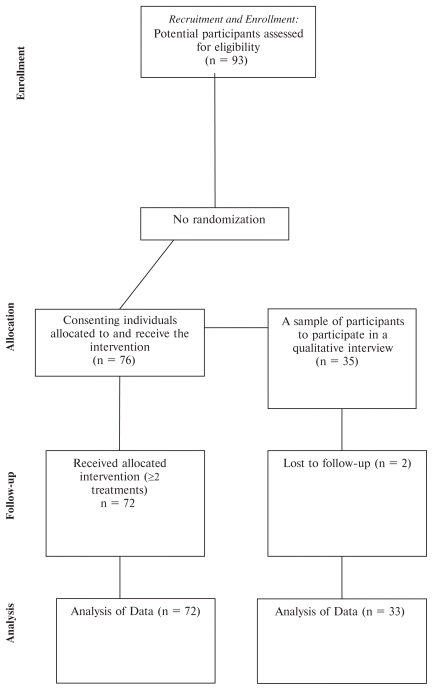
Figure 1 CONSORT diagram for the side effects aspect of the Helping support individuals Pregnant after Experiencing a Stillbirth (HOPES) observational study.
Sarah Fogarty, PhD, MAcup, Dip Remedial Massage,1* Alexander E. P. Heazell, PhD, MBChB, MRCOG,2,3 Niki Munk, PhD, LMT,4,5 Phillipa Hay, PhD, MD, MBChB, FRANZCP, FAED6,7
1School of Medicine, Western Sydney University, Penrith, NSW, Australia,
2Maternal and Fetal Health Research Centre, School of Medical Sciences, University of Manchester, Manchester,
3Department of Obstetrics, Saint Mary’s Hospital, Manchester University NHS Foundation Trust, Manchester, UK,
4School of Health & Human Sciences, Indiana University Indianapolis, Indianapolis, IN, USA,
5Massage Therapy Foundation, Evanston, IL, USA,
6Translational Health Research Institute, Western Sydney University, Penrith, NSW Australia,
7Mental Health Services, South Western Sydney Local Health District (SWSLHD), Campbelltown Hospital, Campbelltown, NSW, AustraliaBackground
Stillbirth is the death, in utero, of a fetus from 20 weeks’ gestation until immediately before birth. This may be spontaneous or can occur after termination for medical reasons (TFMR). The experience of stillbirth profoundly impacts subsequent pregnancies, with mothers frequently experiencing conflicted emotions, heightened anxiety, stress, symptoms of depression, fear, isolation, and a diminished sense of trust in a positive outcome. Supportive care options for individuals pregnant after a stillbirth or TFMR are needed to help meet their psychological and emotional needs. Individuals pregnant after a loss do not feel emotionally safe in their pregnancies; thus, the side effects and perception of safety in support interventions need to be explored.
Purpose
This article reports participants’ experiences of safety, the harms, and adverse events in a study exploring massage as a support for individuals pregnant after a stillbirth.
Methods
The study used questionnaires to collect side effect data and qualitative interviews to examine participants’ experience of safety.
Results
The study found that 75% of participants experienced one or more side effects. Post-massage soreness (45.8%) was the most frequently reported side effect, followed by tiredness (43.1%). The main theme of the qualitative analysis was “safety: so much more than physical safety,” reflecting the importance of safety to study participants and that safety was much more than avoiding physical harm.
Conclusion
Participants needed the massage space to feel safe, both environmentally and psychologically, to facilitate their capacity to engage. Having trained massage therapists was important as this helped reassure participants that massage was a safe treatment for themselves and their baby.
KEYWORDS: Massage therapy; side effects; stillbirth; termination for medical reasons; emotional safety
In Australia, stillbirth is defined as “in utero death from 20 weeks of gestation until immediately before birth”(1–3); approximately six stillbirths occur each day. In Australia, a termination for medical reasons (TFMR) (where parents elect to end a pregnancy due to medical conditions in the fetus or mother) performed at 20 or more weeks of gestation is often recorded as a stillbirth.(4) The experience of stillbirth or TFMR profoundly impacts subsequent pregnancies, with mothers f requently describing the associated stress as something to be “survived.”(5,6) Doyle et al. note that women who had TFMR required mental health support in subsequent pregnancies(7) indicating that individuals who have TFMR have similar needs for psychological support as individuals who experienced a spontaneous loss. Throughout this article, we use the term stillbirth inclusively to refer to parents who have experienced a stillbirth, including those whose loss occurred following a TFMR from 20 weeks’ gestation. The psychological effects of stillbirth on subsequent pregnancies include conflicted emotions, heightened anxiety and stress, symptoms of depression, fear, isolation, and a diminished sense of trust in a positive outcome.(8–13) Additionally, individuals who have experienced stillbirth face increased risks of adverse pregnancy outcomes, such as preterm birth and low birth weight, in subsequent pregnancies.(10,14) The mental health of individuals pregnant after a stillbirth is similarly affected. Research indicates that these individuals are more likely to experience symptoms of post-traumatic stress disorder(15) and exhibit significantly higher rates of depression and anxiety compared to pregnant individuals without a history of stillbirth.(16,17) Standard antenatal care often fails to meet the psychological and emotional needs of individuals pregnant after loss, with many reporting negative experiences, including exacerbated stress and the reactivation of traumatic memories.(12,18) There is a notable lack of specialized antenatal services tailored to the unique needs of individuals pregnant after a stillbirth.(6,12)
In this context of a lack of specialized antenatal services tailored to support the unique needs of individuals pregnant after a stillbirth or TFMR, a research feasibility trial aimed at Helping support individuals Pregnant after Experiencing a Stillbirth (HOPES) was conducted.(19) This trial evaluated the use of individualized Swedish massage as an adjunct approach to care for pregnant individuals with a history of stillbirth, with the goal of assessing its feasibility and potential to improve emotional well-being in this population.(19) Massage therapy, including Swedish and remedial techniques, aimed to support the physiological, structural, and emotional well-being of the mother.(19)
Reporting of harms in randomized clinical trials (i.e., “all important harms or unintended effects in each group”(20)) and in trials in general is an important aspect of ethical conduct in human research.(21) Adverse events and safety are important for individuals pregnant after a loss. Individuals pregnant after a loss do not feel emotionally safe in their pregnancies(22) and individuals mark off the progress of their pregnancy in terms of fetal development and safety.(23) A study involving individuals who had received a massage when pregnant found that safety is made up of not only the treatment that massage therapists provide, but also the environment they provide it in and how they administer both the treatment and the consultation(24) and that the experience of feeling safe, both emotional and physical, was important.(24) There is limited reporting of harms and adverse events in pregnancy massage research studies,(25,26) and the authors could find no massage trial that has reported on harms, adverse events, or experiences of safety for individuals pregnant after a loss. Given the importance of harms, adverse events, and experience of safety for individuals pregnant after a loss, the HOPES feasibility study collected outcome measures related to adverse events and gave participants the opportunity to discuss their experience of safety during the massage(s). This article reports on the HOPES study findings related to harms, adverse events, and experience of safety. The results and findings, including feasibility targets, psychological outcomes, and massage benefits, from the HOPES feasibility study have been published elsewhere.(27)
The HOPES feasibility trial utilized a single-arm, repeated measures, convergent parallel mixed-methods pilot trial design to evaluate the feasibility of Swedish massage as a complementary intervention for pregnant individuals with a prior history of stillbirth. The study ran from February 2023 to July 2024 (see Figure 1). Ninety-three individuals enquired about, or expressed interest in, the study, and 76 individuals enrolled in the study leading to an 84.9% participant conversion rate from interest to enrollment.
