The Effects of Self-Massage on Osteoarthritis of the Knee: a Randomized, Controlled Trial
Dorothea V.
Atkins
,
ThD, RN
,
David A.
Eichler
,
PhD
Holos University Graduate Seminary, Bolivar, MO, USA
Introduction
Recent research has provided a rationale for the efficacy and use of massage therapy in the management of knee osteoarthritis (OA) symptoms. Additionally, research has also implicated the role of the quadriceps muscles in the genesis of knee OA. Although both areas of research have demonstrated strong evidence that the muscles and massage therapy may affect knee OA symptoms, self-massage applied on the quadriceps muscle has received no attention.
Methods
Conducted at the Lourdes Wellness Center in Collingswood, NJ, the study investigated the outcomes of a self-massage intervention applied to the quadriceps muscle on reported pain, stiffness, physical function, and knee range of motion in adults with diagnosed knee OA. Forty adults with diagnosed knee OA were randomly assigned to either an intervention (n = 21) or a wait list control (n = 19) group. The participants applied a narrated 20-minute self-massage therapy twice weekly during ten supervised and three unsupervised intervention sessions. The control group had four supervised assessments with no intervention. Outcome measures were the Western Ontario and McMaster’s Osteoarthritis Index (WOMAC) and assessment of knee range of motion.
Results
Between-groups analyses of WOMAC pain, stiffness, function subscales, and total WOMAC scores indicated significant difference between groups (
p
< .05), n = 36). No significant differences were seen in range of motion.
Conclusions
The study demonstrated that participants who have OA of the knee benefit from the self-massage intervention therapy. Further studies are needed to clarify the long-term effects of self-massage on the progression and symptoms of knee OA.
KEYWORDS:
massage
,
self-massage
,
osteoarthritis
,
self-management
,
knee osteoarthritis
,
musculoskeletal
,
chronic pain
INTRODUCTION
Symptomatic radiographic knee osteoarthritis (OA) has a functional impact on 12% of adults aged 60 or older—4.3 million people—in the United States(1). The knee is one of the joints most commonly affected by OA(2). Given projected increases in the aging and obese populations, the incidence of OA of the knee is predicted to rise(3). Moreover, despite earlier research indicating joint cartilage degeneration as a possible primary cause of knee OA—initiating internal joint inflammation, edema, and pain(2)—recent research has investigated the causative role of the quadriceps muscle, which is located on the anterior thigh. In this muscle, weakness, impairments in function, influence on knee joint loading, and proprioceptive deficits seem to contribute to the development or progression of knee OA(4). Sufficient quadriceps function is essential to basic activities of daily living such as rising from a chair, standing, walking, and ascending and descending stairs(5). Researchers have found correlations among quadriceps weakness, increased pain, and altered walking patterns(6). Symptom management is typically the priority in OA treatment(7), and conventional health care management of knee OA involves nonpharmacological measures—such as patient education, exercise, physiotherapy, and braces—followed by pharmaceutical management and surgery(8).
Previous research(2) has not definitively identified the cause of knee OA. Therefore, the focus of treatment for knee OA is the management of its symptoms with emphasis on self-management therapies such as exercise( 9) and complementary and alternative medicine (CAM) therapies, such as massage(10). Evidence suggests, as noted above, that the quadriceps may play a role in the disease—hence, the emphasis on massage on that muscle in the present study. Following this further, the Perlman et al. 2006 research study(11) on massage for knee, OA suggested “massage therapy is efficacious in the treatment of OA of the knee, with beneficial effects persisting for weeks following treatment cessation.”
This research provided the first examination of the beneficial use of massage therapy as a single modality in the treatment of OA of the knee. Although the trial revealed significant results, the continued use of therapist-administered massage as a regular treatment is often cost-prohibitive in the long-term, nonpharmacological self-management of knee OA. Additionally, in a recent 2012 dose-finding study, Perlman et al.(12) established, as an optimal dose, a 60-minute weekly Swedish massage as a beneficial eight-week protocol for OA of the knee.
The reported benefits of massage include breaking the pain cycle, improving function, reducing edema, promoting relaxation, and facilitating healing in various medical conditions(13). A plethora of research has explored the use of massage for lower back pain and other chronic musculoskeletal conditions(14). A primary goal of conventional treatment for knee OA is self-management of its symptoms with exercise, and research has concluded that exercise does provide benefits for people with knee OA(15). The exploration of a safe, convenient, cost-effective intervention or adjunct therapy that may reduce chronic physical symptoms and affect range of motion in knee OA is the topic addressed by this study. It has examined the effectiveness of a self-massage intervention therapy on knee pain, joint stiffness, physical functioning, and knee joint range of motion for participants diagnosed with knee OA.
