Manju Mohan, RN, RM, Linda Varghese, RN, RM*
Department of Obstetrical and Gynecological Nursing, Amrita College of Nursing, Amrita Vishwa Vidyapeetham, Kerala, India.Background
Reflexology may help induce labour and reduce pain during childbirth. Fear of pain associated with childbirth leads to increase in the irregular use of cesarean method.
Purpose
This study was performed to evaluate the effect of reflexology on relieving labour pain and assess the recipient’s opinion regarding foot reflexology.
Setting
The study taken place in the labour room, Amrita Institute of Medical Sciences, Kerala, South India.
Participants
50 primigravida patients experiencing labour.
Research Design
A quasi-experimental study design was used. Subjects were selected by convenience sampling technique with the first 25 patients allocated to the experimental group and the successive 25 primigravida mothers to a time-control group, to avoid data contamination.
Intervention
Intervention consisted of foot reflexology applied by a trained therapist to five pressure points of both feet that correspond to the uterus. Total intervention time lasted 20 minutes. Control group rested quietly for 20 minutes to serve as a time control.
Main Outcome Measure(s)
Pain associated with labour was recorded on a visual analogue scale immediately prior to intervention, and at 20- and 40-minutes postintervention. Patient satisfaction with reflexology treatment was recorded.
Results
Mean baseline pain score in foot reflexology group was significantly reduced across the study timeframe relative to control group (p < .001). Post hoc tests confirmed a reduction in labour pain at both the 20-min (p < .001, 95%CI 0.764–1.796) and 40-min (p < .001, 95%CI 0.643–1.677) time points. Eighty-one per cent of patients would recommend reflexology during labour.
Conclusion
The findings showed that foot reflexology was effective in relief of labour pain, with a high degree of patient satisfaction in primigravida mothers.
KEYWORDS: foot reflexology, labour pain, primigravida mothers
Pregnancy, childbirth, and motherhood are times during which a woman undergoes a vast change in her body, and it can be termed as an entirely new birth for the woman or as a time of rebirth.(1) The act of giving birth is the only moment when both pain and pleasure converge in a moment of time. The birth starts with the onset of labour, which is usually marked by the beginning of regular uterine contractions. Labour pain is due to contractions, distention of the lower uterine segment, pulling on pelvic ligaments, dilatation of cervix, and stretching of vagina and pelvic floor.(2) Although each labour is different and unique in its own way, labour is generally divided into three main stages: first, second, and third stages.
Among the non-pharmacological methods(3) for labour, pain reflexology is one of the best methods because it is safe, free from side effects, giving lasting cure, economical, and it is compatible with other forms of treatment.(4) Labour is a series of events by which uterine contractions and abdominal pressure expel the fetus, placenta and membranes out of the uterus through the birth canal. The first stage of labour, which is much longer than the second and third stages combined, is divided into three phases. The latent or preparatory phase begins at the onset of regularly perceived uterine contractions and ends when rapid cervical dilatation begins. The active phase begins from cervical dilatation of 4 cm to 7 cm. The transition phase begins from cervical dilatation of 8 cm to 10 cm.(5)
Pain is a physiological component of labour and birth, and an unpleasant sensation of distress resulting from stimulation of sensory nerves. During the first stage of labour, pain results primarily from cervical dilatation and secondarily from the uterine contractions themselves. Painful sensations travel from the uterus via visceral afferent (sympathetic) nerves that enter the spinal cord through the posterior segments of thoracic spinal nerves. The areas of referred pain include the lower abdominal wall, the area over the lumbar region, and the upper sacrum.(6)
Management of pain in labour has a beneficial effect on both mother and fetus.(7) The pharmacological methods include analgesia, which reduces or decreases awareness of pain, and anesthesia which causes partial or complete loss of sensation, but such drugs have many adverse effects.(8) They may cause maternal hypotension that decreases blood flow to the placenta, resulting in foetal hypoxia and acidosis. Drugs may also slow labour progress if given too early before labour is well established. However, non-pharmacological methods include counter pressure, therapeutic touch, walking, rocking, application of heat and cold, transcutaneous electrical nerve stimulation (TENS), showers, breathing techniques, listening to music, imaginary, childbirth education, and reflexology which has no side effects.(9)