|
| ||
|
Figure 1 CONSORT diagram for the side effects aspect of the Helping support individuals Pregnant after Experiencing a Stillbirth (HOPES) observational study. | ||
The study included pregnant individuals who had experienced stillbirth or a TFMR after 20 weeks’ gestation in a prior pregnancy. Participants were recruited through social media platforms and referrals from maternity clinics, shared-care general practitioners, and obstetric clinics located near participating massage therapists across Australia. Recruitment efforts were concentrated in areas proximal to the therapists’ practice locations. Study details were disseminated via obstetric health-care providers and stillbirth support organizations, such as Stillbirth and Neonatal Death Support Australia (SANDS) and Red Nose.
Interested individuals contacted the research team using the provided contact details, and their eligibility was assessed following a clear explanation of the study’s requirements. Participants were given the opportunity to ask questions and deliberate before providing written informed consent. Eligible participants who met the inclusion criteria were then enrolled in the study. Participants were eligible if they were pregnant (under 30 weeks’ gestation), aged 18 or older, had experienced a stillbirth or TFMR from 20 weeks in a previous pregnancy (self-reported), and could attend study massage sessions at an Australian clinic within a 4-month period. Exclusion criteria included scheduling conflicts, lack of access to a nearby study therapist, or inability to travel to sessions. More detailed eligibility criteria are outlined in the published protocol.(19)
Ethics approval was granted by the Western Sydney University Ethics Committee (approval number: H15261). Participants were provided with written information about the study, supplemented by oral explanations if requested. Informed written consent was obtained from all participants prior to their inclusion, ensuring voluntary participation with the right to withdraw at any time.
The primary outcomes for the HOPES trial focused on the feasibility and acceptability of the intervention, as well as identifying optimal timing for massage treatments and collecting measures of anxiety, worry, stress, and self-management. Data were also collected on side effects and adverse events, and this article presents data collected in the HOPES trial related to side effects and experiences of safety.(19) The decision was made to use the term side effect in the participant questionnaire and in publications. Side effects refer to an outcome that occurs as a result of the massage treatment being performed, and we did not specifically clarify that side effects refers to negative consequences. The use of this terminology and not specifically clarifying negative outcomes was selected in preference to terms such as adverse event or harm to avoid unintended implications of danger. This decision reflects the need for sensitivity to the context of our study population while collecting important information about the effects of massage on individuals who are pregnant after a stillbirth.
Side effects questionnaire: Side effect data were collected via a questionnaire. Participants were asked the following question: “Did you experience any side effects from your last massage treatment (e.g., post-massage soreness)?” Participants were then given the following options: (i) no side effects, (ii) post-massage soreness, (iii) headache, (iv) tiredness, (v) other, please specify.(19) This questionnaire was sent 24–28 hours after each massage treatment.(19)
Qualitative data: A subsample of the cohort (n = 33) shared their experiences by interview during the study and thematic analysis was used to analysis participant experiences related to experience of safety.(19) Interviews were conducted after completion of all study treatments, and participants were asked open-ended questions by SF about their experience of safety being part of the massage research study.
The study intervention is detailed in the protocol(19); briefly, it comprised up to five 60-min pregnancy massage sessions using Swedish massage techniques with scheduling tailored to participants’ preferences and availability. Each session was tailored to address the specific needs of the participant on the day of treatment. The intervention was grounded in the vulnerability–stress conceptual framework, which posits that stress can exacerbate individual vulnerabilities, while protective factors mitigate stress.(28) The intervention employed hands-on massage techniques and emphasized active listening and creating a supportive environment to foster a therapeutic alliance. This alliance aimed to introduce protective factors and assist participants in managing the stress of pregnancy following stillbirth. Allowable massage techniques included longitudinal gliding, transverse gliding, digital ischemic pressure, and transverse frictions. These techniques were informed by previous research on pregnancy massage.(16,29) The specific areas treated, depth of pressure, and choice of techniques were guided by the clinical judgment of the massage therapist, mirroring real-world practice.
There were 23 female massage therapists with expertise in pregnancy massage and perinatal loss, across multiple sites in Australia, who were able to provide the study treatments. The average level of experience of the therapists was 9.3 years (standard deviation 5.8 years). The therapists had all undertaken specific pregnancy massage training following their initial qualifications which was a criterion to be part of the study. Eighteen therapists provided 303 massage treatments. All therapists participated in a 3-h online training session in standardizing the intervention delivery.
