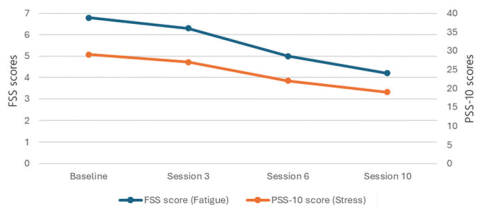
Figure 1 Fatigue Severity Scale (FSS) and Perceived Stress Scale (10-item version; PSS-10) scores across four time points over a 10-week intervention using HeartSpeak Lite for BodyWork.
Anne M. Jensen, MSc, DPhil (PhD)1,2*
1HeartSpeak International, Mackay, QLD, Australia,
2School of Psychology, Deakin University, Warrnambool, VIC, AustraliaFatigue is a multidimensional, subjective experience that can persist despite rest and significantly impair quality of life. While often addressed through physical modalities, fewer manual therapy approaches incorporate emotional processing. This case report describes the use of HeartSpeak Lite for BodyWork, a mindbody technique combining gentle fascial mobilization with guided emotional somatic release, in a client with long-standing fatigue symptoms and stress-related burden. A 52-year-old woman presented with over a decade of persistent fatigue, post-exertional exhaustion, generalized pain, insomnia, and brain fog. She had previously received a diagnosis of chronic fatigue syndrome from her general practitioner in 2019 but had declined pharmacological treatment. Prior use of massage and chiropractic care provided only temporary relief. She sought a natural, integrative option. Over 10 weekly sessions, she received HeartSpeak Lite for BodyWork, which involved structured emotional processing paired with gentle, sustained fascial contact, all delivered in a safety-informed and client-led setting. The client reported progressive improvements in fatigue severity, perceived stress, and daily functioning. Over the 10 weeks, Fatigue Severity Scale scores decreased from 6.8 to 4.2, and Perceived Stress Scale scores improved from 29 to 19. Subjective reports noted greater energy, emotional balance, and increased physical activity tolerance. She also reported feeling safe and supported throughout the intervention, with no adverse effects noted. This case illustrates the potential of a bodywork-based emotional somatic intervention to support individuals with complex fatigue symptoms. While causality cannot be inferred, the observed improvements suggest that gentle, structured, and emotionally attuned approaches may offer benefit by addressing both physical and emotional dimensions of persistent fatigue.
KEYWORDS: Fatigue; stress; psychological; mindbody therapies; emotional regulation; fascia; somatic therapies
Fatigue that persists over time, particularly when not explained by a specific medical condition, often reflects a complex interplay of physiological, emotional, and lifestyle factors.(1) In many cases, stress, unresolved emotional burden, and autonomic dysregulation contribute to fatigue-related symptoms that impact both physical function and emotional well-being.(2,3) Traditional manual therapies such as massage and chiropractic care often provide short-term relief but may not address the underlying emotional or neurological components that perpetuate fatigue.(4)
Recent advances in mindbody approaches highlight the therapeutic value of integrating emotional awareness into body-based treatments.(5,6) Fascia, the body’s connective tissue matrix, is now understood to be richly innervated and involved in interoception, memory storage, and emotional regulation.(7,8) Gentle engagement with fascial tissue, when paired with guided emotional processing, may support downregulation of the nervous system and promote long-term shifts in how stress and fatigue are experienced.(9)
HeartSpeak Lite for BodyWork is a structured emotional somatic technique designed to facilitate the safe and intentional feeling of difficult emotions while gently guiding the body through areas of fascial tension. Unlike many psychological approaches, it does not rely on verbal reflection or analysis. Instead, clients are directed to sense, feel, and process emotional states through the body. This approach may offer a practical, body-informed method for addressing the layered physical and emotional burdens often seen in individuals with long-standing fatigue.
The hypothesized mechanism of change within HeartSpeak Lite for BodyWork involves the activation of implicit emotional memory stored within the fascial system, paired with a supportive context that enables emotional somatic release. Fascia is increasingly seen as a sensory-rich tissue involved in emotional regulation, autonomic function, and interoception.(7,8) When emotional states are accessed and felt fully in the body, particularly in a safe and attuned environment, this may facilitate memory reconsolidation—a process through which emotional responses are updated and integrated.(9) Rather than relying on verbal processing or story retelling, this method emphasizes felt experience and internal awareness as pathways to emotional resolution.