Reflexology is the application of appropriate pressure to specific points and areas on the feet, hands, or ears. Reflexologists believe that these areas and reflex points correspond to different body organs and systems, and have a beneficial effect on the organs and a person’s general health. Reflexology massage is a type of massage that uses the thumb and the forefinger to stimulate some focal points on the foot. It is said that the foot has more than 7,000 nerve endings, which are linked to various organs in the body. Stimulating and applying pressure on these nerve endings can assist with a number of physical problems.(10) The advantages of foot reflexology are improvement in circulation and toxin removal, stimulation of lymphatic drainage, and the boosting of the immune system. It helps to reduce the stiffness and improve flexibility, and also accelerates physical healing, stress relief, sleep, and clarity. North American Indian tribes knew the relationship between the reflex points and the internal organs of the body and used this knowledge to treat disease.(11)
Reflexology has shown to help induce labour and reduce pain during childbirth. In fact, more and more nurses are beginning to learn this specialized type of foot massage and are using it in delivery rooms around the world to ease their patients’ discomfort and reduce the length of labour. While reflexology is best known as a specialized type of foot massage, it is performed on the hands as well.(12) Thus the investigator has a need to assess the effect of reflexology on labour pain and labour duration among primigravida mothers, and also to assist the midwives in assessing the nature and types of labour pain before and after foot reflexology and in managing that pain appropriately. Present study signifies the importance of empowering the Primigravida mothers to cope with labour pain. Managing pain also helps mothers to ease the labour process by reducing the labour duration.
Objectives of the study were to:
Evaluate the effect of foot reflexology on labour pain among primigravida mothers during the first stage of labour; and
Assess the experience regarding foot reflexology during labour among primigravida mothers in the experimental group.
The research design selected for the study was quasi-experimental, non-randomized pre-test/post-test design with intervention and control groups. In order to identify the effect of foot reflexology on labour pain, it is assessed before and after the intervention in both experimental and control groups. The setting was based on easy accessibility and availability of adequate sample and cooperation offered by staff and management.
Study samples were recruited from labour room of Amrita Institute of Medical Sciences during admission time, and the estimated sample size was 23 in each group; to ensure better generalizability, a sample size of 25 each in group was selected. The total sample was 50. Selection criteria for samples are: 1) primigravida mothers in first stage of normal labour admitted in labour room; 2) primigravida mothers with cervical dilation of 3–5 cm checked by doctors; 3) primigravida mothers at or above 37 weeks of gestation; and 4) primigravida mothers between 20–35 years old. Exclusion criteria are primigravida mothers planned for lower segment caesarean section (LSCS), high-risk pregnant mothers who were administered with pain medication within last two hours of selection, and women administered with epidural analgesia within two hours of selection.
Clinical parameters including blood pressure, heart rate, and respiration were assessed using a Mindray patient Monitor B20 (Mindray Medical International Co., Ltd., Nanshan, Shenzhen, China). Pain associated with labour was recorded on a visual analogue scale with numerical anchors from 0 (no pain) to 10 (maximal pain) that best described patients present pain. Uterine contraction was assessed by the investigator by placing the right hand over the fundal region to confirm contraction when the subject verbally reports the contraction. The duration of contraction was recorded in seconds and measured once during each study time phase. Pain and uterine contraction were assessed at baseline, and 20- and 40-minutes following reflexology treatment or resting comfortably.
The data collection began with selection of the samples based on inclusion criteria. The researcher explained the purpose, objectives, and advantages of the study, and obtained informed consent from the participants. Demographic data were collected from the subjects, and clinical data from clinical records.
Obtained approval from the Institutional Thesis Review Committee and the head of the Department of Obstetrical and Gynecology.
The investigator was certified in foot reflexology under an authorized trainer. And she was the only person who applied reflexology in this study.
