
Sarah Fogarty, PhD, M.Acup, Grad. Cert. Domestic Violence, Dip. Remedial Massage,1* Ronna Moore, Dip. Teaching, Dip. Remedial Massage, Grad. Cert. Palliative Care, DrPH Candidate,2 Cal Cates, BA3
1School of Medicine, Western Sydney University, Campbelltown, Australia,
2School of Psychology and Public Health, La Trobe University, Bundoora, Australia,
3Healwell, Arlington, VA, USABackground
Serious illness “is a health condition that carries a high risk of mortality and either negatively impacts a person’s daily function or quality of life or excessively strains their caregivers.”
Purpose
The aim of this review was to explore the contribution of massage and massage therapy to the mental health and well-being of individuals living with a serious and potentially life-limiting illness.
Methods
A scoping review was conducted following Arksey and O’Malley’s six-step scoping review framework and the PRISMA-ScR guidelines. The electronic databases PubMed, CINAHL, MEDLINE (OVID), PsychINFO, CENTRAL, Web of Science, PROQUEST Dissertations and Theses, and Scopus were searched to identify qualitative or mixed-methods studies. The qualitative data were coded from the studies and themes emerged. For the final stage of analysis, a thematic synthesis was utilized.
Findings
Sixteen papers were included from eight countries. The overarching theme was “the effable and ineffable impacts of massage” informed by the following themes: massage as a transcendent experience, existential respite, massage helping to preserve dignity, increased inner resources, well-being and relaxation as part of the individualized and personalized vocabulary for massage for the seriously ill, and varied outcomes of the effect of massage on physical symptoms.
Conclusion
Good mental health and well-being are important aspects of living well with serious illness. The review found there is a considerable body of research which points to the value and impact of massage on outcomes of well-being and mental health and, broadly, on patient experience.
KEYWORDS: Massage; serious illness; mental health; well-being; massage therapy palliative; coping; relaxation; comfort
An estimated 129 million people in the United States have at least one major chronic disease(1) (e.g., heart disease, cancer, diabetes, obesity, hypertension) as defined by the US Department of Health and Human Services. A situation reverberating around the world, the prevalence of serious chronic illnesses constitutes a profound burden of care.(2) Rather than curative treatment, care for such conditions is typically aimed at effective symptom management, maintenance of autonomy, planning for eventual decline, and providing necessary support to maximize multidimensional well-being.(3–5)
The burden of symptoms and other issues associated with serious and potentially life-limiting illness is known to result in decreased quality of life and poorer outcomes.(6–8) Most research about massage in this population tends to focus on patient reporting and rating of symptoms such as pain, anxiety, nausea, and fatigue. While a variety of tools have been developed in recent years to more accurately measure the impact of health-care interventions on quality of life and well-being, there has been minimal interrogation of patient experiences arising from combined physical and psychosocial interventions like massage.(9,10) This signifies a gap in research and outcome measures that address what it means to individuals to receive massage in the context of having a serious illness.(11) We hypothesize that the experience and impact of massage is much broader, more nuanced, and more complex than that captured by the typically applied symptom assessment tools.
It is understood that good mental health and well-being are important aspects of living well with serious illness and that patients’ and families’ ability to achieve and maintain these states is supported by a wide variety of factors.(12,13) Despite growing recognition and evidence of massage therapy’s potential benefits for individuals with serious physical illness, existing research remains fragmented, with a predominant focus on physiological outcomes or quantitative outcomes and there is limited exploration of massage’s impact on mental health and overall well-being. A qualitative scoping review is needed to synthesize the lived experiences, perceptions, and nuanced therapeutic effects of massage in this population, addressing a critical gap in understanding how massage supports holistic well-being beyond clinical measures. By mapping the existing qualitative and mixed-methods research about massage and massage therapy in the setting of serious and potentially life-limiting illness, the goal of this review was to surface data that might demonstrate measurable beneficial impacts of massage on the mental health and well-being of individuals living with serious illness, and thus serve to support its role as a valuable health-care partner.
A scoping review identifies and maps the available evidence about a particular topic and specific populations.(14) This scoping review aimed to explore the contribution of massage and massage therapy to the mental health of individuals living with a serious and potentially life-limiting illness.
The study design was informed by the PRISMA-ScR guidelines(15) and the five-stage process for a scoping review design as outlined by Arksey and O’Malley (2005)(14) and further developed Levac et al.(16) to (i) identify the research question; (ii) identify relevant studies; (iii) study selection; (iv) chart the data; and (v) collate, summarize, and report results. The authors used the Covidence software tool (Veritas Health Innovation Ltd, Melbourne, Australia)(17) for screening and data extraction.
Massage and massage therapy were defined as listed in Box 1 and have been delineated based on the difference between massage from a trained or from a non-trained massage therapist taking into account the capacity for the skills of the massage provider, both in terms of massage techniques and non-hands-on skills, to impact the experience of the intervention. Herein, the term massage will encompass both massage and massage therapy.
Box 1. Definitions of Terms Used in This Paper

The included papers had to use a qualitative or mixed-methods design with a strong qualitative component and be a thesis or published in a peer-reviewed journal.
The people receiving the massage intervention had to have a serious and potentially life-limiting physical illness as per the definition listed above. Massage treatment could be administered at any timeframe along the spectrum of care.
Massage and massage therapy were defined as listed above and have been delineated separately based on the difference between massage from a trained individual and the capacity for the skills of the massage provider both in terms of massage techniques and non-hands-on skills. Throughout the paper the term massage will encompass both massage and massage therapy.
Massage had to be singularly applied or, if it was applied as part of a group of interventions, the massage findings had to be distinguishable from the other therapies.
Papers and/or theses published in the past 20 years in English from January 2004 onwards were included.
