pain.
KEYWORDS: partner chair massage, perinatal mood, perinatal anxiety, perinatal pain
The self-reported prevalence rate of mood/depression or anxiety is approximately 20% during pregnancy.(1–5) Mood and anxiety contribute substantially to pregnancy complications and frequently continue and worsen into the postpartum period.(6–9) Pregnancy-related mood is associated with increased physician visits,(10) preeclampsia,(11) spontaneous abortion,(12) preterm labor and birth, and decreased birth weight.(2,13) Pregnancy-related anxiety has been associated with obstetric complications,(14) preeclampsia,(11) preterm labor and birth,(15) and decreased birth weight.(16) Preterm difficulties and infant death, increased by perinatal mood and anxiety, contributed to costing the United States (U.S.) more than US 26 billion dollars in 2005 for health insurance, education, and other social support systems.(17)
Perinatal mood and anxiety have potentially long lasting consequences to the mother and her family.(16–18) Mood and anxiety can affect maternal–infant bonding and contribute to childhood developmental and behavioral challenges (including health, cognitive, and motor) that can last throughout the life span.(17–19) Chronic disparities (i.e., obesity, metabolic disease, and diabetes) associated with mood and anxiety,(20) frequently begin during fetal development and continue into adulthood.(21) At the extreme, perinatal mood and anxiety can lead to maternal psychosis, resulting in maternal suicide or maternal infanticide.(22) Barriers to seeking health care options for perinatal mood and anxiety include perceived social judgment, time limitations, and economic constraints.(23–28)
Information on complementary treatment options for perinatal mood and anxiety is limited; however, the literature shows pregnant and postpartum women seek massage therapists for care, including relaxation, emotional support, and pain management.(19,26,28–30) A narrative review of several studies reported massage therapy as effective at decreasing anxiety, depressed mood, and pain in pregnant women; group interpersonal psychotherapy attendance was also improved, demonstrating the value of massage alongside more mainstream treatment options.(31) In addition, committed partners of pregnant women were trained to deliver a 20-minute massage, with women in a side-lying position.(13,32,33)
This pilot study addressed the effects of a chair massage on perinatal mood, anxiety, and pain, instead of the side-lying position used in previous studies.(13,32,33) Challenges to implementation of side-lying massage include time and child care concerns, transportation to training sites for instruction, and costs (e.g., massage table, lotions, and oils).(23–28) The current study addressed the barriers to health care seeking and gaps in understanding health outcomes by adapting the partner-delivered, side-lying massage to the use of standard household equipment (a chair), in-home training, and less delivery time.(13,32,33) It reduced the dose of the current partner protocol(32) from 20 minutes to 10, to address women’s concerns related to lack of time. It adapted the length of the study period, from 12–16 weeks to eight weeks, to address attrition that may occur for participants concerned with the length of the study commitment. This study had one hypothesis: a 10-minute chair massage, adapted for moms and delivered by their partners twice weekly, would be associated with a decrease in low mood, anxiety, and pain over an eight-week period. The significance of this study is in managing perinatal mood, anxiety, and pain at home, promoting the health of families, and providing an accessible complementary treatment. Partner-delivered chair massage is a nonpharmacological option that can be used alongside treatment as usual for perinatal care.(34)
This pilot study investigated pre- and postintervention outcomes of self-reported perinatal mood, anxiety, and pain in a single group of women. Blinding did not occur, as the women were aware massage was being applied by their partners, and the principal investigator (PI) handled all study procedures. Sample size was not calculated, as the purpose of the study was to test participant health outcomes prior to planning a larger randomized control trial. The study was approved by The University of Arizona’s Office of Human Subject Protection’s Institutional Review Board before participant contact. Written consent was obtained from all study participants (pregnant women and their partners).
The study took place in Tucson, Arizona. Partner massage training was conducted by the PI, a state-licensed massage therapist with over 20 years’ experience, certified in teaching by the University of Arizona. The massage training was conducted on campus, at the College of Public Health, for the first five couples and in the couple’s homes for the remaining seven. After the one-time training, the pregnant women and their partners conducted the chair massage protocol for the next eight weeks in their homes.
Participants were recruited with support from the local postpartum depression coalition. The coalition offered the PI presentation opportunities at quarterly meetings, as well as its provider directory. Among the providers in the directory were obstetric personal and mental health professionals trained in perinatal mental health. All directory providers were contacted, and those interested in the study posted a recruitment flyer in their offices and on FacebookTM. Participants who self-reported with minor mood, anxiety, and pain symptoms contacted the PI for eligibility screening. Eligibility for study inclusion identified local women, 25–40 years of age, with low-risk pregnancies, who were no later than eight weeks from their due date by training time, and had partners living in the household willing to learn chair massage. Exclusion criteria were women self-reporting with a major mental health concern beyond low-levels of mood, anxiety, and pain, or who were pregnant with more than one fetus. Female participants agreed not to receive massage therapy or other hands-on complementary health care (i.e., acupuncture or chiropractic) during the eight-week period of study. Exclusion criteria for partners included any physical limitations preventing them from standing for 10 minutes to deliver the massage, or conditions that restricted use of their hands (i.e., injuries, arthritis, or infections). Study eligibility also required participants have mobile phones with text messaging and an email account available during the study. Participants and their partners were compensated $25 each for full study participation.
