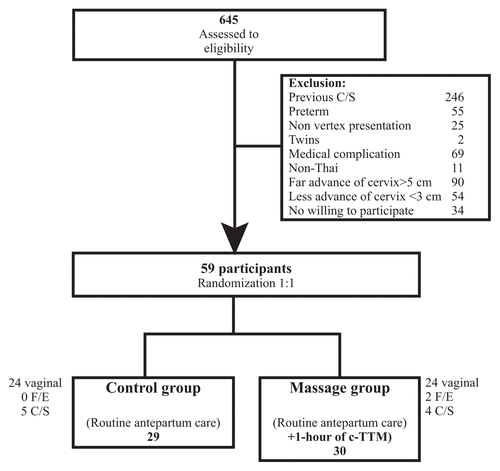
Figure 1 Consort flow diagram. F/E = forcepts extraction; C/S = Cesarean section.
Panya Sananpanichkul, MD1*, Chatchai Sawadhichai, MD, PhD2, Yosapon Leaungsomnapa, PhD3, Paweena Yapanya, BATM4
1Department of Obstetrics and Gynecology, Prapokklao Hospital, Chanthaburi, Thailand
2Department of Medicine, Prapokklao Hospital, Chanthaburi, Thailand
3Department of Adult and Elderly Nursing, Prapokklao Nursing College, Chanthaburi, Thailand
4Department of Thai Traditional Medicine and Alternative Medicine, Prapokklao Hospital, Chanthaburi, Thailand
Background and Objectives
Court-type Thai traditional Massage (c-TTM) applied during intrapartum may have some benefit other than pain relief. This study aimed to evaluate the effect of c-TTM during the first and second stage of labor, as well as pain alleviation in the first stage.
Methods
This was a randomized controlled trial study. Eligible participants were singleton pregnant mothers with cervical dilation between 3–5 cm and no medical complications. Both trial groups received the same routine antepartum care except for 1 hour additional c-TTM given to the experimental group when they were in the active phase of labor. The pain score was taken from the participants at the time before labor pains started, at the time of active labor, 1, 2, 3, and 4 hours after the intervention. Pain was recorded by the researcher using a visual analog scale. The primary outcome during the first and second stages of labor was compared between groups. Pain relief during the first stage of labor and analgesic drugs used were compared as a secondary outcome. This trial is registered under the identification number TCTR20171115003.
Results
Fifty-nine participants were enrolled and randomly assigned with 1:1 allocation to groups. The duration of first and second stage labor was significantly shorter in the experimental c-TTM than in the conventional control group (mean ± SD: 198.37 ± 62.80 minutes: 268.52 ± 137.81 minutes, p value =.02 and 17.54 ± 9.49 minutes: 23.35 ± 15.01 minutes, p value =.03, respectively). There was no difference of pain score between the groups.
Conclusion
One hour of c-TTM can significantly decrease the duration of the first and second stages of labor. The pain score recorded is not statistically different between the groups.
KEYWORDS: intrapartum, Thai massage, labor pain, nonpharmacological pain relief
Labor pain is still one of the obstacles for mothers who wish to try vaginal delivery. When the cervix is fully dilated, effective regular uterine contraction at appropriate intervals and expulsive maternal forces bring about delivery of the baby.(1) However, every time the uterus contracts, it brings about pain, anxiety, stress, and fear to the mother. Some mothers display behavior changes, such as irritability, agitation, anger, grimaces, moans, and cries for help every time the uterus contracts. These result in the change of biochemical substances in the body. Consequently, the sympathetic nervous system (SMS) is stimulated and releases catecholamine and epinephrine. These increase pain perception in the brain and decrease uterine contraction by blocking the release of oxytocin from the posterior pituitary.(2) Stress also increases cortisol hormone secretion, resulting in decreased blood supply to the uterus, and finally causes the uncoordinated myometrial contraction or protraction of labor.