This case report presents the application of HeartSpeak Lite for BodyWork in a client with over a decade of persistent fatigue symptoms. The case explores how a bodywork-based, emotional somatic intervention may support improvements in perceived fatigue, stress, and functional well-being.
HeartSpeak has previously demonstrated potential in addressing chronic pain through emotional somatic release, particularly in movement-based or yoga-informed settings.(10) These findings support further exploration of its use in other stress-related or somatic symptom conditions such as persistent fatigue.
The client was a 52-year-old woman who presented with long-standing fatigue symptoms, generalized musculoskeletal pain, poor sleep quality, and post-exertional exhaustion. She reported experiencing these symptoms for over 15 years, with increasing severity in recent years. In 2019, she had received a diagnosis of chronic fatigue syndrome from her general practitioner; however, no formal diagnostic reassessment or medical testing was conducted as part of this case. At the time of presentation, she was not undergoing any concurrent treatment and had declined pharmacological intervention offered previously. Her history included periodic massage and chiropractic care, which had provided short-term relief, but symptoms would return within 2–3 days. Her goal in seeking care was to find a non-pharmaceutical, sustainable approach to managing her fatigue and associated symptoms.
At baseline, the client reported the following:
Fatigue Severity Scale (FSS): 6.8 out of 7
Perceived Stress Scale (10-item version; PSS-10): 29 out of 40
Common symptoms: brain fog, muscle stiffness, low mood, and difficulty sustaining physical or cognitive activity.
She was living in a high-stress house-hold, caring for a teenage daughter with an eating disorder, while also navigating a strained marital relationship. Although not clinically assessed for depression, the client expressed feelings of helplessness, low motivation, and frustration with her inability to maintain basic routines. She remained functional in daily life but described her quality of life as “barely coping.”
There was no prior therapeutic relationship between the client and the practitioner. Informed consent for treatment and use of anonymized case data was obtained before the intervention commenced. This case was conducted prospectively, with outcomes tracked over the course of the 10-session intervention period. Baseline measures were recorded prior to the first session, and follow-up data were collected immediately after the 10th session.
The client received 10 weekly sessions of HeartSpeak Lite for BodyWork, each lasting approximately 60 min, delivered in a private clinical setting. Sessions were scheduled weekly over a 10-week period. Outcome measures were collected at baseline (prior to the first session) and again after the 10th session. As standardized tools, the FSS (7-item version) and PSS-10 were selected to provide insight into client-perceived changes during this 10-week time frame. While the PSS references the past month, its post-treatment administration was timed to reflect the final 4 weeks of the intervention period. The method integrates gentle fascial mobilization with structured emotional somatic processing, designed to help the client safely access, feel, and process emotional stress through the body. The sessions followed a consistent structure.
Each session began with a brief check-in to identify current areas of physical discomfort or emotional tension. The client was not asked to elaborate on emotional content; instead, the focus was on identifying sensations or reactions present in the body “right now.”
During the main portion of each session, the practitioner invited the client to access a specific emotional feeling (e.g., fear, anger, sadness) using structured verbal cues drawn from the HeartSpeak protocol. Once the client connected with the emotional state and noticed where it was felt in the body, the practitioner applied gentle, non-invasive fascial mobilization to areas of identified tension or restriction (e.g., shoulders, chest, lower back).
Rather than “releasing” fascia in the traditional biomechanical sense, the goal was to facilitate awareness and support the client’s experience of feeling while maintaining gentle contact with the tissue. No sliding, deep pressure, or lubricant was used. The practitioner employed slow, sustained touch—sometimes with subtle directional intention—but avoided any technique that could be interpreted as painful, corrective, or forceful.
The client remained clothed throughout, and verbal interaction during this phase was minimal. Sessions were delivered in silence or with minimal cueing such as “stay with that,” “breathe through it,” or “find what’s here now.”
Each session concluded with quiet grounding and reorientation. The client was encouraged to sense any shifts in the body and to name (without explanation) any qualities that felt more present (e.g., calm, relief, energy). No cognitive interpretation, story retelling, or emotional debrief was included.
Sessions were delivered in a calm, private setting with attention to creating emotional safety. All touch was consented to in advance and described to the client beforehand. The practitioner avoided any painful, invasive, or corrective techniques and maintained gentle, sustained contact only where the client indicated tension. At no point was the client asked to revisit past traumas or discuss distressing events. Instead, she was encouraged to stay present with physical sensations and emotional feelings that arose in the moment. This approach supported the client in remaining within her window of tolerance throughout the intervention.