Couple’s massage training consisted of less than 60 minutes of basic massage instruction by the PI. The instruction provided simple and safe massage techniques to the pregnant woman’s head, neck, shoulders, and back for a 10-minute session. The techniques included effleurage and petrissage,(35–37) with the importance of couple’s communication emphasized throughout the massage training.(38) Before applying techniques, the partners were advised to always ask the pregnant woman if she felt ready to be massaged and was not feeling ill or feverish. If she was receptive, the partner gently placed his hands on the woman’s shoulders, took two calming breaths with her, and applied slow and gradual application of massage to the woman’s comfort level.(36) Partners were encouraged to listen and respond appropriately to both verbal and nonverbal feedback the pregnant women gave throughout the massage.(35,38) Women were encouraged to communicate their preference for pressure and depth.
The massage techniques taught were intended for relaxation, support, and pain management. The techniques used moderate pressure,(39) firm but never painful, with a tailored approach specific to the woman receiving the massage. The partner was taught to observe nonverbal cues, such as the woman pulling away, moving about in her chair, or tensing up, and to adjust accordingly.(35) Partners were also encouraged to vary their techniques and body mechanics in delivering the massage to avoid fatigue, muscle strain, and injury to themselves, and to prevent too forceful of an application to the woman.(37) A protocol checklist was left with the participants with memorable terms and brief descriptors on one side (Table 1) and a diary with a table on the other to record the dose (minutes) and frequency (dates) of each session (Table 2). Participants were encouraged to place the checklist and diary on their refrigerator doors as a convenient reminder. The couples were asked to continue the 10-minute protocol at home, twice weekly for the next eight weeks, for a total of 16 study sessions.
Table 1 Chair Massage Protocol Checklist
Table 2 Chair Massage Participant Diary
Please record the date and number of minutes each time you conduct a chair massage with your partner. Remember to save your input. Thank you!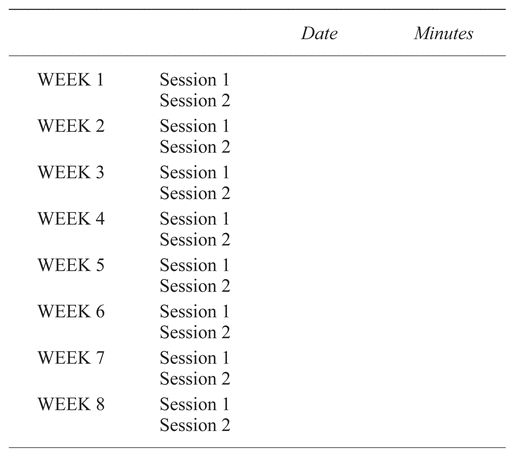
Within 24 hours of the massage training, three validated questionnaires were emailed to the pregnant participants as attachments. The questionnaires were selected based on their brevity, simplicity, and ease of use.
The Edinburgh Postnatal Depression Scale is an easy-to-administer and effective one-page questionnaire with 10 questions.(40) The questionnaire asks respondents to answer the questions most closely associated to how they have felt over the past seven days and has a recommended cutoff score of nine or 10, suggesting higher levels of depression.(40) The Edinburgh Scale has been tested as a reliable indicator of the presence of depression during pregnancy and is used by obstetric personal, pediatricians, and midwives.(41,42)
The STAI portion of the State-Trait Anxiety Inventory is a one-page questionnaire with 10 questions used to measure state anxiety.(43) It has a Likert scale from 1–4, ranging in answers that include “Not at all” to “Very much” to indicate how the respondent feels in the moment based on current life events.(43) The STAI is a reliable indicator of the presence of state anxiety in an individual, and has been validated in pregnancy studies and used by perinatal mental health professionals.(19,44)
The VAS is a 10-centimeter straight line indicating pain ranging from “No Pain” to “Worst Pain”, and is a reliable indicator of subjective pain levels.(45) The respondent is asked to indicate on the line where their pain is relative to the two extremes. The VAS is used universally by pain clinicians and has been validated in pregnancy studies.(46,47)
Within one week of the massage training, the PI text messaged the pregnant participants to address any questions or concerns, and collect the dose and frequency of their sessions over the past week.(48) After eight weeks of text data collection, the mood, anxiety, and pain questionnaires were again emailed to the participants, for postintervention data collection. One-month and three-month follow-up surveys were emailed to the participants to measure sustainability of the chair massage protocol. The surveys were brief, with three statements inquiring about current use of chair massage and respondents could agree or disagree with each. Birth outcomes were collected by text messaging each of the women post-survey follow-up. Data collected were of infant birth weights, birth complications, and gestation week at birth. The questionnaires, diaries, and surveys were completed electronically by the female participants, saved, and returned as email attachments to the PI. The returned forms were electronically saved by the PI in a password-protected file after reviewing the data for quality and completeness and recorded on an Excel™ spreadsheet.
The statistical analyses for study data were generated using IBM SPSS, Version 25TM software. Descriptive statistics were used to analyze the results of the baseline participant data collected, follow-up surveys, and birth outcomes. Paired-sample t tests were applied to analyze the pre- and poststudy effects of partner-delivered chair massage to perinatal mood, anxiety, and pain. T tests were two-tailed, with confidence intervals (CI) of 95% and statistical significance determined with a value equal to or less than an alpha level of 0.05. Cohen’s d was applied to determine the strength of effect size. An independent samples t test was conducted to examine differences in perinatal health outcomes based on training location.
Of 23 women initially screened (January, 2017–January, 2018), three were eligible but did not progress to the consent stage. Six women were ineligible: three were too close to their due dates, one was too young, one was pregnant with twins, and one woman’s partner changed his mind. Of the 14 remaining consenting women: one withdrew before partner training as too busy, and the other had a miscarriage before the first week of in-home study. All participants were receiving perinatal care as usual for their pregnancies. None of the women were seeing mental health professionals. The characteristics of the 12 remaining women are provided in Table 3: 67% white, 33% Hispanic, college educated, married, age averaged 32 years (± 3.86 SD), 67% were expecting a first child, annual incomes ≤ $50,000 (33%), and > $50,000 (67%).
