Niki Munk , PhD, LMT 1,*, Karen Boulanger , PhD, CMT 2
1 Department of Health Sciences, Indiana University - IUPUI, Indianapolis, IN
2 Department of Anesthesia, Stanford University School of Medicine, Stanford, CA
Case reports provide the foundation of practice-based evidence for therapeutic massage and bodywork (TMB), as well as many other health-related fields. To improve the consistency of information contained in case reports, the CARE (CAse REport) Group developed and published a set of guidelines for the medical community to facilitate systematic data collection (http://www.care-statement.org/#). Because of the differences between the practice of medicine and TMB, modifying some sections of the CARE guidelines is necessary to make them compatible with TMB case reports. Accordingly, the objectives of this article are to present the CARE guidelines, apply each section of the guidelines to TMB practice and reporting with suggested adaptations, and highlight concerns, new ideas, and other resources for potential authors of TMB case reports.
The primary sections of the CARE guidelines adapted for TMB case reports are diagnostic assessment, follow-up and outcomes, and therapeutic intervention. Specifically, because diagnosis falls outside of the scope of most TMB practitioners, suggestions are made as to how diagnoses made by other health care providers should be included in the context of a TMB case report. Additionally, two new aspects of the case presentation section are recommended: a) assessment measures, which outline and describe the outcome measures on which the case report will focus, and b) a description of the TMB provider (i.e., scope of practice, practice environment, experience level, training, credentialing, and/or expertise) as part of the intervention description.
This article culminates with practical resources for TMB practitioners writing case reports, including a TMB Case Report Template—a single document that TMB practitioners can use to guide his or her process of writing a case report. Once the template is adopted by authors of TMB case reports, future efforts can explore the impact on the quality and quantity of case reports and how they impact TMB practice, research, education and, ultimately, the clients.
KEYWORDS: case study , massage therapy , manual therapy , evidenced-based practice
Case reports provide the foundation of practice-based evidence for therapeutic massage and bodywork (TMB), as well as many other health-related fields including nursing, physical therapy, occupational therapy, chiropractic, and primary care. The reasons to write and publish case reports have been covered extensively in the literature with Green and Johnson(1) providing an excellent summary. Case reports are written to document a novel condition, clinical hypotheses, and adverse consequences of care(1), as well as to share clinical reasoning, treatment approach, and client outcomes. By generating hypotheses and new research questions, case reports stimulate further research that is relevant to clinical practice. Additionally, multiple well-documented case reports that present similar topics may be combined to provide a bigger “picture” of the condition and outcomes in relation to particular TMB treatment(s). However, the impact of case reports can be attenuated by unsystematic or insufficiently rigorous reporting methods(2).
In efforts to facilitate more uniform reporting across methods of research to enhance the ability to compare and contrast studies on similar topics or with similar methods, several reporting guidelines have been developed and recently reformulated. For example, the CONSORT Statement aids the reporting of randomized controlled trials(3), the STROBE Statement aids reporting observational studies(4), and the PRISMA Statement directs reporting for systematic reviews and meta-analyses(5). To address the unique components of case reports, a set of guidelines has recently been developed for the medical community(2).
