Sylvia L. Burns , M.Ed., LMP
University of Washington Medical Center, Department of Rehabilitation, Roosevelt Center - Exercise Training Center, Seattle, WA, USABackground
Concussion, its recognition, diagnosis, and treatment is a growing public health issue. Massage practitioners who specialize in rehabilitation deal with a variety of injury cases that involve concussion, including those incurred by falls, motor vehicle incidents, and sports injuries.
Purpose
This case study presents a unique massage therapy approach to concussion trauma treatment.
Participant
Male 23-year-old intramural soccer player diagnosed with postconcussion syndrome resulting from a fall.
Intervention
Assessment and treatment were completed in two sessions of 45 minutes spaced two days apart. Massage therapy techniques were applied to injury areas by a Licensed Massage Practitioner.
Results
Using the Balance Error Scoring System (BESS) and self-report, the outcome measures showed diminished concussion symptoms and regained ease in range of motion in the cervical area.
Conclusion
Positive results for this case highlight the potential importance of massage therapy work to reduce headache, dizziness, and nausea in concussion recovery. In the presence of such outcomes, massage therapy may also have a supportive role in a person’s return to function after concussion.
KEYWORDS: massage , musculoskeletal manipulations , postconcussion symptoms , brain injuries
The Center for Disease Control (CDC) states that each year, “traumatic brain injuries contribute to a substantial number of deaths and cases of permanent disability.”(1) Traumatic brain injuries (TBI) are a contributing factor to 30.5% of all injury-related deaths in the US.(2) Between 2002–2006, the estimated average number of TBI in the United States was 1.7 million annually and about 75% of those are concussions or other forms of mild traumatic brain injury (mTBI).(1) The CDC estimates that the true incidence of mTBI, many of which are not seen in the ER, diagnosed or reported, may be 4 million cases per year.(3,4)
The CDC describes TBI as injury caused by a bump, blow or jolt to the head or a penetrating head injury that disrupts the normal function of the brain, with severity ranging from ‘mild’ to ‘severe’. TBI results from external causes of falls, motor vehicle incidents, sports, and military incidents. Faul et al.(2) estimate during the four-year period (2002–2006) , there occurred an increase of TBI fall-related ER visits to youth under 14 of 62%, and adults 65+ (46% ER visits, 34% hospitalizations, 27% deaths). In addition, these findings showed that 95%–97% of chronic headaches were associated with patient concussions. The socioeconomic repercussions of non-fatal TBIs are high, and many lose their ability to hold down a job and must rely on caregivers.(5) Direct and indirect costs of productivity due to TBI in 2000 was estimated to be $76.5 billion in the United States.(6)
Mild TBI is a poorly-understood health problem.(7) Currently, there is little understanding of the classification, evolution, duration or resolution of mTBI.(8) Most individuals with concussion/mTBI recover completely; however, a significant proportion report post-concussive symptoms for months to years following the injury.(9) Persistent symptoms can manifest into neurological and nonneurological problems that can affect functional outcome.(7) To date, no randomized control trials have examined the effects of different approaches for concussion treatment. The rehabilitation approaches with minimal research include hyperbaric oxygen therapy,(10) graduated aerobic exercise,(11) and massage therapy.(12,13) Thus, best practice for symptoms associated with concussion (i.e., headache, whiplash, and muscle imbalance in the cervical spine region) has been primarily informed by clinical expertise from a variety of disciplines rather than research. The current recommended treatment for concussion recovery is graduated aerobic exercise.(11) The clinical rationale for the use of aerobic exercise is that the regulatory system is responsible for maintaining cerebral blood flow and that any dysfunction in cerebral blood flow post-concussion can be restored by controlled, graded symptom-free exercise.(11) For example, the treatment in sports medicine focuses on regulated exercise postconcussion, although this approach resolves symptoms in only some patients.(14) A clinical study(15) showed that four or more symptoms such as drowsiness, concentration difficulties, nausea, and sensitivity to light and noise at the time of initial injury, not a loss of consciousness, predicted ongoing persistent concussion symptoms. The 2013 report of the American Academy of Neurology highlighted the need for “interventions that enhance recovery, reduce recurrent concussion risk, or diminish long-term sequelae”.(16)