Papers reporting other bodywork techniques or therapies that are sometimes under the canopy of massage such as manual lymphatic drainage, Reiki, craniosacral therapy, reflexology, aromatherapy, dry needling, and or acupressure were excluded. Papers investigating massage therapy for those with a serious mental illness were excluded. Papers specifically focusing on the physical health of those with a serious physical illness were excluded.
Other sources of gray literature such as reports, white papers, and government documents were excluded.
Electronic databases including PubMed, CINAHL, MEDLINE (OVID), PsychINFO, CENTRAL, Web of Science, PROQUEST Dissertations and Theses, and Scopus were searched to identify studies potentially eligible for inclusion based on pre-determined criteria. The search strategy included the Boolean terms “OR”/“AND,” and Medical Subject Headings (MeSH). This search strategy used varied combinations of search terms and MeSH terms that were unique to each database. Keywords and their synonyms were combined (massage OR myotherapy OR soft-tissue therapy OR muscle therapy) AND (wellbeing OR mental health) AND (qualitative OR mixed methods). The reference lists of all papers that met the inclusion criteria and any reviews were scanned to identify further relevant studies.
All authors screened all titles and abstracts for inclusion in the study. Following this preliminary screening, the full-text papers were obtained and assessed independently by two authors (SF, CC or RM) for eligibility. Whoever had not completed the screening was available to resolve any disagreements regarding inclusion (see Figure 1). All studies eligible for the review had data extracted by one of the authors and were checked by a different author. A qualitative assessment was undertaken using the JBI qualitative Checklist.(26)
|
| ||
|
Figure 1 PRISMA flow chart for an exploration of the contributions of massage therapy to the mental health of individuals living with a serious and potentially life-limiting physical illness: a scoping review. | ||
All authors identified common descriptions, statements, and concepts that were notable in revealing how massage contributed to the mental health of individuals living with a serious and potentially life-limiting illness. The analysis sought common consensuses and divergences in data alongside explicating the entire context of the data.(27) An interpretation of findings, ledby Braun and Clarke,(28) was achieved by making sense of how massage contributed to the mental health of individuals living with a serious and potentially lifelimiting physical illness through constant engagement with the data leading to the formulation of major themes and subthemes.(28)
Given the interpretive nature of this scoping review, it was important that, as a team, the authors were cognizant of their lived experiences and how these may influence the analysis. Author SF is a massage therapist and researcher who has limited experience working with clients with serious physical illnesses. Author CC is a researcher and former massage therapist whose career in both research and practice has focused almost exclusively on people affected by serious illness. Author RM is a massage therapist and graduate researcher who has extensive experience working with clients with serious physical illnesses.
An initial search from May 1, 2024 to June 18, 2024 found 2,567 articles (see Figure 1). After screening and excluding papers, a total of 16 papers were included.(21–24,29–40) (see Appendix Table S1 and Table 1).
Table 1 The JBI QARI Critical Appraisal Checklist for Interpretive and Critical Research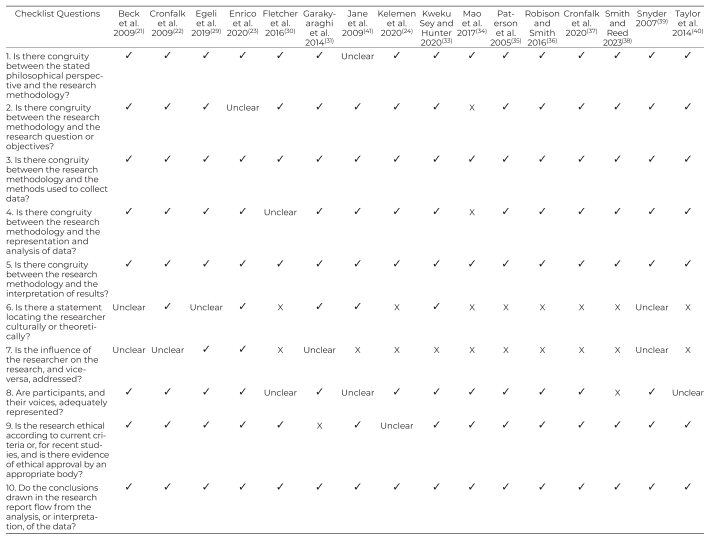
There was a cumulative total of 606 individuals with a serious physical illness who received massage as part of their health care. Seven studies were undertaken in the United States,(24,30,34,36,38–40) three in Sweden,(21,22,37) and one in Canada,(29) Italy,(23) Iran,(31) Taiwan,(32) Australia,(33) and the United Kingdom.(35) Participants in the studies ranged from 40 to 82 years(21–23,29,30,32–35,37–40) except for three studies that had age ranges starting younger (32–84 years,(36) 37–64 years,(24) and 18–60 years(31)). Two studies only specified adults when providing information about age(37,38) and two did not report on age(29,34) although the Egeli cohort was children. There were 84 males collectively and 345 fema les.(21–24,29–32,34–36,39,40) In one study gender was unknown,(33) one was “mixed,”(37) and one listed gender as “all.”(38)
Cancer was the most common serious illness (62.5%).(21–23,32–34,36,38–40) Studies also covered Parkinson’s disease,(35) children with life-threatening conditions,(29) pre-hypertensive individuals,(31) and first-time stroke.(37) Two studies had participants in palliative care(24,30) with the Kelemen study having a cohort with varied illness.
The most common massage was Swedish massage, used in five of the studies,(31,32,38–40) two studies used “soft-tissue massage,”(21,22) one study used “deep whole body (therapeutic) massage,”(35) one “holistic massage,”(23) one “tactile massage,”(37) and four studies did not specify the type of massage provided.(24,29,30,33) Two studies described massage techniques rather than types of massage; Mao et al. used light pressure compressions and effleurage,(34) and Robison and Smith used effleurage and long gliding strokes.(36)
Qualified/licensed massage therapists or massage students under supervision applied the massage in nine studies(22,24,29,34–36,38–40) and nurses in four studies.(21,23,32,37) Nurses in the Jane 2005 study received 4 months of massage training for the purposes of the study and 16 h of training was reported in the paper by Cronfalk et al. (2020). In three studies, it was not clearly stated who provided the massage but extrapolating from other information in the manuscripts the following assumptions are made: nurses provided the treatments in one study(31) and a mixture of therapists provided the treatments in two studies.(30,33) The Fletcher study was a mixture of veterans affairs therapists and massage experienced outside the veterans affairs system, although they did have one massage therapist on staff.(30) The study by Kweku Sey and Hunter had mixed therapists with 30 certified oncology therapists and 20 therapists with other massage styles such as relaxation, Indian, reflexology, or style not stated.