The CARE (CAse REport) guidelines were developed by the CARE Group to address the concern that case reports typically have unsystematic or insufficiently rigorous reporting which poses challenges to the aggregation of such evidence for data analysis, informing research design, or guiding clinical practice(2). The Group’s efforts to develop systematic guidelines for case reports resulted in a 13-item checklist which constitutes the CARE guidelines. Although different from how to write case reports , which has been specifically addressed in TMB text books in the past(6,7), the newly developed and disseminated CARE guidelines offer an opportunity to revisit the subject of effective writing criteria for TMB case reports. The CARE Group advocates for the adoption of these guidelines in all fields that employ case reports in the literature base, and acknowledges that expansion and/or modifications to the guidelines may be necessary to accommodate specific practices or specialties(2,8). Many differences exist between the practices of medicine and TMB, making modification to the CARE guidelines necessary for compatibility with TMB case reports. Accordingly, the primary objectives of this article are to present the CARE guidelines, apply each item to TMB practice and reporting with suggested adaptations, and highlight concerns and other resources for potential authors of TMB case reports. Ultimately, the purpose of this work is to support and facilitate effective reporting of the data contained in TMB case reports.
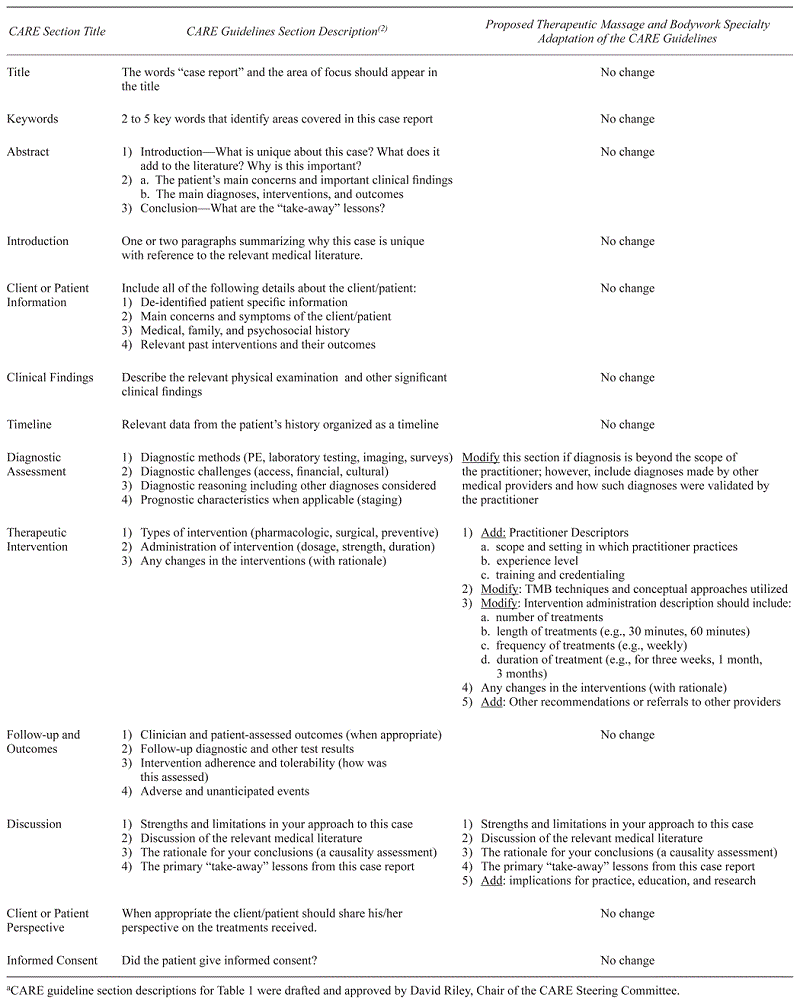
Table 1 presents each CARE section and its description, and any suggestions for modifications and additions to the section for application to TMB case reports (grey text indicates no suggested changes). Each section of the CARE guidelines are numbered 1–13 in Gagnier and colleagues’ work(2): 1) title, 2) keywords, 3) abstract, 4) introduction, 5) patient information, 6) clinical findings, 7) timeline, 8) diagnostic assessment, 9) therapeutic intervention, 10) follow-up and outcomes, 11) discussion, 12) patient perspective, and 13) informed consent. These items can be placed into two groups: those that precede the manuscript (CARE sections 1–3) and those that constitute the manuscript body (CARE sections 4–13). Table 2 presents the full set of resulting TMB case report sections, adapted from the CARE guidelines, which we refer to as the TMB Case Report Template. The order of case report sections presented in Table 2 provides the structure for the discussion of our recommendations below, and reflects the order in which the items should appear in a TMB case report.
Table 1
CARE Guideline Sections and Descriptionsa and TMB Specialty Specific Adaptations
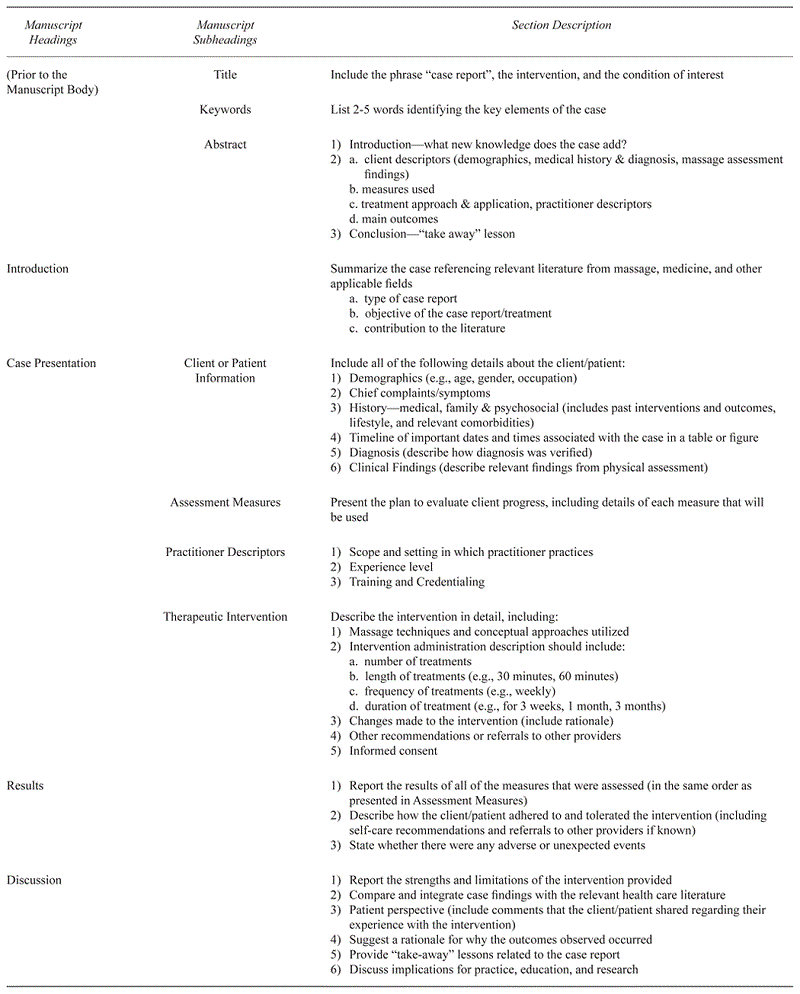
Table 2
Therapeutic Massage and Bodywork Case Report Template
The first three sections of the CARE guidelines checklist (title, keywords, and abstract) address aspects of the case report that precede the body of the manuscript.
Title and keywords are unchanged from prior discussions of case reports in the TMB field and no modifications for application to TMB case reports are needed.
The abstract reflects the body of the report segmented into three sections: an introduction, a case presentation, and a discussion. The aspects of the CARE checklist’s case presentation need to be modified for a TMB case report to reflect appropriate scope of practice. The case presentation should include a description of the client (demographics, medical history and diagnosis, and massage assessment findings), treatment approach and application, therapist description, and main outcomes.
The case report begins with an Introduction. The brief description provided by the CARE guidelines mirror the recommendations of others in the TMB field(6,9). It is helpful to add an appropriate transition from the Introduction to the next sections of the case report. Specifically, a couple of sentences should conclude the case report’s Introduction and state the general objective and some other supporting details. The following is an example template for such a transition that may be used for TMB case reports:
The current manuscript is a retrospective/prospective case report examining the outcomes of a 32-year-old woman with fibromyalgia after a course of massage therapy intended to reduce her pain and improve her ability to participate in life activities. Little evidence exists for massage effects for fibromyalgia and none specifically examines massage therapy combined with craniosacral techniques.
The items of note in this template transition are: a) specification is made as to the type of case report, either prospective or retrospective†; b) the objective for the case report is defined; c) the significance of the case report and what it adds to the literature is identified.
