Fernando Cabo, MSc1*
1Barts Health NHS Trust, London, UK
Background
Conventional pharmacological treatment does not always relieve cancer pain satisfactorily, increasing the need for further medication. Complementary and integrative therapies are offered to cancer inpatients to improve their well-being. Although manual therapies such as massage and reflexology are commonly offered to hospitalized cancer patients in the UK, Shiatsu in this setting is little known and has been studied much less.
Aims
The purpose of this project is to examine the pain-relieving effects of Heisei Shiatsu in hospitalized cancer patients and to compare those results with other bodywork modalities which have been established for longer in this field.
Methods
Fifty-five inpatients received 66 Heisei Shiatsu treatments. Interventions are adapted to health issues and specific pain complaints. Patients scored changes in pain intensity, the relief provided, and changes in mood as a result of the treatment using the validated Integrative Medicine Treatment Evaluation Form. The pre- and post-treatment scores for pain and mood were analyzed with both student’s t-test and the Wilcoxon signed-rank test. Results for relief are given in percentage points. All results were compared to results for other therapies stated in comparable research articles.
Results
Decrease in pain intensity and pain relief was reported after the Shiatsu session by all patients. The average reduction in pain was 40%. Thirty-two percent of the patients said their pain had been completely relieved, and 45% stated the pain had been mostly relieved. Compared to results in similar studies, Shiatsu is more effective than aromatherapy or reflexology in reducing pain among cancer patients. Almost all patients commented on the relaxing and soothing effects of these treatments.
Conclusion
Heisei Shiatsu can be delivered alongside conventional care for patients with cancer. Although the sample size is not big enough to draw definite conclusions, it warrants further research into the safety of Heisei Shiatsu in this setting and its relaxing effects as described by many of the patients.
KEYWORDS: Integrative oncology; massage; oncology massage; Shiatsu; aromatherapy massage; reflexology; Reiki; hospital
Pain continues to be one of the main issues affecting cancer patients for which there is not always a solution. The pain may be a product of the tumor, a side effect of the treatment, or as a consequence of the patient having to stay in bed and not moving enough. In many instances, this results in a limitation to daily activities and a reduction in quality of life (QoL).(1–3) In many occasions, even in cases of complete remission among cancer survivors, pain continues to be a concern, and quite often patients do not understand why this is so.(4,5) One of the most commonly reported types of pain is neuropathic pain, which in itself may have been induced by chemotherapy. Many cancer survivors report the ongoing neuropathic pain as well as pins and needles for a very long time after their treatment has finished.(6–9) Although many cancer patients experience one kind of pain or another that ranges from mild to severe, it would appear that cancer pain is undertreated and underreported—sometimes because it is perceived by patients and doctors that pain is inevitable, either as a result of the disease or of the treatment. Unrelieved pain may in turn reduce patient mobility, resulting in a higher risk of complications such as deep vein thrombosis.(10,11)
One type of pain that is specific to cancer patients is breakthrough pain (BTP). Many patients, despite the use of pain-killing opioids, report BTP, which has been defined as “an episode of severe intensity in patients receiving an adequate treatment with opioids able to provide at least mild analgesia.”(12) Although undoubtedly life-saving and extremely useful, there are limitations to what medical drugs can achieve when controlling cancer pain in general and BTP in particular, since often pharmacological means do not provide the expected relief, leading patients to feel dissatisfied with the subsequent impact on their QoL.(13,14)
Most experts and researchers in the field agree that cancer pain should not be treated exclusively from a purely medical point of view. Care of patients should be holistic and combine the medical treatment with psychological and social support.(15) To explain the multi-dimensional aspect of a patient’s pain experience, Dame Cicely Saunders, a strong advocate for the hospice movement and for the understanding of the emotional connections of pain, coined the term “total pain” over 30 years ago, highlighting the complexity and challenges in the management and assessment of pain in cancer patients.(16) The biopsychosocial model does not view pain as a purely physical phenomenon but a combination of physical, psychological, and social factors. It also acknowledges that physical pain also affects our emotional and social well-being and can therefore have a negative impact on our QoL.(17)
In this respect, a manual therapy such as Heisei Shiatsu massage has the advantage that it may reduce pain and at the same time improve the patient’s mood through the therapist’s presence and communication and the induction of a relaxation response.(18)
Several guidelines for the treatment of cancer pain have been published. Probably one of the most widely used are the guidelines developed by the World Health Organization (WHO) which tried to standardize the pharmacological pain management of cancer pain.(19) These guidelines outline three steps. The first step consists of non-opioids and adjuvants for mild pain. The second step includes opioid and non-opioid painkillers for moderate pain, and the third step recommends strong opioids as well as non-opioid analgesics and adjuvants.(3,20) Some authors have suggested adding a fourth and even a fifth step for the most complex cases when patients have not been helped by the more traditional approach. The suggestion is to adjust the WHO pain management ladder to a more sophisticated five-step scheme, separating potentially reversible neuromodulation from virtually irreparable procedures, such as cordotomy, and include physical and psychological procedures in all the steps.(21)
Opioids remain the mainstay of cancer pain management, but the consequences of tolerance, dependency, and side effects should be taken into account when managing cancer pain. Common problems that recur with the use of opiates are constipation, sedation, nausea and vomiting, dry mouth, toxicity, and morphine intolerance. Constipation, with a very high incidence, and nausea are by far the most common side effects of opioids usage.(22)
Non-pharmacological management of cancer pain is increasingly used by clinics and hospices with the aim of reducing the perception of pain among patients. Mind–body therapies,(23–25) massage,(26–28) transcutaneous electrical nerve stimulation,(29) thermal measures (heat therapy and cryotherapy),(30–32) and counseling(33) have been studied as adjuvants for the treatment of cancer pain. The importance of adapting massage techniques and patient positioning to deliver these interventions more effectively and with less discomfort for receivers is something some research papers have specified.(31,34) These methods may help relieve the pain or increase the patient’s comfort, but the effect may wear off after some time because pain is influenced by many factors. It is clear, however, that the effect of pain medication also wears off.(31) In this respect, the assessment of a patient’s pain and their response should be ongoing.