Table 3 Demographic Characteristics of Pregnant Participants at Baseline
Partner-delivered chair massage ranged from 5.81–20.75 minutes averaged per couple, with a mean of 10.26 minutes (± 3.74 SD) over the eight-week period of study. Sessions completed, ranged from 12–16, with a mean of 14.92 per couple (± 1.38 SD). Sessions missed were due to religious holidays and the flu in winter months, and summer vacations, work travel, and moving in the rest of the year.
The massage elicited a reduction in perinatal mood mean scores of 3.33±1.11 [mean ± standard error] which was statistically significant (p = .012, CI: 0.89–5.78). Cohen’s d of 0.87 indicated a large strength of effect size.
The massage elicited a reduction of 7±1.96 [mean ± standard error] in perinatal anxiety mean scores, which was statistically significant (p = .004, CI: 2.68–11.32) with a large strength of effect size (d = 1.03). The massage elicited a mean reduction of 1.14±0.57 [mean ± standard error] in perinatal pain mean scores pre- to poststudy, indicating a trend that was not statistically significant (p = .71, CI: −0.11–2.39), with a medium strength of effect size (d = 0.58). Differences in effects based on training location indicated no statistical significance: mood (p = .960), anxiety (p = .552), pain (p = .227). Table 4 provides participant’s change scores; Tables 5 and 6, statistical effect summaries.
Table 4 Mood, Anxiety, and Pain Score Changes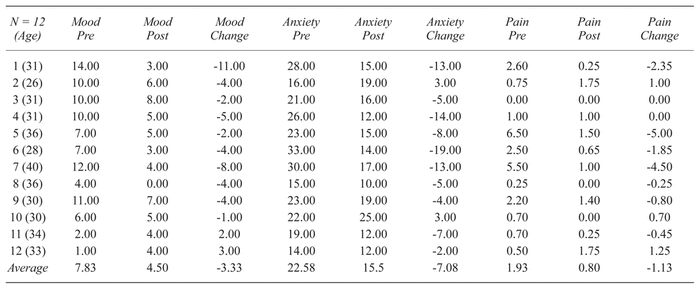
Table 5 Summary of Chair Massage Effects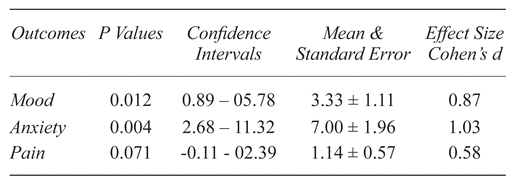
Table 6 Summary of Chair Massage Effects Based on Training Location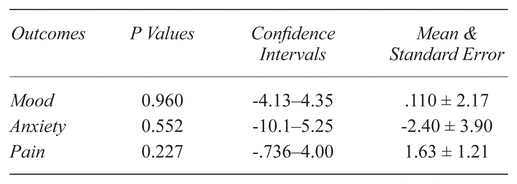
The results of the one-month follow-up surveys showed 25% of the couples were practicing chair massage twice a week, 75% weekly. The results of the three-month follow-up showed that 25% of the couples were practicing chair massage twice a week, 67% weekly, and one couple (8%) was not currently practicing.
The infants born to study participants ranged in weight from 6.02–10.01 pounds, with a mean of 7.26 pounds (±1.41 SD). Gestation ranged from 36–42 weeks, with a mean of 39 weeks (±1.77 SD). All were vaginal deliveries with no birth complications.
The female participants in this study had college educations, and 67% lived in households with annual incomes above $50,000. According to the 2007 Health Information National Trends Survey, US college grads were more likely to use complementary medicine, such as massage, than those with less education.(49) The likelihood of using complementary medicine, however, is associated with all income levels, and as income increases, so does frequency of use.(50)
The rates of study retention (86%) and protocol compliance (94%) were high, with couples averaging 10-minute, twice weekly sessions throughout the eight-week period. Study results demonstrated improvements to perinatal mood, anxiety, and pain, similar to findings in the literature for longer sessions (20 minutes) delivered in a side-lying position, after 12–16 weeks of study.(13,32,33)
The infants born to participants completing this study averaged full gestation at 39 weeks with no birth complications, and were within the normal weight range at 7.26 lbs. The March of Dimes currently defines a full term pregnancy as 39–40 weeks and a low-weight infant as less than five pounds eight ounces. The participant data reporting a miscarriage at 20 weeks have not been included in this analysis. The American College of Obstetrics and Gynecologists reported national miscarriage rates as 10%–25% in 2015;(51) the rate of miscarriage in this study was 8%.
At baseline, the pregnant women in this study showed an average mood score of approximately 8 points—a score considered to be near, but below, the threshold of nine or 10, consistent with clinical concern.(40) After eight weeks of partner-delivered chair massage, perinatal mood scores had decreased to an average of 4.5 points, no longer of clinical concern. Eighty-three percent of the women’s perinatal mood scores showed improvement; only two with the lowest scores did not. Women who self-reported higher mood scores at baseline had the greatest differences in improved outcomes. These results are consistent with findings in the literature demonstrating improvement of perinatal mood after partner-delivered massage.(13,32,33)
At baseline, pregnant participants self-reported average anxiety score of 22.5 points, indicating a sample with more symptomology than the general population (19 points) of females at 32 years of age(43) and common to baseline symptomology found in studies of perinatal anxiety.(44) After the chair massage intervention, average anxiety scores decreased, demonstrating scores (15.5 points) lower than symptomology reported in the general population of women the same age. Eighty-three percent of the women in the current study showed perinatal anxiety improvement; one woman with a score among the lowest did not. The women in this study who presented with the highest anxiety scores at baseline had the greatest differences in improved outcomes postintervention. These results are consistent with findings in the literature, demonstrating improvement of perinatal anxiety after partner-delivered massage.(13,32,33)
Although the current study was likely underpowered to detect greater differences in pain measures, the results are encouraging for future study, and provide insight into how partner-delivered chair massage may affect perinatal pain. At baseline, participants self-reported an average pain score of 1.93 cm, below the average of 5 cm.(47) Perinatal pain decreased to 0.79 cm by the end of this study. Sixty-seven percent of the women showed perinatal pain improvement pre- to poststudy. Two women’s pain scores were unchanged pre- to postintervention, one at the low end of the VAS pain scale and one reporting no pain throughout. Pain increased for two other participants’ pre- to poststudy; these scores were among the lowest at baseline. Alternately, the two highest pain scores at baseline decreased 82% and 77%, respectively, by the end of the study. These results are consistent with findings in the literature, demonstrating improvement of perinatal pain after partner-delivered massage.(13,32,33)
