Bryn Sumpton, BScN1, Amanda Baskwill, PhD, MSc, BEd, RMT2
1Sutherland-Chan Clinic Inc., Toronto, Ontario
2Faculty of Health Sciences and Wellness, Humber College, Toronto, Ontario
Background
Post-traumatic stress disorder (PTSD) is a common mental health diagnosis in Canada with prevalence estimated at about 2.4% in the general population. Previous studies have suggested massage therapy may be able to reduce the symptoms of PTSD. One of the symptoms commonly experienced is difficulty falling or staying asleep. No previously published massage therapy research has specifically assessed sleep symptoms of PTSD.
Objectives
The research question was, “For individuals who have PTSD as a result of experiencing traumatic events, does MT have an effect on sleep quality?”
Methods
A prospective series of case reports describing 10-week MT treatment plans provided by Registered Massage Therapists at Sutherland-Chan Clinic’s Belleville location. Three individuals with PTSD were recruited using promotional posters in the community. Treatment focused on improving sleep quality and followed a pragmatic treatment protocol using light to moderate pressure. Outcomes were measured using a sleep diary, Pittsburgh Sleep Quality Index, and the Leeds Sleep Evaluation Questionnaire.
Results
Data collected at baseline and throughout the series showed inconsistent improvement and worsening of symptoms amongst participants. Treatment was well tolerated and attended. No harmful incidents were noted.
Conclusion
For these participants, MT did not predictably impact sleep quality. It is possible, as the underlying cause of poor sleep quality was unlikely resolved, the participants did not have a significant change in their sleep quality. This differs from findings of previous studies in which MT improved sleep for patients with poor sleep quality due to exposure to traumatic events. There is need for further understanding of how MT affects sleep.
KEYWORDS: massage therapy, posttraumatic stress disorder, PTSD, sleep, sleep quality, symptom management, case study
Post-traumatic stress disorder (PTSD) is a common mental health diagnosis in Canada, with prevalence estimated at about 2.4% in the general population.(1) PTSD is defined as when an individual recurrently re-experiences a traumatic event leading to persistent symptoms of increased arousal that cause clinically significant distress or impairment for a month or longer.(2) One commonly experienced symptom is difficulty falling or staying asleep.(3) Patients diagnosed with PTSD often have comorbid conditions, such as sleep apnea or pre-existing sleep conditions, that further contribute to their poor sleep quality. While the exact economic cost of PTSD in Canada is unknown, U.S.-based studies suggest anxiety disorders, including PTSD, account for $65 billion in both direct and indirect costs.(4) Further, more than half those costs are believed to be associated with ineffectual or repeated use of health care services.(5)
PTSD is associated with exposure to a traumatic event, including those related to violence, danger, or injury experienced by military personnel or first responders.(2,6) In the last 15 years, the Canadian Military has deployed troops in a number of war zones. Since the commencement of combat operations in Afghanistan in 2002, the rate of post-traumatic stress disorder (PTSD) in the Canadian Forces Mental Health Survey has doubled from 2.8% in 2002 to 5.3% in 2013.(7) Additionally, there has been an increasing awareness of the high prevalence of PTSD among first responders.(8) In Canada, the rates of PTSD for first responders has been estimated at 12%–23%.(8)
Treatment for PTSD often includes psychotherapy, medications, or both.(9) These are designed to manage symptoms and reduce, or stop, recurrent re-experiencing of the traumatic event. Medications for PTSD regulate the function of the hypothalamicpituitary-adrenal axis, controlling the release of cortisol; alternatively, medications are selective serotonin reuptake inhibitors, increasing the availability of serotonin.
Patients with PTSD commonly also seek complementary and alternative medicine (CAM) treatment options. Recently, 95% of US veterans with PTSD reported incorporating at least one form of CAM in their treatment programs.(10) In a recent survey of US veterans returning from deployment in Iraq and Afghanistan, over 40% reported using CAM in the last 12 months, with massage therapy as the most common CAM treatment modality at 21%.(11)
Studies suggest massage therapy (MT) may be able to reduce some symptoms of PTSD such as irritability, anxiety, depression, and tension.(12,13) Massage therapy for sleep symptoms related to PTSD have not been studied in this population.(14) While the mechanism for these effects is not clear, MT has been linked to changes in neurotransmitter levels, such as cortisol, serotonin, and dopamine, which control psychological arousal.(15) Additionally, MT improves sleep in certain patient subpopulations.(16–18) Therefore, it is possible that MT may be an effective treatment for sleep-related symptoms of PTSD. The research question was, “For individuals who have PTSD as a result of experiencing traumatic events, does MT have an effect on sleep quality?”
