Diane Mastnardo, BS, LMT1*, Jeanmarie C. Rose, MPA2, Jacqueline Dolata, MBA3, James J. Werner, PhD, MSSA4,56
1Massage of Northern Ohio Practice-Based Research Network, Cleveland, OH, USA
2Center for Community Health Integration, Case Western Reserve University, Cleveland, OH, USA
3Center for Reducing Health Disparities, Case Western Reserve University, Cleveland, OH, USA
4Department of Family Medicine and Community Health, Case Western Reserve University, Cleveland, OH, USA
5Department of Psychiatry, Case Western Reserve University, Cleveland, OH, USA
6Mandel School of Applied Social Sciences, Case Western Reserve University, Cleveland, OH, USA
Background
Communication between massage therapy patients and their medical providers has not been widely described, especially with respect to health care in the United States.
Purpose
To examine which type of medical providers recommend massage therapy (MT), and how often massage therapy patients tell their providers about their treatment.
Setting
Independent massage therapy practices in a Practice-based Research Network (PBRN) in Northeast Ohio.
Participants
21 licensed massage therapists (LMT).
Research Design
A cross-sectional descriptive study. For consecutive, nonrepeating visits to their practices, each LMT completed up to 20 cards with information on the patient and visit. Analysis compared visits for patients based on whether they reported telling their health provider about their use of MT or being recommended for massage by a health provider.
Results
Among 403 visits to 21 LMTs, 51% of patients had told their primary care clinician about seeing an LMT, and for 23%, a health-care provider had recommended visiting an LMT for that visit. Patients who told their primary care provider that they use massage therapy were more likely to be established patients, or to be seen for chronic pain complaints. Visits recommended by a physician were more likely to be for chronic conditions.
Conclusion
Patients who are established in the massage practice and those receiving massage for a specific condition are more likely to tell their primary care provider that they use massage and are also more likely to have been recommended for massage by a health-care provider. This information will help LMTs target and inform patients about the importance of talking with their health-care providers about their use of massage, and provide LMTs with a starting point of which types of health-care providers already recommend massage. This information will further open the dialogue about the integration of massage therapy in conventional health care.
KEYWORDS: massage therapy, card study method, integrative health, patient provider communication
Massage therapy is one of the 10 most commonly used types of complementary and integrative healthcare (CIH) therapies in the United States.(1) Massage therapy is sometimes recommended by health-care providers; however, numerous factors limit the full integration of massage therapy into health care, including the low priority placed on massage and other CIH therapies during medical training.(2) This can result in reduced confidence in recommending massage therapy to patients,(2,3) which limits the development of professional relationships between health-care providers and massage therapists to more fully address patients’ health-care needs.(4)
Patients often refrain from disclosing to their physician about their use of CIH therapies. A systematic review of 12 studies found that rates of nondisclosure ranged from 23% to 72%.(4) Reasons for nondisclosure to health-care providers included patients’ perception that their provider lacked an understanding of CIH therapies, patients’ fear of a negative response from the provider, and because the provider had never asked the patient about whether they were using CIH therapies.(5,6,7)
Understanding why patients choose not to disclose CIH therapies to health-care providers is an important step in improving health-care communication. Less is known, however, about barriers and enabling factors for communicating with health-care providers about massage therapy specifically, which is a more broadly accepted modality than many CIH therapies.(1) In addition, little is known about which specialties recommend massage therapy most often, and the types of health conditions that are most likely to be referred for massage. The purpose of the study reported here was to investigate these questions. The study was approved by the Institutional Review Board of University Hospitals Cleveland Medical Center.
This study was implemented in a practice-based research network (PBRN) of licensed massage therapists (LMTs) in Ohio, the Massage Northern Ohio Practice-Based Research Network (MNO-PBRN). Its mission is to study important issues related to massage therapy, and translate research findings into practice. It is the first known PBRN of regional massage therapists.