As women progress through their pregnancy, rates of anxiety frequently increase and mood fluctuates.(1,52) Rates of anxiety have been reported as 18.2% in the first trimester, 19.1% in the second, and 24.6% in the third.(1) In the current study, the majority of women enrolled in their second trimester, with anxiety decreasing 31% from second to third trimesters after the massage intervention and before the birth. Rates of low mood have been reported as high in the first and third trimesters compared to the second.(52) Mood scores decreased 58% from the second to third trimesters in the current study, postintervention and before infant birth. Improvement to mood and anxiety before the birth is important because of the known risk for pregnancy complications, low infant birth weight, and postpartum mental health effects.(2,8,15,31)
Pregnancy frequently involves low-back and pelvic pain.(47,53,54) The onset of pregnancy-related low-back and pelvic pain occurs near the 18th week and reaches peak intensity 24–36 weeks.(46) In the current study, although pain reduction was not statistically significant with mean scores below the norm at baseline, pain decreased for the majority of women from second to third trimesters. These results are important because onset of pain during pregnancy is a risk factor for persistent postpartum low-back and pelvic pain, and pain in subsequent pregnancies.(54)
The results of the follow-up surveys indicated that the majority of the couples were practicing chair massage at least weekly. The one-month surveys were completed at a point when most couples were nearing their due dates.
An unsurprising benefit of participation was that partner massage skills may have helped women manage the birth process. A review of pain during labor found massage helped women cope with pain intensity when the cervix was dilated during the first stage, increased satisfaction with childbirth overall, and provided women with a greater sense of control.(55) The three-month follow-up was conducted at a time when most couples had brought their infants home and family responsibilities had increased. The important point may be that couples can use their skills as needed for postpartum health and in subsequent pregnancies.
A strength of this study was in successfully piloting a partner-delivered chair massage to promote perinatal health, addressing perceived barriers to mental health care seeking expressed by pregnant women with low mood and anxiety.(23,24,27) Barriers to perinatal mental health care seeking include time constraints, costs, child care, and perceived social judgment.(23,24,27) A 10-minute chair massage allowed for a safe and no-cost approach (using equipment couples already had), was practiced at home (addressing child care concerns), and delivered by trusted partners in established relationships (avoiding perceived social judgment). Chair massage is efficient, as it does not require the receiver to take time to disrobe and can be applied without need for lotions or oils. Chair massage allows for brief self-care sessions which are practical, sustainable, and may fit into daily routines with the least amount of disruption.
Another strength of this study is that partner-delivered chair massage allowed husbands to be more actively involved in the process of pregnancy by providing support and nurturance at a time of change, physically, mentally, and socially for their wives.(19) Having the skills to manage perinatal mood, anxiety, and pain may provide the partner with a sense of valued contribution to an important life-changing family event.(19) These results may be important to Massage Therapists (MTs) who serve disadvantaged populations who otherwise might not receive massage therapy.(56) MTs could also promote their work and extend beneficial client outcomes between visits by teaching partners simple skills; however, regulations should be checked, as they may vary state to state.
Among notable limitations to this study include the small sample size, lack of control group, self-reports, and short follow-up periods. Justification for a sample size of 12 was based on feasibility, precision of the mean and variance, and regulatory considerations.(57) Future study should consider a larger design with more participants, targeting disadvantaged groups from different areas. Participants relaxing in a quiet room might work as a study control. Additionally, a heavy reliance on self-report methodology is subjective and could be affected by memory or recall concerns. Physiological measures related to primary outcomes (i.e., heart rate, blood pressure) could be included in future perinatal research for objective measures;(39,58,59) however, subject burden must be considered. A longer period of follow-up at the one-year mark would be desirable, keeping in mind budget and financial constraints.
Additional important limitations to this study are potential for bias and internal control. The principle investigator is a massage therapist, which carries the risk of confirmation bias, or favoring one outcome over another based on evidence that confirms ones’ beliefs.(60) Additionally, the participants could have been experiencing social desirability response bias or sympathy or compassion for the investigator, aware of project work efforts, and therefore inflating responses to appear more favorable.(61) Lastly, an in-home protocol delivered by multiple partners is more difficult to control than in a private lab setting with a single therapist. The tradeoff, however, in this case, is increased external validity through a real-world, translatable application that can be tailored to each family’s needs.
Twelve perinatal women and their partners demonstrated high rates of study retention and compliance with the intervention and responded well to treatment. No adverse events were attributed to the study. Analyses supported the hypothesis that participants would experience improvements to perinatal mood, anxiety, and pain with a partner-delivered 10-minute chair massage. The chair massage took half the time and the study occurred over less period of investigation than the previously studied side-lying method.(13,32,33) This study presents the first research on partner-delivered chair massage as a safe and effective public health complementary intervention for perinatal mood, anxiety, and pain.
The author declares no institutional, corporate, or financial conflicts. All study aspects carried out by the author.
1 Falah-Hassani K, Shiri R, Dennis C-L. The prevalence of antenatal and postnatal co-morbid anxiety and depression: a meta-analysis. Psychol Med. 2017;47(12):2041–2053.