The beginning of what could be considered the “Methods” section of a TMB case report starts with patient/client information. The only modification we suggest is to adjust the title of the section accordingly, to reflect the nomenclature of the case report’s setting. Specifically, the term “patient” or “client” should be used depending on which is most customary from the author of the report’s perspective and used consistently throughout the manuscript.
A detailed timeline presented in a table or figure could be an effective way to illustrate the duration of the condition, while placing the TMB treatment in relation to the condition’s progression and current and/or previous treatment strategies. Although the CARE Group lists this as an inclusion item, we consider a timeline in a TMB case report optional, most appropriate for case reports where the information is known, and it helps place the TMB treatment in context.
Modification may be required for the diagnostic assessment section for applicability to TMB case reports. Keeping in mind that diagnosis is outside of most TMB practitioners’ scope of practice in North America and in other parts of the world, this section of the TMB case report should include diagnostic assessments that have been made by other medical providers. While those who provide TMB under another field’s scope of practice (Doctors of Osteopathy, Doctors of Chinese Medicine, physical therapists, etc.) may use specific diagnostic assessments, the way this guideline is described by the CARE Group does not apply to most TMB practitioners. Therefore, we suggest a more appropriate inclusion of this CARE guideline for a TMB case report and for it to be included as part of the patient information presentation. It is important to note here that client self-diagnosis would not be appropriate for inclusion as part of the diagnosis assessment. It is important for the TMB practitioner to verify diagnoses either through contact with the health care provider (with appropriate HIPAA compliance) or through materials provided by the client (e.g., test results, physician orders, etc.) because clients are sometimes poor historians. For example, a client may report a herniated disk in their lower back, while a physician report identifies a fracture of two vertebras, the presence of arthritis, and degenerative disc disease—all of which would alter the treatment plan of a TMB practitioner.
Changing the order presented by the CARE Group, the next section is clinical findings, defined as information relevant and derived from a physical assessment. TMB practitioners may document their assessment of the client in relation to the condition from within their scope of practice. This may include visual observations from a postural and/or gait analysis, or information gathered during palpation and active or passive range of motion. It is also appropriate to provide clinical reasoning for speculations the practitioner may have in regard to the information gathered during the assessment.
Addressed later in the CARE guidelines as part of follow-up and outcomes is the reporting of the measures and/or methods used to gather primary or secondary outcomes. We suggest the introduction of these measures comprises its own section and should be titled assessment measures. For TMB case reports, the case report outcome measures and methods should be described after the clinical findings section. Accordingly, this information would be collected during the interview and physical examination prior to the commencement of treatment application. Organizing the assessment measures section is important. For each assessment, state what was measured, why that measure was chosen, as well as how, where, and when it was measured. Psychometric properties and clinically meaningful change, especially in the context of TMB, should also be included, if available. These sorts of details allow for better replication in future work, and a more pertinent and contextual discussion of the case report’s results.