The investigator instructed the subject to relax for 2 to 3 minutes and pre-test was done, which included visual analogue scale (VAS) for pain scoring and monitored uterine contractions. It is a unidimensional method of pain intensity, which has been widely used in different populations. The scale is most commonly anchored by “no pain” (score of 0) and “pain as bad as it could be” (score of 100) on the 10 cm line, and the respondent was asked to place a line at the point that represents their pain intensity. Foot reflexology intervention was performed to each subject about 20 minutes when the cervix is 4 cm to 5 cm dilated. The investigator stood on the foot end of the bed and advised the subject to select comfortable sitting or supine position. If she opted for sitting position, the investigator ensured that her back is well supported with pillows. A pillow was kept under the knee in the case of the supine position.
Foot reflexology was applied by giving massage and application of pressure on five different pressure points of the feet which corresponds to the uterus in the body: back of the big toe, back of the little toe, joining space between second and third toes, space around the ankle, and space behind the ankle. Three different techniques were used: direct pressure, press & release motion, clockwise/anticlockwise and sliding motion using thumb of the investigator on specific areas.
First, the investigator holds the right foot of the subject, with her dominant hand and the thumb placed on the back of the big toe and applied all three techniques (i.e., press & release motion, direct pressure, clockwise/anticlockwise & sliding motion) using the thumb for four minutes each. Each motion was repeated for 10 times on the areas. The procedure continued for other four areas with the same procedure sequentially. The left foot is then treated. The total intervention lasted 20 minutes.
Twenty minutes after completion of the intervention, the Post-test I was given which included VAS for pain scoring, while vital signs and uterine contractions continued to be monitored. The Post-test II was done again after 40 minutes of intervention.(13,14,15)
Twenty-five mothers in control group were given routine intranatal care in the setting which included assessment of maternal and fetal well-being, monitoring contractions, but no foot reflexology. Control group patients rested quietly for 20 minutes to serve as a time match for the reflexology group.
The collected data were analyzed based on the objectives including descriptive and inferential statistics using Statistical Package for Social Science (IBM SPSS 25, IBM, Armonk, NY) analysis. Demographic and baseline clinical variables are reported as frequency measures and were analyzed using chi-square test of independence. An independent t test was used to compare change score (pre-test to post-test) for clinical values between groups. A two-way repeated-measures ANOVA method was used to evaluate the effect of foot reflexology compared to control group across tine on pain and uterine contraction.(16) Post hoc analysis was conducted using an independent t test. A p value of .05 was used as the threshold for statistical significance.
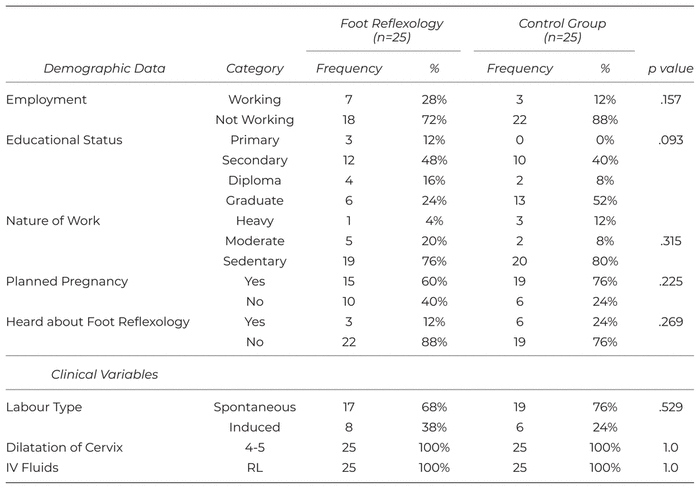
Distribution of demographic and clinical variables is given in detail in Table 1. In the study, the foot reflexology and control groups have similar demographic and clinical characteristics (p > .05). A majority of the women fell into the age group below 35 years and the mean age of the group was 24.16. Eighty-eight per cent of women in the foot reflexology group and 76% in the control group reported that they had no previous knowledge regarding foot reflexology in labour pain (p = .269). A majority of mothers (68%) had spontaneous labour, and all of them had dilatation between 4–5 cm upon study entry.
Table 1 Distribution of Primigravida Mothers Based on Demographic and Clinical Variables
Mean scores for clinical parameters in foot reflexology and control groups are presented in Table 2. No difference in pretest to post-test change scores (40 minutes after reflexology for experimental group and 40 minutes after the recruitment) for blood pressure, heart rate, or respiratory rate were found (p > .05).