The number of treatments varied with some studies having one treatment(32,34,36) and others multiple treatments; 3,(24) 4,(23) 6,(38) 8,(35) 9,(22,37) 10,(31) and 21(39,40) with four studies not stating the number of treatments received.(21,29,30,33) The most common length of treatment was 20 min(21,23,24,34,36,37) with other treatment lengths being 10–15 min,(31) 25 min,(22) 30 min,(38) 38–50 min,(32) 50 min,(39,40) 60 min,(35) and not stated in three studies.(29,30,33) The most common frequency of treatment was three times per week.(24,31,37–40) Other frequencies of treatment were once,(32,34,36) two times per week,(23) two to three times per week,(21) four to five times per week,(22) and not stated in three studies.(29,30,33)
The areas of the body treated varied between studies. Four studies provided full-body treatments,(32,35,39,40) three studies provided individualized treatments,(21,23,34) two studies treated the hands or feet,(22,37) one study treated the hands/lower arms or feet/lower legs,(36) and one study treated the face, neck, shoulders, and upper chest.(31) Two studies did not report on the areas of the body treated.(29,30) The areas of the body treated did not appear to be related to the serious illness the massage was treating with each area of the body being treated covering various conditions except for the hands and feet/lower limbs which were more likely to be treated when applied during chemo infusion.
Every paper contained mention of psychological benefits from receiving massage(21–24,29–40) (see Table S1). These psychological benefits embraced many aspects of psychological/mental health benefits, with the most comment areas of benefits being improved mood (such as from depression, anxiety, death anxiety, anger(21–24,29–34,36,37)) and relaxation/stress relief.(22–24,29,31–36,38–40)
The scoping review exploring how massage contributes to the mental health of individuals living with a serious and potentially life-limiting illness revealed an overarching theme of “the effable and ineffable impacts of massage” informed by the following themes: massage as a transcendent experience, existential respite, massage helping to preserve dignity, increased inner resources, well-being and relaxation as part of the individualized and personalized vocabulary for massage for the seriously ill, and varied outcomes of the effect of massage on physical symptoms.
“The effable and ineffable impacts of massage” theme captures the complexity of trying to describe the impact of massage and the varied impacts it can have on individuals with serious and potentially life-limiting physical illnesses. These impacts were not linear or predictably structured, and not all impacts were experienced by all participants or by participants every time they received a massage. For some people, massage inspired meaningful changes in symptoms or functions such as decreased pain or improved energy which was easier to describe (effable). For others, the impact of massage transcended the initial symptom change, such as pain, leading to other more profound changes. Some participants’ experience was more difficult to express in words (ineffable) where massage impacted a person’s soul, sense of value, capacity to hope and dream, sense that their life had meaning, and feelings of dignity.
Transcendence, in health care for individuals with serious physical illness and life-limiting conditions, is the engagement and support of individuals to find “meaning and purpose, and to experience connectedness to the self, others, and the significant, or sacred.”(42) Massage was able to provide a transcendent experience for many individuals.(21–23,29,32,36) Some participants experienced massage as facilitating a connection to a sense of self that was significant and sacred, and they were able to find comfort and value in the moment and beyond.
“I had great pleasure from the massage, not only during the moment when she (massage therapist) was here but also afterwards. I felt satisfied and happy afterwards even if the circumstances in which I am in do not usually have the effect on me.”(22)
“It’s also a way of just reintegrating all my pieces and I’m not sure if grounding is the correct word for that, but it’s like I can get back into the world and it’s okay again.”(29)
For others, massage was perceived as caring for all aspects of themselves (physical, spiritual, emotional) and massage felt like a holistic treatment that connected them back to themselves as a whole and provided a sense of home. This was emphasized by one participant who stated that “massage is a cure for souls.”(23)
“I’m so relaxed [in] mind, body, [and] spirit. It’s the whole thing; your body is not just cancer.”(36)
“I just felt secure because of the tactile touch and having a professional around. It was just like [a] return to Mom’s womb.”(32)
Existential distress/suffering is defined as “a distress arising from an inner realization that life has lost its meaning”(43) and can include feelings of hopelessness, spiritual distress, and depression.(44) While not all individuals with serious physical and life-limiting illness will experience existential distress, existential distress is common in this population.(44) Several studies found that individuals experienced existential respite during or after the massage.(22,24,29,31,34,37,38,40) Participant experiences were wide-ranging, reflecting the multifactorial and individualized nature of existential distress and were represented by three subthemes: making connections, presence in the moment, and finding refuge.
For some, massage fostered a sense of meaningful connection with massage being described as “always very warm and comforting(40)” and seeing the therapist “became the highlight of the day when she came and then the massage on top of that….(22)” The massage treatments were impactful as they provided something to look forward to and a sense of physical connection to somebody providing supportive care.