2 Grote NK, Bridge JA, Gavin AR, Melville JL, Iyengar S, Katon WJ. A meta-analysis of depression during pregnancy and the risk of preterm birth, low birth weight, and intrauterine growth restriction. Arch Gen Psychiatry. 2010;67(10):1012–1024.


3 Gelaye B, Rondon MB, Araya R, Williams MA. Epidemiology of maternal depression, risk factors, and child outcomes in low-income and middle-income countries. Lancet Psychiat. 2016;3(10):973–982.
4 Anderson FM, Hatch SL, Comacchio C, Howard LM. Prevalence and risk of mental disorders in the perinatal period among migrant women: a systematic review and meta-analysis. Arch Womens Ment Health. 2017;20(3):449–462.


5 O’Hara MW, Wisner KL. Perinatal mental illness: definition, description and aetiology. Best Pract Res Clin Obstet Gynaecol. 2014;28(1):3–12.
6 Almond P. Postnatal depression: a global public health perspective. Perspect Public Health. 2009;129(5):221–227.

7 Baker-Ericzen M, Connelly C, Hazen A, Duenas C, Landsverk J, Horwitz S. A collaborative care telemedicine intervention to overcome treatment barriers for Latina women with depression during the perinatal period. Fam Syst Health. 2012;30(3): 224–240.