Among the manual therapies that have been more studied for the management of pain in cancer patients are massage (with and without aromatherapy oils) and reflexology.(35) Only one Shiatsu study was found in which results for pain were analyzed as part of the effects on all types of symptoms among cancer patients.(36)
From the research literature, there are also indications that Shiatsu massage may help in reducing pain levels when treating headaches(37) and fibromyalgia,(38) so it was thought that studying the effects of Shiatsu on only one symptom, such as pain, might give more credibility to its usefulness in a hospital setting.
The analgesic effects of massage in cancer patients have been studied, but the evidence is not conclusive. Several studies have shown these effects in a palliative care setting. The same studies have also shown that massage, as a pain reduction technique, is usually more effective on those who feel strong pain before the intervention.(39) Some studies that include reflexology report slightly better results in pain reduction for reflexology than massage.(40,41)
However, many of these studies have been deemed inadequate to investigate efficacy because most of the trials done with massage and reflexology do not have adequate numbers. Researchers have also reported an unwillingness among healthcare practitioners to refer patients to this type of study because they do not want their patients randomized to the non-massage control group.(42)
It has also been pointed out that the link between the manipulation of the body with manual therapies and any relief experienced by patients for their symptoms is not completely understood and that the connection between mind and body in the application of these therapies, and symptom relief, should be further investigated. Physiological pathways, as well as the effects, that explore the processes and connections between massage, blood flow, and central nervous system adaptations are areas of research that may facilitate the design of appropriate randomized controlled clinical trials.(43)
A number of charities and hospices offer Shiatsu as part of their complementary therapies service. At the time of writing, however, despite the fact that many public hospitals with cancer inpatients in the UK offer complementary and integrative therapies (CITs), research papers have not identified any centers offering Shiatsu.(44) An internet search for “shiatsu cancer patients hospital uk” returns only five hospitals in the whole of the UK that offer this manual therapy as part of their complementary therapies service. If we change the word “patients” for “inpatients,” only three of those offer the service to inpatients (The five hospitals are Whipps Cross Hospital (Margaret Centre), St Bartholomew’s Hospital, Weston Park Hospital (Weston Park cancer charity), West Middlesex University Hospital (Mulberry Centre), and Royal Surrey Hospital (Fountain Centre). Only the first three appear to offer Shiatsu for inpatients.).
It was thought relevant to compare the results of Heisei Shiatsu from this study to the results from aromatherapy massage and reflexology in two studies carried out in the UK in hospital settings(45,46) to see if this type of intervention shows effectiveness to the same level.
The aim of this study is to analyze the effects of Heisei Shiatsu massage on the perception of pain reduction and relief in a group of cancer inpatients in a London hospital, see its value as a possible adjunct to the pharmacological treatment of cancer-related pain, and compare the results with other bodywork modalities which have been established for longer in this field.
Shiatsu can be defined as “a manual therapy applied by leaning forward in a relaxed manner with the relaxed weight of one’s body to an optimum point, and the correct use of fingers, palms, etc., in order to apply sustained, stationary pressure gradually and rhythmically on different parts of the body. It is a holistic therapy that aims to treat most of the body in each session, but which can be applied exclusively on specific parts of the body, i.e., only the feet or only the head.”(47–49)
This definition encompasses all the different styles and schools of Shiatsu. Although styles may differ in some of their theoretical constructs and preferences in the use of the palms of the hands, the thumbs, or the elbows to apply pressure, all styles agree that Shiatsu should be performed with the transfer of one’s own weight when leaning forward to apply pressure. This is the reason why “pressure” has a very specific meaning in Shiatsu, and it does not mean the same as in other manual therapies and bodywork.(49,50)
To this basic definition, it can be added that Shiatsu does not use creams or oils and is performed through clothing so patients do not remove their clothes, although in the context of hospital patients, sometimes it is necessary to inspect under the clothes to check for contraindications.
Like in other bodywork modalities, there are different styles of Shiatsu. They all agree on the relaxed use of the weight,(50) which sometimes is expressed as “pressing” instead of “pushing.”(51) However, the systematic approach, the philosophy, and focus or emphasis on certain aspects of the bodywork can vary quite a lot.(52) Some focus on viscero-cutaneous and sensory reflexes, others believe that which points you press is the most important aspect of their Shiatsu, while others highlight diagnostic systems.(53,54)
Heisei Shiatsu is a style of Shiatsu developed by the author with the help of some of his students and derived from his long experience giving Shiatsu in hospitals and events. His past experience includes 6 years of giving Shiatsu three times a week to children in the dialysis department before they were connected to the machines, and brief stints in the same pediatric hospital in the intensive care unit, mostly with new-born babies, as well as delivering Shiatsu for children who suffered from osteogenesis imperfecta at AHUCE (Asociación de Huesos de Cristal España—the Spanish brittle bone disease association) annual conferences. The ongoing experience includes over 10 years in two London hospitals delivering Shiatsu for cancer and palliative care patients and 2 years giving Shiatsu at The Disability Foundation where he has treated patients with such diverse conditions as Tourette syndrome, Crohn’s disease, Ehlers–Danlos syndrome, osteoporosis, osteoarthritis, rheumatoid arthritis, arthrogryposis, and epiphyseal dysplasia.(55,56)
To the definition and explanation given above, Heisei Shiatsu is a style that adds two defining principles, the no-pain principle and the adaptation of the treatment to the circumstances and mobility of the patient. The no-pain principle is the more important of the two and states that the treatment itself should be painless. A qualified therapist in Heisei Shiatsu should have acquired a deep, soft, painless pressure and know how to adjust the intensity and speed of their pressure to deliver painless, soothing, and pain-relieving treatments. As far as the author knows, no other style or school of thought within Shiatsu has made the quality of the pressure applied the main basis, the main tenet of its philosophy, and practical application. Heisei Shiatsu has explored and highlighted the difference between “deep pressure” and “strong pressure”.(57) In Heisei Shiatsu, pressure is always adapted to the needs and comfort of the patients. Heisei Shiatsu is also based on the principle that the whole body is connected and therefore there is no need to focus the work on painful areas. Relieving other muscles helps reduce the pain anywhere in the body. The reason why Heisei Shiatsu insists on painless treatments is because pain causes muscles to contract when the aim is to relax them.(57,58)
The second principle is adapting our posture and our movements to the needs of particular patients. This is not unique to Heisei Shiatsu. Other styles, but not all, have adopted it too.(59) Adaptation is especially important with hospitalized patients. Many of these patients have mobility issues, so it is up to the therapist to reach as many areas as possible without inconveniencing the patient. For example, a Heisei Shiatsu therapist will work on the upper back while the patient is lying on their back, not asking them to move if this causes any inconvenience, or will work on the feet without the need to remove the footboard. In this sense, Heisei Shiatsu may be more versatile than other types of massage which require specific positions from patients.(60) It can be adapted to almost any position or situation whether the patient is in bed, sitting, or in a wheelchair.(47,56) The beds in the hospital can be reclined for those patients with respiratory conditions such as lung cancer or chronic obstructive pulmonary disease, so that they feel comfortable during the session.
