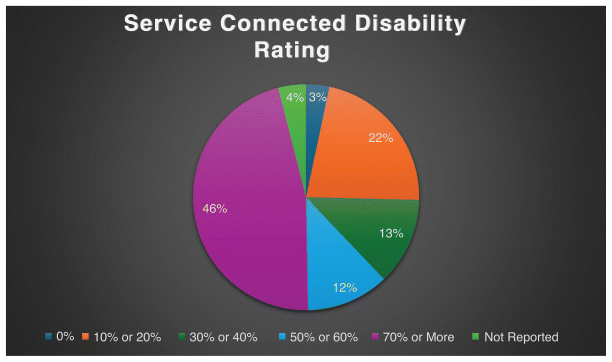
Figure 1 Service connected disability rating.(5)
Christopher Rodriguez, MS,1* Jude Matyo-Cepero, PhD2
1Graduate School of Business, University of the Cumberlands, Williamsburg, KY, USA,
2College of Education, University of Nebraska at Kearney, Kearney, NE, USA, Professor EmeritaProfessionals in the massage therapy field strive to help clients gain pain relief. Military veterans are a small group that experiences significant pain due to service-related physical and mental disabilities. The struggle of these veterans in the United States and Canada has been a concern after decades of combat overseas and rigorous training stateside. Nearly a quarter century after the September 11 attacks, government organizations such as the medical branch of the Department of Veterans Affairs (VA) in the United States have recognized the benefits of massage therapy for veterans. The VA has gone as far as paying for massage therapy treatments at no cost to the veteran. This commentary provides a brief overview of the physical and mental disabilities faced by U.S. and Canadian military veterans, an example of the VA in the U.S. supporting veterans with massage therapy, and considerations for the future.
KEYWORDS: Military veterans; Veterans Affairs; Whole Health; massage therapy; physical and mental well-being
The 9/11 attacks that occurred at the start of this century have changed our way of life and how countries use their military. The attacks were followed by various military campaigns, including an International Security Assistance Force (ISAF) from the North Atlantic Treaty Organization (NATO) that involved nearly 50 nations.(1) With conflicts such as the 2001–2021 War in Afghanistan now over, there remain veterans who served there or trained during that time who suffer from physical disability related to their service in this era and require help, such as massage therapy, to relieve their pain.(2)
Times have changed, and a quarter century after the 9/11 attacks, veterans’ changing medical needs must be met with treatments that work for them. As a result, treatment offerings in the United States, considered “new” by American Medical standards, have received interest and have been a welcome addition to support veterans. In 2022, the Veterans Health Administration (VHA) Directive 1,137 was approved. This directive offered the opportunity for Complementary and Integrative Healthcare when deemed clinically necessary by the medical care team of the veteran. Massage therapy was included in that list.(3) This was the groundwork to be a significant relief for those veterans suffering from physical and mental disabilities in the United States, with the possibility of other countries following suit.
Military veterans are a unique population facing complex physical and mental challenges. There are several reasons for this. The military is a physically demanding career field. Military members must maintain strength and readiness through physical fitness. Prospective recruits in the United States can serve full-time (active duty) in the U.S. Army, U.S. Marine Corps, U.S. Navy, U.S. Air Force, U.S. Coast Guard, or the U.S. Space Force. They also have the option to join part-time in the National Guard or Reserves. In any option, they could face stress, demanding challenges, and life-threatening situations.(2)
The past few decades saw U.S. military members deployed (sometimes more than once) to combat in Iraq or Afghanistan. These deployments typically involve the daily use of heavy gear. Examples of heavy gear include body armor, rucksacks, and weapons. Most military members regularly carry heavy gear weighing at least 60 pounds. Using the gear for extended periods can cause physical stress and muscle pain. For example, on deployment, military members wear helmets (weighing 4 pounds) and vision goggles (weighing 2 pounds) for lengthy periods, which can cause stress and pain to the head, neck, and spine. This can cause physical issues such as pain, muscle fatigue, and headaches. If left unaddressed, it can develop into a disability.(2)
Regardless of whether a military member is deployed to combat or not, they are still facing risks of injury at a higher rate than those who never served.(2) Military members face years of running on hard surfaces, wearing heavy boots, being in confined spaces, falling, and having accidents. Those deployed to combat and participate in combat logistics patrols (also known as convoys) or any activity outside the base faced the risk of contact with an Improvised Explosive Device (IED), also known as a roadside bomb, significantly increasing the likelihood of an immediate physical or mental disability.(2)