8 Hübner-Liebermann B, Hausner H, Wittmann M. Recognizing and treating peripartum depression. Dtsch Arztebl Int. 2012;109(24):419–424.

9 Wisner K, Parry B, Piontek C. Clinical practice: postpartum depression. N Engl J Med. 2002;347(3):194–199.

10 Andersson L, Sundstrom-Poromaa I, Wulff M, Astrom M, Bixo M. Implications of antenatal depression and anxiety for obstetric outcome. Obstet Gynecol. 2004;104(3):467–476.

11 Kurki T, Hiilesmaa V, Raitasalo R, Mattila H, Ylikorkala O. Depression and anxiety in early pregnancy and risk for preeclampsia. Obstet Gynecol. 2000;95(4):487–490.
12 Sugiura-Ogasawara M, Furukawa TA, Nakano Y, Hori S, Aoki K, Kitamur T. Depression as a potential causal factor in subsequent miscarriage in recurrent spontaneous aborters. Hum Reprod. 2002;17(10):2580–2584.

13 Field T, Diego MA, Hernandez-Reif M, Schanberg S, Kuhn C. Massage therapy effects on depressed pregnant women. J Psychosom Obstet Gynecol. 2004;25(2):115–122.
14 Field T. Prenatal depression risk factors, developmental effects and interventions: a review. J Pregnancy Child Health. 2017;4(1):1–25.
15 Dunkel Schetter C, Niles AN, Guardino CM, Khaled M, Kramer MS. Demographic, medical, and psychosocial predictors of pregnancy anxiety. Paediatr Perinat Epidemiol. 2016;30(5):421–429.

16 Field T. Touch for socioemotional and physical well-being: a review. Dev Rev. 2010;30(4):367–383.
17 Behrman RE, Butler AS, eds. Preterm Birth: Causes, Consequences, and Prevention. Institute of Medicine (IOM) Committee on Understanding Premature Birth & Assuring Health Outcomes. Washington, DC: The National Academies Press; 2007.
18 O’Hara MW, McCabe JE. Postpartum depression: current status and future directions. Annu Rev Clin Psychol. 2013;9:379–407.
19 Field T, Diego M, Hernandez-Reif M. Prenatal depression effects and interventions: a review. Infant Behav Dev. 2010;33(4):409–418.