Manual therapies have characteristics that depend on the practitioner, and these may influence treatment effects and affect trials’ results.(61) As recommended in other studies,(62) qualifications, affiliation, experience, and clinical expertise of the practitioner are reported below.
The shortest treatment lasted 25 min and the longest one 40 min with an average time for treatment of 30 min. Treatments are always individualized depending on contraindications, what the therapist feels, and on feedback from the patient. The therapist performing the treatments for this study graduated in 2002, has been a teacher of Shiatsu since 2007, and is a member of the Complementary and Natural Healthcare Council. He was trained in therapeutic bodywork in cancer and palliative care at the Margaret Centre at Whipps Cross Hospital, London.
The complementary therapies service at St Bartholomew’s Hospital cancer wards in London, UK is offered 2 days per week. Patients are informed of the service, and they self-refer to receive treatments if interested. CITs on offer at the time of writing are biodynamic massage, Bowen technique, Shiatsu, massage, reflexology, and Reiki. Patients usually stay from 1 to 6 weeks in the wards, so the number of treatments they can receive varies, but many patients will only have one session, although approximately a third of them will have at least two sessions. A consultation form is used to assess the condition of the patients and establish contraindications, to explain the treatment process, to decide on length of treatment, and to get the patient’s consent.(57,58)
All patients who received a Shiatsu treatment and reported any type of pain and/or ache were eligible to be included in this project. Excluded were those who suffered from dementia or had any impediment—such as a speech impediment—that made communicating their experience of pain and pain relief difficult. Patients who had taken analgesics prior to the treatment were also excluded since it would have been too great a confounding factor.
Exclusion from the study did not preclude patients from receiving a Shiatsu session.
Data were collected from November 2022 to December 2023 at St Bartholomew’s Hospital (Bart’s) in London, UK, as part of the service evaluation which is presented to governance for the continuation of the service. In the past, this has been done using the Measure Yourself Concerns and Wellbeing (MYCaW) pretest–posttest questionnaire, but it has been decided to use the Integrative Medicine Treatment Evaluation Form (IMTEF). The data presented here are a subset of all the data collected as part of the standard complementary therapies service.
The questionnaire is distributed among those patients/service users who have chosen a complementary therapy intervention before the service evaluation. There was no randomization or allocation, and the questionnaire is designed and evaluates current care. As established by the UK’s National Research Ethics Service, this is considered a service evaluation and as such does not require ethics approval.(63,64)
For this study, it was deemed appropriate to use the pretest–posttest design of the validated IMTEF questionnaire. The complementary therapists delivering the service ask patients to fill in the form or help them fill it in when patients request it before and after the intervention. All collected forms are stored at the hospital. The data collected record the main concern or area of pain experienced by the patient, pre- and post-treatment scores, the patient’s perspective on relief obtained from the intervention, and any changes in mood as a result of the treatment.(65) Patients were given the form to complete before and after the intervention although there were a few cases in which the patients asked the therapist to complete the form.
Numerical data were analyzed using MedCalc online statistical software (Med-Calc Software Ltd., Ostend, Belgium). The calculation for sample size for paired samples t-test with a mean difference of 1, a standard deviation (SD) of 1.72, and the standard type I error 0.05 and type II error 0.2 returns 26 minimal required number of pairs which the sample in this paper satisfies.
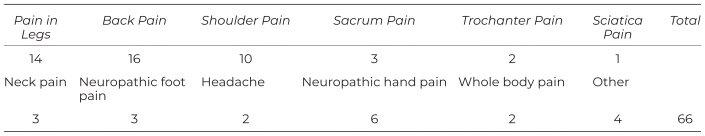
All data were anonymized before being analyzed for the writing of this paper. Baseline and endline data were collected for 55 inpatients—19 males and 36 females, age ranging from 24 to 81 years with an average age of 53 years—for a total of 66 treatments. Forty-four patients had only one session. Eight had two sessions, two had three sessions, and one patient had four sessions. Table 1 shows the main complaint from which patients suffered prior to the Heisei Shiatsu treatment.
The data on self-reported perception of pain on a scale of 0–10 have been analyzed with both the paired samples t-test and the Wilcoxon signed-rank test as shown in Table 2.
Table 2 Differences in Pain Scores
Based on a significance level of 0.05, both the Wilcoxon signed-rank test and the paired student’s t-test indicated that post-treatment ranks and means were lower than pre-treatment ranks and means in pain scores. The two-tailed p-value is <0.001. By conventional criteria, this difference is considered to be statistically significant. The minimal clinically important difference (MCID) is not a standardized measurement, and as such, it varies in individual practices and is usually related to different types of pain.(66,67) In manual therapies, it is generally accepted that a 2-point difference in a 10-point numerical scale or 2 cm in a 10-cm visual analog scale is the MCID.(68,69) The mean improvement was 4.05 on a scale of 0–10 which corresponds to a 40% improvement.