Given the recruitment methods and study detail dissemination, it is unknown how many people were informed about or viewed the study details. Ninety-three individuals expressed interest in the study, and 76 individuals signed up for the study (see Figure 1). At least one participant came from each Australian state and territory. Participants were predominately from the east coast of Australia (87.5%), with the majority of the study population coming from New South Wales and Victoria (n = 48; 66.7%). Over half of the participants were professionals (n = 39; 54.2%), with managers being the next most common occupation (n = 12; 16.7%). Almost all participants were married or partnered (n = 68; 95.5%). Participants had, on average, three pregnancies and one birth. The majority of participants had a stillbirth (n = 47; 65.2%) followed by TFMR (n = 16; 22.2%). Almost two-thirds were classified as high risk in their current pregnancy (n = 46; 63.9%), almost all participants had had prior experience of massage (n = 69; 95.8%), and over half had prior experience of pregnancy massage (n = 45; 62.5%).
A convergent parallel mixed-methods methodology was utilized for the HOPES study.(19) Although the qualitative and quantitative findings are reported in separate articles, the data on side effects and participants’ experience of safety were not reported in these publications. In the current article, the data on harm or side effects and emotional safety were not compared and related for areas of convergence or divergence and then interpreted. This is due to the importance of the meaning of safe (“safe” means the preservation of value, such as human health and life”(30)) and safety, particularly in the context of a pregnancy after stillbirth or TFMR, as compared to participants’ experience of “feeling emotionally safe.” It is important that these concepts, alongside side effects, are kept separate as this study was not powered, nor designed, to assess safety.
The participant’s demographic and clinical characteristics, as well as the side effect data, were summarized using descriptive statistics. Outcomes did not differ between participants who had early versus late gestation stillbirth or the duration of the interpregnancy interval,(19) so all side effect data were pooled and analyzed collectively.
The in-depth interview data were analyzed using thematic inductive analysis. The author SF immersed themselves in the data to ascertain and identify the key concepts.(31) All authors discussed emerging themes until a consensus was reached. As mentioned in the study protocol,(19) the concept of data saturation and its determination vary significantly depending on the qualitative research approach and the specific saturation model employed.(32–35) Thus, rather than relying solely on data saturation as a determinant for qualitative data collection, the final sample size for this study was guided by the adequacy of the data, its richness, and complexity in addressing the research question.(32)
All authors are parents and researchers. Two of the authors have lived experience of pregnancy after stillbirth or loss (SF and AEPH). SF is a massage therapist who works with parents who have experienced a loss and are pregnant after a loss. AEPH is the clinical lead for a specialist pregnancy after loss clinic in the UK but has no experience of massage therapy in that clinical setting. PH is a psychiatrist with expertise in counseling individuals and families following the experience of a stillbirth and an interest in furthering the understanding of psychotherapeutic modalities that may be more acceptable to individuals during pregnancy, for example, medications. NM is an experienced massage therapist and researcher who works with vulnerable populations.
The trustworthiness of the results and that the findings authentically represented the participants’ perspectives were ensured through member checking.(36) After the initial results were drafted, all participants were invited to review and provide feedback on whether the descriptions and selected quotes accurately reflected their experiences.
Eighteen participants (25%) experienced no side effects after any of their treatments. Of the remaining 54 participants who experienced side effects, 45 (83.3%) experienced one or more treatments with no side effects. Nine participants (16.7%) experienced side effects at each treatment. Participants reported no adverse effects after 158 of the 287 treatments (55.1%).
Of the reported side effects, the most frequent was post-massage soreness, with 33 participants (45.8%) reporting this after one or more of their treatments, totaling 67 incidents among these 33 participants. The next most frequent side effect was tiredness, experienced by 31 participants (43.1%) after one or more of their treatments. There were 59 incidents of tiredness. The third most frequent side effect was headache, experienced by 16 participants (22.2%). There were 21 reports of headache post-treatment across 16 participants. Nineteen participants (26.4%) experienced “other” effects after one or more of their treatments, totaling 29 episodes. The other incidences including both positive and negative effects are listed in Table 1.
Table 1 Other Incidences Reported
A chi-square test of independence was performed to examine the relation between side effects and the treatment visit number, for example, treatment 1 or treatment 2. The relation between these variables was not significant, X2 (1, N = 287) = 6.9; p = 0.142. Individuals were not more likely to experience a side effect from one visit over another (see Table 2).
Table 2 Side Effects by Treatment (n = 287)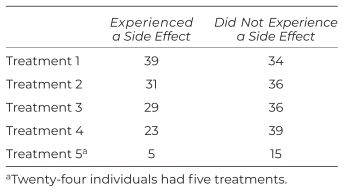
Four people explained their side effects, particularly where the side effect might not have been directly related to the massage. Participant 36 said, “my headache was probably due to lack of water – I’ll drink water during the massage next time,” and participant 08: “I have had post-massage soreness, but I think that is due to pregnancy aches and pains and coming off immune suppressants and steroids.” For participant S31, they felt a “bit emotional in the evening although more related to anniversary of first bubs birth coming up this weekend.” One participant (participant 15) explained that their side effect was positive: “Tiredness was a positive—I had felt tension, but massage allowed me to relax and experience my body’s actual tiredness and willingness to sleep.”
Thirty-three study participants provided qualitative data via interview. Five responded to the request for feedback during the member checking. All reported that the results resonated with their experiences, and no one added anything or asked for changes. No themes emerged that were specific to participants who had early versus late gestation stillbirth or those who had a TFMR compared to those who did not.
Safety is more than physical harm or danger. It is the combination of physical, emotional, environmental, and psychological safety. Safety was important for the study participants; the aspects of massage care that helped them feel safe were feeling secure so they could relax, believing that massage was not a harmful treatment for themselves and their baby, and not experiencing therapists’ reactions that indicated distress when discussing the loss and where the responsibility was not on the participant to “f ix” any distress. The participants also needed the massage space to feel safe, both in terms of the environment and from a psychological perspective. Some participants used the massage as a source of reassurance that helped them navigate pregnancy aches and pains. The subthemes were a safe appointment, the importance of choice and voice, navigating the discomfort, a sense of belonging and inclusion, safety as a precursor, a resource to reassure me, and professional and trained. Analysis revealed a significant crosscutting theme of a non-verbal therapeutic space which refers to the environment created in therapy which is a safe space to express oneself without the need to verbalize everything. This was emphasized by participant 52: “it’s like she doesn’t know me, but somehow, she got it all much more straight away. It’s like she just seems to understand.” Figure 2 presents a visual representation of the interaction of crosscutting themes and subthemes that contribute to the main theme.
|
| ||
|
Figure 2 Representation of safety, the study themes, and how they intersect. | ||
An element of safety for participants was that they could enter a space that would not traumatize them or cause distress. For TFMR participants, massage was perceived as a health-care appointment where they were unlikely to receive “bad” news: “I’ve got medical appointments all to do with the baby and the pregnancy and medical stuff and I always feel like there’s a potential that something could go wrong every time I go to an appointment. There’s going to be no test results [at the massage appointment], there’s going to be no, yeah, nothing that can pop up and confront me at any point. It’s just relaxing” (participant 33).