The culture of the military is also a factor in delaying care for physical and mental disabilities. Often, military teams foster a culture of training through pain, and members could feel shame for seeking care that takes them out of physical training or missions. As humans, we all age, and it can become more difficult for older military members to train and prove their worth. This can often lead to increased chances of an injury. They may even neglect the time needed for injuries to heal to get back in the game. This could lead to reinjury, which could lead to long-term consequences. Common injuries among all military members are injuries to the neck, shoulders, feet, ankles, knees, and back. These physical disabilities could create lifetime challenges.(2)
Military members often face mental health challenges. Lack of sleep is common in military units due to mission demands, long shifts, and varying shifts. In the U.S. Navy, it is common to see members staying awake for up to 72 hours. Military members are often away from home due to deployments or short-term assignments, which can disrupt their normal sleep patterns. Long work hours while at home, traveling for assignments, and short- and long-term military base moves are primary factors leading to increased stress and reduced wellness in military members.(2) Post-traumatic stress disorder (PTSD) is common among members of the military, especially those deployed to combat. Other common mental health conditions among the military are depression and anxiety.(4)
Veterans receive disability compensation ratings from the Veterans Affairs (VA), ranging from 0% to 100%. Ratings can be for both physical and mental health disabilities. The rating determines the amount of monthly compensation a veteran receives. In 2023, the U.S. Census Bureau reported that of approximately 16 million veterans, almost 5 million received a disability compensation rating. Those with a rating of 10% or 20% were over 1 million, while those with 70% or higher were over 2 million, or 46% of the group. Figure 1 shows the breakdown.(5)
|
| ||
|
Figure 1 Service connected disability rating.(5) | ||
Those who served in the Canadian military faced a similar experience to their American counterparts. Veterans in Canada experienced similar physical and mental health-demanding challenges during their service in the military. Before the significant War on Terror efforts, only 12% of medical releases were due to medical reasons, including physical and mental health issues. Due to service in Afghanistan, the medical releases increased to 25%.(6) Roughly half of the veterans had at least one disability. Of those, 43% of veterans aged 45–64 years and 55% of those aged 65 years and above had at least one disability. Pain-related disabilities were at 72%, and 66% were classified as physical. Additionally, 26% of veterans identified with a disability had disability benefits, with 65% of those veterans having a disability benefit from the Canadian VA. Figure 2 shows the breakdown of some of these statistics.(7)
|
| ||
|
Figure 2 Veteran disabilities in Canada.(7) | ||
Whole Health is a model developed by the VA and launched as a pilot program in 2013 to provide personalized care to veterans. The idea is to provide care to veterans that is outside the use of opioids and other Western medical care approaches. The Whole Health program was created in part to help address the opioid epidemic in the United States. In 2014, the VA’s integrative health coordinating center was established.(8)
There were specific mandates for the Whole Health program, one being that it must be accessible to all veterans at a VA medical facility or within the community. The VA would cover the entire cost when veterans are referred to the community for care. Referring veterans to the community for care is known as community-based care. To promote the physical well-being of veterans, the Whole Health program offers acupuncture, meditation, yoga, Tai Chi, Qi Gong, biofeedback, clinical hypnosis, guided imagery, and massage therapy. The Mission Act of 2018 mandated the VA to create modernized systems for veterans to promote lifelong health and resiliency. The use of the Whole Health program is often tied to integrative medicine care at the VA.(8)
Veterans who receive massage therapy through the Whole Health program reported that it helped to reduce pain, increase mobility, and reduce their use of opioids.(9) A study found that massage therapy substantially benefited veterans facing pain and knee osteoarthritis challenges. The study was done by collaborating with the Duke University Integrative Medicine clinic and the VA Medical Center in Durham, North Carolina. Twenty-five symptomatic knee osteoarthritis veterans underwent eight weekly 1-hour sessions of full-body Swedish massages. The results were promising. After 8 weeks, these veterans reported a 36% improvement in knee pain and a 30% improvement in knee stiffness and function. The authors discussed how the results demonstrated that massage therapy could help reduce knee pain and stiffness and improve function.(10)