We suggest several additions to the CARE guideline therapeutic intervention for adaptation to TMB case reports. This section should begin with a description of the TMB practitioner, in addition to the environment in which treatments are provided (e.g., hospital, private practice, spa, gym). Unlike most health care-related fields, entry-level standard education and practice guidelines for TMB do not exist. Therefore, practitioner descriptions become very important when seeking to understand the context and/or generalizability of a particular case report to clinical practice, education, or other research activities. Specifically, the TMB practitioner’s scope of practice, experience level, training, credentialing, and/or expertise would provide pertinent context to the treatment results and implications(11). In addition, other professionals (e.g., physical therapists and chiropractors) may provide TMB within their scope, but from an overall different approach. TMB interventions that are applied by professionals from other fields need to be clearly reported as such for accountability and utility in methodology.
Practitioners/authors should next report the conceptual approach within which the actual intervention techniques were applied. While techniques such as skin rolling, effleurage, petrissage or gentle rocking are used in many different TMB modalities, nuance as to their application may be different, if applied, for example, from the Barnes Myofascial Release or Trager approaches. Clarifying such conceptual approaches, if applicable, may assist in case report applicability and utilization in practice, research, and education settings. Additionally, the number, length, and frequency of treatment applications, in addition to the techniques applied (with description), to which body regions, and for approximately how long, are required(6). Peirson(12) provides an excellent example of a “treatment plan outline” in the form of a table, saving space in the body of the case report for substantive discussion (case reports are often limited in word counts from 1,500–3,000 words). The therapeutic intervention section should end with any recommendations for self-care (e.g., stretches, exercise, stress management) or referrals to other providers (e.g., medical specialist, chiropractor, acupuncturist).
We recommend including the informed consent at the end of the case presentation section for TMB case reports. In order to meet ethical obligations in reporting and publishing client personal information (never including names, contact information, unmasked images, and the like), all efforts to secure informed consent should be made for case reports.
The items included in the CARE guidelines for the Results section of a manuscript (titled by the CARE Group as Follow-Up and Outcomes) are all applicable to TMB case reports and need no specific modifications. For clarity, results should be reported in the order in which the measures used were presented in the assessment measures section. As a reminder, the Results section is not the place for results interpretation , and care must be taken to simply present the information without commentary. Presenting the results by way of tables, figures, and photographs can be very effective and is used effectively in many previously published TMB case reports(13,14). It is notable that client adherence to and/or compliance with self-care tasks and referrals to other providers made by the TMB practitioner should be reported in the Results section of the TMB case report, if the information is known.
The CARE Group gives a brief description of the discussion item in four points to which we add a fifth: “take-away” lessons should include suggestions for interpreting the findings in light of TMB practice, education, and research. As a reminder, it is essential that statements made in the Discussion of all case reports are objective and free of unsubstantiated claims(1). Case reports do not prove anything or establish cause–effect relationships between an intervention and outcome. While findings from a single case report are not generalizable to other clients or similar populations, they do provide practice-based evidence for clinical consideration and application for various practitioners in fields with TMB that fall within their scope of practice.
Inclusion of the patient (or client) perspective in the discussion gives an opportunity for the client to “voice” his or her perspective on the experience.