“I look forward to the physical connection with somebody and somebody touching you. It just feels so nice to have someone touching you, helping you with certain issues or problems that you have in certain areas. You feel like you’ve been treated special for the hour.(29)
“[The massage therapist and I] connected and that connection is what gave me that certain ease where I can just flow right on into that massage.”(24)
For some individuals, having a massage provided an experience of awareness of the present moment, a feeling of being grounded and connected to their body and mind.(22,31,38) This allowed participants the time for their body to be tended to and participants felt replenished during and after the massage treatment, often describing a feeling of floating away: “Relaxing and interesting. Very useful, my anxiety is greatly reduced. I felt at ease somehow, calm and wonderfully at peace floating away on clouds….”(31)
“Many have asked me if I was thinking of anything specific (while receiving the massage) but I don’t know if I did… It is like getting to sleep somehow and being in a wonderful atmosphere of feeling good…. I almost feel happy in a way… not in a religious way… it was just wonderful around me.”(22)
“It gave me another place and time that was quiet and I was able to connect again”(38)
Many studies reported the experience of massage as facilitating the capacity to relegate negative thoughts and feelings to the background (bracketing) and for a moment forget about their serious illness.(21,22,24,31,38) For participants this was viewed as a sanctuary and respite from their health concerns and/or thoughts about end of life.
“It helps me just relax and be at ease and kind of forget about it for a little bit.”(24)
“It was very relaxing, I could forget about everything. It let me daydream. I did not want it to stop. I had wonderful feeling. It surprised me….”(31)
Living with a serious and potentially life-limiting physical illnesses can undermine a person’s sense of dignity and capacity to preserve dignity. Due to the illness itself and/or the medical care administered, there can be numerous situations or occasions where there is loss of personal privacy, or a loss of physical or emotional independence. Massage provided moments of preservation of dignity where individuals were able to experience caring and respectful touch. Touch that was not perceived as “medical” but experienced as caring and compassionate was valued: “Tactile therapies such as massage provide a nurturing touch unlike the medical touch.”(33)
“Physical touch is underestimated—it feels great and has a soothing effect. It meant a lot to me and that someone showed compassion.”(22)
“The security in knowing that someone dares touch me too… without me having to ask for it.”(21)
For some, preservation of dignity was related to their environment, and massage transformed their environment either by having a respite from the environment they were continually in or changing the feeling about a static environment which they could not leave.
“The hospital was not as cold as before and it was more homelike. The bed was not a hospital bed, rather it was my home bed.”(32)
“Having 1 hour where you are not in your room and you are not having medical stuff done and people aren’t talking to you about taking your pills or other medical things.”(29)
The massage therapist/provider of the massage treatment was also part of the experience of preservation of dignity. The way that the massage therapist/provider of the massage treatment interacted with the recipient, their compassionate presence, their communication, body language, verbal interaction, and time spent with the recipient engendered a sense of dignity.
“As for the rest of the nursing staff it’s mostly about medicines and such. … and with the masseur it’s a different kind of support… Well, it is knowing it’s there, that she will come … I think she can look at me in a special kind of way.”(21)
“I felt uplifted and happy. It was more than just a massage it had to do with one person (the therapist) giving of herself.”(22)
Massage was viewed as a resource or tool that participants had in their armory to help manage their illness. For some, this was experienced as a resource that helped them manage and carry the impacts of living (and dying) with a serious physical illness.
“In a way it (the massage) had a calming effect on my disturbing thoughts.”(22)
“… and look back and think, like you say, that there is a nice moment still. Because I’m saying you can’t go on carrying it the whole time. And just that short moment means so much.”(21)
In one study where massage was provided during medical care, massage helped them “stay in my body when being in my body was hard due to sickness from chemo.”(33)
For others, massage brought forth a sense of power despite the objective frailty and limitations of having a serious physical illness.
“…… I feel like a new woman, I feel extra power in me. I was cheerful the day that I received massage, I felt more composed somehow, it’s difficult to explain but I felt strengthened in some way….”(31)
“I am in a very difficult situation, the massage helped me to gain strength.”(22)
Massage provided some individuals with an increase in energy which allowed them to do the things that they felt were important to them.
“Fantastic, I do not feel tired after the massage. I was full of energy and without any tiredness. I could follow my responsibility, and interestingly all my daily fatigue was eliminated with massage….”(31)
“It was relaxing, it puts you on the point of having a nap…like you’re meditating and when I’m done…you have that energy to concentrate and do stuff and interact with people.”(24)
For many participants, massage was a resource that provided distraction,(34,36–38) particularly when provided while receiving medical care: “I like that the massage can take my mind off the chemo.”(34) The distraction was also useful as it took participants’ mind off their situation and the negative thoughts and emotions that accompany serious physical illness.
“It was really enjoyable and relaxing. It takes your mind off what you are really doing here.”(36)
“It was a way to disengage from worrying thoughts and anxiety and so on. And that’s what was important…To feel the warm hand touching me, that was actually peaceful. Very comforting, I could dissolve my thoughts from my brain, just disappear and not think about all the strange thoughts and of being scared, just disappear into the massage.”(37)
Participants in the studies used the words relaxation and well-being frequently to describe the impact of massage.(31,33–35,37) The words relaxation and well-being were applied to a variety of experiences (anxiety, pain, troubled thoughts), highlighting the complexity, and the physical and psychological components of relaxation and well-being.(45,46) In the context of serious and potentially life-limiting physical illnesses, participants used semantic augmentation (introduction of new meanings to words) to create their personal meaning of well-being and relaxation that allowed them to describe their experiences of massage. There was no pattern to how participants used well-being and/or relaxation other than they applied it uniquely to their circumstances at the time. It was clear, however, that these overarching terms are allegories for deeper meaningful changes after a massage. For some individuals, well-being was used where the participants felt a sense of lightness as well as a regained sense of self:
“When offered the opportunity to take part in a trial of oncology massage for prostate patients I agreed. Although not severe at the time I was finding the effects of fatigue very intrusive in my life and felt a little disoriented and not quite in control. I was astonished at the end of each session of oncology massage at the “lightness” I felt, the sense of well-being that had been increasingly eluding me. It is astounding, and its positive effect came at a crucial time in my treatment, and I believe has greatly assisted my shaking of the fatigue I had experienced and to allow me to get back to feeling my old self.”(33)
For others, well-being was used in the context of living well with the symptoms of their illness: “Marvellous. My well-being, you know overall well-being has been really great. I’ve gained confidence. I’ve been really good. Doctor just can’t believe it.”(35)
Relaxation was also used with individual meaning for participants. For some participants, relaxation was linked with a reduction in anxiety: “Massage was surprisingly relaxing; it helped me relax, especially in such a short time. I definitely feel better, and it relieves some anxiety. It stimulated relaxation….”(31) and for others it was used when they experienced a respite from thinking about their illness: “Makes me relax. Takes my thoughts off of my health.”(34) Others used it when the massage fulfilled their specific needs at the time.
