Yolanda Casciaro, BSc, RMT
Massage Therapy, MacEwan University, Edmonton, AB, Canada.Introduction
Parkinson’s disease (PD) is a complex neurological disorder. The disease is progressive and, in time, results in severe disability. Many patients turn to massage in an attempt to alleviate symptoms of pain and rigidity, though the effects of massage with respect to PD are not well studied. This case adds one more instance in which massage therapy has provided temporary respite from resting tremor, one unrelenting symptom of PD.
Objective
To determine if massage therapy can produce favorable outcomes with respect to the severity of rigidity and tremor in a patient with PD.
Case Presentation
A 63-year-old female patient with idiopathic, long-standing, Hoehn-Yahr Stage 4 PD was treated with massage therapy five times over the course of six weeks. A SPES/SCOPA Motor Impairments rating scale was used to measure rigidity and tremor pre- and post-treatment, to gauge treatment effectiveness. The massage treatments consisted of deep longitudinal stroking, muscle squeezing techniques, passive range of motion movements, and general relaxation techniques to encourage a soothing environment while promoting a decrease in muscular tone and hyperactivity. Massage therapy administration was by a student near the end of her two-year diploma.
Results
The results obtained indicated that massage therapy treatment had a positive effect on reducing resting and postural tremor in a patient with long-standing PD. The treatment was also effective in temporarily reducing rigidity during treatment, but did not produce a lasting effect.
Conclusion
Further study is required; however, the results of this case were consistent with the limited research available on the subject of massage therapy and Parkinson’s disease, in that positive change with respect to tremor—and to a lesser degree, rigidity—were achieved with focused, intentional treatment.
KEYWORDS: neurologic disorders, Parkinsonism, tremor, muscle rigidity
Parkinson’s disease (PD) is a well-known, if not well-understood, disorder. The British physician, James Parkinson, first described the manifestation of symptoms as a shaking palsy in 1817.(1) After nearly 200 years, Dr. Parkinson’s clinical documentation of the disorder is still accurate today, with only a few exceptions.(2)
While the chemical interactions in the brain that result in the symptoms PD have been deciphered, the root cause is still unknown. These symptoms are well-documented and consist of both a primary category of manifestations and a subsequent secondary category. Nonspecific achiness and fatigue, resting tremors, bradykinesia, rigidity and poor postural reflexes comprise the primary category; while shuffling gait, difficulty with speech and eating, micrographia, sleep disorders, depression, and mental degeneration comprise the secondary.(1) The three most recognizable and debilitating symptoms of PD include rigidity, which is described as a resistance to motion; resting tremor, which slows or stops with intentional movement, sleep, and relaxation; and bradykinesia, which makes ambulation difficult and requires extra time, concentration, and effort for initiation and cessation of activity.(2)
According to the Parkinson Society Canada website, there are approximately 100,000 Canadians living with PD, with an incidence rate of 10 to 20 new cases per 100,000 people each year.(3) Both the incidence and prevalence of PD rise with age, with prevalence rates approaching 1 in 50 in a population group over the age of 80.(4) All ethnic groups are affected, with men being 1.5 times more likely to develop PD than women.(4) In Canada, 85% of PD cases occur in those over the age of 65, a demographic group that is expected to increase from nearly one in ten Canadians to nearly one in four over the next 30 years.(3)
Complications abound in the management of PD, with many options and combinations of medications available to treat the symptoms of the disease; all of which become ineffective as time wears on.(1) Many surgical options for treatment and management of symptoms are available once the patient has become unresponsive to pharmacotherapy; however, these procedures tend to be controversial, risky, and expensive.(5)
Today, the majority of PD cases are effectively treated with a combination of medications, including the drug levodopa; however, the degenerative effects of PD will still eventually lead to the progressive deterioration of neuromuscular control affecting bodily functions and activities of daily living.(6) A study reviewing the research base states that, while many PD patients receive regular massage to alleviate PD symptoms, the lack of high-quality studies leaves the efficacy of the intervention for improvement of any measure other than relaxation, sleep, or emotional health unknown.(6)
A number of recent global studies have been conducted in an attempt to determine complementary and alternative medicine (CAM) usage by PD patients, with a worldwide usage rate varying between 26% to 76%, and usage of massage therapy (MT) in particular varying between 7% and 40%.(7) The patients generally tending to turn towards CAM treatments in addition to the medical and pharmaceutical care they are receiving are those who have had a younger onset or longer duration of disease, those on higher doses of levodopa, and those with more severe motor symptoms.(7)
Since massage therapy is a popular choice of CAM for PD patients, it is surprising that so few studies measuring the efficacy of massage have been conducted. A search of the literature resulted in only six studies that investigated the effect of various forms of therapeutic massage with respect to PD patients. Of the studies retrieved, one investigated traditional Japanese massage (TJM), one investigated Neuromuscular Therapy (NMT), and one investigated the Alexander Technique (AT). The remainder investigated nonspecific generalized “massage” (MT). Please refer to Table 1 Summary of the Literature for a detailed summary of each.