The previous aspects of this article introduce the CARE guidelines to TMB practitioners, while suggesting modifications and additions to better reflect TMB practices and enhance their applicability and utility for TMB case reports. We present our suggestions of TMB case report sections in a logical order to mirror the order in which such details would appear in a TMB case report manuscript. We have also framed these sections within the main paper headings for a TMB case report: Introduction, Case Presentation, Results, and Discussion. Table 1 is composed in such a way as to clearly highlight the intellectual content presented by the CARE guidelines, by having a column solely dedicated to its section description and a separate column highlighting our suggestions for adaptability needs for TMB case reports. However, TMB practitioners may find a single and concise resource for guidance during the composition of a case report more helpful. Furthermore, clear subheadings expected in a TMB case report are difficult to clearly identify with the presentation of Table 1.
The TMB Case Report Template (Table 2) is a single document that a TMB practitioner can use to guide his or her writing process of a case report. With this resource, we have compiled all of the TMB case report sections (adapted from the CARE guidelines) and presented them within the headings and subheadings that will clearly identify these aspects in the TMB case report and appropriately frame the overall manuscript. We hope that TMB practitioners, regardless of the field from which they practice, find the TMB Case Report Template a valuable resource, along with our detailed explanations of CARE guideline modifications and additions and practical writing advice.
There are other resources which would likely benefit a potential author of a TMB case report. The first category includes educational efforts to assist with case report writing. Volunteers from the Massage Therapy Foundation, in collaboration with Associated Bodywork and Massage Professionals, created a five-part case report webinar series covering the various aspects of writing a TMB case report(9). The recordings are available free of charge at http://info.massagetherapyfoundation.org/blog/bid/295070/Writing-Case-Reports-Free-Five-Part-Webinar-Series. In addition, TMB practitioner and case report author Michael Hamm contributed a book chapter on case report development and completion to Dryden and Moyer’s text Massage Therapy: Integrating Research and Practice (6). TMB practitioner and researcher Glenn Hymel also provides discussion on the writing of case reports in his book, Research Methods for Massage and Holistic Therapies (7).
The second category of resources relate to the value of reading previously prepared and/or published case reports when preparing to write your own. CaseRe3 is a searchable online open access repository for case reports in integrative health care (http://www.casere3.org/)(15). TMB case reports published in peer reviewed journals are also an excellent resource for use as examples when preparing a TMB case report. In the past decade, TMB case reports have been published on ankylosing spondylitis(16), cervical degenerative disk disease(17), erythromelalgia(18), lumbar fusion(19), Lyme disease(20), Morton’s neuroma(21), narcolepsy(13), patellofemoral pain syndrome(14), rheumatoid arthritis(22), spinal cord injury(23), and temporomandibular joint dysfunction(12) in the International Journal of Therapeutic Massage and Bodywork ( IJTMB ), and on abdominal pain(24), diabetic neuropathy(25), dwarfism(26), fibular hemimelia(27), low back pain(28), lumbar spondylolisthesis(29), and scoliosis(30) in The Journal of Movement and Bodywork Therapies . New case reports are published periodically in both of these Journals and both consider the publication of case reports as valuable contributions to their Journal and the TMB field(31–33). While published TMB case reports may be challenging to access for the typical TMB practitioner due to subscription cost and/or inexperience with peer-review publication retrieval, some applicable journals are open access. Open access allows case reports published in IJTMB (http://www.ijtmb.org), for example, available free of charge.