The data on self-reported perception of pain relief obtained from the treatment is shown in Table 3. Patients reported to have gained at least some relief, and in almost 78% of treatments, they reported their pain had been mostly or completely relieved. No patient reported any increase in pain after treatment.
Table 3 Differences in Mood After Treatment
Table 4 shows the change in mood scores given by patients before and after the treatment. IMTEF uses a scale of −5 to 5 for this purpose to differentiate how positively or negatively one is feeling at that particular moment with 0 as a neutral point.
Table 4 Comparison of Pain Score Differences After Treatment Between Heisei Shiatsu at Bart’s Hospital and Aromatherapy Massage, and Reiki at UCLH, London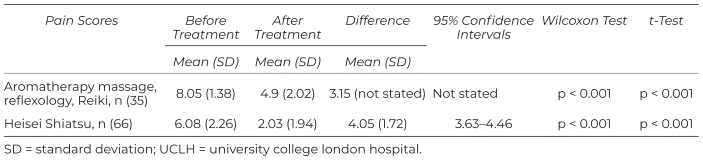
The perceived mood difference was an increase of 2.45 points (1.34 SD) in how patients felt after treatment.
On the IMTEF, patients are asked to relate how the treatment has made them feel or what effect it has had on them. Apart from answering that question, sometimes patients spontaneously add comments which are also recorded.
Some of the replies were “I feel relieved of the tension and at peace. I’m going to have a nap now,” “I haven’t felt this relaxed in months,” “The ache has disappeared and I feel very, very relaxed,” “This is the second massage I receive in my life. The first one was so hard I couldn’t move for two days. This one is so relaxing,” “I have had back pain for 3 days. This the first day I feel relief,” “Before, I couldn’t lie on my back for more than 10 minutes without experiencing a lot of pain. I have been lying on my back for 25 minutes now and I don’t feel any pain,” and “Very nice and gentle.” The most common comments were about pain reduction, feeling relaxed, or feeling so relaxed they were going to sleep immediately after treatment.
Some of the patients’ family members and friends who stayed in the room during the treatment session commented “I feel more relaxed just by watching.” Others who chose to leave the room said they appreciated to have a bit of time to relax or go for a walk.
This paper includes the comparison of Heisei Shiatsu to the results of other types of CIT interventions for cancer patients in similar settings. The results are compared to the results obtained from two London hospitals where complementary therapies are offered to cancer patients. The data from these two hospitals are publicly available in published research papers. Table 5 compares the results with the results obtained for aromatherapy massage, reflexology, and Reiki at the University College Hospital, London,(45) and Table 6 compares the results with those results obtained for aromatherapy massage and reflexology at The Royal Marsden Hospital, London.(46)
Table 5 Comparison of Proportion of Patients with a Change Greater Than One Point on the MYCaW Scores at The Royal Marsden Hospital and Equal or Greater Than Two Points on the IMTEF
Table 6 Self-Reported Perception of Pain Relief Provided by the Heisei Shiatsu Treatment
This study is comparing data collected with different scales, so scales have been converted for comparison. The two studies compared to the results of the intervention in this paper used the MYCaW form with a scale of 0 (best) to 6 (worst),(70) while the research carried out for this paper used the IMTEF form with a scale of 0 (best) to 10 (worst).(65) To be able to compare both scales, MYCaW results have been reset to a 0–10 scale, a process known as scale resetting or normalization (see Appendix 1).
This research paper intended to present the feasibility of introducing Shiatsu alongside other CITs for cancer patients in hospital and hospice settings as well as showing its benefits in the management of pain. Many if not most of the characteristics of Heisei Shiatsu are shared by other Shiatsu styles,(48,49,52,71) although those styles might put more emphasis on other aspects of Shiatsu.(57) However, it has been difficult to carry out research that included other styles because no other Shiatsu therapists work at St Bart’s Hospital, and other hospitals that offer CITs for cancer patients do not include Shiatsu among their therapies, making it difficult to obtain more data.(44) An integrative approach that includes CITs to the treatment of cancer patients means that there might be added benefits for symptom control compared to cases in which only pharmacological control of those symptoms is offered. CITs also help improve the sense of well-being and QoL.(72) Shiatsu can be easily adapted to the circumstances of a hospital setting and the needs of inpatients, making it a useful intervention in the CITs field alongside the other modalities offered at present in other hospitals and hospices. At St Bartholomew’s Hospital, London, the nurses, physiotherapists, doctors, and the rest of the health-care workers appreciate the fact that CITs are on offer and refer patients to the team because they can see the benefits.
From the data on Tables 5 and 6, it would appear that Heisei Shiatsu can be considered at least as effective as other therapies such as aromatherapy massage and reflexology in the treatment of pain complaints among cancer patients.
Although the interventions in this study were geared toward the relief of pain, in the majority of cases, patients reported the effects not only as pain relieving but as deeply relaxing, calming, and soothing, giving this type of treatment an extra dimension which analgesics sometimes do not provide.
Clinically significant improvement in 11-point numerical rating scales such as the IMTEF have been reported in the research literature as between 1.41 and 1.65 points,(73,74) while for MYCaW it is considered that an improvement of 1 point is clinically significant.(75) For the purposes of this study and of comparison with other CITs modalities, it has been considered that any change of ≥2 points on the IMTEF scale is clinically significant.
The data show that in improvement scores (Table 2), perception of pain relief (Table 3), and mood changes due to the intervention (Table 4), Heisei Shiatsu is a useful adjunct to the pharmacological treatment of cancer pain among inpatients which warrants further research.
In four of these cases, the pain relief appears to have held, and the following sessions started with a lower pain score. In the other three cases, the area of pain has changed. In four cases, the pain score at the beginning of each session was almost the same, but the relief was great. In total, 11 patients had more than one session. The sample is too small and the results too dissimilar to draw any conclusions on the possible effects of having more sessions.
The data also show that Heisei Shiatsu is at least comparable in effectiveness to other CITs used in hospitals for cancer patients. When compared to other therapies used in some UK hospitals for cancer patients, Table 5 shows that the mean improvement for pain is slightly above the one obtained in another hospital, and Table 6 shows that the percentage of those who have had a clinically significant change is higher than the results shown for aromatherapy massage and reflexology, although in this case, it must be taken into account that the results presented for aromatherapy massage and reflexology are for all types of concerns and not only for pain.