20 Hoffman MC, Wisner KL. Psychiatry and obstetrics: an imperative for collaboration. Am J Psychiatry. 2017;174(3):205–207.


21 Allen J, Balfour R, Bell R, Marmot M. Social determinants of mental health. Int Rev Psychiatry. 2014;26(4):392–407.

22 Topiwala A, Hothi G, Ebmeier KP. Identifying patients at risk of perinatal mood disorders. Practitioner. 2012;256(1751): 2,15–18.
23 Battle CL, Salisbury AL, Schofield CA, Ortiz-Hernandez S. Perinatal antidepressant use: understanding women’s preferences and concerns. J Psychiatr Pract. 2013;19(6):443–453.


24 Goodman JH. Women’s attitudes, preferences, and perceived barriers to treatment for perinatal depression. Birth. 2009;36(1):60–69.

25 Hall HG, Griffiths DL, McKenna LG. The use of complementary and alternative medicine by pregnant women: a literature review. Midwifery. 2011;27(6):817–824.

26 Hall HR, Jolly K. Women’s use of complementary and alternative medicines during pregnancy: a cross-sectional study. Midwifery. 2014;30(5):499–505.
27 Ko JY, Farr SL, Dietz PM, Robbins CL. Depression and treatment among U.S. pregnant and nonpregnant women of reproductive age, 2005–2009. J Women’s Health. 2012;21(8):830–836.
28 Steel A, Adams J, Sibbritt D, Broom A, Gallois C, Frawley J. Utilisation of complementary and alternative medicine (CAM) practitioners within maternity care provision: results from a nationally representative cohort study of 1,835 pregnant women. BMC Pregnancy Childbirth. 2012;12(1):146.


29 Deligiannidis KM, Freeman MP. Complementary and alternative medicine therapies for perinatal depression. Best Pract Res Clin Obstet Gynaecol. 2014;28(1):85–95.

30 Hall H, Cramer H, Sundberg T, Ward L, Adams J, Moore C, et al. The effectiveness of complementary manual therapies for pregnancy-related back and pelvic pain: a systematic review with meta-analysis. Medicine (Baltimore). 2016;95(38):e4723.
31 Field T. Prenatal anxiety effects: a review. Infant Behav Dev. 2017;49:120–128.

32 Field T, Figueiredo B, Hernandez-Reif M, Diego M, Deeds O, Ascencio A. Massage therapy reduces pain in pregnant women, alleviates prenatal depression in both parents and improves their relationships. J Bodyw Mov Ther. 2008;12(2):146–150.

33 Field T, Diego M, Hernandez-Reif M, Deeds O, Figueiredo B. Pregnancy massage reduces prematurity, low birthweight and postpartum depression. Infant Behav Dev. 2009;32(4):454–460.

34 Naruse SM, Cornelissen PL, Moss M. ‘To give is better than to receive?’ Couples massage significantly benefits both partners’ wellbeing. J Health Psychol. April 2018:135910531876350 [Epub ahead of print].
35 Salvo SG. Massage Techniques, Joint Mobilizations, and Stretches. In: Salvo SG, author. Masssage Therapy Principles and Practice, 5th ed. St. Louis, MI: Elsevier; 2016:136–177.
36 Tappan FM. General Procedures of Massage. In: Tappan FM, author. Healing Massage Techniques, Holistic, Classic, and Emerging Methods, 2nd revised ed. Norwalk, CT: Appleton & Lange; 1988:67–69.
37 Fritz S. Body Mechanics. In: Mosby’s Fundamentals of Therapeutic Massage, 2nd ed. St. Louis, MO: Mosby; 1999:251–278.
38 Benjamin PJ. Social and Communication Skills. In: Professional Foundations for Massage Therapists. Upper Saddle River, NJ: Pearson Prentice Hall; 2009:107–129.
39 Field T. Massage therapy research review. Complement Ther Clin Pract. 2014;20(4):224–229.


40 Cox JL, Holden JM, Sagovsky R. Detection of postnatal depression: development of the 10-item Edinburgh Postnatal Depression scale. Br J Psychiatry. 1987;150(JUNE):782–786.

41 Bergink V, Kooistra L, Lambregtse-van den Berg MP, Wijnen H, Bunevicius R, van Baar A, et al. Validation of the Edinburgh Depression Scale during pregnancy. J Psychosom Res. 2011;70(4):385–389.