Another resource for practitioners regarding the development and completion of TMB case reports involves assistance with choosing appropriate measures to monitor client outcomes. The Canadian Interdisciplinary Network for Complementary and Alternative Medicine Research (IN-CAM) Outcomes Database(34) (http://www.outcomesdatabase.org/) is a searchable database which provides measures across nine domains, including quality of life, social, physical, psychological, and individualized. Information describing each measure includes sample items, administration instructions, and references about its reliability and validity. See Kania and colleagues(35) for an in-depth description of the relevance and application of the database for TMB practitioners.
Finally, writing in isolation for any author is challenging. This challenge is all the more intense for individuals with little experience or training in scientific and/or academic writing, and few TMB practitioners have such training. Seeking a writing partner or mentor to share authorship in no way diminishes the value or contribution of the TMB practitioner, especially if such a pairing strengthens the overall writing, thereby improving the report’s chances for successful publication and dissemination. For TMB practitioners who feel intimidated by, or are less confident with, the challenges posed by writing for publication, we strongly encourage you to find a writer with whom to collaborate. Suggestions as to how such collaborative partnerships can develop are available in the current TMB literature(32,36).
This article and the TMB Case Report Template are the result of our work to make the CARE guidelines accessible and applicable to TMB practitioners who wish to write case reports. While we have sought and considered feedback from others in the TMB field (gratefully thanked in the Acknowledgments), we acknowledge the inherent limitations of these suggestions being made primarily by the consensus of two people. However, we are in a unique position to offer such insight because each of us has been a TMB practitioner, researcher, educator, and journal editor, as well as a mentor to TMB practitioner authors of case reports. In addition, our experience with TMB case reports, specifically as journal editors working with TMB practitioners from diverse education and specialization backgrounds, has given us insight into the information that TMB practitioners need to successfully write and publish meaningful case reports.
The CARE guidelines presented by Gagnier and colleagues(2) are a timely and much-needed resource for clinical practitioners seeking to inform their field and contribute to the foundations of patient/client care research. Similar to medical case reports, nonstandardized and inconsistent reporting of TMB case reports challenge the impact of these contributions on the field and in the research literature. Due to the unique qualities of TMB practice, modifications and additions to the medical case report guidelines presented by the CARE Group are needed for complete applicability. In response to this, we considered the CARE guidelines in light of TMB practice and adjusted the specific sections accordingly resulting in our TMB Case Report Template. Once the template is adopted by authors of TMB case reports, future efforts can explore the impact on the quality and quantity of case reports and how they impact TMB practice, research, education and, ultimately, the clients. We welcome discussion with us and among all TMB practitioners, educators, and researchers as to how the CARE guidelines and our TMB Case Report Template can improve the TMB field overall and allow more practitioners the opportunity to contribute to the research foundation of our field through the writing and publishing of high-quality case reports.
Thanks and acknowledgement is extended to David Riley, Chair of the CARE Steering Committee, in his support and contribution to the manuscript, specifically in creating the CARE guideline section description used in Table 1. The authors would also like to thank and acknowledge the support and feedback received from two groups in the drafting and revising of this manuscript. Members of the Massage Therapy Foundation Board of Trustees: John Balletto, Jerrilyn Cambron, Ann Blair Kennedy, and Michael Hamm. Indian University’s Department of Occupational Therapy Writing Group: CJ Liu, Fengyi Kuo, Patricia Scott, and Sharon Pape. We thank you each for your thoughtful feedback and suggested considerations regarding our recommendations for CARE guideline adaptability for TMB case reports.
The authors declare there are no conflicts of interest.
1 Green BN, Johnson CD. How to write a case report for publication. J Chiropr Med. 2006;5(2):72–82.