Table 1 Summary of the Literature
While informative, the three studies focused on a specific style of massage (TJM, NMT, and AT) are not directly applicable to this case. The key outcome in each case was that the treatments, tailored to each patient’s needs, showed marked improvements in outcome measures. Comparable treatment techniques and approaches have been extrapolated and incorporated in the treatment plan for this case. The other three studies investigating generalized massage included MT as a secondary tool for control or enhancement of other main outcome measures. The massage techniques were applied in a more generalized fashion and are not directly applicable to the administration of clinical massage therapy for PD patients. Applicable outcomes have again been extrapolated and incorporated in the treatment plan for this case.
The objective of this prospective case report was to describe the MT treatment and outcomes for a patient with idiopathic PD who uses MT as an adjunct therapy to help cope with some of the PD symptoms she experiences. When reviewing the literature with the aim of formulating a treatment plan, it became evident that a significant gap exists in the knowledge base with respect to therapeutic massage for patients with PD. Consistent themes appear to indicate that treatments should be conducted to maximize the patient’s ability to relax and should consist of Swedish massage techniques, applied with firm pressure and at frequent intervals. This case report serves to illustrate an example of the application of intentional, focused massage therapy in accordance with the best available knowledge to date.
A 63-year-old female patient presented to the clinic with a diagnosis of idiopathic PD established 14 years prior. The patient regularly sees a neurologist once per week and a PD specialist once per year. Her left side is more greatly affected with rigidity and resting tremor from the neck down, and her right facial muscles have more recently become involved with spasm and loss of voluntary control. On the right side, from the neck down, a resting tremor is also observable, though the rigidity on the right is much less than that on the left. This patient has many functional limitations and uses a walker to assist with ambulation. She has a stooped posture, festinating gait with circumduction of the left leg, and has fallen several times. A home care nurse visits two times per day to assist with activities of daily living (ADL), as the patient has difficulty with dressing, grooming, cooking, and cannot function at all upon waking for approximately 30 minutes, until her morning dose of medication takes effect. Her speech is affected with some slurring and stuttering, though she is still able to communicate. While sleeping, the patient stacks two pillows under her head at night in an attempt to avoid breathing problems. The patient also suffers from fluctuations in blood pressure, headaches, nausea, and almost constant constipation. Her home care provider administers rectal enemas and both the patient and her home care provider perform regular abdominal massages to help encourage bowel movements. The patient only experiences success in moving her bowels approximately weekly.
In order to manage the symptom picture described above, the patient has been prescribed Sinemet (a levodopa medication) to manage her PD, as well as a number of secondary medications to manage the resultant side effects. Medications are taken four times per day, and all of this patient’s symptoms worsen in the evening as the effects of her medications wear off.