To investigate the research question, a prospective case series was undertaken. Participants received 10-weeks of massage therapy treatment, and measures were used to assess sleep quality. Research ethics approval was granted by Humber College’s Research Ethics Board. Consent for the study was obtained prior to the first treatment and ongoing consent for treatment was given throughout.
Over a three-month period, new patients presenting with a diagnosis of PTSD were screened for eligibility. The inclusion criteria required that participants were a member of the Canadian military, a Canadian military veteran, a first responder, or retired first responder; were currently experiencing decreased sleep quality; were receiving treatment from a primary health care provider for PTSD; and were willing to complete a 10-week MT treatment plan. Exclusion criteria included having conditions contraindicated for MT treatment, a diagnosis of PTSD within the last six months, or an inability to provide consent.
One woman and two men were enrolled. Their ages ranged from 38 to 59 (mean of 50) years. One participant was a first responder and two were veterans of the Canadian military. They had been diagnosed with PTSD, and the time since diagnosis ranged from four to 19 years (mean of 10). All three had symptoms of disturbed sleep including difficulty falling asleep, frequent waking, nightmares or disturbing dreams, and also had difficulty returning to sleep after waking. Additionally, all there were receiving concurrent treatment for PTSD from other health care providers and where taking medications for the symptoms of PTSD.
Participant 1, female, 59 years old, had a previous hand injury with chronic pain, a history of colitis, and presented with back and neck pain. Participant 2, male, 53 years old, had previous abdominal surgery due to cancer, high blood pressure, and presented with back and leg pain. He had been diagnosed with sleep apnea and used a continuous positive airway pressure (CPAP) machine while sleeping. Participant 3, male, 38 years old, had previous abdominal surgery for an umbilical hernia, had nerve damage and compartment syndrome in both legs, patella femoral disorder in both knees, a history of migraines and concussion, and presented with back and arm pain.
Three therapists provided treatment at the Belleville, Ontario, clinic. All were female, had completed a 2-year MT program in Ontario within the last six years, and were RMTs in good standing with the College of Massage Therapists of Ontario (CMTO). The therapists had between one and five years of clinical experience. None had previous experiences treating patients with PTSD. Clinical support for treatment was provided by the clinic owner; an RMT with 18 years of clinical experience and previous experience working with patients with PTSD. All therapists were provided a study orientation sheet which included information on PTSD and its symptoms, an outline of the study’s methods, aims, and measurement tools, as well as information on additional treatment resources in the community.
An information session was provided by one author and an RMT experienced in the treatment of the sleep symptoms of PTSD prior to commencement of treatment. No PTSD-specific training was provided beyond the resources indicated and the information session. Each participant was treated by the same therapist for all treatments except for Participant 2, who was treated by two therapists.
Sixty-minute MT sessions were provided once a week for 10-weeks. A pragmatic MT treatment protocol was followed, within the scope of practice for Ontario,(19) which allowed therapists to choose from a selection of massage therapy techniques that best suited the participant and individual presentation. Therapists were instructed to focus on improving sleep, include the whole body, use light to moderate pressure, and to not use muscle stripping, trigger point release, fascial release, or other deep pressure techniques.(20) Treatment occurred in a professional multidisciplinary clinic in Belleville, Ontario.
Participants completed the Pittsburgh Sleep Quality Indicator (PSQI), the Leeds Sleep Evaluation Questionnaire (LSEQ), and kept a daily sleep diary. The PSQI is a 10-item, self-report questionnaire designed to capture sleep quality and disturbances over the previous month.(21) The PSQI was completed by patients prior to their first and last treatment. Permission was granted by Anne Germain, PhD, Associate Professor of Psychiatry and Psychology at the University of Pittsburgh, School of Medicine.