The immediate outcome measures were obtained by an unblinded study therapist, possibly leading to the overestimation of beneficial effect by patients. The generalizability to all cancer patients who experience pain is uncertain. The differential beneficial effect of Heisei Shiatsu therapy is not conclusive in the absence of a standard care control group and randomization. The comparison of the results for inpatients in Heisei Shiatsu has been with the results for outpatients with other CIT modalities, with the inpatients getting shorter treatments of 30 min, while outpatients at the Royal Marsden were getting 1 h of treatment. Outpatients got four sessions although the frequency is not stated, while the sessions inpatients get vary. These factors might represent a confounding factor.
Also, it is felt that pain should be scored/measured not only before and after treatment, as it has been done for this study, but also at certain intervals after the treatment to measure the duration of the effect. However, this is not possible in most cases since patients may have been discharged and the therapist will not have any further contact with them.
The results demonstrated the feasibility and usefulness of providing Heisei Shiatsu massage to hospitalized cancer patients. This study suggests that Heisei Shiatsu is helpful in relieving pain after each session. The study also showed that patients were appreciative of the intervention and felt better and much more relaxed after the treatment. These preliminary findings support further study of Heisei Shiatsu massage as a complementary therapy adjuvant to pain management in hospitalized cancer patients. Investigating the physiological effects and mechanisms of the intervention may be of interest to provide the scientific evidence base to guide future clinical practice especially when applied to pain relief.
The author thanks profusely Neil Browne for his training in therapeutic bodywork for cancer, for his help in setting up the project, and his support during the running of the project. The service evaluation was set up with the help of Neil Browne.
The author declares there are no conflicts of interest.
No sources of funding were used in this study.
The author did the writing and analysis of data.
1. Pharo GH, Zhou L. Pharmacologic management of cancer pain. J Am Osteopath Assoc. 2005;105:S21–S28.
PubMed
2. Glare P, Aubrey K, Gulati A, Lee YC, Moryl N, Overton S. Pharmacologic management of persistent pain in cancer survivors. Drugs. 2022;82:275–291. https://doi.org/10.1007/s40265-022-01675-6
Crossref PubMed PMC
3. Virgen CG, Kelkar N, Tran A, Rosa CM, Cruz-Topete D, Amatya S, et al. Pharmacological management of cancer pain: novel therapeutics. Biomed Pharmacother. 2022;156:113871. https://doi.org/10.1016/j.biopha.2022.113871
Crossref PubMed
4. Nijs J, Wijma AJ, Leysen L, Pas R, Willaert W, Hoelen W, et al. Explaining pain following cancer: a practical guide for clinicians. Braz J Phys Ther. 2019;23:367–377. https://doi.org/10.1016/j.bjpt.2018.12.003
Crossref PubMed PMC
5. O’Regan A, Fish LJ, Makarushka C, Somers T, Fitzgerald Jones K, Merlin JS, et al. Managing chronic pain in cancer survivorship: communication challenges and opportunities as described by cancer survivors. Am J Hosp Palliat Care. 2024;41:78–86. https://doi.org/10.1177/10499091231164634
Crossref
6. Bennett MI, Rayment C, Hjermstad M, Aass N, Caraceni A, Kaasa S. Prevalence and aetiology of neuropathic pain in cancer patients: a systematic review. Pain. 2012;153:359–365. https://doi.org/10.1016/j.pain.2011.10.028
Crossref
7. Rayment C, Hjermstad MJ, Aass N, Kaasa S, Caraceni A, Strasser F, et al. Neuropathic cancer pain: prevalence, severity, analgesics and impact from the European Palliative Care Research Collaborative-Computerised Symptom Assessment study. Palliat Med. 2013;27:714–721. https://doi.org/10.1177/0269216312464408
Crossref
8. Zajaczkowską R, Kocot-Kępska M, Leppert W, Wrzosek A, Mika J, Wordliczek J. Mechanisms of chemotherapy-induced peripheral neuropathy. Int J Mol Sci. 2019;20:1451. https://doi.org/10.3390/ijms20061451
Crossref
9. Dupoiron D, Brill S, Eeltink C, Barragán B, Bell D, Petersen G, et al. Diagnosis, management and impact on patients’ lives of cancer-related neuropathic pain (CRNP): a European survey, Eur J Cancer Care (Engl). 2022;31:e13728. https://doi.org/10.1111/ecc.13728
10. Antón A, Montalar J, Carulla J, Jara C, Batista N, Camps C, et al. Pain in clinical oncology: patient satisfaction with management of cancer pain. Eur J Pain. 2012;16:381–389. https://doi.org/10.1002/j.1532-2149.2011.00036.x
Crossref PubMed
11. Stoorvogel H, van Haastregt J, Theunissen M, Schoenmaekers J, Hoeben A, van den Beuken-van Everdingen M. Unacceptable pain in oncology: the patients’ perspective on reasons for absence of pain interventions. Eur J Cancer Care (Engl). 2022;31:e13628. https://doi.org/10.1111/ecc.13628
12. Mercadante S. Breakthrough pain in cancer patients: prevalence, mechanisms and treatment options. Curr Opin Anaesthesiol. 2015;28:559–564. https://doi.org/10.1097/ACO.0000000000000224
Crossref PubMed
13. Vellucci R, Mediati RD, Gasperoni S, Piergallini LM, Valentino MC, Bruno GM, et al. PSY42—Pharmacoeconomic considerations about breakthrough cancer pain. Value Health. 2015;18:A665–A666. https://doi.org/10.1016/j.jval.2015.09.2426
Crossref
14. Mercadante S, Maltoni M, Russo D, Adile C, Ferrera P, Rossi R, et al. The prevalence and characteristics of breakthrough cancer pain in patients receiving low doses of opioids for background pain. Cancers (Basel). 2021;13:1058. https://doi.org/10.3390/cancers13051058
Crossref PubMed PMC
15. British Pain Society. Managing cancer pain - information for patients. 2010. https://www.britishpainsociety.org/static/uploads/resources/files/book_cancer_pain_patients_1.pdf. Accessed December 17, 2023.