A cross-sectional study was designed using the PBRN card study method, in which clinicians use a brief survey to record deidentified information about a series of visits. The card study method allows the clinician to quickly collect a small amount of observational data without interrupting the course of routine practice.(8,9,10)
The research questions and card study items were developed by the MNO-PBRN steering committee with guidance from a clinical research facilitator from the PBRN Shared Resource. The card was reviewed by members of MNO-PBRN, and it is provided in Appendix A. Implementation instructions were provided at a semi-annual membership meeting. The data collection card consisted of six multipart questions to capture information, including massage patients’ demographics, reason for visit to the massage therapist, whether patients disclosed use of massage to healthcare providers, reasons for nondisclosure, and the specialty of health-care providers who recommended massage therapy to the patient. Practice volume varies for LMTs within the PBRN from 5 to 30 massages per week, to allow equal participation and decrease potential bias; higher volume practices collected more cards than smaller practices with the members chosing up to 20 cards to be collected per therapist.
Each participating LMT filled out up to 20 data collection cards with deidentified data immediately after consecutive, nonrepeating visits by eligible massage patients, beginning with a self-chosen index date during a two-month period. If a patient was seen more than once during the collection period, only their first visit was recorded. All cards were mailed in a self-addressed envelope to the research facilitator for analysis. Eligible patients were adults over the age of 18; anyone under 18 years of age was excluded.
Participation in the card study was open to any active licensed massage therapist (LMT) who was a member of the MNO-PBRN. Criteria for becoming a member of the PBRN is holding an active Massage Therapy License. There are currently 60 registered members. Active members attended at least one meeting within the past year. Twenty-six active members attended the semi-annual meeting where the card was reviewed, and 21 LMTs participated in the study.
Analysis was conducted by the research facilitator and data analyst, and cross-referenced by the lead author for consistency. All variables were categorical, and descriptive statistics were computed to examine the distributions. Pearson’s chi-squared test for independence was used to determine the extent to which associations existed between the categorical variables. We used an alpha level of .05 for all statistical tests.
A total of 403 study cards were returned by 21 participating massage therapists.
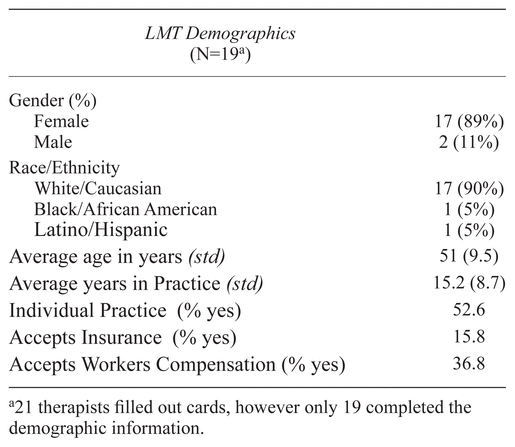
Nineteen of the twenty-one participating LMTs returned personal demographic information with their cards. The majority of participating massage therapists self-designated as White/Caucasian (90%) females (89%), with an average age of 51 years, who have been in practice on average for 15 years. Their practices were mostly independent (52%), some accepted workers compensation (36.8%), and fewer accepted insurance (15.8%), as shown in Table 1 and consistent with industry standards.(11)
Table 1 Characteristics of Participating Licensed Massage Therapists (LMTs)
The majority of patients were female (65.3%) and were established in a massage practice (75.0%). Established is defined for this study as seen by therapist more than once. Approximately two-thirds received massage for a specific complaint (65.1%), and onehalf of complaints involved musculoskeletal pain (49.9%), as shown in Table 2. Approximately one-half of patients indicated that they informed their healthcare provider about their use of massage therapy. The most frequently selected option for not disclosing the use of massage was that it did not occur to the patient to tell the provider. Primary care providers recommended patients for massage most frequently (38.7%), followed by orthopedists (19.4%).
Table 2 Characteristics of Patients and Visits with LMT
As shown in Table 3, patients who were new to the massage practice were significantly less likely to tell providers that they use massage than established patients (31.7% vs. 56.5%, p < .001). Patients seeking massage for a specific problem were significantly more likely to inform their health-care providers of their use of massage than patients seeking massage for general relaxation (56.2% vs. 40.3%, p < .002).