A study conducted by Mitchinson and colleagues aimed to examine the benefits of massage therapy for female veterans experiencing pain, depression, and anxiety. Ninety-six women veterans were part of the study. Of those 96 women, 79% reported a history of chronic pain, and 65% were diagnosed with depression and anxiety. Massage therapy was performed on their back, neck, hands, arms, legs, and feet. The veterans reported a reduction in their physical pain and reduced feelings of depression and anxiety. The study authors noted the need for a larger sample size to provide more evidence and to better learn how massage therapy can help with physical pain and mental health condition symptoms among women veterans.(11)
Military veterans of the United States and Canadian militaries face significant challenges with pain and physical disabilities. Massage therapy is a proven benefit for military veterans who have served in the Global War on Terrorism era. The example of the VA in the United States supporting and providing cost-free access to massage therapy benefits could serve as a model for other government VA branches. With approximately 50 nations that engaged in combat in Afghanistan, there is a high chance of veterans from those nations facing pain and physical disability challenges due to their service. Massage therapy can be an excellent benefit for veterans. There is a great opportunity to expand this proven benefit to veterans worldwide by the following:
In conclusion, this commentary covered a brief overview of the physical and mental disabilities faced by U.S. and Canadian military veterans, an example of the VA in the United States supporting veterans with massage therapy, and considerations for the future. While this health-care offering is still in the initial stages in the United States, the possibility of positive potential results worldwide is encouraging. Veterans made sacrifices to serve and protect. It is our turn to ensure they receive the support and care they need for a healthier future. By advocating for solutions such as massage therapy, we can offer meaningful relief to those who have sacrificed so much. Let us take action today to improve the lives of veterans and establish a global standard of care for those who served.
The first author reports that they are a U.S. Army veteran. The second author has no competing interests to declare.
No sources of funding were used in this study.
1. North Atlantic Treaty Organization. NATO and Afghanistan. Nato.int; 2022. Available from: https://www.nato.int/cps/en/natohq/topics_8189.htm.
2. Salvo S. Massage Therapy Principles and Practice. 6th ed. Elsevier; 2020.
3. U.S. Department of Veterans Affairs. IHCCWhole Health. U.S. Department of Veterans Affairs; (n.d.). Available from: https://www.va.gov/WHOLEHEALTH/professional-resources/Massage_Therapy.asp#:~:text=We%27re%20here%20anytime%2C%20day,Espa%C3%B1ol
4. Moore MJ, Shawler E, Jordan CH, Jackson CA. Veteran and Military Mental Health Issues. StatPearls; 2023. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572092/.
5. U.S. Census Bureau. Service-Connected Disability-Rating Status and Ratings for Civilian Veterans 18 Years and Over. U.S. Census Bureau; 2023. Available from: https://data.census.gov/table/ACSDT1Y2023.B21100?q=Veterans&y=2023.
6. Aiken A, Buitenhuis A. Supporting Canadian Veterans with Disabilities: A Comparison of Financial Benefits. Queen’s University; 2011. Available from: https://www.queensu.ca/cidp/sites/cidpwww/files/uploaded_files/Claxton13(1).pdf
7. Government of Canada. Snapshot of Canadian Veterans with Disabilities, 2022. Government of Canada; 2022. Available from: https://www150.statcan.gc.ca/n1/pub/11-627-m/11-627-m2024049-eng.htm.
8. Gantt CJ, Donovan N, Khung M. Veterans affairs’ whole health system of care for transitioning service members and veterans. Mil Med. 2023;188:28–32. https://doi.org/10.1093/milmed/usad047
Crossref PubMed
9. Fletcher CE, Mitchinson AR, Trumble EL, Hinshaw DB, Dusek JA. Perceptions of other integrative health therapies by veterans with pain who are receiving massage. J Rehabil Res Dev. 2016;53(1): 117–126. https://pubmed.ncbi.nlm.nih.gov/27004453/.
Crossref
10. Juberg M, Jerger KK, Allen KD, Dmitrieva NO, Keever T, Perlman AI. Pilot study of massage in veterans with knee osteoarthritis. J Altern Complement Med. 2015;21(6):333–338. https://doi.org/10.1089/acm.2014.0254
Crossref PubMed PMC
11. Mitchinson A, Fletcher CE, Trumble E. Integrating massage therapy into health care of female veterans. Fed Pract. 2022;39(2):86–92. https://doi.org/10.12788/fp.0223
PubMed PMC
Corresponding author: Christopher Rodriguez, School of Business, University of the Cumberlands, 6178 College Station Drive, Williamsburg, KY 40769, USA. E-mail: justcallmechris2018@gmail.com
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
International Journal of Therapeutic Massage and Bodywork, Volume 18, Number 4, December 2025