“As I am overwhelmingly satisfied, I can only say that nothing I have previously experienced have had the same effect. I felt relaxed. I think it must be the same for everyone, I mean the deep sense of relaxation that the massage contributes with”(37)
Physical symptoms were often improved with massage, but the ways recipients described that impact varied. For some participants, massage resulted in an improvement in physical symptoms alone, which was important in the context of serious illness and receiving treatment for their illness.
“It [massage] doesn’t make it [pain] go away permanently but it does make you feel better for a while, which when you are in pain all the time is a big thing.”(30)
“Had massages once a week during chemo. Helped me tolerate the pain.”(34)
For some participants, a change in physical symptom elicited physical and psychological benefits that transcended the challenges of the initial physiological state.
“It [massage] helped me relax and that decreased the pain and helped me to sleep and relieving some of the anxiety”(22)
“To me, the most precious benefit of massage was to ease the tightness [in my] chest, so I felt more [relaxed] while I breathed.”(32)
“I feel whole again. This morning my knees were a little shaky…now they feel like they’re solid.”(39)
The objective of this scoping review was to surface the qualitative aspects of the impact on mental health and well-being of massage in the context of serious physical illness. A striking feature of participant reflections, signifying the complexity of describing subjective experiences, was the extent to which participants constructed highly individualized descriptive accounts and vocabularies, richly imbued with personal metaphors and meanings about their massage experiences, in general, and in relation to relaxation and well-being in particular. The review found that mental health and well-being are important experiences of massage care for individuals with a serious physical illness and our theme, the “effable and ineffable impacts of massage,” describes the wide-ranging and meaningful impacts of massage.
The effable and ineffable impacts of massage are not unique to those receiving care for a serious illness. Massage is a body-based practice that has the capacity to address a broad range of symptom and quality-of-life issues and, in so doing, traverses the biopsychosocial domains of human illness experiences. In the context of individuals with a serious physical illness, massage is distinguishable from usual clinical care in that massage is not treating the illness as such. Rather, massage care can principally and purposively focus on actions that facilitate a pleasant care experience such as an experience of ease and comfort, an experience free from discomfort or pain. Smith et al. (2009)(47) and Smith and Reed (2023)(38) identified the critical factors for massage delivery as care, connection, contact/touch, and comfort. Kolcaba’s theory of comfort locates comfort as a primary goal of care, and identified comfort as a fundamental human need for relief, ease, or transcendence that is more than the absence of pain or physical discomforts.(48) Similarly, Wensley et al. (2020) describes comfort as transient and dynamic, holistic, and multidimensional, associated with relief from pain, emotional and physical distress, feeling safe, feeling in control, and feeling cared for and valued.(49) Theories, concepts, and frameworks can help individuals understand, clarify, communicate, and generally make sense of phenomena. For many massage therapists, cultivating comfort, ease, and relaxation is a “base-camp” goal. For therapists working with the seriously ill, it is integral. Illness is a multi-faceted phenomenon, with each manifestation of the illness influencing another in dynamic and iterative ways. As recounted in the participant commentary and captured in the review themes, massage interposed within this dynamic interacts with this iterative process. The capacity of massage to engender feelings of comfort, relaxation, safety, and/or connection was personal and on a spectrum from something seemingly simple (effable) to something quite transformational or transcendent (ineffable).
The objective of the review was to explore the impacts of massage on the mental health and well-being of the participants. While mental health impacts and well-being were mentioned and described in the included studies, they were often not mentioned explicitly. Instead, phrases such as “I felt strengthened,” “I felt uplifted and happy,” “a wonderful atmosphere of feeling good,” and “so calming” capture a sense of well-being in the moment from which it can be inferred that the mental health of the individuals in those moments benefited, sometimes profoundly, from the experience, and it was common that people reported those feelings lasting beyond the moments of the massage itself. These were experiences beyond a “mere” cessation of pain or worry; rather they described actively positive states of wellbeing. It can be inferred from the identified themes that the mental health of some participants was enhanced in ways that might be expected (relaxation, well-being) and in ways both unexpected and reaching beyond the immediate effect (meaning restoration, inner resource building). However, each of the themes represent states or complex constructs that, thus far, are resistant to objective measurement in the context of massage practice. The paucity, overall, of objective measurement of massage effects (the ineffable in particular) minimizes the value (recipient aside) of such effects. Several studies in this review reported both quantitative and qualitative data and it may be that this is the means through which rich and meaningful data may continue to be sourced.