Table 2 Clinical Parameters Before and After Intervention (mean ± SD)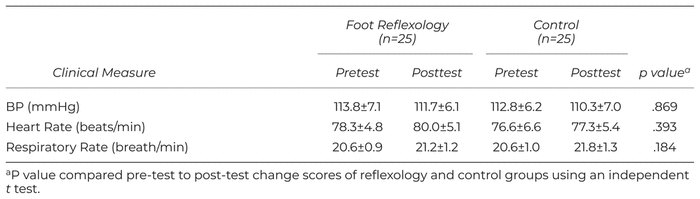
This section deals with comparison of the labour pain score before and after application of foot reflexology. It is evident from Figure 1 that there is significant difference in pain score between experimental and control group across time (F(2,48)=25.359, p < .001); hence the null hypothesis that foot reflexology would not affect labour pain score was rejected. Mauchly’s Test of Sphericity indicated that the assumption of sphericity had been violated, χ2 =17.79, p < .001; therefore, statistics are presented using a Greenhouse–Geisser correction. Due to the significant group by time interaction for labour pain, post hoc tests were performed. Mean baseline labour pain for reflexology and control groups was 8.84 ± 0.85 and 8.48 ± 81.16, respectively (p = .217). However, labour pain for patients receiving foot reflexology decreased significantly at 20-minutes post-intervention (7.16 ± 0.94 vs. 8.44 ± 0.87, p < .001 [95%CI 0.764–1.796]) and remained at that level at the 40-minute post-intervention time point (7.12 ± 0.88 vs. 8.28 ± 0.94, p < .001 [(95%CI 0.643–1.677]) compared to the control group.
|
|
||
|
Figure 1 Labour pain across the study timeframe. Labour pain was recorded on using a visual analogue scale at baseline, and at 20- and 40-minutes following reflexology or resting quietly (control). The interaction effect showed a reduction in pain for patients receiving reflexology relative to control treatment, with pain significantly lower at both the 20- and 40-minute post intervention time points. |
||
Mean uterine contraction time for foot reflexology and control groups at pre-intervention, 20- and 40-minutes post-intervention are depicted in Table 3. Analysis with repeated measures ANOVA detected a significant change between the groups over time (F(2,48)= 15.787, p = .03) indicating the treatment and control groups responded differently. However, while both groups reported similar pre-intervention contraction duration time of 34.8 seconds, post hoc tests indicated that neither group differed from the other at any of the time points (p > .05). A main effect of time was detected indicating that, collectively, uterine duration of contraction increased across the study (F(2,48)=45.42, p < .001).
Table 3 Uterine Contraction Duration Across the Study Time Framea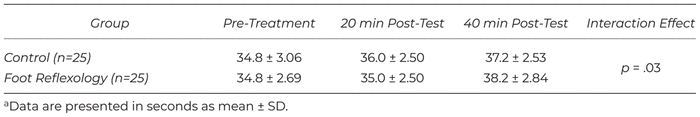
Figure 2 shows the mothers’ experiences following the foot reflexology treatment. Women who had undergone foot reflexology overwhelmingly responded that they felt like it reduced pain (74%) and was safe (82%), and they would recommend it to other primigravida mothers undergoing childbirth (81%).
|
|
||
|
Figure 2 Percent of patients responding in agreement following receipt of foot reflexology (n=25). |
||
The present study was conducted in the state of Kerala, South India, among fifty primigravida mothers in labour. Study results found that there was a significant reduction in pain in the experimental group that was greater than in the control group, while the clinical outcomes were not significant between groups. The difference in the level of labour pain was significant at 0.001 levels. There was a significant reduction in pain after the intervention in the experimental group, but no significant changes were found in uterine contractions after interventions.