Entering the same spaces or environments that related to their stillbirth or TFMR was difficult and distressing, and having the location of the massage appointment not in these spaces made the massage feel like a health-care option that they could manage.
“I think that the environment was perfect, like it’s a normal massage clinic, it’s not like you’re going into a hospital, and it’s not like you’re going into a therapist’s office which can provoke anxiety and almost prevent people from attending. Whereas I feel like it’s a much less threatening environment, going into a massage room” (participant 69).
The massage consultation was a healthcare option that did not require detailed information or discussion about how or why the loss occurred, details about the procedures, or discussion of memorial events. Having the stillbirth or TFMR already known before attending the first massage appointment eased participants’ feelings of anxiety as “knowing that the information was already out there meant that it was easier to just say what I had to say or wanted to say or how I was feeling” (participant 66). The freedom to be able to share only what parts of their journey they wanted to share, if any, empowered participants and gave them options and choice.
“Not having to explain my story was really helpful as well, not having to go into it. Everywhere I go, I have to tell people, people ask me questions and I have to go into everything … And it was just nice to be able to go to an appointment and not have to explain that to anyone” (participant 33).
For one TFMR client, the massage space was a safe place to acknowledge the pregnancy prior to the 20-week scans while still having the autonomy to share only what they felt comfortable and not be subjected to multiple questions. “It [the massage] was probably more helpful in a way because nobody knew I was pregnant, and I was unable to really acknowledge the pregnancy or really do too much specifically for it in a safe way because I didn’t have the energy probably to access other certain supports … because I didn’t want to have to tell them that I was early stages of pregnancy and then have to have all of the questions that come with it. And so, I would just avoid those sorts of treatments or those sorts of things regardless of whether or not it might make me feel good” (participant 7). The choice to share and talk was not just about loss but the option to chat or be silent during the massage: “So, I definitely felt like it was a nice safe space and if I could, if I wanted to, I’d know that she would have been there to chat” (participant 50).
An aspect of feeling safe in the massage consultation was about navigating discomfort. For participants experiencing pregnancy after a stillbirth or TFMR, this involved two subthemes: not having to manage other people’s discomfort and able to manage my discomfort.
Not having to manage other people’s discomfort: Participants experiencing pregnancy after a stillbirth or TFMR highlighted the importance of having a space to go where the burden is not placed on the bereaved parent to manage people’s discomfort in response to conversations about pregnancy loss. “It’s [stillbirth] a difficult thing to bring up… There wasn’t awkwardness [at the massage appointment], there wasn’t hesitation, it was just, you know, how are you? And … those kinds of things, that started the conversation that just made it feel very safe” (participant 66).
The negation of the practitioners’ discomfort meant that participants felt comfortable to be themselves and be honest about the stress of being pregnant after a stillbirth or TFMR as evidenced by participant 09 who valued being able to be a mother: “I think that’s what made it feel like such a safe space as well. Like that I wasn’t doing something wrong by speaking about my baby and sharing my experience, that I was simply just talking to someone.”
Able to manage my discomfort: An important aspect of feeling safe was the capacity for participants to be vulnerable and express or display stigmatized emotions such as sadness, anxiety, and dysregulation: “I definitely felt safe there. Even if there was a hair’s breadth of hesitation, that day that I went there after the psychiatrist, like, she just dealt with me so well. I was the most dysregulated I had been in years. I was a mess” (participant 3). Participants felt that they did not need to suppress their emotions in the massage space and that they could experience their emotions while maintaining self-control such as participant 68 who felt the massage space “is I guess a little bit of a gradual space where you can feel things, where it feels safe but it doesn’t necessarily feel like you’re going to unravel and never be able to put yourself back together.”
A sense of acceptance, inclusion, and connection is important to a sense of belonging. A sense of belonging encompasses not only the conversation that occurred at the consultations but also the physical spaces that the participants visited and spent time in. Participants experienced the massage intervention and the physical environment as a place where they could feel like they belonged and where social isolation was reduced: “I definitely felt like I belonged” (participant 31).
An important aspect of participants feeling like they belonged was feeling like the therapists understood the participants’ needs in pregnancy after stillbirth or TFMR and used appropriate conversation and treatment techniques to reinforce this. Participants appreciated that the study therapists understood the physical and psychological impacts of a pregnancy after stillbirth or TFMR, and they found the massage space to be a safe place: “[the massage space] felt like a safe place, someone that understood physically what I might have been going through at that time and … about how I was feeling more from the psychological perspective as well” (participant 61).
Participants who experienced a late stillbirth articulated that it was particularly important to be understood, and this enabled them to feel that they could access care. They felt that when misunderstood, this negatively influenced their decision about accessing massage: “with both my boys [in pregnancies after stillbirth], I kind of treated myself to a massage when I got past 20 weeks. I would have liked to have gone more often, but then, again, you’re weighing up... seeing a therapist who might not necessarily understand” (participant 17).
At times, a single question from a practitioner can convey a lack of understanding and impact a person’s sense of safety, inclusion, and belonging. Participants articulated that avoiding triggering questions and conversations in the massage space was an integral part of feeling like they belonged. Difficult and stressful questions included “is this your first?” which was commonly mentioned by study participants as being difficult: “everyone asks you that question over and over again and it just gets exhausting” (participant 13). Having a space where these difficult questions and conversations did not occur was appreciated by participants: “So, you know, she didn’t ask questions about numbers of children and prior pregnancies and gender and all that stuff that just brings these things up” (participant 6).