42 Chorwe-Sungani G, Chipps J. A systematic review of screening instruments for depression for use in antenatal services in low resource settings. BMC Psychiatry. 2017;17(1):112.


43 Spielberger C, Gorsuch R, Lushene R, Vagg P, Jacobs G. State-Trait Anxiety Inventory for AdultsTM: Manual. Menlo Park, CA: Mind Garden, Inc.; 1983.
44 Newham JJ, Westwood M, Aplin JD, Wittkowski A. State-Trait Anxiety Inventory (STAI) scores during pregnancy following intervention with complementary therapies. J Affect Disord. 2012;142(1–3):22–30.

45 Hjermstad MJ, Fayers PM, Haugen DF, Caraceni A, Hanks GW, Loge JH, et al. Studies comparing Numerical Rating Scales, Verbal Rating Scales, and Visual Analogue Scales for assessment of pain intensity in adults: a systematic literature review. J Pain Symptom Manage. 2011;41(6):1073–1093.

46 Mujezinovic F, Alfirevic Z. Analgesia for amniocentesis or chorionic villus sampling. Cochrane Database Syst Rev. 2011;(11):CD008580.
47 Wu WH, Meijer OG, Uegaki K, Mens JM, van Dieën JH, Wuisman PI,,et al. Pregnancy-related pelvic girdle pain (PPP), I: Terminology, clinical presentation, and prevalence. Eur Spine J. 2004;13(7):575–589.


48 Kannisto KA, Koivunen MH, Välimäki MA. Use of mobile phone text message reminders in health care services: a narrative literature review. J Med Internet Res. 2014;16(10):e222.


49 Laiyemo MA, Nunlee-Bland G, Lombardo FA, Adams RG, Laiyemo AO. Characteristics and health perceptions of complementary and alternative medicine users in the United States. Am J Med Sci. 2015;349(2):140–144.

50 Kristoffersen AE, Stub T, Musial F, Fønnebø V, Lillenes O, Norheim AJ. Prevalence and reasons for intentional use of complementary and alternative medicine as an adjunct to future visits to a medical doctor for chronic disease. BMC Complement Altern Med. 2018;18(1):109.


51 American College of Obstetricians and Gynecologists (ACOG) Committee on Practice Bulletins—Gynecology. Early pregnancy loss. Practice Bulletin No. 150. Obstet Gynecol. 2015:125(5):1258–1267.

52 Lee AM, Lam SK, Sze Mun Lau SM, Chong CSY, Chui HW, Fong DYT. Prevalence, course, and risk factors for antenatal anxiety and depression. Obstet Gynecol. 2007;110(5): 1102–1112.

53 Herrera I. Ending Pain in Pregnancy: Trade Secrets for an Injury-Free Childbirth, Relieving Pelvic Girdle Pain, and Creating Powerful Pelvic Muscles, 2nd ed. New York, NY: Duplex Publishing; 2016.
54 Mogren IM. BMI, pain and hyper-mobility are determinants of long-term outcome for women with low back pain and pelvic pain during pregnancy. Eur Spine J. 2006;15(7):1093–1102.


55 Smith CA, Levett KM, Collins CT, Dahlen HG, Ee CC, Suganuma M. Massage, reflexology and other manual methods for pain management in labour. Cochrane Database Syst Rev. March 2018;3:CD009290.

56 Madigan D, Cambron J, Kennedy AB, Burns K, Dexheimer J. Volunteerism of massage therapists: a MassageNet study [abstract]. Int J Ther Massage Bodywork. 2016;9(4):14–21.
57 Julious SA. Sample size of 12 per group rule of thumb for a pilot study. Pharm Statistics. 2005;4(4):287–291.
58 Gholami-Motlagh F, Jouzi M, Soleymani B. Comparing the effects of two Swedish massage techniques on the vital signs and anxiety of healthy women. Iran J Nurs Midwifery Res. 2016;21(4):402–409.


59 Givi M. Durability of effect of massage therapy on blood pressure. Int J Prev Med. 2013;4(5):511–516.

60 Elster J. Explaining Social Behavior: More Nuts and Bolts for the Social Sciences, 2nd ed. Cambridge, UK: Cambridge University Press; 2015.
61 Furnham A. Response bias, social desirability and dissimulation. Personal Individ Differ. 1986;7(3):385–400.
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 12, NUMBER 2, JUNE 2019