The LSEQ is a self-report questionnaire consisting of ten 100 mm visual analog scales.(22) Each line represents a stage of sleep (i.e., getting to sleep, trouble upon waking, etc.). The patient marks a line they feel best represents their experience.(23) The LESQ was completed each week prior to treatment. The daily sleep diary noted the time participants fell asleep, the time they woke, and the number of times they awoke. It was completed after the first treatment until the final treatment, recording each day’s sleep cycle.
The PSQI was analyzed using the instructions provided (available from http://www.psychiatry.pitt.edu/node/8240). The resulting score was categorized as ‘good sleep quality’ or ‘poor sleep quality’. The LESQ was evaluated by measuring the length from the starting end to the line made by the participant. This was measured by both research assistants and averaged to produce 10 scores for each week. A global score was calculated by adding all 10 scores together. The percent change was calculated for each category and global score using (Week 10 - Week 1)/Week 1. The average number of hours slept and times awake were calculated from sleep diary data.
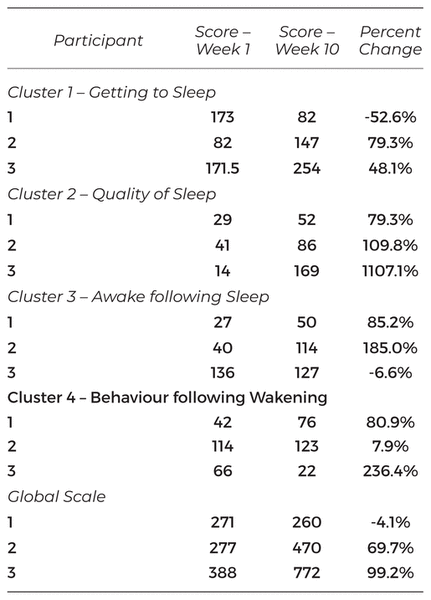
All three participants completed the treatment period. There were no harmful incidents reported by participants. Treatment was well tolerated, and all participants adhered to the treatment with the exception of one missed appointment provided the following day. The results of the measures are described by participant below and presented in Table 1.
Table 1 Results of Leeds Sleep Evaluation Questionnaire (LSEQ)
The PSQI indicated the participant began and ended with poor sleep quality (pre = 17; post = 15). The results of the LSEQ are presented by cluster and then global score. For Participant 1, there was a 52.6% worsening in the Getting to Sleep (GTS) cluster. Quality of Sleep (QOS) improved by 79.3%. The clusters of Awake Following Sleep (AFS) and Behaviour Following Wakening (BFW) both improved by 85.1% and 80.1%, respectively. The global score for the LESQ worsened by 4.1%. Despite this worsening, Participant 1 continued to receive treatment following the study. The results of the sleep diary indicate Participant 1 attempted to sleep an average of 6.6 hours a night. Participant 1 awoke, on average, three times a night. In addition, Participant 1 noted that, in an effort to accurately complete the sleep diary, she would repeatedly check her clock to note the time.
For Participant 2, the PSQI showed poor sleep quality at the beginning and end of the study (pre = 13; post = 15). The LSEQ showed a 79.3% improvement for the GTS cluster, a 109.8% improvement for the QOS cluster, a 185.0% improvement for the AFS cluster, and a 7.9% increase in the BFW cluster. Participant 2 reported having difficulty falling asleep after waking due to memories of combat or nightmares, although he noted this improved following a visit with a psychiatrist. The global score for the LSEQ improved by 69.7%. The sleep diary showed Participant 2 attempted to sleep, on average, 7.5 hours a night and woke three times. However, he reported that sometimes the amount of time he was awake was sometimes more than the time he was asleep. Participant 2 reported he noticed his mood had improved.
The PSQI indicated the participant began and ended with poor sleep quality (pre = 9; post = 8). For Participant 3, there was a 48.1% improvement in Getting to Sleep. Quality of Sleep improved by 1107.1%. The participant noted a worsening in Awake Following Sleep (AFS) by 6.6%. Improvement noted in Behaviour Following Wakening of 236.4%. The global score improved by 99.2%. The results of the sleep diary indicate Participant 3 attempted to sleep an average of 7.2 hours and awoke 2 times a night. Participant 3 started using baclofen and amitriptyline in Weeks 5 and 6, respectively, and discontinued their use in Week 7 (baclofen) and Week 9 (amitriptyline).