There was one instance where a common but difficult question was asked in the study materials and the participant remarked how challenging this was: “The form that you filled in at XXX’s clinic had a question that said, do you have any children? And then the next question was, how old is your child? I found that quite a hard question … I was like, I don’t know how to answer that question. Do I say, yes, I have a child who’s zero?” (participant 13).
Therapists in the study were also able to avoid some of the clichéd platitudes and expressions of excitement and happiness that commonly occur when a pregnancy is shared. Avoiding clichéd responses bypassed the potential anxiety that accompanies these platitudes: “I imagine if I were to book a pregnancy massage, it’s just like, it would just be so like, carefree, and like, you’re pregnant, and isn’t it all amazing? It’s so exciting! Yeah, and …, it just doesn’t fit. You’re just kind of like, yeah, sure, but like none of that applies to me. And these are the kind of things that irritate me” (participant 21).
An environment where it is safe to relax: Feeling safe and comfortable was the foundation needed for participants to be able to relax. For some participants, this was facilitated by the therapist, such as participant 38, who felt her therapist made her very comfortable: “XXX made me very comfortable physically but also in terms of checking in to see if I was okay and letting me know what was going to happen. I felt like I could really trust her and properly relax.” For other participants, it was the massage experience that allowed them to feel safe and switch their brain off: “I don’t turn my brain off because I just can’t. And that is the one time I can switch off and just, it just feels like you’re dreaming but in a nice way and you’re safe and you know you’ve got an hour of not being disturbed and it’s lovely” (participant 33).
Fostering a sense of connection: Safety was also the precursor for fostering a sense of connection. Being able to talk freely, without judgment about their loss and their experience in this pregnancy, created a connection between participants and therapists, decreasing their sense of isolation: “It is particularly important for any kind of support for pregnant individuals, especially after loss, is that it can feel very isolating because you don’t want to talk to many people about how hard pregnancy is or how difficult because people don’t really want to hear that. So, to have a space where you can be honest about how very difficult it is and how unenjoyable it is, is I think part of the therapeutic aspect of it” (participant 67).
Connection was fostered, for some participants, not just with the therapist but with their body and their baby, such as participant 51, who expressed: “to know [the therapist] and connect in a safe and relaxing space, encouraged me to connect to my body and my baby.” This was also the case for participant 61, who was able to feel safe: “feel safe in my body again … because a lot of dissociation happens, I think massage just allows you to feel your body again.”
An unexpected aspect of the massage care provided during the study was the support that massage therapists provided in reassuring participants that their pregnancy musculoskeletal aches and pains were “normal”: “I have found early on, I found some of the pains quite triggering. And a lot of them did feel really similar to around the same time, especially after having a termination for medical reasons. And some of the discomforts in my body in those two days between having his heart stopped and then giving birth, a lot of them were really similar. So having some of the pains and the sensations in my body are quite triggering, but it has helped having, yeah, massage to support my body and knowing that it’s my body and not the baby and having that sort of reaffirming like knowledge I guess or having someone else tell me that you know it’s normal” (participant 9).
Having pregnancy massage-trained therapists providing the study treatments was more important to the stillbirth participants than those who had a TFMR. This was important: “because I guess I’m a bit more cautious in so far as, not that I think anything could go wrong, but it would just alleviate that fear so it wouldn’t be an extra thing that I have to think about on top of everything else” (participant 49).
Participants expressed that the pregnancy massage training alleviated their fears and was an assurance that the massage would not put them or their baby at risk: “because you’re already high risk and you don’t want to risk anything else” (participant 72).
Safety mattered to the study participants, but in this context, it was described much more than physical safety. Participants’ experience of emotional safety facilitated numerous aspects of the research study and their positive experiences of massage, as they felt able to relax and attend appointments as therapists were understanding and non-judgmental. Having trained massage therapists was important as this helped reassure participants that massage was a safe treatment for themselves and their baby. Participants needed the massage space to feel safe both in terms of the environment and psychologically.
The role of the massage therapist in the experience of individuals pregnant after a stillbirth or TRFM feeling safe was an important aspect of the support offered in the massage consultation. Reassurance as part of psychological supportive health care has not been extensively explored as part of massage care; however, it has been studied more extensively in nursing.(37) Reassurance as part of health care requires health-care providers to “demonstrate self-awareness and emotional connectedness and apply verbal and non-verbal techniques to help restore confidence and empower patients.”(37) Our study findings demonstrate that reassurance, as described above, was an important aspect of study participants’ experience of safety mediated by emotional connectedness, compassion, and capacity for participants to be honest and empathetic. Professional competence and verbal forms of reassurance, particularly around “normal” pregnancy aches and pains, were also important. The use of reassurance as part of massage care is difficult to teach, replicate, and/or standardize in clinical care and research studies, because it involves non-verbal and verbal interactions that are often complex and situational, and it can be difficult to express or record as aspects of care. Indeed, what might be perceived as reassuring for one client group such as individuals pregnant after a stillbirth or TFMR may not be reassuring for other client groups. Nevertheless, one way to increase knowledge of reassurance in massage care is to document massage therapists’ experience of providing reassurance, particularly for different client groups, so that common themes and important aspects of reassurance can be identified.
Having an emotionally safe support option was important to the participants in the study. Individuals pregnant after a loss have reported feeling a lack of support from others, fear of bad news, and worries never end.(38) Care provision that includes support by skilled and familiar care teams knowledgeable about the pervasive impact of stillbirth on the subsequent pregnancy and beyond(39) has been identified as critical, and our findings support these critical and important aspects, in particular, the perception of emotional safety. Where possible, all supportive care provided to individuals pregnant after a stillbirth or TFMR needs to ensure that the environment in which the care is provided and the care itself do not exacerbate existing concerns, anxieties, worries, and fears.(40) Care that intensifies individuals’ concerns, worries, anxieties, and fears and a lack of understanding about the pervasive impact of stillbirth can be barriers for accessing and continuing supportive care. Feeling emotionally safe was associated with the removal of barriers to receiving supportive care and allowed individuals to access services in a place where they felt like they belonged. Feeling isolated has been reported by individuals pregnant after a stillbirth,(41,42) and having a place where individuals can be themselves, feel safe to be vulnerable and themselves, and create connections is an important aspect of supportive care, potentially decreasing the isolation individuals feel.(43) Individuals pregnant after a loss seek health-care options and social support to help manage and cope with pregnancy after a loss,(43,44) and our findings indicate that massage might be a support that provides a sense of connection which could decrease isolation and help individuals pregnant after a stillbirth or TFMR.