Based on the Hoehn-Yahr Scale descriptions, and in consideration of the symptom picture described above, it is likely that this patient is at Stage 4: “Fully developed, severely disabling disease; the patient is still able to walk and stand unassisted but is markedly incapacitated.”(8)
A scanning examination as described in Magee(9) to assess the patient’s orthopedic impairments was completed on the first visit to the clinic. A greatly reduced cervical range of motion, with pain on left side flexion, forward flexion and extension, and tenderness on palpation at the C6 spinous process and left transverse process, was noted. Weakness in the C1, C2, right C3, C5, left C6, left C7, and left T1 myotomes was observed. All cervical isometrics except extension were weak (Grade 3+ as described in Magee(9) (Muscle Test Grading)), with pain experienced when resisting left and right rotation. All upper extremity reflexes presented with a Grade 4 (clonus) response, as described by Magee (Deep Tendon Reflex Grading). Left deviation of the jaw was not possible, and when asked to protrude her tongue, the tongue deviated to the right. All scapular and glenohumeral motions were limited in range, especially on the left side where the patient felt pain in the musculature of the infraspinous fossa of the scapula. Superficial tactile and temperature sensation testing was found to be normal.
The patient would like to have some relief from the rigidity and resting tremors she experiences, and the resultant pain in her back, neck, head, left upper thoracic and shoulder area, left hand and foot, and occasionally left leg.
After the examination visit, a series of five MT treatments were planned for weekly administration in 60-minute sessions over the course of five weeks. On the sixth week, a follow-up examination was completed, with a significantly shortened MT treatment administered on that day. No SPES/SCOPA assessment measures as described below were collected on the sixth visit.
In a review of a number of Parkinson’s disease rating scales, including the Short Parkinson’s Evaluation Scale (SPES)/SCales for Outcomes in Parkinson’s disease (SCOPA), conducted by Marinus et al.,(10) it was found that the reproducibility of clinical assessments of patients with PD was high and that the scales were valid for use in both research and clinical practice applications. The Motor Impairments (MI) section of the rating scale was deemed to be most applicable for measurement of potentially achievable outcomes as a result of a massage therapy treatment plan. Other sections of the rating scale have to do with ambulation, self-care, swallowing, and speech. It was decided that none of these major disabilities were likely to be affected in this case. According to the Landis & Koch “strength of agreement” classification, the inter-rater reliability of the Motor Impairments (MI) section of the SPES/SCOPA ranges from fair (0.21–0.40) to substantial (0.61–0.80) when assessing resting tremor, postural tremor, and rigidity, with rigidity being the least reproducible measure and resting tremor being the most reproducible.(10) The low inter-rater reliability scores in the MI section of the SPES/SCOPA can be partially explained by potential differences in the patient’s state at time of evaluation by different raters, as the inter-rater reliability of assessments of video recordings of patients rises to substantial (0.61–0.80) or almost perfect (0.81–1.0). (10) The MI section of the SPES/SCOPA was therefore determined to be a reliable rating scale and was chosen as a before- and after-assessment tool for the effectiveness of the MT treatment with respect to the patient’s rigidity and tremor (refer to Appendix A).
Therapeutic massage treatments were administered by a student in her fifth semester of a six-semester, 2,200-hour massage therapy diploma program at MacEwan University in Edmonton, Alberta, Canada. The patient attended the student clinic at the university to receive treatment.
Several contraindication considerations informed treatment plan development. Specifically, painful or prolonged aggressive techniques should be avoided so that the patient can maintain a feeling of rest and relaxation.(11) Extremes of temperature should be avoided if the patient is experiencing hypertension at the time of treatment.(12) The patient’s blood pressure (BP) was taken at the start of every treatment to determine if a heat application would be appropriate for that treatment. The patient may also experience hypotension, as blood pressure fluctuations are common with PD medications, and may experience dizziness or require assistance with rising after the treatment.(2)
The treatment plan developed for this patient is described in Table 2. It should be noted that the plan was not followed verbatim at every treatment; modifications were made as necessary, depending on the condition in which the patient presented to the clinic. Informed consent was obtained prior to the start of each session.
First and foremost, the goal of the treatment is to decrease activity in the sympathetic nervous system, as generalized patient relaxation alone can help to reduce rigidity.(2) The treatment was performed working proximally to distally with slow, deep continuous strokes, coupled with slow, smooth passive range of motion (PROM) exercises and stretching; frictions at origins and insertions of the spastic muscles for maximal reduction in spasticity were also included.(11) These recommendations are consistent with the findings in the literature review described above.