This case series provides preliminary evidence that massage therapy is a well-tolerated treatment for individuals with PTSD. There was concern participants may be challenged to attend regularly scheduled treatment, as this population sometimes has issues with absenteeism.(24,25) However, each participant attended all appointments and no safety incidents were reported. This suggests massage therapy was well tolerated by participants and may have a role in the treatment of PTSD-related sleep symptoms.
This case series also illuminated the need to reconsider the choice of outcome measures. All participants mentioned to their RMT they felt they were sleeping better, which corresponds to the results of the QOS cluster of the LSEQ. While some improvement was seen within the LSEQ for each participant, the area and amount of improvement varied. If the sleep diary data were reviewed alone, participants would seem to have, on average, an adequate number of hours of sleep with few awakenings. However, all participants began, and ended, with poor sleep quality. The results captured in the outcome measures did not match patients’ communicated experience. Furthermore, Participant 2 reported that he noticed his mood had improved, which was an outcome not measured. Participant 1 continue to receive treatment following the study despite experiencing a worsening of LSEQ global score, suggesting she found some benefit that was not captured.
Using the sleep diary, the number of hours slept is calculated by the difference between when the participant awoke and when they went to bed.(26) However, what is actually used is the time the participant ‘got up’ the next morning and the time they went to bed. For example, if the participant went to bed at 9:00 p.m. but could not fall asleep until 11:00 p.m., this is not noted, which may be why the results suggest participants got an adequate number of hours of sleep per night.
Further, the number of awakenings relies on the participant recording the number of awakenings they remember or tracking their awakenings while they try to get back to sleep. Participant 1 noted she found herself watching the clock at times so she could accurately complete the sleep diary. Participant 2 reported his sleep diary did not accurately record his sleep quality, as the amount of time he was awake was sometimes more than the time he was asleep.
In future, wearable technology to evaluate sleep, in addition to patient self-report measures, should be explored. A study conducted on university students concluded that Fitbit© (Fitbit Inc., San Francisco, CA) was a “valid, reliable, and alternative device to use for sleep evaluation”.(27) As technology continues to improve and become more accessible, wearable devices should be considered as a way to non-invasively monitor sleep.(28)
Poor sleep quality persisted for participants, as measured by the PSQI. Review of the ongoing notes and participant health histories led to the hypothesis that MT had little impact as it did not remove the cause. Participant 2 reported having difficulty falling asleep after waking due to memories of combat or nightmares. He reported improved sleep following a visit with a psychiatrist, which may have better addressed the cause of his sleep disturbance.
Medication may have also impacted the results. Participant 3 started using baclofen and amitriptyline in Weeks 5 and 6, respectively. In Week 7, the patient stopped taking baclofen and, in Week 9, stopped taking amitriptyline. Both amitriptyline and baclofen have potential side effects of troubled sleep, nightmares, and depression or anxiety.(29,30) The use or disuse of these over a short period may have had an impact on sleep quality.
In clinical practice, the results illustrate a need to consider sleep evaluation. A sleep diary may not be useful for either patient or practitioner. Exploring technology to more accurately discuss patterns of sleep quality may be useful. The LSEQ would be worthwhile for practitioners provided they focus on any changes seen and reported by the patient, rather than the actual number, to gauge patients’ progress.
In entry-to-practice education programs, students should be exposed to sleep and its role in health. Further, students should monitor sleep and use the results of common sleep assessment tools. Both entry-to-practice and continuing education should explore mental health conditions, such as PTSD, so students and RMTs understand their role within the larger health care team. Programs, such as Mental Health First Aid,(31) should be offered to both students and RMTs, so they thoughtfully support patients with mental health issues.