To address the American Academy of Neurology’s call, this case study describes the results of a manual therapy treatment approach for mTBI. Massage practitioners who specialize in rehabilitation of patients’ medical conditions deal with a variety of injury cases including those incurred by falls, motor vehicle incidents, and sports injuries. Any of these traumas may include concussion symptoms. The American Academy of Neurology (AAN) recognizes concussion as a clinical syndrome of biomechanically induced alteration of brain function, typically affecting memory and orientation, which may involve loss of consciousness.(16) The Consensus Statement on Concussion in Sport(17) says that concussion is “due to a complex pathophysiological processes affecting the brain, induced by biomechanical forces”. The atlanto-occipital joint can be slightly subluxated as a result of concussion trauma impact. The importance of addressing positioning of the atlanto-occipital joint in the treatment of concussion is apparent in the biomechanical studies of head trauma by Viano(18) and Unterharschneidt(19) that demonstrate the multidirectional movements of the cranium in relationship to the atlas in the atlanto-occipital joint during a trauma event. The head kinematics include rapid head displacement, z-axis rotation, and neck tension up to the time of maximum strain in the midbrain.(13) It was the premise of this case study that a subluxated atlanto-occipital joint can be effectively returned to its anatomical position using soft tissue massage and manual therapy techniques to reduce concussion symptoms.
This retrospective mTBI case study illustrates the application of massage therapy techniques in efforts to allow the atlanto-occipital joint to correct into preferred anatomical position for a patient with diagnosed post-concussion condition with persistent symptoms. This case study provides a clinical care example of massage therapy to address concussion related symptoms in an effort to educate the therapeutic massage and bodywork field and promote future research.
A 23-year-old male graduate student sustained a head injury during an intramural soccer game. He fell, hitting the back of his head on a bench. He lost consciousness for 20–30 seconds as witnessed by his teammates. The blow was to the right occipital area which left a bump and caused pain. He had a 4 cm edematous bruise on the right occipital area. Treated at the scene with ice compresses, he was sent for medical evaluation which indicated no fractures or bleeding. The patient denied seizures, worsening headaches, vision changes, hearing loss, difficulty with speech, memory loss, and loss of strength or sensation in extremities. This was the patient’s first known concussion injury.
The first day postinjury, the patient reported headaches upon waking. The patient sought care from his primary care provider at the university’s student health center. He reported that his headache pain was in the 8–9 level range on a 10-point scale in which 10 is most severe. The patient also reported motion sickness with car or boat travel, which was particularly troubling because he did field work for his graduate research aboard a boat. The headaches were accompanied by nausea and difficulty concentrating such that they interfered with normal functioning and daily tasks. Cervical strain symptoms were apparent in bilateral soreness and stiffness. The primary care provider prescribed several medications for symptom resolution, as well as rest.
After three weeks he returned to the health clinic as he was experiencing continued symptoms including headache, nausea with movement (such as leaning over to tie shoes), and difficulty concentrating on computer tasks. He described his thinking as “fuzzy”, and reported that he was unable to operate a fishing boat and was only able to focus on data analysis for 15 minutes at a time. The patient received no neuro-cognitive testing. At this point, the provider, familiar with the concussion and trauma work of the author, referred the patient for massage therapy treatment. There were no other modalities applied to the patient other than prescribed massage therapy.
The massage practitioner’s intake procedure included review of the patient’s medical chart, patient’s general health and history of the event, treatment since the trauma event, and patient complaints including intensity, duration, and frequency of signs and symptoms. Self-reported VAS pain levels were noted. The physical assessment involved postural observation to assess for any imbalances or asymmetries in the pelvic girdle, shoulder girdle, cervical area. Then standing balance was evaluated using the static postural stability clinical test, Balance Error Scoring System (BESS),(20,21) which involved standing on two feet and then one foot with eyes closed using both a hard and soft standing surface. The BESS evaluation has moderate to good reliability to assess static balance which includes feedback functioning from visual, somatosensory and vestibular systems. Scoring is based on the number of times the person commits errors including opening of eyes, removing hands from hips, lifting heels or forefoot from surface, moving hips more than 30° of flexion or abduction, stepping, stumbling, or falling, or staying out of the testing position more than 5 seconds. Multiple errors occurring at once counts as one point. A lower score indicates fewer errors were committed.