Skin rolling is effective in softening and lengthening tissue(11) and was applied in this case, as the patient’s tissues hold in rigid form most of the time and may therefore be adaptively shortened. The patient’s rigidity, especially on the left side of her body, greatly restricted the regular useful range of motion at the left glenohumeral joint. Graded oscillations joint mobilization techniques as described by Kisner & Colby(13) are useful to encourage synovial fluid exchange and to maintain joint cartilage health. A Grade II oscillations technique, where the glenohumeral joint was distracted, then oscillated back and forth between its resting position and just short of its available distraction range was applied with the intention of achieving the fluid exchange goal.
A Cochrane Review of bowel management strategies indicated that favorable results were obtained with the use of abdominal massage to aid patients with central neurological diseases in the management of constipation.(14) This patient has difficulty moving her bowels and has been prescribed laxatives. She also regularly drinks prune juice, self-administers abdominal massage, and requests her home care nurse to do the same. Since she experiences much trouble with constipation, abdominal massage has been included in the treatment protocol to aid with bowel movements and as a teaching opportunity for more effective self-administration at home. During treatment, patient was advised to drink prune juice 30–60 minutes in advance of massage appointments.
Heat applications are well-known for their therapeutic relaxation effect and their ability to encourage pliability in muscle tissue.(12) Contractures resulting from rigidity and resting tremor can also be treated with a heat application, followed by slow, smooth PROM with overpressure.(2) A moist heating pad, removed from the its hot water bath 10 to 15 minutes prior to application in order to temper the amount of heat being applied, may produce both a relaxation effect as well as reduce the rigidity and pain experienced in the infraspinous fossa of the left scapula at end ranges of glenohumeral motion.
The patient was treated five times with a 60-minute massage per the treatment plan described, over the course of six weeks. Each time, clinical examinations 1–4 from the MI section of the SPES/SCOPA rating scale were performed before and after treatment. The patient was not capable of performing clinical examinations 5 or 6. With exception of Treatment 4, when the patient presented with no tremors, improvements in at least one measurement category were obtained, with improvements in more than one category evident in three of the treatments. In general, rigidity was at the most difficult PD symptom to reduce, with measurable reduction evident at only one treatment. Relaxation and muscle softening lasting one to two minutes at a time was achieved at each treatment. Tremor, when present, was effectively reduced at all treatments. On the patient’s most severe day (Treatment 3), only resting tremor was positively impacted, with no overall change in rigidity or postural tremor by the end of that treatment. Results are summarized in Table 3.
Table 3 Results of Motor Impairments (MI) Section of the SPES/SCOPAa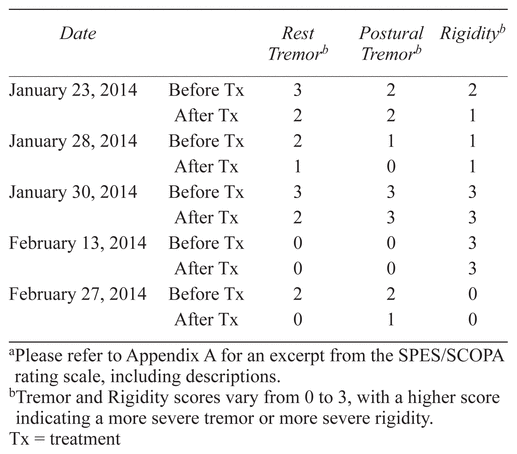
On the sixth visit, after the last visit where the treatment plan described above was implemented, a scanning orthopedic examination was completed once more. The results of the second scan were in accordance with the first and generally unremarkable.
The goal for this case was to determine if massage therapy could be beneficial to a patient suffering from PD. The results obtained showed a consistent decrease in resting tremor for every client visit at which the patient presented with resting tremor. This result confirms previous findings whereby NMT reduced tremor scores in PD patients.(15) Rest and relaxation in general is also reported to be beneficial to aid in decreasing PD tremors.(2) Since there was no control case to compare the effects of MT versus rest and relaxation alone, it is difficult to say whether the effects were a direct result of the MT treatment or a secondary result of rest and relaxation. Postural tremor was reduced, in two of the four visits at which the patient presented to the clinic experiencing postural tremor. Rigidity was by far the most difficult measure in which to effect change for this patient. Rigidity was only reduced by a measurable margin on the first visit. All visits to the clinic were effective in temporarily reducing rigidity for a few minutes at a time during the treatment, but a measurable reduction was not consistently achieved.