METHODS
Participants
A two-group, randomized, controlled trial was conducted in a single center at the Lourdes Wellness Center, Collingswood, NJ, between September 2009 and December 2009. The Institutional Review Board of Lourdes Medical Center granted full approval of the study’s protocol, recruitment materials, and consent form. All participants provided written informed consent, acknowledge the receipt of Health Insurance Portability and Accountability (HIPPA) forms, and written diagnosis of knee OA by their health care provider before participating in the study. The intervention group continued usual care and performed a supervised self-massage intervention therapy twice weekly for eight weeks. This was followed by unsupervised self-massage intervention therapy twice weekly at home for three weeks, after which participants returned for a supervised visit on the twelfth week. The control group continued usual care only, returned for assessments at four-week intervals, and received optional dates at which times they would receive the knee self-massage training.
Men and women aged 50 years or older who possessed no limitations that prevented mobility of the knee and had a written diagnosis of OA of the knee were recruited during August and September 2009.
Recruitment was accomplished through Lourdes Wellness Center’s Fall Program Guide, a mass email mailing, and advertisements in local newspapers and on radio. Individuals were screened by telephone for the following inclusion criteria: knee pain, pain on most days of the prior month, age 50 or greater, morning stiffness lasting less than 30 minutes, crepitus on motion, and bony enlargement at affected joints(16). Additional criteria included willingness to attend 75% of scheduled self-massage sessions, agreement to practice no new exercise or stretching program, and commitment to receiving no other massage therapy during the study. Those accepted were contacted by the researcher who conducted further screening to exclude persons who had active rheumatoid arthritis or other serious medical conditions, or who had received an intra-articular knee injection of a steroid within the previous three months or a surgical procedure on either lower extremity within the past six months.
Individuals who met all inclusion criteria were invited for orientation, at which time they agreed to participate in either a self-massage or to be assigned to a wait-list group. During orientation, all consent forms, baseline assessment outcome surveys, and knee range of motion (ROM) were obtained from each participant.
Forty participants, women and men with knee OA, were recruited and then randomly assigned either to the intervention group (
n
= 21), which was designed to evaluate effects of a self-massage protocol, or the control group (
n
= 19), the members of which continued their usual care returning only for assessments. We verified that with our results (small standard deviations), this did not affect the statistical validity of a two-tailed test of intervention compared to no intervention, at 80% power.
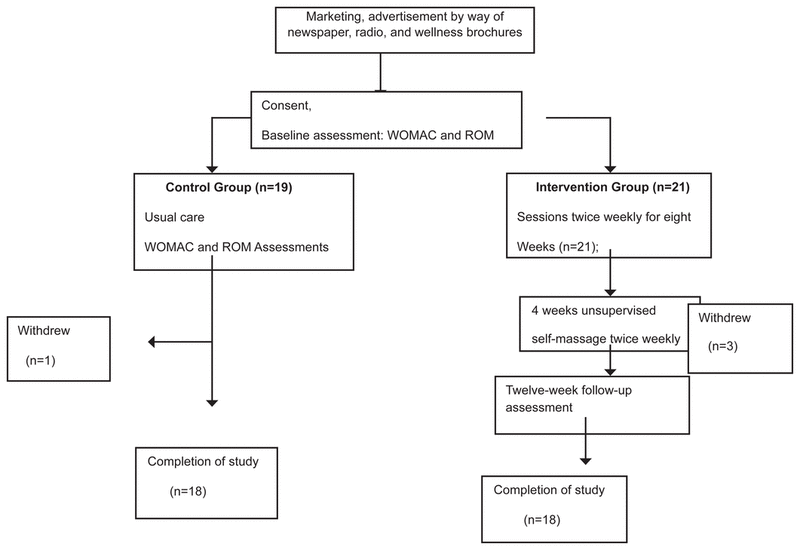
The randomization was assigned using a uniform distribution. Logically, because the current study relies on self-treatment, participants could not be blinded to group assignment. Following randomization, the participants were notified and the study began the following week. The random selection of the wait-list control group was large enough for statistical analysis. One out of the nineteen (or 5%) participants in this group dropped out of the study (see Figure 1).
| |
|
|
|
Figure 1
Flow diagram for randomized, controlled study. The self-massage intervention was conducted in a room with all seats facing a centered desk, theater style, for greater supervision, which facilitated both observation and the individual adaptations necessary in the performance of the intervention.
|
Assessments
The primary outcome measures in this study were the evaluation of the participants for changes in pain, joint stiffness, physical function, and active knee joint ROM using two instruments: 1) the self-report Western Ontario and McMaster’s Osteoarthritis Index (WOMAC) questionnaire(17), and 2) changes in knee ROM using a universal goniometer.
WOMAC subscale measurements consisted of knee pain, which encompassed questions 1 through 5. Joint stiffness involved questions 6 and 7, and physical functioning was covered by questions 8 through 24. The WOMAC instrument is an established, reliable, and validated, disease-specific, self-administered questionnaire. It assesses the perceived measurement of three subscales: pain, stiffness, and physical functioning of knee and hip OA(17). Each question is scored on a 5-point Likert scale: none-0, mild-1, moderate-2, severe-3, and extreme-4. Higher scores on the WOMAC indicate greater perceived pain, stiffness, and functional limitations.