Once the patient was on the table, palpation of the pelvic, cervical, and shoulder region was done to assess muscle hypertonicity and strength in these areas. Table 1 outlines the assessment tools, methods, and rationale used in the completion of this case study.
Table 1
Interventions — Tools and Assessment Methods

The goal of the intervention treatments was to facilitate musculoskeletal balance. A foundation principle for this case’s treatment plan is the concept that when there is imbalance in the symmetry of the body or body part, antagonist muscles contract in an effort to pull the body back to anatomically preferred position. If the imbalance is removed, the muscles revert to normal tonicity.
One month following the injury incident, the patient received two massage therapy sessions focused on concussion care, each 45 minutes in length. These sessions were administered two days apart at a medical center clinical massage office. The massage practitioner based the intervention on knowledge of anatomy/kinesiology, of biomechanical effects of the incident, of massage and manual techniques, as well as 20 years of clinical experience.
The patient was observed and evaluated for postural balance, specific cervical symmetry, pain level, and symptoms at each session prior to applying treatment. One week after the second treatment application, the patient returned for a follow-up appointment during which information was collected but no massage intervention was applied. The patient was discharged from care at that time.
The patient lay clothed, in a prone position on a massage table for the start of each treatment. In acknowledgment of its role to provide a base for spinal structure and function, treatments began with the pelvic girdle and moved up the body to the cervical area. Using massage techniques, the practitioner focused on release of myofascial tissues, reduction of hypertonicities in muscle groups with origins in the cervical area, and insertions in the shoulder girdle such as levator scapula, sternocleidomastoid, and scalenes. Table 2 outlines the position, techniques, objectives, and rationale used in planning the individualized integrated body treatment. A more specific description of the techniques is reported below.
Table 2
Intervention Physical Techniques
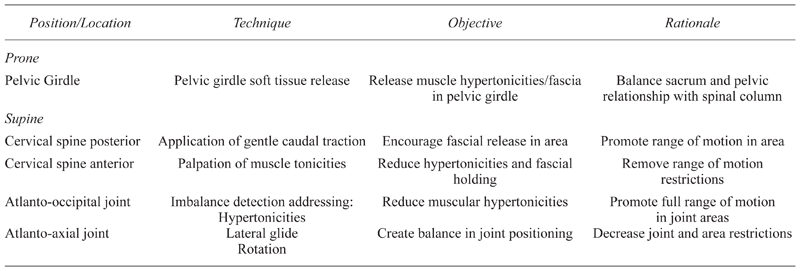
After work on the pelvic girdle was complete, as indicated in Table 2, the muscle groups and fascial tissues surrounding the erector spinae were “warmed” using gentle massage strokes. The shoulder girdle muscle groups with cervical attachments were then massaged using effleurage, petrissage, circular frictions, linear frictions, fascial releases, and tender point releases to reduce hypertonicity to normal tonus.
The patient was then asked to turn so that he lay supine on the table and the focus of the massage techniques moved to the cervical and cranial region. The same massage techniques highlighted above were used to release fascial and muscular tissues, specifically the suboccipital muscle and ligamental attachments. Following this, gentle caudal traction to the spine was provided while cradling the cranium in both hands.
The atlanto-occipital imbalance was addressed at the end of the treatments with experienced palpation (which can detect vertebral transverse processes at C1) serving as an essential component. Bilateral palpation of the transverse processes of the cervical vertebrae was done to note the positional balance, rotation or glide and hypertonicity of attached muscles. The following description outlines the exact process used during the treatments.
The practitioner placed an index finger on either end of the patient’s C1 transverse processes to assess the vertebra’s position symmetry/balance.