Table 3 Characteristics of Patients and Visits by Disclosure Attitude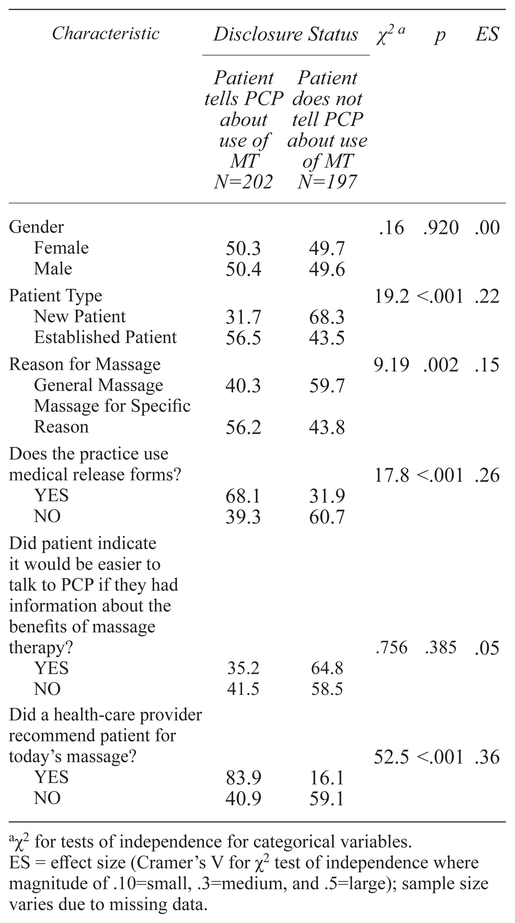
Health-care providers were significantly more likely to recommend massage for patients who reported a specific complaint at the massage visit than patients who did not have a specific complaint (31.1% vs. 8.8%, p < .001; see Table 4). Patients who informed their health-care provider about their use of massage were significantly more likely to have massage recommended by their provider (38.6% vs. 7.7%, p < .001).
Table 4 Characteristics of Patients and Visits by Recommendation Status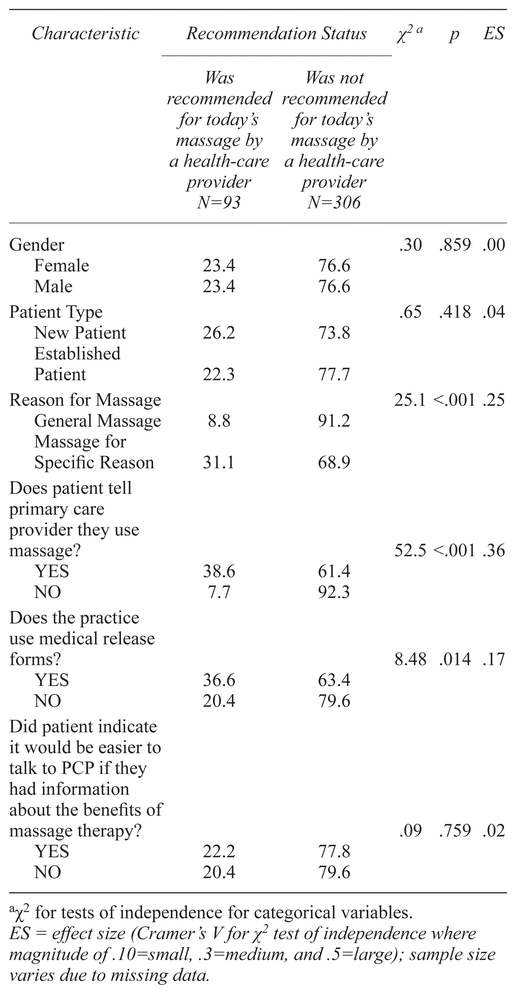
We also found significant associations between the type of massage visit (specific complaint vs. general massage) and patients’ interest in obtaining information about massage that can be shared with health-care providers. Of those who indicated it would be easier to talk to their provider if they had information about the benefits of massage therapy, most were using massage for a specific complaint (90.7%) versus those receiving general massage (9.3%, p < .05). Furthermore, when available, those who signed a release of information form allowing the LMT to communicate with their medical provider were more likely to be receiving massage for a specific complaint (80.3%) versus general massage (19.7%, p < .001).