Bering Liisberg(17) in a study on the effect of reflexology on the labour outcome found that, out of 68 pregnant women who chose reflexology, 61 (89.71%) expressed that reflexology was helpful in reducing the pain, 6 (8.82%) did not feel any effect, and 1 subject felt increased pain in response to reflexology. Another study done by Samuel and Ebenezer(18) reported that foot reflexology attenuates acute pain in human volunteers, and can increase both pain threshold and tolerance in human volunteers exposed to acute pain. These findings highlighted the possibility of using reflexology in the management of pain. Several reasons were proposed for the effect of reflexology, which are: touching skin can cause the release of endogenous endorphins of the body and reduces stress; therefore, with stress reduction, pain was consequently reduced and vice-versa. The second reason was that reflexology alleviated fatigue and anxiety. The third reason was applying pressure on hands or feet activated large diameter fibers to close the pain gate, thereby inhibited the transmission of pain. The findings of the present study were similar to the supporting study, so the result was interpreted as foot reflexology had a positive effect on labour pain reduction. The effect of intervention between groups was statistically highly significant and within groups was significant at the 0.05 level.
Various study results supported the present study findings on clinical parameters. A study done by Valiani et al.(19) to review the effect of reflexology on the pain and certain features and outcomes of labour on the primiparous women showed that systolic and diastolic blood pressure, and respiratory and pulse rates in the study subjects was lower than control groups.
Another study by McVicar et al.(20) about the effect of reflexology on the vital signs and other body organs demonstrated that reflexology reduced the stress of the volunteers. Measuring of cardiovascular parameters (pulse and blood pressure) showed that reflexology had been effective on reducing these parameters. The present study findings were more or less consistent in nature, with no significant difference found in both groups. This may be due to any number of factors such as individual differences, etc.
Firoozi et al.(21) in a study on the effect of reflexology on labour found that reflexology can facilitate labour through an increase in uterine contractions, and the reduction in pain and the need for intervention. In another study, which assessed the effect of reflexology on labour pain indicated that reflexology can facilitate labour progress through increased uterine contractions, and reduce the intensity of the pain and the need for augmentation. In the present study there was no significant difference found in the duration of uterine contraction between experimental and control group, but statistically significant difference was seen within groups. The findings are more or less consistent with the previous study findings by Firoozi and colleagues and may not be clinically significant.
The present study revealed that all of the primigravida mothers in experimental group had a positive experience with foot reflexology. All of them were comfortable with the procedure and more than half of the subjects were highly satisfied with foot reflexology given in labour. These findings were in agreement with Mirzai et al.(22) which assessed the effect of reflexology on the labour outcome and which found that 90% of study participants said that reflexology was helpful in reducing pain, while 9% did not feel any effect and 1 subject increased pain in response to reflexology. Therefore, the use of reflexology in maternity care appears to demonstrate high levels of maternal and staff satisfaction. The present study results were in agreement with the supporting study findings.
However, further research in this field must be continued in order to explore foot reflexology’s effectiveness in reducing pain, so that it can be implemented in normal vaginal deliveries. This study finding will be a simple and vital support for the forthcoming researches with its limitations.
Non-generalizability due to less sample size and non-randomization are the limitations of the study, therefore it could lead to potential bias. The study period was extended for one more month, since there were few last-minute dropouts due to relative indications and shifted for emergency LSCS.
Foot reflexology is an emerging trend in pain relief measures. In the future, midwifery practice that includes foot reflexology may lead to benefits for mothers in labour as it helps to convey caring, encouragement, support, and participation and comfort in nursing practice, and in reducing the need and frequency of administration of analgesics. It also helps to conserve the energy of the mother during first stage, which helps to put her own effort during second stage. It is hoped that foot reflexology could be made an integral part of pain relief in the management of labour pain. The findings of the study help to expand the scientific body of professional knowledge upon which further research can be conducted.
Sincere thanks to AIMS Management, all study participants and Labour Room staff. Special thanks to Dr. Albert Moraska PhD for his timely support, patience, and encouragement during the modification and re-submission of the manuscript. Heartfelt gratitude towards Dr. Joydeep Chaudari for the mentorship in modifying write-ups regarding intervention.
The authors declare there are no conflicts of interest.
1 Vijaya Prajula S. A Study to Assess the Effectiveness of Self Instructional Module on Knowledge Regarding Maternal Reflexology in Reducing Labour Pain and Labour Duration Among Staff Nurse Working in Selected Hospital at Bangalore[Thesis, Masterslevel]. Bangalore, India: Rajiv Gandi University of Health Sciences; 2011.