From a level position, the practitioner used visual observation on the sagittal plane to assess whether one transverse process was more posterior and one more lateral. In this case, the transverse process was posterior on the right.
The practitioner held with the index finger on the transverse process of the atlas, stabilizing it through the patient’s movement of rotation for a pinning and stretching effect of the attached muscles. Moving slowly and gently, the patient followed the verbal prompt to rotate his head to the right. During this process, the practitioner instructed the patient that he was in charge of his movements and that, if he had any pain or discomfort, he was to stop.
The patient took a deep breath at the end of ROM, held the position for 15 seconds for relaxation, and then slowly returned to forward facing position. Effleurage and gentle friction were then applied with the intention to release contracting muscle and fascia tissues.
To detect lateral glide of the cranium, the practitioner gently provided traction to the cervical area to extend the muscle and fascia. Firmly supporting the head with both hands, keeping traction level, and moving laterally, she asked the patient to contract lateral muscles to assist movement in each lateral direction.
It was observed that one side moved laterally more than the other, and a second pinning and stretching technique toward the more flexible side was used in an effort to reduce hypertonicity. The intention of this step was to encourage cranium and C1 realignment.
Fascial tissue in the posterior and anterior cervical area was addressed with effleurage, petrissage, friction, and fascial release, followed with manual lymphatic drainage in the neck area to conclude the treatments.
The patient reported constant headaches at 8/10 pain level, dizziness, “fuzziness”, tenderness and stiffness in the cervical and cranial areas, and motion sickness with car or boat travel. Severe muscle hypertonicity extended bilaterally in the shoulder girdle, reducing range of motion in the cervical and shoulder joints. These severe muscle hypertonicities presented in both anterior and posterior aspects of the cervical region. BESS results indicated a high level of instability. The patient was unable to perform any elements of the balance testing, even with eyes open. When the patient moved from vertical to horizontal or vice versa, it intensified the vertigo and nausea. Through palpation and visual assessment of the atlanto-occipital area, an imbalance and incongruity in the interrelationship of the C1 and cranium positioning, strength, and balance in supporting structural muscles were observed.
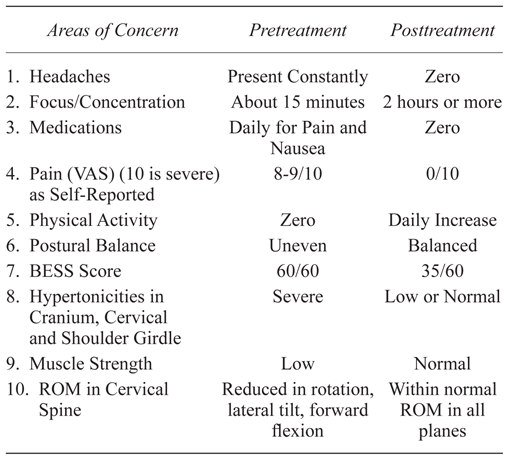
To insure stability and to record the postural balances and tests, the patient returned a week later for a discharge appointment from the postconcussion treatments. The same evaluation as in the initial assessment was used during the follow-up assessment. Table 3 highlights measures of interest at pre- and posttreatment. Briefly, his range of motion, balance, and physical symptoms had all resolved with no adverse events.
Table 3
Pretreatment to Posttreatment Changes
Although no further follow-up visits or assessments were scheduled as part of the treatment plan, additional follow-up was possible due to patient visits to the clinic for other services which afforded communication between the practitioner and patient. During such an encounter one month after the patient’s discharge from care, he reported in person that, after the treatments, he had incrementally returned to his normal student course work load, daily computer use of several sessions of 2 hours apiece each day, and short periods of physical conditioning, including fitness running, swimming, and light weights.
The patient initiated cordial contact again six months later, stopping by the clinic to “check-in,” report his improved status, and thank the therapist. He reported completion of the academic term and his Master’s thesis. In addition, he mentioned that he was able to complete activities of daily living, operating trucks and fishing boats, performing fitness activities of soccer and running, enjoying social activities of viewing movies on screen and playing cards, as well as handling his work on computer screens as he had done prior to the head trauma.