The reporting of adverse events or harms in pregnancy massage research studies is limited.(25,26) The Mueller and Grunwald systematic review on pregnancy massage found that only two studies reported adverse events. One study had two adverse events reported (exacerbation of anxiety and tiredness),(45) and the other study found 2% (n = 48) of individuals reported side effects (tiredness after treatment).(46) All of the included papers in the review either excluded individuals with pregnancies or preexisting physical complications (i.e., placenta previa, premature labor, blood clotting disorders, or diabetes)(25) or did not report whether the individuals had any known preexisting conditions. These low levels of adverse events is in stark contrast to an observational study that found 40% of individuals receiving massage in a clinical setting (n = 32) experienced one or more post-massage side effects.(26) The two most common side effects experienced in the observational study were post-massage soreness (n = 30) and tiredness (n = 7).(26) Our study found 75% of participants experienced one or more side effects, with post-massage soreness (45.8%) and tiredness (43.1%) being the two most common side effects. The intensity or severity of the side effects was not measured, so it is unclear what the severity of these side effects was, or whether they were viewed by participants positively or negatively. Individuals who are pregnant after a stillbirth or TFMR can experience a hyperawareness of their physical body and any changes or sensations in their body(8,23) which might make them more aware of any massage side effects.
Given the frequency of reported side effects in our study, future studies should look at collecting data about the intensity or severity of side effects from massage in a population of pregnant after loss. While this study collected data on the area of the body treated and area(s) of focus for the session, data were not collected on how long a therapist spent on each area of the body or which techniques were used on what parts of the body. Collecting this information would allow an analysis to determine if there was an association between the area of the body treated, the choice of techniques, and side effects. Ethnicity and country of birth were not collected as part of the demographic information as this is not usual in Australia; however, the country of birth should be included to future research to determine if ethnicity or country is a factor in the experience of safety.
The study was not intended to provide a complete view of maternal or fetal “safety” of massage, which would require a much larger sample size and different research methodology. This article should not be interpreted as making any conclusions or statements about the safety of massage for individuals pregnant after a loss, but rather as identifying facets of safety that were important to participants of this feasibility study. The study methodology and massage treatment aligns closely to real-world clinical practice which enhances applicability and relevance for replication of findings in clinical practice, in particular it provides information for participants of future studies about likely side effects. However, the sample of participants was not heterogeneous which may impact the generalizability of the findings, and the contributions of massage may not be applicable to all individuals pregnant after a stillbirth or TFMR. Due to the use of social media in recruitment, we were unable to determine how many women viewed the study advertisement. As a result, we could not calculate the proportion of those exposed to the study information, and this limits knowledge about recruitment efficiency and potential barriers to participation.
Safety and side effects are important aspects of research and research outcomes. Minor side effects were experienced by three-quarters of the study population. Safety mattered to the study participants and was much more than physical safety, encompassing emotional and environmental elements. Participants needed the massage space to feel safe, both environmentally and psychologically, and this facilitated participants’ capacity to engage in supportive adjunct health care. Therapists’ understanding and knowledge about the difficulties experienced in a pregnancy after a stillbirth or TFMR were key factors in creating a safe therapeutic space.
Thank you to all the participants in the study. This study was not possible without the participants who shared their pregnancy after loss journey with the researchers. It was also not possible without the support of many community loss organizations who kindly shared details about this study. Thank you to the Massage Therapy Foundation for their financial and administrative support in making this study possible.
SF is a practicing massage therapist. NM is a full-time academic, long-time consultant, and mentor to SF, who receives no financial compensation for her effort on this work and is the Research Director of the Massage Therapy Foundation. It is not expected that the study findings will yield any financial gain for SF or NM. NM’s role at the Massage Therapy Foundation has no bearing on the study implementation or results. PH has received sessional and lecture fees from the Australian Medical Council, Therapeutic Guidelines publication, and New South Wales Institute of Psychiatry and royalties from Hogrefe and Huber, McGraw Hill Education, and Blackwell Scientific Publications, and she has received research support from CAPES, NHMRC, and ARC. She is the Chair of the National Eating Disorders Collaboration in Australia (2019–current). She has been a consultant for Tryptamine Therapeutics Pharmaceuticals.
The study is funded by the 2022 Research Support Grant from the Massage Therapy Foundation awarded to SF. The funders had no role in the design of this trial and will not have any role during its execution, analyses, data interpretation, or decision to submit results.
SF, PH, NM, and AEPH contributed to all phases of the protocol writing (initial idea, research question, design and assessments). SF completed ethics proposal and amendments. SF and NM developed the massage treatment protocol. All authors read and approved the final manuscript.