We found that the majority of participants who received a recommendation from a health-care provider for massage, either currently or in the past, reported receiving it from a primary care provider (PCP) (38.7%). Perhaps this is because massage is most successful at the early stages of discomfort or disease when patients are likely to seek care at primary care offices.(12) While “Other practitioner” totaled 48.4%, this category included 15 provider types. Chiropractor and physical therapist referred the most.
Patients seeking massage for a specific condition were more likely to tell their providers about their use of massage than patients obtaining general massage. These results are consistent with the findings of Rao et al.(13) who found that that patients who use CIH therapies to manage a specific diagnosis are more likely to inform their doctors of their use of CIH.
Patients who received massage for a specific condition were more likely to tell their providers they use massage. Interestingly, these patients were also more likely to indicate that it would be easier for them to discuss massage with their PCPs if provided with information about the benefits of massage. They were also more likely to sign a release form, when available, giving their LMT permission to communicate with their provider. This suggests that patients telling their providers about massage express an interest to open up even more communication between themselves and their health-care providers and between their LMTs and their providers. This suggests that patients with muscularskeletal pain and chronic conditions are seeking a more holistic approach to health care, and working towards closing the gap between LMTs and health-care providers. For some of these patients, massage may be a vital component of their pain management, and the desire to bring more attention to the practice is important to their wellness.
Furthermore, it is promising that one-half of patients informed their health-care providers that they use massage therapy. “Did not occur to patient” was the main reason patients reported for not telling their provider about their use of massage therapy. It is reassuring that patients did not refrain from informing their providers out of fear or discomfort, but simply did not think to communicate. However, this may suggest that patients regard massage as a significantly different modality from those used in conventional health care. Additionally, the second most-stated reason for patients not disclosing their use of massage to providers was that the provider did not ask, which is consistent with research that found that physicians do not usually ask patients about their use of CIH and they mainly find out about patient use via patient self-disclosure.(14,15) This knowledge can help LMTs encourage patients to communicate with their providers about their use of massage as this may lead to more patient-centered care.
LMTs have been seeking to gain legitimacy in conventional health care for some time, and perhaps the best way to achieve this is to develop professional relationships with individual health-care providers. The literature indicates that many primary care providers want to learn more about CIH and massage so they can properly recommend therapies that are safe and effective and dissuade patients from harmful practices.(14,15,16,17) A starting point for LMTs may be to reach out to providers who are already recommending massage to their patients’ and offer to share useful patient tools and evidence-based information with them. By being of assistance and building trust, LMTs can create mutually beneficial working relationships, while PCPs develop a more complete understanding of the therapeutic applications of massage. This may open opportunities for professional organizations in massage therapy to develop PBRN methodology, learn from stakeholders, and help bridge the gap between primary care and massage therapy.(18)
This cross-sectional observational study was not designed to test hypotheses or find causal relationships, but rather to permit a description of patients’ reasons for obtaining massage and their communication about massage with their health-care providers. The study was conducted in a relatively small geographical area (northeast Ohio) and its findings may not generalize to other settings. Finally, readers should be cautioned in interpreting findings from patients who reported both receiving a recommendation for massage from their health-care provider and informing their provider of their use of massage. Due to the design of the data collection card, it is not known if these patients informed their providers before or after their providers recommended massage. These situations are substantially different, as providers who recommended massage prior to patients mentioning their use of it may have significant confidence in the potential benefits of massage. Conversely, providers who recommended massage after learning about patients’ use of it may have endorsed it largely because it was already being used by the patient.
This publication was made possible by the Clinical and Translational Science Collaborative of Cleveland, UL1TR000439 from the National Center for Advancing Translational Sciences (NCATS) component of the National Institutes of Health and NIH Roadmap for Medical Research, and in part by grants MD002265 and TR000439 from the National Institutes of Health. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the NIH.