Analgesia given during the intrapartum period is not only for somatic therapy but also for psychological therapy. Pharmacological approaches aim to decrease or eliminate the physical sensation of labor pain. By contrast, nonpharmacological approaches are mainly to increase comfort, help the laboring woman to cope with the pain and decrease suffering.(3)
The International Society for the Study of Pain describes pain as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage”.(4) Both uterine contraction and perineal pressure contribute to the pain experienced during labor. Uterine pain is typically transmitted via nerve roots T10 to L1, and perineal sensation is transmitted through nerve roots S2 to S4.(3) In theory, massage creates a stimulus via myelinated nerve fibers that interferes with the transmission of pain to the dorsal root ganglia, effectively “closing the gate” to the reception of pain.(5,6) It is suggested that massage stimulates the release of endorphins and increases serotonin levels to inhibit the transmission of noxious nerve signals to the brain.(7) Consequently, the benefits of intrapartum massage are a decrease in labor pain and anxiety level, shorter duration of labor,(8,9,10) and reduction of maternal depression in the prenatal period that results in greater gestational age and higher neonatal birthweight.(11)
Traditional Thai massage, a precious knowledge-system of Thailand, has been passed from generation to generation. It is believed that traditional Thai massage originated within families as family members offered relief to one another by using various parts of their body to relieve muscle pain. This type of massage is called Cha Loei Sak, or ‘unofficial massage’. ‘Official massage’ is performed using both hands and no other parts of the body. This is also known as court-type massage.(12)
This investigation aims to study the effectiveness of court-type Thai traditional massage (c-TTM) in decreasing the duration of the first and second stages of labor, as well as pain alleviation in the first stage of labor.
This study was an open-label, randomized controlled trial done between December 1, 2017 and February 28, 2018. Ethical approval was received from Chanthaburi Research Ethics Committee (COA number CTIREC 076), and the trial was registered to the Thai Clinical Trials Registry on November 14, 2017 (TCTR 20171115003).
Eligible participants were pregnant Thai woman who regularly attended antenatal care clinics. They were singleton pregnancies (37–41 completed weeks) with cephalic presentation, spontaneous labor pain with cervical dilation between 3–5 centimeters (first stage of labor), no medical complications, and willing to cooperate in the research. Exclusion criteria were multifetal pregnancy, previous cesarean section, abnormal uterine bleeding, and pre-existing medical complications such as cardiovascular disease, hypertension, and diabetes.
A randomized block design was employed during this experiment with 1:1 allocation. A web-based, computer-generated randomization sequence was prepared via the ‘Sealed Envelope’ website (https://www.sealedenvelope.com). The numbered opaque envelopes prepared by the researcher were opened directly after interview to reveal the allocation group.
Participants who met the inclusion criteria were informed of the study process by nurse and informed consent was obtained immediately after recruitment. The privacy rights of human subjects were always respected. The participants were then randomized using a 1:1 randomization ratio into two groups (the experimental group and the control group). Both groups were treated with routine antepartum care, while the study group received an hour of c-TTM from one licensed Thai traditional practitioner. Routine antepartum care was based on clinical practice guidelines of the institute. The pregnant women were assessed every 2 hrs, which included monitoring vital signs and fetal heart rate, as well as pelvic examination to evaluate the progression of labor.(13) Only one dosage of pethidine (25 mg.) was given intravenously for each participant upon request when there was a pain score of more than 8. Baseline characteristics such as age, parity, gestational age, education, residency, monthly income, height, and weight were recorded. Pain score was calculated using the visual analog scale (VAS), and was recorded by the researcher before labor pain started, at the time of active labor, and 1, 2, 3, and 4 hrs after the intervention.
In the c-TTM experimental group, the practitioner pressed and kneaded along designated lines (“sen”) and points of the body. The exception was for the abdomen, especially the uterus. The intensity of force was adjusted according to the sensitivity of muscle resistance. The practitioner usually pressed with soft and gentle pressure, holding down for a moment at each point on the body. The practitioner moved from one point to the next at intervals of 10–15 s.(14) The details of the body lines are described below.(12)
The “leg line” is divided into upper and lower sections. The practitioner starts from the upper section (thigh) to the lower part (ankle). The patient lies in a lateral recumbent position while the practitioner is behind on the bedside.
The “back line” starts from the waist or lower back along one side of the spine to the level of the neck. The practitioner circularly kneads behind the patient’s back and continues even if the uterus has contracted.(15) Then, the practitioner will press along the coccyx, sacrum and hip.
The “shoulder line” is the line starting from the inner scapula and moving along the vertebra line.
The “arm line” is separated into the outer and inner arm, and includes the palm.
For all the lines mentioned above, the practitioner pressed for 5 rounds per line and continued to knead according to the patient’s request. However, the time of c-TTM was strictly limited to 1 hr.