Clearly, PD is a complex and life-altering disease. The results obtained in this case showed that MT could be of benefit to a patient suffering from PD in that tremors can be effectively reduced with treatment. Rigidity may also be reduced; however, some alteration of the frequency, duration, or techniques used may be necessary to effect more consistent change. This case is consistent with findings from the limited research base available on the subject in that direct, intentional MT treatment of a patient with PD is beneficial for improving some aspect of the symptom picture of PD. Further study has been recommended by each of the six studies cited on this subject, indicating longer treatment cycles, more patients, better controls, and better follow-up would be beneficial. The recommendation for further study as a result of this case is a reiteration of the same. Of benefit would be a study of a statistically significant sample size of patients with PD, over a recommended treatment cycle of one year. A year’s duration may potentially be long enough to gauge the effects of regular MT treatments on medication dosages, ADL, and deterioration rates of the primary PD symptoms of tremor, bradykinesia, and rigidity. Shorter, more frequent MT treatments may be beneficial based on the findings of this case and previous work, since the effects tend to be temporary. A pilot study to determine ideal frequency, duration, and treatment location (i.e., at the patient’s home, at a neutral location), as well as subject commitment to continue participation for the duration of a longer-term study, would be recommended. Comparisons of patients receiving regular semiweekly MT in conjunction with pharmacotherapy, versus a rest and relaxation plus pharmacotherapy control group, versus a pharmacotherapy only control group, would go a long way towards deciphering if massage therapy may be of long-term benefit to those suffering from PD.
The author would like to extend thanks and appreciation to the staff and faculty at MacEwan University for their guidance, support, and encouragement offered throughout the case management and writing process. It is also with great gratitude to the Massage Therapy Foundation that this report is being submitted for publication. If not for their generous sponsorship and encouragement through the Student Case Report Competition, the thought would never have otherwise crossed my mind. Finally, the author would like to acknowledge the SCOPA-PROPARK (PROfiling PARKinson’s Disease) research team for their kind permission to use the SPES-SCOPA questionnaire.
The author declares there are no conflicts of interest.
1 Werner RA. A Massage Therapist’s Guide to Pathology, 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2013.
2 Rattray F, Ludwig L. Clinical Massage Therapy: Understanding, Assessing and Treating over 70 Conditions. Elora, Ontario, CA: Talus Incorporated; 2000.
3 Parkinson Society Canada. Parkinson Society Canada [Web site]. http://www.parkinsons.ca. Updated June 1, 2013. Accessed January 28, 2014.
4 Chadhuri KR, Clough CG, & Sethi KD. Fast Facts: Parkinson’s Disease, 3rd ed. Abingdon, UK: Health Press Limited; 2011.
5 Marieb EN, Hoehn K. Human Anatomy & Physiology, 8th ed. San Francisco, CA: Pearson Benjamin Cummings; 2010.
6 Nijkrakea MJ, Keus SH, Kalf JG, Sturkenboom IH, Munneke M, Kappelle AC, et al. Allied health care interventions and complementary therapies in Parkinson’s disease. Parkinsonism Relat Disord. 2007;13(Suppl 3):S488–S494.
7 Wang Y, Xie CL, Wang WW, Lu L, Fu DL, Wang XT, et al. Epidemiology of complementary and alternative medicine use in patients with Parkinson’s disease. J Clin Neurosci. 2013;20(8):1062–1067.
8 Hoehn MM, Yahr MD. Parkinsonism: onset, progression, and mortality. Neurol. 1967;17:427–442.
9 Magee DJ. Orthopedic Physical Assessment, 5th ed. St. Louis, MO: Saunders Elsevier; 2008.
10 Marinus JJ, Visser M, Stiggelbout AM, Rabey JM, Martinez-Martin P, Bonuccelli U, et al. A short scale for the assessment of motor impairments and disabilities in Parkinson’s disease: the SPES/SCOPA. J Neurol Neurosurg Psychiat. 2004;75:388–395.