16. Wood J. Cicely Saunders, ‘Total Pain’ and emotional evidence at the end of life. Med Humanit. 2022;48:411–420. https://doi.org/10.1136/medhum-2020-012107
Crossref
17. Dams L, Van der Gucht E, Haenen V, Lauwers M, De Pauw S, Steurs T, et al. Biopsychosocial risk factors for pain and pain-related disability 1 year after surgery for breast cancer. Support Care Cancer. 2022;30:4465–4475. https://doi.org/10.1007/s00520-022-06805-0
PubMed
18. Kutner JS, Smith MC, Corbin L, Hemphill L, Benton K, Mellis BK, et al. Massage therapy versus simple touch to improve pain and mood in patients with advanced cancer: a randomized trial. Ann Intern Med. 2008;149:369–379. https://doi.org/10.7326/0003-4819-149-6-200809160-00003
Crossref PubMed PMC
19. World Health Organization. WHO guidelines for the pharmacological and radiotherapeutic management of cancer pain in adults and adolescents. 2019. https://www.who.int/publications/i/item/9789241550390 Accessed January 20, 2026.
20. Yang J, Bauer BA, Wahner-Roedler DL, Chon TY, Xiao L. The modified WHO analgesic ladder: is it appropriate for chronic non-cancer pain? J Pain Res. 2020;13:411–417. https://doi.org/10.2147/JPR.S244173
Crossref PubMed PMC
21. Nersesyan H, Slavin KV. Current approach to cancer pain management: availability and implications of different treatment options. Ther Clin Risk Manag. 2007;3:381–400.
22. Benyamin R, Trescot AM, Datta S, Buenaventura R, Adlaka R, Sehgal N, et al. Opioid complications and side effects Pain Physician. 2008;11:S105–120.
Crossref PubMed
23. Lyman GH, Greenlee H, Bohlke K, Bao T, DeMichele AM, Deng GE, et al. Integrative therapies during and after breast cancer treatment: ASCO endorsement of the SIO Clinical Practice Guideline. J Clin Oncol. 2018;36:2647–2655. https://doi.org/10.1200/JCO.2018.79.2721
Crossref PubMed
24. Paice JA, Portenoy R, Lacchetti C, Campbell T, Cheville A, Citron M, et al. Management of chronic pain in survivors of adult cancers: American Society of Clinical Oncology Clinical Practice Guideline. J Clin Oncol. 2016;34(27):3325–3345. https://doi.org/10.1200/JCO.2016.68.5206
Crossref PubMed
25. Ngamkham S, Holden JE, Smith EL. A systematic review: mindfulness intervention for cancer-related pain. Asia Pac J Oncol Nurs. 2019;6(2):161–169. https://doi.org/10.4103/apjon.apjon_67_18
Crossref PubMed PMC
26. Gentile D, Boselli D, Yaguda S, Greiner R, Bailey-Dorton C. Pain improvement after healing touch and massage in breast cancer: an observational retrospective study. Int J Ther Massage Bodywork. 2021;14(1):12–20. https://doi.org/10.3822/ijtmb.v14i1.549
Crossref PubMed PMC
27. Zhang Y, Wang S, Ma X, Yuan Y, Cheng H, Lin L, et al. Massage therapy can effectively relieve cancer pain: a meta-analysis. Medicine. 2023;102(27):e33939. https://doi.org/10.1097/MD.0000000000033939
Crossref PubMed PMC
28. Win Myint O, Yoong SQ, Toh E, Lei F, Jiang Y. Effectiveness of massage therapy for cancer pain, quality of life and anxiety levels: a systematic review and meta-analysis, J Clin Nurs. 2025;34:49–87.
Crossref
29. Vance CGT, Dailey DL, Chimenti RL, Van Gorp BJ, Crofford LJ, Sluka KA. Using TENS for pain control: update on the state of the evidence. Medicina. 2022;58:1332. https://doi.org/10.3390/medicina58101332
Crossref PubMed PMC
30. Chandler A, Preece J, Lister S. Using heat therapy for pain management. Nurs Stand. 2002;17(9):40–43. https://doi.org/10.7748/ns2002.11.17.9.40.c3297
Crossref PubMed
31. Gatlin CG, Schulmeister L. When medication is not enough: nonpharmacologic management of pain. Clin J Oncol Nurs. 2007;11(5):699–704.
Crossref PubMed
32. Ferrer-Mileo L, Luque Blanco AI, González-Barboteo J. Efficacy of cryoablation to control cancer pain: a systematic review. Pain Pract. 2018;18:1083–1098. https://doi.org/10.1111/papr.12707
Crossref PubMed
33. Teo I, Krishnan A, Lee GL. Psychosocial interventions for advanced cancer patients: a systematic review. Psychooncology. 2019;28:1394–1407. https://doi.org/10.1002/pon.5103
Crossref PubMed
34. Collinge W, MacDonald G, Walton T. Massage in supportive cancer care. Semin Oncol Nurs. 2012;28:45–54. https://doi.org/10.1016/j.soncn.2011.11.005
Crossref PubMed
35. Shin ES, Seo KH, Lee SH, Jang JE, Jung YM, Kim MJ, et al. Massage with or without aromatherapy for symptom relief in people with cancer. Cochrane Database Syst Rev. 2016(6):CD009873. https://doi.org/10.1002/14651858.CD009873.pub3
PubMed PMC
36. Browne N, Bush P, Cabo F. Relieving pressure – an evaluation of Shiatsu treatments for cancer & palliative care patients in an NHS setting. Eur J Integr Med. 2018;21:27–33. https://doi.org/10.1016/j.eujim.2018.06.002
Crossref
37. Villani V, Prosperini L, Palombini F, Orzi F, Sette G. Single-blind, randomized, pilot study combining shiatsu and amitriptyline in refractory primary headaches. Neurol Sci. 2017;38:999–1007. https://doi.org/10.1007/s10072-017-2888-7
Crossref PubMed
38. Yuan SLK, Berssaneti AA, Marques AP. Effects of Shiatsu in the management of fibromyalgia symptoms: a controlled pilot study. J Manipulative Physiol Ther. 2013;36:436–443. https://doi.org/10.1016/j.jmpt.2013.05.019
Crossref PubMed
39. Falkensteiner M, Mantovan F, Müller I, Them C. The use of massage therapy for reducing pain, anxiety, and depression in oncological palliative care patients: a narrative review of the literature. ISRN Nurs. 2011(1):929868. https://doi.org/10.5402/2011/929868
PubMed PMC
40. Hodgson NA, Lafferty D. Reflexology versus Swedish massage to reduce physiologic stress and pain and improve mood in nursing home residents with cancer: a pilot trial. Evid Based Complement Alternat Med. 2012(1):456897. https://doi.org/10.1155/2012/456897
PubMed PMC
41. Stephenson NLN, Swanson M, Dalton J, Keefe FJ, Engelke M. Partner-delivered reflexology: effects on cancer pain and anxiety. Oncol Nurs Forum. 2007;34:127–132.