The sample size was calculated based on data from Silva Gallo et al.(16) The χ2 and t tests were used for univariate analysis of categorical and continuous data, respectively. The Mann-Whitney U test was used to compare when the dependent variable was either ordinal or continuous, but not normally distributed. Significance was set at as α of 0.05. Data were analyzed using SPSS V. 22 (IBM SPSS Statistics for Windows, Version 22.0).
A total of 645 women were eligible for the study, of whom 586 were excluded. The exclusion was due to previous cesarean section (246), preterm labor (55), nonvertex presentation (25), twin pregnancy (2), medical complication (69), non-Thai (11), inappropriate dilation of cervix (144), and no willingness to participate (34), as shown in Figure 1. Fifty-nine participants were included in the study. The demographic character of the participants is shown in Table 1.
|
|
||
|
Figure 1 Consort flow diagram. F/E = forcepts extraction; C/S = Cesarean section. |
||
Table 1 General Demographic Characteristic of the Population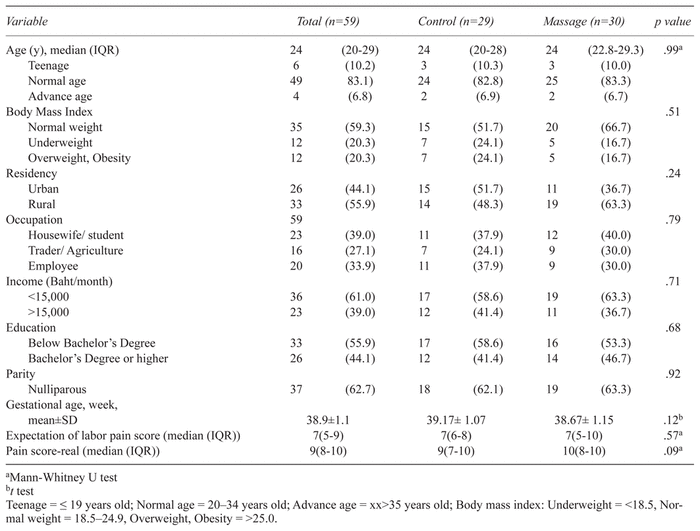
The duration of the first and second stages of labor was significantly shorter in the c-TTM experimental group than in the control group (mean ± SD: 198.37 ± 62.80 min: 268.52 ± 137.81 min, p value = .02 and 17.54 ± 9.49 min: 23.35 ± 15.01 min, p value = .03; respectively) (Table 2). There was no statistical difference of pain score during the intrapartum period between the groups, as shown in Table 3. Analgesic drugs were used less during the first stage of labor in the c-TTM experimental group than in the control group, but there was no statistical significance (14 (46.7%) and 18 (69.2%), p value = .09) (Table 2). The study showed that pregnant woman suffered from greater labor pain than they expected in both control and massage groups (expectation: experience; 7:9; 7:10; respectively) (Table 3).
Table 2 Intrapartum Characteristics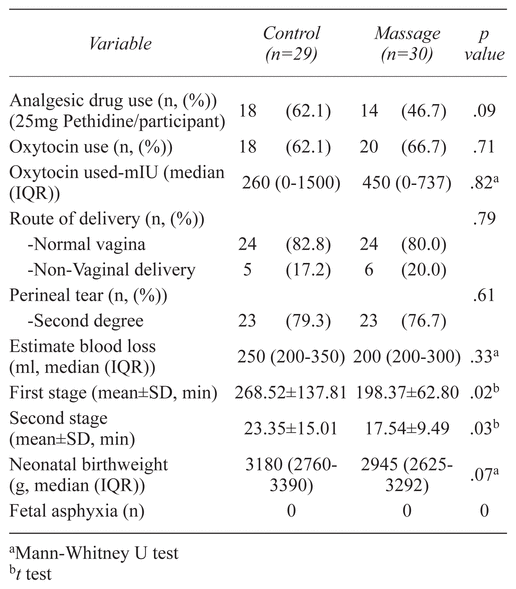
Table 3 Pain Score in First Stage of Labor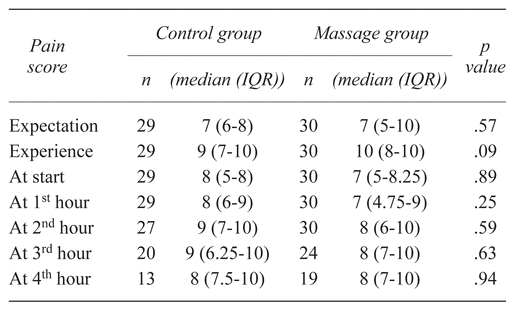
Massage with soft force along the shoulder, waist, hip, arm, hand, and leg can relieve pain during the second stage of labor.(8,9,10,17) Mortazavi et al.(8) studied 120 primiparous women and showed lower pain in the first and second stages of labor accompanied by a shorter duration of the active phase of labor in the experimental massage group. In all previous studies, massage or touch was applied to the pregnant woman at regular intervals in the first stage and/or in the second stage. This is a different procedure from the present study because c-TTM was applied only once in the active phase of labor. The data from this investigation do not show a decrease in the pain score of the massage group. Although pain score evaluation in the experimental group was not statistically different to the control group, the duration of the first and second stages of labor were significantly shorter in the c-TTM group. This supports the studies of Lund et al.(18) and Turner et al.,(19) who argued that one massage session stimulates oxytocin release from the neurohypophysis and repeated massage sessions stimulate an increase in pain threshold that seems to be mediated by an interaction between oxytocin and opioid neurons. Analgesic drugs were also used less in the c-TTM experimental group than in the control group, though this was not statistically significant. In future experiments, researchers should consider how long the effect from c-TTM lasts.