At present, in the global sphere of health care, there is a “push” toward person-centered care (PCC).(49–51) The primary components of PCC are the engagement of patients in care, co-design of treatments, attention to patient preference and needs, and the utility of patient-reported outcome measures (PROMS) and patient-reported experience measures (PREMS).(52) These are goals of care congruent with massage practice. However, of interest here is the possibility of the development of sensitive and specific-to-massage PROMS and PREMS to robustly capture massage effects in accurate and comprehensive ways for application in research and practice. Capturing massage effects in this way may further cultivate the integration of massage therapy into the clinical care of individuals with serious illnesses, which has gained increasing recognition as a complementary approach to enhancing patient well-being and quality of life. While quantitative research indicates that massage therapy can provide significant benefits for individuals with conditions such as cancer, advanced cardiovascular disease, and neurodegenerative disorders by alleviating pain, reducing anxiety, improving sleep, and enhancing overall emotional resilience,(41,53,54) qualitative research has shown that massage therapy can foster a sense of connection and support, addressing psychosocial aspects of illness that are often inadequately managed by standard medical interventions.(55) Through development of sensitive and specific-to-massage PROMS and PREMS, it may be possible to gather the data to further support access to massage and massage therapy in populations, such as the seriously ill, to have the opportunity for ease, relief, and transcendence and further establish the evidence-based guidelines to facilitate the incorporation of massage therapy into multidisciplinary models of care.(56)
This review expands on the increasing understanding of the contributions of massage and massage therapy to the mental health and well-being of individuals living with a serious and potentially life-limiting physical illness. Some relevant studies may not have been included due to the exclusion of studies published in a language other than English. There is a lack of heterogeneity of study participants which may impact the transferability of the findings, and the contributions of massage may not be applicable to all individuals living with a serious and potentially life-limiting physical illness.
Good mental health and well-being are important aspects of living well with serious illness. The review found there is a considerable body of research which points to the value and impact of massage on outcomes of well-being and mental health and, broadly, on patient experience. The data synthesis underlined the complexity of describing subjective experiences, and that the impact of massage was highly individualized, and participants constructed personalized descriptive accounts and vocabularies, richly imbued with personal metaphors and meanings, to describe their massage experiences. Massage therapy can have an important role as a meaningfully integrated health-care intervention in clinical care that enhances well-being and quality of life for individuals with a serious physical illness. To strengthen its presence, rigorous, mixed-methods research needs to be conducted to better understand the impact of massage therapy on patient experience and, thereby, on clinical outcomes beyond pain management. Future massage research should use research methodologies that ensure that these personalized and profound impacts are captured.
Authors SF and RM work clinically as massage therapists. CC is part of an organization that advocates and teaches massage for individuals affected by illness.
No sources of funding were used in this study.
1. Benavidez GA, Zahnd WE, Hung P, Eberth JM. Chronic disease prevalence in the US: sociodemographic and geographic variations by zip code tabulation area. Prev Chronic Dis. 2024;21:230267. https://doi.org/10.5888/pcd21.230267
Crossref
2. GBD 2021 Diseases and Injuries Collaborators. Global incidence, prevalence, years lived with disability (YLDs), disability-adjusted life-years (DALYs), and healthy life expectancy (HALE) for 371 diseases and injuries in 204 countries and territories and 811 subnational locations, 1990–2021: a systematic analysis for the Global Burden of Disease Study 2021. Lancet. 2024;403(10440):2133–2161. https://doi.org/10.1016/S0140-6736(24)00757-8
Crossref PubMed PMC
3. Pan CX, Palathra BC, Leo-To WF. Management of respiratory symptoms in those with serious illness. Med Clin North Am. 2020;104(3):455–470. https://doi.org/10.1016/j.mcna.2019.12.004
Crossref PubMed
4. Teoli D, Schoo C, Kalish VB. Palliative care. In: Stat-Pearls. StatPearls Publishing; 2024. Copyright © 2024.
5. Warner LM, Ziegelmann JP, Schüz B, Wurm S, Tesch-Römer C, Schwarzer R. Maintaining autonomy despite multimorbidity: self-efficacy and the two faces of social support. Eur J Ageing. 2011;8(1):3–12. https://doi.org/10.1007/s10433-011-0176-6
Crossref PubMed PMC
6. Murali KP, Yu G, Merriman JD, Vorderstrasse A, Kelley AS, Brody AA. Latent class analysis of symptom burden among seriously ill adults at the end of life. Nurs Res. 2021;70(6):443–454. https://doi.org/10.1097/nnr.0000000000000549
Crossref PubMed PMC
7. Ge L, Ong R, Yap CW, Heng BH. Effects of chronic diseases on health-related quality of life and self-rated health among three adult age groups. Nurs Health Sci. 2019;21(2):214–222. https://doi.org/10.1111/nhs.12585
Crossref
8. Lotfaliany M, Bowe SJ, Kowal P, Orellana L, Berk M, Mohebbi M. Depression and chronic diseases: co-occurrence and communality of risk factors. J Affect Disord. 2018;241:461–468. https://doi.org/10.1016/j.jad.2018.08.011
Crossref PubMed
9. Cohen SR, Russell LB, Leis A, Shahidi J, Porterfield P, Kuhl DR, et al. More comprehensively measuring quality of life in life-threatening illness: the McGill Quality of Life Questionnaire – Expanded. BMC Palliat Care. 2019;18(1):92. https://doi.org/10.1186/s12904-019-0473-y
Crossref PubMed PMC
10. Donlan J, Zeng C, Indriolo T, Li L, Zhu E, Zhou J, et al. The Edmonton Symptom Assessment System is a valid, reliable, and responsive tool to assess symptom burden in decompensated cirrhosis. Hepatol Commun. 2024;8(4):e0385. https://doi.org/10.1097/hc9.0000000000000385
Crossref PubMed PMC
11. Cates C, Jordan K, Munk N, Farrand R, Kennedy AB, Groninger H. Massage therapy in palliative care populations: a narrative review of literature from 2012 to 2022. Ann Palliat Med. 2023;12(5):963–975. https://doi.org/10.21037/apm-23-126
Crossref PubMed
12. Cherak SJ, Rosgen BK, Amarbayan M, Wollny KMN, Doig CJ, Patten SB, et al. Mental health interventions to improve psychological outcomes in informal caregivers of critically ill patients: a systematic review and meta-analysis. Crit Care Med. 2021;49(9):1414–1426. https://doi.org/10.1097/ccm.0000000000005011
Crossref PubMed PMC
13. Min JA, Lee CU, Lee C. Mental health promotion and illness prevention: a challenge for psychiatrists. Psychiatry Investig. 2013;10(4):307–316. https://doi.org/10.4306/pi.2013.10.4.307
Crossref
14. Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32. https://doi.org/10.1080/1364557032000119616
Crossref
15. Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, et al. PRISMA extension for Scoping Reviews (PRISMA-ScR): checklist and explanation. Ann Int Med. 2018;169(7):467–473. https://doi.org/10.7326/M18-0850
Crossref PubMed
16. Levac D, Colquhoun H, O’Brien KK. Scoping studies: advancing the methodology. Implement Sci. 2010;5(1):69. https://doi.org/10.1186/1748-5908-5-69