This case study documents a specific massage intervention to address postconcussion treatment and demonstrates the utility of such an approach in restoration of the atlanto-occipital joint to anatomically preferred placement for symptom reduction. An anatomical review of the cervical and cranial brain stem structures(22) highlights the complexity and wide-spread effects of trauma to this area during concussion. The following may also provide insight into the possible underlying mechanisms responsible for the positive outcomes highlighted by this case study. With concussion, even minimal movement out of anatomical position appears to disturb homeostasis, setting up an incongruous positioning between the atlas and the cranium.(18,19) Anatomical consequences may include compression or pinch on a portion of the dural covering of the brain stem, and interference of the neurovascular passages through the area.(18,23) Muscles within the affected area become hypertonic and naturally “cast” to protect the area from further movement and damage.(18)
These dysfunction factors may emerge as concussion symptoms of headache, dizziness, and “fuzziness”. In conjunction with the incongruous relationship between the cranium and atlas, there may be an asymmetrical alignment of the eyes and inner ears, which affects balance and produces symptoms of headache and dizziness, as well as nausea and vomiting. Facilitating return to preferred anatomical form through therapy allows for function restoration. This case study demonstrates a complete return to preconcussion activities and function with no continued symptoms following a short and specific massage series.
There are clinical implications for delivery of this type of intervention in concussion treatment. The techniques used in this case study are not those typically taught in foundational massage and bodywork programs. Rather, advanced massage or manual techniques are needed to learn these treatment mechanics, and can be best found through specialized workshops involving physical manipulation techniques. In addition, experience with head trauma is important and likely best found through medical massage and rehabilitation medicine environments. The complexity and length of care needed to address the biomechanical effects of concussion depend on the trauma’s severity and extent. The location of the impact, head kinematics, as well as age, gender, sport or trauma setting, neck muscle strength and flexibility, are variables that factor into the severity of the concussion.
This case study demonstrates the potential benefits of massage therapy techniques for concussion related symptomology. More specifically, it is the clinical judgment of this bodywork practitioner that massage therapy techniques restored ideal alignment of the atlanto-occipital joint for the patient described. There was a reduction in pain, muscle hypertonicity, headaches, and reduced medication use, as well as improved balance, posture, cervical range of motion, mental focus, and physical activity. The massage therapy approach used in this case study is a reproducible and efficient intervention for practitioners with advanced training in physical manipulation techniques and sensitive palpation skills. The positive findings from this case study provides preliminary evidence for massage therapy techniques to be used as an intervention for concussion-related symptomology, especially in cases of subluxation of the atlanto-occipital joint. The nonpharmacologic treatment approach used in this case study needs further research examination to better determine its effectiveness in meeting the American Academy of Neurology’s call(16) for new interventions to improve postconcussion treatment.
For the ongoing positive support in organizing and composing, my thanks to Cynthia Price, PhD, LMP, Research Associate Professor, University of Washington, Seattle, WA, and IJTMB’s Editor-in-Chief and Practice Section Editor Karen Boulanger, PhD, CMT and Niki Munk, PhD, LMT, respectively. For the mentorship and excellent workshops teaching about balancing the body, my thanks to Paul St. John, LMP, The St. John-Clark Pain Treatment Clinic, Clearwater, FL.
The author declares there are no conflicts of interest.
1 US Dept of Health and Human Services. Centers for Disease Control and Prevention. Get the Stats on Traumatic Brain Injury in the United States. Available from: http://www.cdc.gov/traumaticbraininjury/pdf/BlueBook_factsheet-a.pdf
2 Faul M, Xu L, Wald MM, Coronado VG. Traumatic Brain Injury in the United States: Emergency Department Visits, Hospitalizations and Deaths 2002–2006. Atlanta, GA: Centers for Disease Control and Prevention, National Center for Injury Prevention and Control; 2010.
3 Coronado VG, Xu l, Basavaraju SV, McGuire LC, Wald MM, Faul MD, et al. Surveillance for traumatic brain injury-related deaths – United States, 1997–2007. MMWR Surveill Summ. 2011;60(5):1–32.