Crossref
42. Corbin L. Safety and efficacy of massage therapy for patients with cancer. Cancer Control. 2005;12:158–164.
Crossref PubMed
43. Sagar SM, Dryden T, Wong RK. Massage therapy for cancer patients: a reciprocal relationship between body and mind. Curr Oncol. 2007;14:45–56.
Crossref PubMed PMC
44. Egan B, Gage H, Hood J, Poole K, McDowell C, Maguire G, et al. Availability of complementary and alternative medicine for people with cancer in the British National Health Service: results of a national survey. Complement Ther Clin Pract. 2012;18(2):75–80. https://doi.org/10.1016/j.ctcp.2011.11.003
Crossref PubMed
45. Charlesworth E, Hughes J, Plant H, Carballo L. Complementary therapy for people with cancer; the patient’s perspective. Eur J Integr Med. 2018;17:26–32. https://doi.org/10.1016/j.eujim.2017.10.009
Crossref
46. Dyer J, Thomas K, Sandsund C, Shaw C. Is reflexology as effective as aromatherapy massage for symptom relief in an adult outpatient oncology population? Complement Ther Clin Pract. 2013;19:139–146. https://doi.org/10.1016/j.ctcp.2013.03.002
Crossref PubMed
47. Tsiormpatzis S. Safety and risks of shiatsu: protocol for a systematic review. Eur J Integr Med. 2019;28:20–26. https://doi.org/10.1016/j.eujim.2019.03.006
Crossref
48. Cabo F, Baskwill A, Aguaristi I, Christophe-Tchakaloff S, Guichard JP. Shiatsu and acupressure: two different and distinct techniques. Int J Ther Massage Bodywork. 2018;11(2):4–10. https://doi.org/10.3822/ijtmb.v11i2.391
Crossref PubMed PMC
49. Cabo F, Aguaristi I. Similarities and differences in East Asian massage and bodywork therapies: a critical review. OBM Integr Complement Med. 2020;5(1):013. https://doi.org/10.21926/obm.icm.2001013
Crossref
50. Bernardinelli N, Valery A, Barrault D, Dorland JM, Palut P, Toumi H, et al. Effectiveness of Shiatsu on fatigue in patients with axial spondyloarthritis: protocol for a randomized cross-over pilot study. Rheumatol Ther. 2023;10(4):1107–1117. https://doi.org/10.1007/s40744-023-00558-w
Crossref PubMed PMC
51. Jarmey C. Shiastu Foundation Course. 1st ed. Alresford, UK: Godsfield Press; 1999.
52. Di Novi A. Les grandes familles de shiatsu. Shiatsu France; 2020. https://www.shiatsu-france.com/article-les-courants-shiatsu.html. Accessed May 4, 2025.
53. Syndicat des Professionnels de Shiatsu. Quels types de Shiatsu. Le Shiatsu; 2025. https://www.syndicatshiatsu.fr/quels-types-de-shiatsu/. Accessed May 4, 2025.
54. The Shiatsu Society (UK). Styles of Shiatsu. Shiatsu - The Art and Science of Touch; 2021. https://www.shiatsusociety.org/styles-of-shiatsu. Accessed May 4, 2025.
55. TDF. The Disability Foundation History. 2013. https://www.tdf.org.uk/abou/history/. Accessed December 17, 2023.
56. TDF. Complementary therapies at the disability foundation (TDF). Youtube [Online Video]; 2023. https://www.youtube.com/watch?v=LmiH0T_HPpI. Accessed December 17, 2023.
57. Cabo F. Heisei Shiatsu: Deep Shiatsu and the No-Pain Principle. 1st ed. London: Fernando Cabo, Self-published; 2023.
58. Ferreira M. Heisei Shiatsu therapy explained. TraditionalBodywork.Com; 2022. https://www.traditionalbodywork.com/heisei-shiatsu-therapy-explained-thumbs-based-acupressure/. Accessed December 17, 2023.
59. Bel I. La petite interview Shiatsu avec Fanny Roque: aider les malades du cancer avec le Shiatsu. Ryoho Shiatsu Youtube Channel; 2025. https://www.youtube.com/watch?v=-FRQeiD1w7U. Accessed May 5, 2025.
60. Cassileth BR, Vickers AJ. Massage therapy for symptom control: outcome study at a major cancer center. J Pain Symptom Manage. 2004;28:244–249. https://doi.org/10.1016/j.jpainsymman.2003.12.016
Crossref PubMed
61. Russell NC, Sumler SS, Beinhorn CM, Frenkel MA. Role of massage therapy in cancer care. J Altern Complement Med. 2008;14:209–214.
Crossref PubMed
62. Lee SH, Kim JY, Yeo S, Kim SH, Lim S. Meta-analysis of massage therapy on cancer pain. Integr Cancer Ther. 2015;14:297–304. https://doi.org/10.1177/1534735415572885
Crossref PubMed
63. National Research Ethics Service, National Patient Safety Agency. Defining research. London: National Research Ethics Service, National Patient Safety Agency; 2009. https://www.uhbristol.nhs.uk/media/1572809/defining_research_leaflet_1_.pdf. Accessed March 15, 2025.