2 Gagnier JJ, Kienle G, Altman DG, Moher D, Sox H, Riley D. The CARE Guidelines: consensus-based clinical case reporting guideline development. J Clin Epidemiol. 67(1):46–51.
3 Moher D, Hopewell S, Schulz KF, Montori V, Gøtzsche PC, Devereaux PJ, et al. CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. J Clin Epidemiol. 2010;63(8):e1–e37.

4 von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: guidelines for reporting observational studies. Prev Med. 2007;45(4):247–251.

5 Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151(4):264–269.

6 Hamm M. Chapter 20: Clinical Case Reports. In: Dryden T, Moyer CA, editors. Massage Therapy: Integrating Research and Practice. Champaign, IL: Human Kinetics; 2012. p.233–242.
7 Hymel G. Research Methods for Massage and Holistic Therapies. St. Louis, MO: Elsevier Health Sciences; 2005.
8 CARE Steering Committee, Riley D, Gagnier J, Kienle G, Moher D, Plotnikoff G, et al. CARE Guideline: Website for Case Reports [Accessed: June 10, 2014]. Available from: http://www.care-statement.org/#
9 Vulkits M. Writing Case Reports: Free Five-Part Webinar Series [blog post]. Feb. 19, 2013. [Accessed: June 10, 2014]. Available from: http://info.massagetherapyfoundation.org/blog/bid/295070/Writing-Case-Reports-Free-Five-Part-Webinar-Series
10 Hess DR. Retrospective studies and chart reviews. Respiratory Care. 2004;49(10):1171–1174.
11 Porcino AJ, Boon HS, Page SA, Verhoef MJ. Exploring the nature of therapeutic massage bodywork practice. Int J Ther Massage Bodywork. 2013;6(1):15–24.