During each session, the client’s comfort and sense of safety were continuously monitored using both verbal and non-verbal cues. The practitioner checked in periodically with gentle prompts such as “How is this for you?” or “Do you feel okay to continue?” and adjustments were made immediately if any sign of distress or discomfort was noted. The client was explicitly encouraged at the outset—and reminded during sessions—that she could pause or stop the session at any time and that her embodied experience would guide the pace. Post-session check-ins were conducted after each appointment to assess physical and emotional well-being and to ensure that the client left feeling grounded and stable.
At the conclusion of the initial 10-session intervention period, outcome assessments were completed, and this case report was prepared. The client continued with follow-up sessions beyond this initial care block.
Over the course of 10 weekly sessions, the client reported progressive improvements across multiple domains, including fatigue, stress, physical discomfort, and overall well-being. Changes were tracked using standardized self-report measures and subjective feedback.
FSS: Improved from 6.8 (pre-treatment) to 4.2 (post-treatment), indicating a shift from severe to moderate perceived fatigue (Figure 1).
PSS-10: Improved from 29 to 19, reflecting a meaningful reduction in perceived stress (Figure 1).
Subjective Units of Distress Scale: Measured at the beginning and end of each session. Initial scores consistently ranged from 7 to 8 out of 10, while post-session scores dropped to 1 to 2 out of 10, suggesting immediate reductions in emotional and physiological tension following each session.
The client described feeling safe and supported throughout the intervention. Her comment was made spontaneously in the final session and not in response to any direct questioning.
|
| ||
|
Figure 1 Fatigue Severity Scale (FSS) and Perceived Stress Scale (10-item version; PSS-10) scores across four time points over a 10-week intervention using HeartSpeak Lite for BodyWork. | ||
Session 3: Client reported slightly improved energy and clearer thinking (FSS: 6.3; PSS-10: 27).
Session 6: Noted increased mobility, reduced back pain, and greater ability to participate in light activities (FSS: 5.0; PSS-10: 22).
Session 10: Reported significant improvement in energy, mood, and overall function (FSS: 4.2; PSS-10: 19).
The client described feeling “lighter” after sessions, with fewer emotional “crashes.”
She resumed short walks and light housework without feeling depleted.
She reported a greater ability to stay present with emotions rather than shutting down.
Her sleep improved gradually, and she began expressing optimism about her future.
No adverse effects were reported during or after the intervention.
This case illustrates how a bodywork-based, emotional somatic technique may support improvements in perceived fatigue and stress in a client with long-standing symptoms. The structured mindbody approach used in HeartSpeak Lite for BodyWork was associated with meaningful shifts in well-being, as reported by the client and reflected in standardized outcome measures over the 10-week intervention. These included reductions in self-reported fatigue and stress, alongside increased energy, improved sleep, and enhanced emotional resilience.
The most notable changes occurred in the client’s self-reported fatigue severity and perceived stress, as measured by standardized scales. These improvements were accompanied by increased physical activity tolerance and greater subjective well-being. Importantly, these shifts were not attributed to physical manipulation alone, but rather to the combination of feeling guided emotional states while receiving gentle, non-invasive fascial contact.
The fascial system may play a meaningful role in this process. Fascia is increasingly understood as a tissue of interoception—rich in sensory receptors that contribute to emotional regulation, autonomic function, and embodied self-awareness.(7) Furthermore, fascia has been proposed as a potential storage site for long-term implicit memory and unresolved emotional stress.(8) By accessing these felt experiences through the body, clients may engage in a process akin to memory reconsolidation—where outdated emotional responses are accessed and updated within a supportive context.(9) While Heart-Speak Lite for BodyWork does not involve verbal analysis or cognitive reframing, the client in this case appeared to experience therapeutic change through the process of sensing, expressing, and shifting emotional states while receiving gentle physical support. These observed effects align with the hypothesized mechanisms of action underlying this approach.
This case also reinforces that not all bodywork must rely on pressure or mechanical release. The intervention involved light, sustained fascial contact without sliding, oil, or force. The emphasis was not on “correcting” dysfunction, but rather on providing somatic support while the client remained attuned to internal emotional shifts. This model may offer bodyworkers a non-pathologizing, accessible way to engage with clients experiencing persistent fatigue and emotional distress—particularly those who prefer non-verbal or embodied approaches.