Researchers should consider how to measure the most appropriate dosage of MT needed to achieve outcomes related to sleep. The appropriate dosage of MT for sleep outcomes is unknown, and the dosage used in this study may not be realistic in practice. Changes in chronicity, such as a shorter period between diagnosis and intervention, could be explored as it relates to dosage and outcome. Further, future studies should explore other tools to measure sleep quality. The PSQI has an extension for PTSD that might improve how participants’ experiences are recorded,(32) and wearable technology may improve the assessment of sleep.
This study adds to the growing body of research for MT. The ecological validity is high due to the use of case study design. The participants, while not representative of the entire population of individuals with PTSD, illustrate patients’ complex health presentations. The MT intervention was pragmatic, and practitioners provided techniques based on the patient’s presentation, with few limitations. The lack of experience treating individuals with PTSD of the practitioners may be a limitation, although the training that was provided attempted to reduce this. Caution should be taken when broadly applying these results.
The participants did not experience a demonstrable change in sleep quality following MT treatment. Practitioners should consider how they are measuring sleep quality and consider using tools, such as the Leeds Sleep Evaluation Questionnaire, as a way to discuss their patients’ experiences. As there are multiple factors that impact sleep quality, RMTs should ensure their patients are receiving treatment as part of a larger health care team and connect with the other practitioners treating the individual.
The benefit of case study design and, subsequently, case series design, is that it is the closest to the actual setting in which MT is practiced. However, this also limits the generalizability. Future research should explore dosage of MT treatment, the use of wearable technology in the measurement of sleep, both in practice and in research settings, and multidimensional tools to measure sleep quality.
We would like to thank the registered massage therapists who participated by providing treatment, and Trish Dryden for her mentorship regarding massage therapy care for individuals with PTSD. We would also like to thank our research assistants Sarah Wadhwa and Natalie Rinaldi. Funding and support from Humber College, Sutherland-Chan Clinics, and the Registered Massage Therapists’ Association of Ontario made this study possible.
The authors declare there are no conflicts of interest.
1 Van Ameringen M, Mancini C, Patterson B, et al. Post-traumatic stress disorder in Canada. CNS Neurosci Ther. 2008;14(3):171–181.

2 American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed. Washington, DC: APA; 2013.
3 Koffel E, Khawaja IS, Germain A. Sleep disturbances in posttraumatic stress disorder: updated review and implications for treatment. Psychiatric Ann. 2016;46(3):173–176.
4 DuPont RL, DuPont CM, Rice DR. The economic costs of anxiety disorders. In: Stein DJ, Hollander E, Rothbaum BO, editors. Textbook for Anxiety Disorders, 2nd edition. Washington, DC: American Psychiatric Assoc. Pub.; 2002. p. 475–483.
5 Greenberg PE, Sisitsky T, Kessler RC, et al. The economic burden of anxiety disorders in the 1990s. J Clin Psychiatry. 1999;60(7):427–435.
6 Young A. Reasons and causes for post-traumatic stress disorder. Transcultural Psychiatric Res Rev. 1995;32(3):287–298.
7 Pearson C, Zamorski M, Janz T. Mental health of the Canadian Armed Forces. Ottawa, ON: Statistics Canada; 2014.
8 Wilson JP. PTSD and complex PTSD: Symptoms, syndromes, and diagnoses. In: Wilson JP, Keane TM, editors. Assessing Psychological Trauma and PTSD, 2nd ed. New York NY: Guilford Prss; 2004. p. 7–44.
9 National Institute of Mental Health. Post-traumatic stress disorder. Bethesda, MD: NIMH; 2016. Available from: https://www.nimh.nih.gov/health/topics/post-traumatic-stress-disorder-ptsd/index.shtml
10 Libby DJ, Pilver CE, Desai R. Complementary and alternative medicine in VA specialized PTSD treatment programs. Psychiatric Services. 2012;63(11):1134–1136.
11 Park CL, Finkelstein-Fox L, Barnes DM, et al. CAM use in recently-returned OEF/OIF/OND US veterans: demographic and psychosocial predictors. Complement Ther Med. 2016;28:50–56.

12 Collinge W, Kahn J, Soltysik R. Promoting reintegration of National Guard veterans and their partners using a self-directed program of integrative therapies: a pilot study. Military Med. 2012;177(12): 1477–1485.