The global rate of cesarean section is about 19%. It ranges from 6% to 27% from the least to more developed regions, respectively.(20) In Thailand, the rate of cesarean section increases every year, ranging from 15.2% (1990) to 22.4% (1996) to 34% (2007) and 34.8% in 2009.(21,22) There is no evidence to support the benefits for women or infants of cesarean section performed with no indication. A systematic review in 2015 concluded that a cesarean section rate higher than 10% was not associated with reduction of maternal and neonatal mortality rate.(23,24)
One of the maternal reasons to choose elective operative delivery is avoidance of labor pain. This study showed that pregnant women suffered from greater labor pain than they expected. The c-TTM may be a form of complementary treatment added to the routine care package in order to alleviate pain and decrease the number of requested cesarean sections. This is supported by the fact that fewer analgesics were used in the c-TTM group, although this was not statistically significant.
The limitation of this study is the small sample size. Most of the pain scores reported in this paper relied on self-report measures, which may cause some error. As in many other countries, pregnant women have limited insurance coverage for this complementary therapy. The Thai Ministry of Health still does not support c-TTM as part of the national health program.
One hour of c-TTM can significantly decrease the duration of the first and second stages of labor, thus decreasing the potential duration of suffering from labor pain. Moreover, a decrease in the number of analgesic drugs used in first stage of labor was observed in the experimental c-TTM group, although there was no statistical difference. Promotion of 1 hr of c-TTM to target groups of pregnant women may be used as one strategy to decrease the rate of cesarean sections.
We would like to thank Dr. Surasawadee Sawadhichai for her graceful opinion.
The authors have no conflicts of interest relevant to this article and no funding support for this article.
1 Friedman EA. An objective approach to the diagnosis and management of abnormal labor. Bull NY Acad Med. 1972;48(6):842–858.
2 Zwelling E, Johnson K, Allen J. How to implement complementary therapies for labouring women. MCN Am J Matern Child Nurs. 2006;31(6):364–370.
3 Committee on Practice Bulletins-Obstetrics. Practice Bulletin No. 177: Obstetric analgesia and anesthesia. Obstet Gynecol. 2017;129(4):e73–e89.
4 Gebhart GF. Scientific issues of pain and distress. In: National Research Council (US) Committee on Regulatory Issues in Animal Care and Use. Definition of Pain and Distress and Reporting Requirements for Laboratory Animals: Proceedings of the Workshop Held June 22, 2000. Washington, DC: National Academies Press; 2000. Available from: https://www.ncbi.nlm.nih.gov/books/NBK99533/
5 Melzack R, Wall PD. Pain mechanisms: a new theory. Science. 1965;150(3699):971–979.
6 Deave T, Johnson D, Ingram J. Transition to parenthood: the needs of parents in pregnancy and early childhood. BMC Pregnancy Childbirth. 2008;8:30.