64. Moule P, Armoogum J, Dodd E, Donskoy AL, Douglass E, Taylor J, et al. Practical guidance on undertaking a service evaluation. Nurs Stand. 2016;30(45):46–51. https://doi.org/10.7748/ns.2016.e10277
Crossref
65. Cabo F, Browne N. The development, validity, and responsiveness of a patient-centred outcome measurement tool for evaluating integrative medicine interventions. Int J Ther Massage Bodywork. 2023;16(3):20–34. https://doi.org/10.3822/ijtmb.v16i3.859
Crossref PMC
66. Desai N, Albrecht E. Minimal clinically important difference: bridging the gap between statistical significance and clinical meaningfulness. J Clin Anesth. 2024;94:111366. https://doi.org/10.1016/j.jclinane.2023.111366
Crossref
67. Saithna A, Cote MP. Editorial Commentary: The minimal clinically important difference is less important than it sounds: patients seek to achieve substantial clinical benefits and not minimally perceptible improvements when they undergo arthroscopic surgery. Arthroscopy. 2024;40(4):1089–1092. https://doi.org/10.1016/j.arthro.2023.10.014
Crossref
68. Dworkin RH, Turk DC, Wyrwich KW, Beaton D, Cleeland CS, Farrar JT, et al. Interpreting the clinical importance of treatment outcomes in chronic pain clinical trials: IMMPACT recommendations. J Pain. 2008;9(2):105–121. https://doi.org/10.1016/j.jpain.2007.09.005
Crossref
69. Espejo-Antunez L, Cardero-Duran MLA, Heredia-Rizo AM, Casuso-Holgado MJ, Albornoz-Cabello M. Effects of adding electro-massage to manual therapy for the treatment of individuals with myofascial temporomandibular pain: a randomized controlled trial. J Appl Oral Sci. 2024;32:e20240109.
Crossref PMC
70. Jolliffe R, Seers H, Jackson S, Caro E, Weeks L, Polley MJ. The responsiveness, content validity, and convergent validity of the Measure Yourself Concerns and Wellbeing (MYCaW) patient-reported outcome measure. Integr Cancer Ther. 2015;14(1):26–34. https://doi.org/10.1177/1534735414555809
Crossref
71. Bel I. Perpendicular and continuous pressure. In: The Spirit of Shiatsu. Singing Dragon; 2025.
72. Marchand L. Integrative and complementary therapies for patients with advanced cancer. Ann Palliat Med. 2014;3:160–171. https://doi.org/10.3978/j.issn.2224-5820.2014.07.01
73. Kendrick DB, Strout TD. The minimum clinically significant difference in patient-assigned 11-point numeric pain scale scores for pain. Ann Emerg Med. 2004;44:S86–S87. https://doi.org/10.1016/j.annemergmed.2004.07.283
74. Bahreini M, Safaie A, Mirfazaelian H, Jalili M. How much change in pain score does really matter to patients? Am J Emerg Med. 2020;38:1641–1646. https://doi.org/10.1016/j.ajem.2019.158489
Crossref
75. Polley MJ, Jolliffe R, Boxell E, Zollman C, Jackson S, Seers H. Using a whole person approach to support people with cancer: a longitudinal, mixed-methods service evaluation. Integr Cancer Ther. 2016;15:435–445. https://doi.org/10.1177/1534735416632060
Crossref PubMed PMC
76. Giannoulis C. Rescaling sets of variables to be on the same scale. The Analysis Factor; 2020. https://www.theanalysisfactor.com/rescaling-variables-to-be-same/. Accessed March 22, 2025.
77. Clement SL, Severin-Nielsen MK, Shamshiri-Petersen D. Device effects on survey response quality. A comparison of smartphone, tablet and PC responses on a cross sectional probability sample. Surv Methods Insights Field. 2020. https://doi.org/10.13094/SMIF-2020-00020
78. Seci M. Normalization, the Coding Club. n.d. https://ourcodingclub.github.io/tutorials/data-scaling/#Standardization. Accessed March 22, 2025.
Corresponding author: Fernando Cabo, Margaret Centre, Whipps Cross University Hospital, Margaret Road, London E11 1NR, UK, E-mail: fernando.cabo@nhs.net, Tel: +44 2085395522
When comparing tables that use several variables with different ranges and units, we need to convert or rescale some or all of them so that we get the same lower and upper levels for each scale. Normalization is one of the processes used in these cases. The formula is
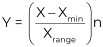 where Y is the adjusted variable, X = value on original variable, Xmin = minimum on original variable, Xrange = range on the original variable, and n = upper limit of the new variable.(76–78)
where Y is the adjusted variable, X = value on original variable, Xmin = minimum on original variable, Xrange = range on the original variable, and n = upper limit of the new variable.(76–78)
Measure Yourself Concerns and Wellbeing (MYCaW) uses a scale of 0–6 with 0 being the lower value (best, not bothering me at all) and 6 the upper value (worst, bothering me greatly). To convert/rescale to a 0–10 scale, we get for 6,
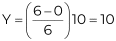 , and for 0,
, and for 0,
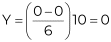 .
.
The following table gives the results for MYCaW units.
The following table gives the conversion for University College London Hospital pain scores as stated on Table 5.
Table S1 Conversion of a 0–6 scale to a 0–10 scale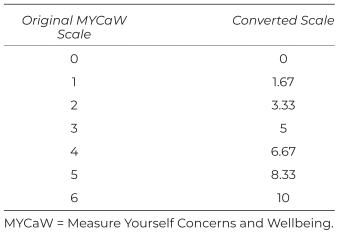
Table S2 Rescaling of table 4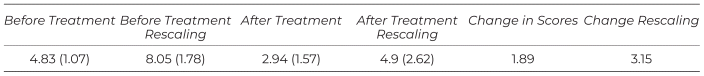
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
International Journal of Therapeutic Massage and Bodywork, Volume 19, Number 1, March 2026