12 Pierson MJ. Changes in temporomandibular joint dysfunction symptoms following massage therapy: a case report. Int J Ther Massage Bodywork. 2011;4(4):37–47.
13 Hill R, Baskwill A. Positive effects of massage therapy on a patient with narcolepsy. Int J Ther Massage Bodywork. 2013;6(2):24–28.

14 Zalta J. Massage therapy protocol for post-anterior cruciate ligament reconstruction patellofemoral pain syndrome: a case report. Int J Ther Massage Bodywork. 2008;1(2):11–21.

15 CaseRe3. CaseRe3: Case Report Research Repository. [Accessed: June 10, 2014]. Available from: http://www.casere3.org/
16 Chunco R. The effects of massage on pain, stiffness, and fatigue levels associated with ankylosing spondylitis: a case study. Int J Ther Massage Bodywork. 2011;4(1):12–17.

17 Avery RM. Massage therapy for cervical degenerative disc disease: alleviating a pain in the neck? Int J Ther Massage Bodywork. 2012;5(3):41–46.

18 Dicks K, Rizek P. Massage therapy techniques as pain management for erythromelalgia: a case report. Int J Ther Massage Bodywork. 2010;3(4):5–9.

19 Keller G. The effects of massage therapy after decompression and fusion surgery of the lumbar spine: a case study. Int J Ther Massage Bodywork. 2012;5(4):3–8.
20 Thomason MJ, Moyer CA. Massage therapy for lyme disease symptoms: a prospective case study. Int J Ther Massage Bodywork. 2012;5(4):9–14.
21 Davis F. Therapeutic massage provides pain relief to a client with Morton’s neuroma: a case report. Int J Ther Massage Bodywork. 2012;5(2):12–19.

22 Cubick EE, Quezada VY, Schumer AD, Davis CM. Sustained release myofascial release as treatment for a patient with complications of rheumatoid arthritis and collagenous colitis: a case report. Int J Ther Massage Bodywork. 2011;4(3):1–9.

23 Manella C, Backus D. Gait characteristics, range of motion, and spasticity changes in response to massage in a person with incomplete spinal cord injury: case report. Int J Ther Massage Bodywork. 2011;4(1):28–39.

24 Muscolino JE. Abdominal wall trigger point case study. J Bodyw Mov Ther. 2013;17(2):151–156.

25 Finch P, Baskwill A, Marincola F, Becker P. Changes in pedal plantar pressure variability and contact time following massage therapy: a case study of a client with diabetic neuropathy. J Bodyw Mov Ther. 2007;11(4):295–301.
26 Hanson AA. Improving mobility in a client with hypochondroplasia (dwarfism): a case report. J Bodyw Mov Ther. 2010;14(2):172–178.

27 Larson ER. Massage therapy effects in a long-term prosthetic user with fibular hemimelia. J Bodyw Mov Ther. [in press] Available at: http://dx.doi.org/10.1016/j.jbmt.2014.04.005
28 Bell J. Massage therapy helps to increase range of motion, decrease pain and assist in healing a client with low back pain and sciatica symptoms. J Bodyw Mov Ther. 2008;12(3):281–289.

29 Halpin S. Case report: the effects of massage therapy on lumbar spondylolisthesis. J Bodyw Mov Ther. 2012;16(1):115–123.
30 Hamm M. Impact of massage therapy in the treatment of linked pathologies: scoliosis, costovertebral dysfunction, and thoracic outlet syndrome. J Bodyw Mov Ther. 2006;10(1):12–20.
31 Chaitow L. The ‘humble’ case-study [editorial]. J Bodyw Mov Ther. 2006;10(1):1–2.
32 Munk N. Case reports: a meaningful way for massage practice to inform research and education. Int J Ther Massage Bodywork. 2013;6(3):3–5.

33 Boulanger KT. From the practice section editor’s perspective. Int J Ther Massage Bodywork. 2008;1(1).

34 IN-CAM. IN-CAM: Outcomes Database [Accessed: June 10, 2014]. Available from: http://www.outcomesdatabase.org/content/welcome-cam-outcomes-database
35 Kania A, Verhoef MJ, Dryden T, Ware MA. IN-CAM Outcomes Database: its relevance and application in massage therapy research and practice. Int J Ther Massage Bodywork. 2009;2(1):8–16.

36 Werner R. How to Connect with a Researcher [e-book]. Massage Therapy Foundation; 2014. Available from: http://info.massagetherapyfoundation.org/blog/bid/320441/How-to-mingle-with-researchers-at-a-conference
† Retrospective case reports use data from treatment notes after the fact that were documented in the course of usual care(10). A prospective case report or study is one in which criteria, measures, and treatment parameters are established first, and then a person or people who meet that criteria is/are included. ( Return to Text )
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License . ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK , VOLUME 7 , NUMBER 3 , September 2014