7 Brar S, Tang S, Drummond N, Palacios-Derflingher L, Clark V, John M, et al. Perinatal care for South Asian immigrant women and women born in Canada: telephone survey of users. J Obstet Gynaecol Can. 2009;31(8):708–716.
8 Mortazavi SH, Khaki S, Moradi R, Heidari K, Vasegh Rahimparvar SF. Effects of massage therapy and presence of attendant on pain, anxiety and satisfaction during labor. Arch Gynecol Obstet. 2012;286(1):19–23.
9 Chang MY, Chen CH, Huang KF. A comparison of massage effects on labor pain using the McGill Pain Questionnaire. J Nurs Res. 2006;14(3):190–197.
10 Field T, Hernandez-Reif M, Taylor S, Quintino O, Burman I. Labor pain is reduced by massage therapy. J Psychosom Obstet Gynaecol. 1997;18(4):286–291.
11 Field T. Massage therapy research review. Complement Ther Clin Pract. 2014;20(4):224–229.

12 Centre of Applied Thai Traditional Medicine, Ayurved Thamrong School. Court-type Thai traditional massage. Bangkok: Faculty of Medicine, Siriraj Hospital, Mahidol University; 2009. p.35–49.
13 Satin AJ, Leveno KJ, Sherman ML, Brewster DS, Cunningham FG. High-versus low-dose oxytocin for labor stimulation. Obstet Gynecol. 1992;80(1):111–116.
14 Chang M, Wang S, Chen C. Effects of massage on pain and anxiety during labour: a randomized controlled trial in Taiwan. J Advanced Nurs. 2002;38(1):68–73.
15 Kimber L. Effective techniques for massage in labor. Pract Midwife. 1998;1(4):36–39.
16 Silva Gallo RB, Santana LS, Jorge Ferreira CH, Marcolin AC, Polineto OB, Duarte G, et al. Massage reduced severity of pain during labour: a randomised trial. J Physiother. 2013;59(2):109–116. doi:10.1016/S1836-9553(13)70163-2
17 McNabb MT, Kimber L, Haines A, McCourt C. Does regular massage from late pregnancy to birth decrease maternal pain perception during labour and birth? A feasibility study to investigate a programme of massage, controlled breathing and visualization, from 36 weeks of pregnancy until birth. Complement Ther Clin Pract. 2006;12(3):222–231.
18 Lund I, Yu L-C, Uvnas-Moberg K, Wang J, Yu C, Kurosawa M, et al. Repeated massage-like stimulation induces long-term effects on nociception: contribution of oxytocinergic mechanisms. Eur J Neurosci. 2002;16:330–338.
19 Turner RA, Altemus M, Enos T, Cooper B, McGuiness T. Preliminary research on plasma oxytocin in normal cycling women: investigating emotion and interpersonal distress. Psychiatry. 1999;62(2):97–113.
20 Betrán AP, Ye J, Moller AB, Zhang J, Gülmezoglu AM, Torloni MR. The increasing trend in caesarean section rates: global, regional and national estimates: 1990–2014. PLoS One. 2016;11(2):e0148343. doi:10.1371/journal.pone.0148343
21 Hanvoravongchai P, Letiendumrong J, Teerawattananon Y, Tangcharoensathien V. Implications of private practice in public hospitals on the caesarean section rate in Thailand [original online article]. 2000 [cited 2018 March 15]. Available from: http://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.553.9700&rep=rep1&type=pdf
22 Festin MR, Laopaiboon, M, Pattanittum P, Ewens MR, Henderson- Smart DJ, Crowther CA. Caesarean section in four South East Asian countries: reasons for, rates, associated care practices and health outcomes. BMC Pregnancy Childbirth. 2009;9:17.

23 Betrán AP, Torloni MR, Zhang J, Ye J, Mikolajczyk R, Deneux-Tharaux C, et al. What is the optimal rate of caesarean section at population level? A systematic review of ecologic studies. Reprod Health. 2015;12:57.

24 Ye J, Zhang J, Mikolajczyk R, Torloni MR, Gülmezoglu AM, Betran AP. Association between rates of caesarean section and maternal and neonatal mortality in the 21st century: a worldwide population-based ecological study with longitudinal data. BJOG. 2016;123(5):745–753.

Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 12, NUMBER 1, MARCH 2019