2 Kaur N, Saini P, Kaur R. A quasi-experimental study to assess the effect of foot reflexology on anxiety, labour pain and outcome of the labour among primipara women admitted in labour room at SGRD hospital, Vallah, Amritsar. Int J Health Sci Res. 2020;10(2):135–141.
3 Ramesh K, Krishnapriya M, Anupriya, Nair SC. An outlook to non-pharmacological and novel approaches to combat the uncurable firing disorder. Int J Pharm Sci Rev Res. 2016;40(1):55–61.
4 Pilewska-Kozak AB, Klaudia P, Celina Ł, Beata D, Grażyna S, Magdalena B. Non-pharmacological methods of pain relief in labor in the opinion of puerperae – a preliminary report. Ann Women’s Health. 2017;1(1):1005.
5 Childbirth [Def. 1] (n.d.). In Wikipedia, The Free Encyclopedia. Retrieved February 21, 2017, from: https://en.wikipedia.org/w/index.php?title=Childbirth&oldid=766125601
6 Albers L. Midwifery management of pain in labour. J Nurse – Midwifery. 1998;43(2):77–82.
7 Pillitteri A. Maternal & Child Health Nursing, 5th ed. Philadelphia: Lippincott Williams & Wilkins Company; 2007.
8 Palat G, Biji MS, Rajagopal MR. Pain management in cancer cervix. Indian J Palliative Care. 2005;11(2):64–73.
9 Weisenberg M, Caspi Z. Cultural and educational influences on pain of childbirth. J Pain Symptom Manage. 1989;4(1):13–19.
10 Prasertcharoensuk W, Thinkhamrop, J. Non-pharmacologic labour pain relief. J Med Assoc Thai. 2004;87 (Suppl 3):S203–S206.
11 Dolatian M, Hasanpour A, Montazeri SH, Heshmat R, Majd HA. The effect of reflexology on pain intensity and duration of labor on primiparas. Iran Red Crescent Med J. 2011;13(7):475–479
12 Davim RM, Torres GD, Dantas JD. Effectiveness of non-pharmacological strategies in relieving labor pain [in Portuguese]. Rev Esc Enferm USP. 2009;43(2):438–445.
13 Smith JS, Bindu C. Effect of foot reflexology on labour pain during the first stage of labour. Global J Res Analysis. 2015;4(12):136–137
14 Moghimi-Hanjani S, Mehdizadeh-Tourzani Z, Shoghi M. The effect of foot reflexology on anxiety, pain, and outcomes of the labor in primigravida women. Acta Med Iran. 2015;53(8):507–511
15 VassarStats: Website for Statistical Computation. Two-Factor ANOVA with Repeated Measures on One Factor. Available from: http://vassarstats.net/anova2corr.html
16 Liisberg BG. The effects of reflexology on labor outcome. Tidsskrift for Jordemodre. 1989;3:11–15.
17 Samuel CA, Ebenezer IS. The effects of reflexology on pain threshold and tolerance in an ice-pain experiment in healthy human subjects. Complement Ther Med. 2008;16:233–237.
18 Valiani M, Shiran E, Kianpour M, Hasanpour M. Reviewing the effect of reflexology on the pain and certain features and outcomes of the labor on the primiparous women. Indian J Nurs Midwifery Res. 2010;15(Suppl 1):302.
19 McVicar AJ, Greenwood CR, Fewell F, D’arcy V, Chandrasekharan S, Alldridge LC. Evaluation of anxiety, salivary cortisol and melatonin secretion following reflexology treatment: a pilot study in healthy individuals. Complement Ther Clin Pract. 2007;13(3):137–145.
20 Firoozi M. Application of Reflexology in midwifery. J Nurs Midwifery Mashhad University of Medical Sciences. 2003;9(2).
21 Mirzaei F, Kaviani M, Jafari P. Effect of foot reflexology on duration of labor and severity of first-stage labor pain. Iran J Obstet Gynecol Infert. 2010;13(1):27–32.
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 14, NUMBER 1, March 2021