Crossref PubMed PMC
17. Veritas Health Innovation. Covidence systematic review software. http://www.covidence.org/. Accessed March 18, 2025.
18. Kelley AS, Bollens-Lund E. Identifying the population with serious illness: the “Denominator” challenge. J Palliat Med. 2018;21(S2):S7–S16. https://doi.org/10.1089/jpm.2017.0548
Crossref
19. World Health Organization. Mental health. World Health Organization; 2022. https://www.who.int/news-room/fact-sheets/detail/mental-health-strengthening-our-response. Accessed 3 January, 2025.
20. Huppert FA. Psychological well-being: evidence regarding its causes and consequences. Appl Psychol: Health Well-Being. 2009;1(2):137–164. https://doi.org/10.1111/j.1758-0854.2009.01008.x
21. Beck I, Runeson I, Blomqvist K. To find inner peace: soft massage as an established and integrated part of palliative care. Int J Palliat Nurs. 2009;15(11):541–545. https://doi.org/10.12968/ijpn.2009.15.11.45493
Crossref
22. Cronfalk BS, Strang P, Ternestedt BM, Friedrichsen M. The existential experiences of receiving soft tissue massage in palliative home care: an intervention. Support Care Cancer. 2009;17(9):1203–1211. https://doi.org/10.1007/s00520-008-0575-1
PubMed
23. Enrico DL, Maddalena G, Daniela R, Luana P. Integrating massage within oncology nursing care: an Italian pilot study. Int J Caring Sci. 2020;13(1):194–206.
24. Kelemen A, Anderson E, Jordan K, Cates LC, Shipp G, Groninger H. “I Didn’t Know Massages Could Do That:” A qualitative analysis of the perception of hospitalized patients receiving massage therapy from specially trained massage therapists. Complement Ther Med. 2020;52:102509. https://doi.org/10.1016/j.ctim.2020.102509
Crossref
25. Kennedy AB, Cambron JA, Sharpe PA, Travillian RS, Saunders RP. Clarifying definitions for the massage therapy profession: the results of the best practices symposium. Int J Ther Massage Bodyw Res Educ Pract. 2016;9(3):15–26. https://doi.org/10.3822/ijtmb.v9i3.312
26. Lockwood C, Munn Z, Porritt K. Qualitative research synthesis: methodological guidance for systematic reviewers utilizing meta-aggregation. Int J Evid Based Healthc. 2015;13(3):179–187. https://doi.org/10.1097/XEB.0000000000000062
Crossref PubMed
27. Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101. https://doi.org/10.1191/1478088706qp063oa
Crossref
28. Braun V, Clarke V. One size fits all? What counts as quality practice in (reflexive) thematic analysis? Qual Res Psychol. 2021;18(3):328–352. https://doi.org/10.1080/14780887.2020.1769238
Crossref
29. Egeli D, Bainbridge L, Miller T, Potts J. Interdisciplinary perspectives on the value of massage therapy in a pediatric hospice. J Hosp Palliat Nurs. 2019;21(4):319–325. https://doi.org/10.1097/NJH.0000000000000576
Crossref PubMed
30. Fletcher CE, Mitchinson AR, Trumble EL, Hinshaw DB, Dusek JA. Perceptions of other integrative health therapies by Veterans with pain who are receiving massage. J Rehabil Res Dev. 2016;53(1):117–126. https://doi.org/10.1682/JRRD.2015.01.0015
Crossref PubMed PMC
31. Garakyaraghi M, Givi M, Moeini M, Eshghinezhad A. Qualitative study of women’s experience after therapeutic massage. Iran J Nurs Midwifery Res. 2014;19(4):390–395.
PubMed PMC
32. Jane S-W. Effects of a full-body massage on pain intensity, anxiety, and physiologic relaxation in Taiwanese patients with metastatic bone pain: a pilot study. University of Washington; 2005. https://dissertation.com/abstract/1770331#:~:text=Massage%20was%20shown%20to%20have,20%20minutes%20after%20the%20intervention. Accessed June 2, 2025.