1. Australian Government. Mothers & Babies. Accessed February 7, 2018. https://www.aihw.gov.au/reports-statistics/population-groups/mothersbabies/about
2. Australian Government. Australia’s Mothers and Babies. Accessed November 15, 2020. https://www.aihw.gov.au/reports/mothers-babies/australias-mothers-babies/contents/stillbirths-neonatal-deaths/stillbirths-and-neonatal-deaths-in-australia
3. PWC. The economic impacts of stillbirth in Australia. 2016. https://stillbirthfoundation.org.au/wp-content/uploads/2020/08/Economic-Impacts-of-Stillbirth-2016-PwC.pdf
4. Australian Government. Australia’s Mothers and Babies. Data source: National Perinatal Mortality Data Collection. Updated May 14, 2025. Accessed July 3, 2025 https://www.aihw.gov.au/reports/mothers-babies/australias-mothers-babies/contents/technical-notes/data-quality-andavailability#Definitions
5. Gower S, Luddington J, Khosa D, Thaivalappil A, Papadopoulos A. Subsequent pregnancy after stillbirth: a qualitative narrative analysis of Canadian families’ experiences. BMC Pregnancy Childbirth. 2023;23(1):208. https://doi.org/10.1186/s12884-023-05533-5
Crossref PubMed PMC
6. Mills TA, Roberts SA, Camacho E, Heazell AEP, Massey RN, Melvin C, et al. Better maternity care pathways in pregnancies after stillbirth or neonatal death: a feasibility study. BMC Pregnancy Childbirth. 2022;22(1):634. https://doi.org/10.1186/s12884-022-04925-3
Crossref PubMed PMC
7. Doyle C, Che M, Lu Z, Roesler M, Larsen K, Williams LA. Women’s desires for mental health support following a pregnancy loss, termination of pregnancy for medical reasons, or abortion: a report from the STRONG Women Study. Gen Hosp Psychiatry. 2023;84:149–157. https://doi.org/10.1016/j.genhosppsych.2023.07.002
Crossref PubMed
8. Côté-Arsenault D. Threat appraisal, coping, and emotions across pregnancy subsequent to perinatal loss. Nurs Res. 2007;56(2):108–116. https://doi.org/10.1097/01.Nnr.0000263970.08878.87
Crossref PubMed
9. Cacciatore J. Psychological effects of stillbirth. Semin Fetal Neonatal Med. 2013;18(2):76–82. https://doi.org/10.1016/j.siny.2012.09.001
Crossref
10. Ellis A, Chebsey C, Storey C, Bradley S, Jackson S, Flenady V, et al. Systematic review to understand and improve care after stillbirth: a review of parents’ and healthcare professionals’ experiences. BMC Pregnancy Childbirth. 2016;16:16. https://doi.org/10.1186/s12884-016-0806-2
Crossref
11. Meaney S, Everard CM, Gallagher S, O’Donoghue K. Parents’ concerns about future pregnancy after stillbirth: a qualitative study. Health Expect. 2017;20(4):555–562. https://doi.org/10.1111/hex.12480
Crossref PMC
12. Mills TA, Ricklesford C, Cooke A, Heazell AE, Whitworth M, Lavender T. Parents’ experiences and expectations of care in pregnancy after stillbirth or neonatal death: a metasynthesis. BJOG. 2014;121(8):943–950. https://doi.org/10.1111/1471-0528.12656
Crossref PubMed
13. Thomas S, Stephens L, Mills TA, Hughes C, Kerby A, Smith DM, et al. Measures of anxiety, depression and stress in the antenatal and perinatal period following a stillbirth or neonatal death: a multicentre cohort study. BMC Pregnancy Childbirth. 2021;21(1):818. https://doi.org/10.1186/s12884-021-04289-0
Crossref PubMed PMC
14. Wojcieszek AM, Shepherd E, Middleton P, Lassi ZS, Wilson T, Murphy MM, et al. Care prior to and during subsequent pregnancies following stillbirth for improving outcomes. Cochrane Database Syst Rev. 2018;12(12):CD012203. https://doi.org/10.1002/14651858.CD012203.pub2
PubMed PMC
15. Turton P, Hughes P, Evans CD, Fainman D. Incidence, correlates and predictors of post-traumatic stress disorder in the pregnancy after stillbirth. Br J Psychiatry. 2001;178:556–560. https://doi.org/10.1192/bjp.178.6.556
Crossref PubMed
16. Gravensteen IK, Jacobsen E-M, Sandset PM, Helgadottir LB, Rådestad I, Sandvik L, et al. Anxiety, depression and relationship satisfaction in the pregnancy following stillbirth and after the birth of a live-born baby: a prospective study. BMC Pregnancy Childbirth. 2018;18(1):41. https://doi.org/10.1186/s12884-018-1666-8
Crossref PubMed PMC
17. Hughes PM, Turton P, Evans CD. Stillbirth as risk factor for depression and anxiety in the subsequent pregnancy: cohort study. BMJ. 1999;318(7200):1721– 1724. https://doi.org/10.1136/bmj.318.7200.1721
Crossref PubMed PMC
18. Ladhani NNN, Fockler ME, Stephens L, Barrett JFR, Heazell AEP. No. 369 - Management of pregnancy subsequent to stillbirth. J Obstet Gynaecol Can. 2018;40(12):1669–1683. https://doi.org/10.1016/j.jogc.2018.07.002
Crossref PubMed
19. Fogarty S, Heazell AEP, Munk N, Hay P. Swedish massage as an adjunct approach to Help suppOrt individuals Pregnant after Experiencing a prior Stillbirth (HOPES): a convergent parallel mixed-methods single-arm feasibility trial protocol. Pilot Feasibility Stud. 2024;10(1):67. https://doi.org/10.1186/s40814-024-01499-z
Crossref PubMed PMC
20. Junqueira DR, Zorzela L, Golder S, Loke Y, Gagnier JJ, Julious SA, et al. CONSORT Harms 2022 statement, explanation, and elaboration: updated guideline for the reporting of harms in randomized trials. J Clin Epidemiol. 2023;158:149–165. https://doi.org/10.1016/j.jclinepi.2023.04.005
Crossref PubMed
21. National Health and Medical Research Council. National Statement on Ethical Conduct in Human Research. 2023.
22. Côté-Arsenault D, Morrison-Beedy D. Women’s voices reflecting changed expectations for pregnancy after perinatal loss. J Nurs Scholarsh. 2001;33(3):239–244. https://doi.org/10.1111/j.1547-5069.2001.00239.x
Crossref
23. Côte-Arsenault D, Mahlangu N. Impact of perinatal loss on the subsequent pregnancy and self: women’s experiences. J Obstet Gynecol Neonatal Nurs. 1999;28(3):274–282. https://doi.org/10.1111/j.1552-6909.1999.tb01992.x
Crossref PubMed
24. Fogarty S, Barnett R, Hay P. Safety and pregnancy massage: a qualitative thematic analysis. Int J Ther Massage Bodywork. 2020;13(1):4–12.