The authors have indicated they have no potential conflicts of interest to disclose.
1 Barnes PM, Powell-Griner E, McFann K, Nahin RL. Complementary and alternative medicine use among adults: United States, 2002. Adv Data. 2004;(343):1–19.
2 Wahner-Roedler DL, Vincent A, Elkin PL, Loehrer LL, Cha SS, Bauer BA. Physicians’ attitudes toward complementary and alternative medicine and their knowledge of specific therapies: a survey at an academic medical center. Evid-Based Complement Alt Med. 2006;3(4):495–501.
3 Rich GJ. Massage therapy: significance and relevance to professional practice. Prof Psychol Res Pract. 2010;41(4):325–332.
4 Frenkel MA, Borkan JM. An approach for integrating complementary– alternative medicine into primary care. Fam Pract. 2003;20(3):324–332.
5 Robinson A, McGrail MR. Disclosure of CAM use to medical practitioners: a review of qualitative and quantitative studies. Complement Ther Med. 2004;12(2–3):90–98.
6 Chao MT, Wade C, Kronenberg F. Disclosure of complementary and alternative medicine to conventional medical providers: variation by race/ethnicity and type of CAM. J Nat Med Assoc. 2008;100(11):1341–1349.
7 Davis EL, Oh B, Butow PN, Mullan BA, Clarke S. Cancer patient disclosure and patient-doctor communication of complementary and alternative medicine use: a systematic review. Oncologist. 2012;17(11):1475–1481.

8 Green LA. The weekly return as a practical instrument for data collection in office based research. Fam Med. 1988;20(3): 182–184.
9 Green LA, Reed FM, Miller RS, Iverson DC. Verification of data reported by practices for a study of spontaneous abortion. Fam Med. 1988;20(3):189–191.
10 Westfall JM, Zittleman L, Staton EW, Parnes B, Smith PC, Niebauer LJ, et al. Card studies for observational research in practice. Ann Fam Med. 2011;9(1):63–68.

11 American Massage Therapy Association (AMTA). Massage Therapy Industry Fact Sheet. Evanston, IL: AMTA; 2018. Available from: https://www.amtamassage.org/infocenter/economic_industry-fact-sheet.html#profession Accessed June 2, 2019.
12 Van Haselen RA, Reiber U, Nickel I, Jakob A, Fisher PAG. Providing complementary and alternative medicine in primary care: the primary care workers’ perspective. Ther Med. 2004;12(1):6–16.
13 Rao JK, Mihaliak K, Kroenke K, Bradley J, Tierney WM, Weinberger M. Use of complementary therapies for arthritis among patients of rheumatologists. Am Intern Med. 1999;131(6):409–416.
14 Winslow LC, Shapiro H. Physicians want education about complementary and alternative medicine to enhance communication with their patients. Arch Intern Med. 2002;162(10):1176–1181.
15 Schofield P, Diggens J, Charleson C, Marigliani R, Jefford M. Effectively discussing complementary and alternative medicine in a conventional oncology setting: communication recommendations for clinicians. Patient Edu Counsel. 2010;79(2):143–151.
16 Flannery MA, Love MM, Pearce KA, Luan J, Elder WG. Communication about complementary and alternative medicine: perspectives of primary care clinicians. Altern Ther Health Med. 2006;2(1):56–63.
17 Wardle JL, Sibbritt DW, Adams J. Referral to massage therapy in primary health care: a survey of medical general practitioners in rural and regional New South Wales, Australia. J Manip Physiol Ther. 2013;36(9):595–603.
18 Munk N, Dyson-Drake J, Mastnardo D. What should we do different, more, start and stop? Systematic Collection and Dissemination of Massage Education Stakeholder Views from the 2017 Alliance for Massage Therapy Educational Congress. IJTMB. 2019;12(1):29–39.

|
|
||
|
|
||
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 12, NUMBER 3, September 2019