33. Kweku Sey A, Hunter J. Finding the value in oncology massage: a mixed-method study of cancer services and survivors in Australia. Adv Integr Med. 2020;7(3):126–134. https://doi.org/10.1016/j.aimed.2020.01.003
Crossref
34. Mao JJ, Wagner KE, Seluzicki CM, Hugo A, Galindez LK, Sheaffer H, et al. Integrating oncology massage into chemoinfusion suites: a program evaluation. J Oncol Pract. 2017;13(3):e207–e216. https://doi.org/10.1200/JOP.2016.015081
Crossref PubMed PMC
35. Paterson C, Allen JA, Browning M, Barlow G, Ewings P. A pilot study of therapeutic massage for people with Parkinson’s disease: the added value of user involvement. Complement Ther Clin Pract. 2005;11(3):161–171. https://doi.org/10.1016/j.ctcp.2004.12.008
Crossref PubMed
36. Robison JG, Smith CL. Therapeutic massage during chemotherapy and/or biotherapy infusions: patient perceptions of pain, fatigue, nausea, anxiety, and satisfaction. Clin J Oncol Nursng. 2016;20(2):E34–E40. https://doi.org/10.1188/16.CJON.E34-E40
Crossref
37. Cronfalk BS, Åkesson E, Nygren J, Nyström A, Strandell A-M, Ruas J, et al. A qualitative study—patient experience of tactile massage after stroke. Nursing Open. 2020;7(5):1446–1452. https://doi.org/10.1002/nop2.515
Crossref
38. Smith MC, Reed SM. A unitary theory of healing through touch. Adv Nurs Sci. 2023;46(2):219–232. https://doi.org/10.1097/ANS.0000000000000487
Crossref
39. Snyder AEW. Effects of massage therapy and touch on quality of life outcomes for autologous stem cell transplant patients. University of Virginia; 2007. https://libraetd.lib.virginia.edu/public_view/k3569435m#:~:text=Results%3A%20An%20immediate%20effect%20in,seen%20in%20the%20massage%20group
40. Taylor AG, Snyder AE, Anderson JG, Brown CJ, Densmore JJ, Bourguignon C. Gentle massage improves disease- and treatment-related symptoms in patients with acute myelogenous leukemia. J Clin Trials. 2014;4:1000161. https://doi.org/10.4172/2167-0870.1000161
Crossref PubMed PMC
41. Jane SW, Wilkie DJ, Gallucci BB, Beaton RD, Huang HY. Effects of a full-body massage on pain intensity, anxiety, and physiological relaxation in Taiwanese patients with metastatic bone pain: a pilot study. J Pain Symptom Manage. 2009;37(4):754–763. https://doi.org/10.1016/j.jpain-symman.2008.04.021
Crossref
42. Post L, Ganzevoort RR, Verdonck-de Leeuw IM. Transcending the suffering in cancer: impact of a spiritual life review intervention on spiritual reevaluation, spiritual growth and psycho-spiritual wellbeing. Religions. 2020;11(3):142. https://doi.org/10.3390/rel11030142
Crossref
43. Gaignard M-E, Pautex S, Hurst S. Existential suffering as a motive for assisted suicide: difficulties, acceptability, management and roles from the perspectives of Swiss professionals. medRxiv. 2022. https://doi.org/10.1101/2022.03.21.22272665
44. Martins H, Silva RS, Bragança J, Romeiro J, Caldeira S. Spiritual distress, hopelessness, and depression in palliative care: simultaneous concept analysis. Healthcare (Basel). 2024;12(10):960. https://doi.org/10.3390/healthcare12100960
Crossref PubMed PMC
45. Steghaus S, Poth CH. Feeling tired versus feeling relaxed: two faces of low physiological arousal. PLoS One. 2024;19(9):e0310034. https://doi.org/10.1371/journal.pone.0310034
Crossref PubMed PMC
46. McCaffery M. Nursing Management of the Patient with Pain. 2nd ed. Lippincott; 1979.
47. Smith JM, Sullivan SJ, Baxter GD. The culture of massage therapy: valued elements and the role of comfort, contact, connection and caring. Complement Ther Med. 2009;17(4):181–189. https://doi.org/10.1016/j.ctim.2009.05.003
Crossref PubMed
48. Kolcaba K, Schirm V, Steiner R. Effects of hand massage on comfort of nursing home residents. Geriatr Nurs. 2006;27(2):85–91. https://doi.org/10.1016/j.gerinurse.2006.02.006
Crossref PubMed
49. Wensley C, Botti M, McKillop A, Merry AF. Maximising comfort: how do patients describe the care that matters? A two-stage qualitative descriptive study to develop a quality improvement framework for comfort-related care in inpatient settings. BMJ Open. 2020;10(5):e033336. https://doi.org/10.1136/bmjopen-2019-033336
Crossref PubMed PMC
50. Björkman I, Dellenborg L, Ringström G, Simrén M, Jakobsson Ung E. The gendered impact of Irritable Bowel Syndrome: a qualitative study of patients’ experiences. J Adv Nurs. 2014;70(6):1334–1343. https://doi.org/10.1111/jan.12294
Crossref
51. Björkman I, Ringström G, Simrén M, Myrgren J, Jakobsson Ung E. An intervention for person-centered support in irritable Bowel syndrome: development and pilot study. Gastroenterol Nurs. 2019;42(4):332–341. https://doi.org/10.1097/SGA.0000000000000378
Crossref PubMed
52. Edgman-Levitan S, Schoenbaum SC. Patient-centered care: achieving higher quality by designing care through the patient’s eyes. Isr J Health Policy Res. 2021;10(1):21. https://doi.org/10.1186/s13584-021-00459-9
Crossref PubMed PMC
53. Ferrell BR, Temel JS, Temin S, Alesi ER, Balboni TA, Basch EM, et al. Integration of palliative care into standard oncology care: American Society of Clinical Oncology Clinical Practice Guideline update. J Clin Oncol. Jan 2017;35(1):96–112. https://doi.org/10.1200/jco.2016.70.1474
Crossref
54. Kutner JS, Smith MC, Corbin L, Hemphill L, Benton K, Mellis BK, BS, et al. Massage therapy versus simple touch to improve pain and mood in patients with advanced cancer: a randomized trial. Ann Intern Med. 2008;149(6):369–379. https://doi.org/10.7326/0003-4819-149-6-200809160-00003
Crossref PubMed PMC
55. Smith MC, Kemp J, Hemphill L, Vojir CP. Outcomes of therapeutic massage for hospitalized cancer patients. J Nurs Scholarsh. 2002;34(3):257–262. https://doi.org/10.1111/j.1547-5069.2002.00257.x
Crossref PubMed
56. Williams ACC, Fisher E, Hearn L, Eccleston C. Psychological therapies for the management of chronic pain (excluding headache) in adults. Cochrane Database Syst Rev. 2020;8(8):CD007407. https://doi.org/10.1002/14651858.CD007407.pub4
PubMed PMC
Corresponding author: Sarah Fogarty, PO Box 8218, Ferntree Gully, Victoria 3156, Australia, E-mail: fogarty@ijtmb.org
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
International Journal of Therapeutic Massage and Bodywork, Volume 18, Number 3, September 2025