Crossref PubMed PMC
25. Mueller SM, Grunwald M. Effects, side effects and contraindications of relaxation massage during pregnancy: a systematic review of randomized controlled trials. J Clin Med. 2021;10(16):3485. https://doi.org/10.3390/jcm10163485
Crossref PubMed PMC
26. Fogarty S, McInerney C, Stuart C, Hay P. The side effects and mother or child related physical harm from massage during pregnancy and the postpartum period: an observational study. Complement Ther Med. 2019;42:89–94. https://doi.org/10.1016/j.ctim.2018.11.002
Crossref PubMed
27. Fogarty S, Heazell AEP, Munk N, Hay P. Swedish massage as an adjunct approach to Help suppOrt individuals Pregnant after Experiencing a prior Stillbirth (HOPES): feasibility and acceptability findings from a convergent parallel mixed-methods single-arm trial. BMC Complement Med Ther. 2026. https://doi.org/10.1186/s12906-026-05244-2
Crossref PubMed PMC
28. Gois C, Dias VV, Raposo JF, do Carmo I, Barbosa A. Vulnerability to stress, anxiety and depressive symptoms and metabolic control in type 2 diabetes. BMC Res Notes. 2012;5:271. https://doi.org/10.1186/1756-0500-5-271
Crossref PubMed PMC
29. Burden C, Bradley S, Storey C, Ellis A, Heazell AE, Downe S, et al. From grief, guilt pain and stigma to hope and pride – a systematic review and meta-analysis of mixed-method research of the psychosocial impact of stillbirth. BMC Pregnancy Childbirth. 2016;16(1):9. https://doi.org/10.1186/s12884-016-0800-8
Crossref
30. Vandeskog B. Safety is the preservation of value. J Saf Res. 2024;89:105–115. https://doi.org/10.1016/j.jsr.2024.02.004
Crossref
31. Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101. https://doi.org/10.1191/1478088706qp063oa
Crossref
32. Braun V, Clarke V. To saturate or not to saturate? Questioning data saturation as a useful concept for thematic analysis and sample-size rationales. Qual Res Sport Exerc Health. 2021;13(2):201–216. https://doi.org/10.1080/2159676X.2019.1704846
Crossref
33. Fofana F, Bazeley P, Regnault A. Applying a mixed methods design to test saturation for qualitative data in health outcomes research. PLoS One. 2020;15(6):e0234898. https://doi.org/10.1371/journal.pone.0234898
Crossref PubMed PMC
34. Malterud K, Siersma VD, Guassora AD. Sample size in qualitative interview studies: guided by information power. Qual Health Res. 2016;26(13):1753–1760. https://doi.org/10.1177/1049732315617444
Crossref
35. Saunders B, Sim J, Kingstone T, Baker S, Waterfield J, Bartlam B, et al. Saturation in qualitative research: exploring its conceptualization and operationalization. Qual Quant. 2018;52(4):1893–1907. https://doi.org/10.1007/s11135-017-0574-8
Crossref PubMed PMC
36. Creswell JW. Research Design: Qualitative, Quantitative, and Mixed Methods Approaches. 4th ed. Sage; 2014.
37. Akyirem S, Salifu Y, Bayuo J, Duodu PA, Bossman IF, Abboah-Offei M. An integrative review of the use of the concept of reassurance in clinical practice. Nurs Open. 2022;9(3):1515–1535. https://doi.org/10.1002/nop2.1102
Crossref PubMed PMC
38. DeBackere KJ, Hill PD, Kavanaugh KL. The parental experience of pregnancy after perinatal loss. J Obstet Gynecol Neonatal Nurs. 2008;37(5):525–537. https://doi.org/10.1111/j.1552-6909.2008.00275.x
Crossref PubMed PMC
39. Heazell AEP, Barron R, Fockler ME. Care in pregnancy after stillbirth. Semin Perinatol. 2024;48(1):151872. https://doi.org/10.1016/j.semperi.2023.151872
Crossref
40. Côté-Arsenault D, Schwartz K, Krowchuk H, McCoy TP. Evidence-based intervention with women pregnant after perinatal loss. MCN Am J Matern Child Nurs. 2014;39(3):177–186.
Crossref PubMed
41. Phelan L. Experiences of pregnancy following stillbirth: a phenomenological inquiry. Can J Couns Psychother. 2020;54(2):150–171.
42. Smith DM, Thomas S, Stephens L, Mills TA, Hughes C, Beaumont J, et al. Women’s experiences of a pregnancy whilst attending a specialist antenatal service for pregnancies after stillbirth or neonatal death: a qualitative interview study. J Psychosom Obstet Gynaecol. 2022;43(4):557–562. https://doi.org/10.1080/0167482x.2022.2098712
Crossref PubMed
43. Hutti MH, Armstrong DS, Myers J. Healthcare utilization in the pregnancy following a perinatal loss. MCN Am J Matern Child Nurs. 2011;36(2):104–111. https://doi.org/10.1097/NMC.0b013e3182057335
Crossref PubMed
44. Camacho Ávila M, Fernández Medina IM, Jiménez-López FR, Granero-Molina J, Hernández-Padilla JM, Hernández Sánchez E, et al. Parents’ experiences about support following stillbirth and neonatal death. Adv Neonatal Care. 2020;20(2):151–160. https://doi.org/10.1097/anc.0000000000000703
Crossref PubMed
45. Hall H, Munk N, Carr B, Fogarty S, Cant R, Holton S, et al. Maternal mental health and partner-delivered massage: a pilot study. Women Birth. 2021;34(3):e237–e247. https://doi.org/10.1016/j.wombi.2020.05.003
Crossref
46. Manber R, Schnyer RN, Lyell D, Chambers AS, Caughey AB, Druzin M, et al. Acupuncture for depression during pregnancy: a randomized controlled trial. Obstet Gynecol. 2010;115(3):511–520. https://doi.org/10.1097/AOG.0b013e3181cc0816
Crossref PubMed
Corresponding author: Sarah Fogarty, Western Sydney University, Locked Bag 1797, Penrith, NSW 2751, Australia, E-mail: s.fogarty@westernsydney.edu.au
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
International Journal of Therapeutic Massage and Bodywork, Volume 19, Number 1, March 2026