13 Field T, Seligman S, Scafidi F, et al. Alleviating posttraumatic stress in children following Hurricane Andrew. J Appl Dev Psychol. 1996;17(1):37–50.
14 Mckenna Longacre MM, Silver-Highfield E, Lama P, et al. Complementary and alternative medicine in the treatment of refugees and survivors of torture: a review and proposal for action. Torture. 2012;22(1):38–57.
15 Field T, Hernandez-Reif M, Diego M, et al. Cortisol decreases and serotonin and dopamine increase following massage therapy. Int J Neurosci. 2005;115(10):1397–1413.
16 Kashani F, Kashani P. The effect of massage therapy on quality of sleep in breast cancer patients. Iran J Nurs Midwifery Res. 2014;19(2):113–118.

17 Hill R, Baskwill A. Positive effects of massage therapy on a patient with narcolepsy. Int J Ther Massage Bodywork. 2013;6(2):24–28.

18 Oliveira DS, Hachul H, Goto V, et al. Effect of therapeutic massage on insomnia and climacteric symptoms in postmenopausal women. Climacteric. 2012;15(1):21–29.
19 Government of Ontario. Massage Therapy Act, 1991. Ottawa, ON: Queen’s Press; 1991.
20 Andrade CK. Outcome-Based Massage: Putting Evidence Into Practice, 3rd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2014.
21 Buysse DJ, Reynolds CF, Monk TH, et al. The Pittsburgh Sleep Quality Index (PSQI): A new instrument for psychiatric practice and research. Psychiatry Res. 1989;28(2):193–213.
22 Parrott, AC. The Leeds Sleep Evaluation Questionnaire [online document]. 1980. Available from: https://www.theseus.fi/bitstream/handle/10024/36268/leeds-sleep-evaluation-questionnaire.pdf?sequence=4&isAllowed=y
23 Parrott AC, Hindmarch I. Factor analysis of a sleep evaluation questionnaire. Psychological Med. 1978;8(2):325–329.
24 Hoge CW, Terhakopian A, Castro CA, et al. Association of posttraumatic stress disorder with somatic symptoms, health care visits, and absenteeism among Iraq war veterans. Am J Psychiatry. 2007;164(1):150–153.
25 Belleville G, Marchand A, St-Hilaire MH, et al. PTSD and depression following armed robbery: patterns of appearance and impact on absenteeism and use of health care services. J Trauma Stress. 2012;25(4):465–458.
26 Carney CE, Buysse DJ, Ancoli-Israel S, et al. The consensus sleep diary: standardizing prospective sleep self-monitoring. Sleep. 2012;35(2):287–302.

27 Lee PH, Suen LK. The convergent validity of Actiwatch 2 and ActiGraph Link accelerometers in measuring total sleeping period, wake after sleep onset, and sleep efficiency in free-living condition. Sleep Breath. 2017;21(1):209–215.
28 Shih PC, Han K, Poole ES, et al. Use and adoption challenges of aearable activity trackers. iConference 2015 Proceedings. Urbana-Champaign, IL: IDEALS University of Illinois; 2015.
29 Rexall. Elavil. What side effects are possible with this medication? Toronto, ON: Rexall; 2017. Available from: http://www.rexall.ca/articles/view/591/Elavil#adverseeffects_title
30 Rexall. Apo-Baclofen. What side effects are possible with this medication? Toronto, ON: Rexall; 2017. Available from: http://www.rexall.ca/articles/view/856/Apo-Baclofen#adverseeffects_title
31 Mental Health Commission of Canada. Mental health first aid. Ottawa, ON: The Commission; 2017. Available from: http://www.mentalhealth-firstaid.ca/en
32 Germain A, Hall M, Krakow B, et al. A brief sleep scale for posttraumatic stress disorder: Pittsburgh Sleep Quality Index Addendum for PTSD. J Anxiety Disord. 2005;19(2):233–244.
Corresponding author: Bryn Sumpton, BScN, Sutherland-Chan Clinic Inc.—Head Office, 738 Spadina Ave., Suite 200, Toronto, ON, M5S 2J8, E-mail:bryn@sc-clinic.com
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 12, NUMBER 4, December 2019