11 Andrade CK. Outcome-Based Massage: Putting Evidence into Practice. Baltimore, PA: Lippincott Williams & Wilkins; 2014.
12 Sinclair M. Modern Hydrotherapy for the Massage Therapist. Philadelphia, PA: Wolters Kluwer Health, Lipincott Wiliams & Wilkins; 2008.
13 Kisner C, Colby LA. Therapeutic Exercise: Foundations and Techniques, 5th ed. Philadelphia, PA: F. A. Davis Company; 2007.
14 Coggrave M, Norton C, Cody JD. Management of faecal incontinence and constipation in adults with central neurological diseases. Cochrane Database System Rev. 2014;1:CD002115.
15 Craig LH, Svircev A, Haber M, Juncos JL. Controlled pilot study of the effects of Neuromuscular Therapy in patients with Parkinson’s disease. Movement Disord. 2006;21(12):2127–2133.
16 Donoyama N, Ohkoshi N. Effects of Traditional Japanese massage therapy on various symptoms in patients with Parkinson’s disease: a case-series study. J Altern Complement Med. 2012;18(3):294–299.
17 Stallibrass C, Sissons P, Chalmers, C. Randomized controlled trial of the Alexander Technique for idiopathic Parkinson’s disease. Clin Rehab. 2002;16(7):695–708.
18 Hernandez-Reif M, Field T, Largie S, Cullen C, Beutler J, Sanders C, et al. Parkinson’s disease symptoms are differentially affected by massage therapy vs. progressive muscle relaxation: a pilot study. J Bodywork Movement Ther. 2002;6(3):177–182.
19 Paterson C, Allen JA, Browning M, Barlow G, Ewings P. A pilot study of therapeutic massage for people with Parkinson’s disease: the added value of user involvement. Complement Ther Clin Pract. 2005;11(3):161–171.
20 Törnhage CJ, Skogar Ö, Borg A, Larsson B, Robertsson L, Andersson L, et al. Short- and long-term effects of tactile massage on salivary cortisol concentrations in Parkinson’s disease: a randomised controlled pilot study. Complement Altern Med. 2013;13:357.
Rest tremor
assess each arm separately during 20 seconds; hands rest on thighs; if tremor is not evident at rest, try to keep the patient attentive, e.g. by having him/her count backwards with eyes closed
0 = absent
1 = small amplitude (< 1 cm) occurring spontaneously, or obtained only while keeping patient attentive (any amplitude)
2 = moderate amplitude (1–4 cm), occurring spontaneously
3 = large amplitude (≥ 4 cm), occurring spontaneously.
Postural tremor
check with arms outstretched, pronated and semipronated, and with index fingers of both hands almost touching each other (elbows flexed); assess each position during 20 seconds
0 = absent
1 = small amplitude (< 1cm)
2 = moderate amplitude (1–4 cm)
3 = large amplitude (≥ 4 cm).
Rapid alternating movements of hands
rapid alternating pronation/supination movements of upper hand, each time slapping the palm of the horizontally held lower hand during 20 seconds; each hand separately
0 = normal
1 = slow execution, or mild slowing and/or reduction in amplitude; may have occasional arrests
2 = moderate slowing and/or reduction in amplitude or hesitations in initiating movement or frequent arrests in ongoing movements
3 = can barely perform task.
Rigidity
assess passive movements of elbow and wrist over full range, with the patient relaxed in sitting position; ignore cogwheeling; check each arm separately
0 = absent
1 = mild rigidity over full range, no difficulty reaching end positions
2 = moderate rigidity, some difficulties reaching end positions
3 = severe rigidity, considerable difficulties reaching end positions.
Rise from chair
patient is instructed to fold arms across chest; use straight back chair
0 = normal
1 = slowly; does not need arms to get up
2 = needs arms to get up (can get up without help)
3 = unable to rise (without help).
Postural instability
stand behind the patient and pull patient backwards, while s/he is standing erect with eyes open and feet spaced slightly apart; patient is not prepared
0 = normal, may take up to 2 steps to recover
1 = takes 3 or more steps; recovers unaided
2 = would fall if not caught
3 = spontaneous tendency to fall or unable to stand unaided.
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK, VOLUME 9, NUMBER 1, MARCH 2016