4 Kay T, Harrington DE, Adams R, Anderson T, Berrol S, Cicerone K, et al. Definition of mild traumatic brain injury. J Head Trauma Rehabil. 1993:8(3):86–87.
5 Enci Mary Kan, Eng-Ang Ling, Jia Lu. Microenvironment changes in mild traumatic brain injury. Brain Res Bull. 2012;87(4–5):359–372.
6 Finkelstein E, Corso P, Miller T. The Incidence and Economic Burden of Injuries in the United States. New York: Oxford University Press; 2006.
7 Gessell LM, Fields SK, Collins CL, Dick RW, Comstock RD. Concussions among United States high school and collegiate athletes. J Athl Train. 2007;42(2);495–503.
8 McMahon P, Hricik A, Yue JK, Puccio AM, Inoue T, Lingsma HF, et al. Symptomatology and functional outcome in mild traumatic brain injury: results from the prospective TRACK-TBI Study. J Neurotrauma. 2013;31(1):1–8.
9 King EG, Kretzmer TS, Vanderploeg RD, Asmussen SB, Clement VL, Belanger HG. Pilot of a novel intervention for postconcussive symptoms in active duty, veterans, and civilians. Rehabil Psychol. 2013;58(3):272–279.
10 Harch PG. Hyperbaric oxygen therapy benefit in traumatic brain injury (TBI) [Lecture at BIALA New Orleans 2013]. J Neurotrauma. 2013.
11 Page P. Cervicogenic headaches: an evidence-led approach to clinical management. Int J Sports Phys Ther. 2011;6(3):254–266.

12 Thompson WR, Carter R, Rohe B, Duncan RL, Cooper CR. A novel massage therapy technique for management of chronic cervical pain: a case series. Int J Therapeut Massage Bodywork. 2011;4(3):6–12.
13 Noudeh YJ, Vatankhah N, Baradaran HR. Reduction of current migraine headache pain following neck massage and spinal manipulation. Int J Therapeut Massage Bodywork. 2012;5(1):5–13.
14 Willer B, Leddy J. New treatment for post-concussion syndrome pioneered at UB [Electronic version]. Medical News Today. 2006. Accessed 18 Feb 2013. http://www.medicalnewstoday.com/releases/53995.php
15 Chrisman SPD, Rivara FP, Schiff MA, Zhou C, Comstock RD. Risk factors for concussive symptoms 1 week or longer in high school athletes. Brain Inj. 2013;27(1):1–9.
16 Borich MR, Cheung KL, Jones P, Khamova V, Gavrailoff L, Boyd LA, et al. Concussion: current concepts in diagnosis and management. J Neurologic Phys Ther. 2013;37(3):133–137.
17 McCrory P, Meeuwisse W, Aubry M, Cantu R, Dvorak J, Echemendia RJ, et al. Consensus statement on concussion in sport: 4th International Conference on Concussion in Sport held in Zurich, November 2012. Br J Sport Med. 2013;47:250–258.
18 Viano DC, King AI, Melvin JW, Weber K. Injury biomechanics research: an essential element in the prevention of trauma. J Biomech. 1989;22(5):403–417.
19 Unterharnscheidt F, Higgins LS. Pathomorphology of experimental head injury due to rotational acceleration. Acta Neuropath. 1969;12(2):200–204.
20 Balance Error Scoring System [online]. Available from: http://www.carolinashealthcare.org/documents/carolinasrehab/bess_manual_.pdf
21 Bell DR, Guskiewicz KM, Clark MA, Padua DA. Systematic review of the balance error scoring system. Sports Health. 2011;3(3):287295.
22 Giza CC, Kutcher JS, Ashual S, Barth J, Getchius T, Gioia G. Summary of evidence-based guideline update: evaluation and management of concussion in sports. Neurology. 2013;80(24):2250–2257.

23 Viano DC, Casson IR, Pellman EJ. Concussion in professional football: biomechanics of the struck player – part 14. Neurosurgery. 2007;61(2):313–327.
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK , VOLUME 8 , NUMBER 2 , June 2015