As a single case report, these findings cannot be generalized to broader populations. No control condition was used, and placebo effects, practitioner–client rapport, or natural symptom fluctuation may have influenced the outcome. The client’s prior familiarity with bodywork and her openness to mindbody techniques may have also contributed to the positive response. Additionally, all outcome measures were self-reported and not confirmed by medical follow-up.
This case invites further exploration of how manual therapies that incorporate emotional somatic processes may benefit individuals with complex fatigue or stress-related conditions. Controlled trials, larger samples, and objective physiological measures are needed to better understand mechanisms of change. Future research might also explore the feasibility of training bodyworkers in guided emotional facilitation that respects professional boundaries while enhancing client outcomes.
This case illustrates the potential benefit of integrating emotional somatic processing with gentle fascial engagement in a bodywork context. Over 10 weeks, the client experienced meaningful improvements in perceived fatigue, stress, pain, and energy levels. The structured yet non-verbal nature of HeartSpeak Lite for BodyWork allowed the client to access and process emotional tension through physical sensation, without relying on talk therapy. The client reported feeling safe and supported throughout the intervention, with no adverse effects observed. While further research is needed, this approach may offer bodyworkers a practical, embodied method to support clients dealing with persistent fatigue and stress-related symptoms.
The author declares there are no conflicts of interest.
No sources of funding were used in this study.
1. Jason LA, Sunnquist M, Brown A, Evans M, Vernon SD, Furst J, et al. Examining case definition criteria for chronic fatigue syndrome and myalgic encephalomyelitis. Fatigue. 2013;2(1):40–56. https://doi.org/10.1080/21641846.2013.862993
2. Van Houdenhove B, Luyten P. Customizing treatment of chronic fatigue syndrome and fibromyalgia: the role of perpetuating factors. Psychosomatics. 2008;49(6):470–477. https://doi.org/10.1176/appi.psy.49.6.470
Crossref
3. Lakhan SE, Schofield KL. Mindfulness-based therapies in the treatment of somatization disorders: a systematic review and meta-analysis. PLoS One. 2013;8(8):e71834. https://doi.org/10.1371/journal.pone.0071834
Crossref PubMed PMC
4. Li YH, Wang FY, Feng CQ, Yang XF, Sun YH. Massage therapy for fibromyalgia: a systematic review and meta-analysis of randomized controlled trials. PLoS One. 2014;9(2):e89304. https://doi.org/10.1371/journal.pone.0089304
Crossref PubMed PMC
5. Lumley MA, Schubiner H. Emotional awareness and expression therapy: a novel treatment for somatic symptom disorders and medically unexplained symptoms. Psychotherapy. 2019;56(4):460–473.
6. Price CJ, Hooven C. Interoceptive awareness skills for emotion regulation: theory and approach of mindful awareness in body-oriented therapy (MABT). Front Psychol. 2018;9:798. https://doi.org/10.3389/fpsyg.2018.00798
Crossref PubMed PMC
7. Schleip R, Jäger H. Interoception: a new correlate for intricate connections between fascial receptors, emotion, and self recognition. In: Schleip R, Findley TW, Chaitow L, Huijing PA, eds. Fascia: The Tensional Network of the Human Body. 2nd ed. Elsevier; 2021.
8. Tozzi P. Does fascia hold memories? J Bodyw Mov Ther. 2014;18(2):259–265. https://doi.org/10.1016/j.jbmt.2013.11.010
Crossref
9. Winblad NE, Changaris M, Stein PK. Effect of somatic experiencing resiliency-based trauma treatment training on quality of life and psychological health as potential markers of resilience in treating professionals. Front Neurosci. 2018;12:70. https://doi.org/10.3389/fnins.2018.00070
Crossref
10. Jensen AM, Hotek MS. A novel approach to the management of chronic pain using HeartSpeak®, an emotional-somatic release technique, in a yoga context. Ann Yoga Phys Ther. 2023;6(1):1053. https://doi.org/10.26420/annyogaphysther.2023.1053
Corresponding author: Anne M. Jensen, HeartSpeak International, PO Box 242, Mackay, QLD 4740, Australia, E-mail: admin@HeartSpeak.com, Tel: +61 447349951
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
International Journal of Therapeutic Massage and Bodywork, Volume 19, Number 1, March 2026