The effect of the self-massage intervention on knee ROM, both flexion and extension, was measured using a universal goniometer with 14-inch arms. This instrument’s measurements have been tested for validity and reliability(18).
The first null hypothesis of the study was as follows: The intervention of self-massage would have no effect on the pain, stiffness, and physical functions of participants with knee OA as demonstrated in their responses to the WOMAC questionnaire.
The second null hypothesis of the study was that the self-massage intervention would have no effect on knee ROM in terms of flexion or extension as assessed using a goniometer.
The analyses of covariance (ANCOVA) were used to test differences between control and experimental groups using Statistical Package for the Social Sciences (SPSS) 20(19). This package was used to code and tabulate collected data and test the two hypotheses of WOMAC and knee ROM. Analyses of covariance (ANCOVA) were used to test differences between control and experimental groups after controlling for preexisting factors. The independent variable was grouped, with two levels—control and experimental. Twenty-eight analyses were conducted, 24 for aspects related to WOMAC measures, and four related to knee ROM measures. Postscores for each of the 28 measures were included as dependent variables in the analyses, with prescores as covariates.
Protocol
All participants in the intervention group came to Lourdes Wellness Center twice weekly (Monday and Thursday, either 2:00–3:00 p.m. or 6:00–7:00 p.m.) for eight weeks; both weekly intervention sessions had the same information and format. Research participants could select which session was more convenient and also agreed to schedule a make-up appointment within one week for any missed appointments. The supervised intervention session was one hour in length and included ten minutes for preparation, the 20-minute intervention session, 15 minutes for completion of the WOMAC written survey, and 15 minutes for individual ROM assessments. All sessions were conducted by two research therapists, one of whom narrated the scripted sequence, while the other led the intervention sequence as participants followed along. The researcher was present at all sessions. During the three-week period of at-home, unsupervised self-massage intervention, participants were encouraged to continue their twice-weekly practice of self-massage. The wait-list control group participants continued their usual care, returning for assessments at four-week intervals.
Four massage therapists who completed a 500-hour training program in massage therapy at an approved school were selected to participate. Training of research therapists included the administration of the scripted and standardized self-massage intervention, written instructions on administrating the WOMAC self-report questionnaire(20), and the measurement and recording of knee ROM procedures. Immediately after each session, all data were rechecked for accuracy for the number of subjects for each session, for missing data, or for missed recordings. The data were entered onto data sheets and then sent to the statistician.
A small randomized pilot study of 20 participants (n = 10) wait list control and (n = 10) intervention had been conducted earlier with volunteers with diagnosed knee OA to study the effects of self-massage. Participants of the intervention group in the pilot study had four weeks of supervised self-massage and four weeks of unsupervised self-massage at home. The intervention group demonstrated improvements in the WOMAC(17) pain, stiffness, and physical function and knee ROM as compared to the control group. The massage strokes chosen for this intervention in both the pilot and the study reported here were deep gliding strokes (effleurage) to soften and lengthen muscle fibers, tapping (tapotement) applied with a loose fist to stimulate circulation, and friction applied without lubricant to compress a small area while moving the tissue back and forth using short strokes around both knees’ tendon attachments(21).
The decision to choose the massage strokes and to use the quadriceps muscle was based on the muscles’ function and location in knee OA(4). The participants were asked to wear loose-fitting clothes, shorts, or skirts that allowed modest and easy access to the quadriceps muscle. A method to protect the arm from overuse or repetitive strain involved using the upper-body weight rather than the muscles of the arm for deep gliding strokes. This was achieved by extending the arm while the heel of the hand was in position and rocking forward and backward with each gliding stroke to the quadriceps, beginning at the hip and ending at the top of the knee. A five-minute warm-up of gentle stretching of shoulders, arms, and wrist is followed by ten minutes of massage strokes which included moderate to deep effleurage (gliding) and tapotement (tapping) applied to the top, lateral, and medial aspects of the quadriceps muscle, followed by friction strokes around the knee.
The room was set up theater style so that the participants faced one of the two the research therapist (RT). The RTs were trained as group facilitators and narrators of the knee self-massage intervention. One RT narrated while the other led the intervention sequence. Participants were encouraged to report any skin discolorations, swelling or adverse signs or symptoms to the researcher. Each intervention participant received a detailed handout containing instructions and illustrations of each step in the self-massage sequence (see Appendix A) during the final week in preparation for the three weeks of unsupervised, at-home intervention sessions. For the reported study, the self-massage intervention, its administration, and the narration required no modification from the pilot study.
RESULTS
Baseline demographics along with WOMAC and ROM data comparing the intervention group to the control group are presented in Table 1. The Wilcoxon rank-sum test was used to compare continuous and ordinal variables, and Fisher’s exact test was used to compare discrete variables. There is an insignificant p-value for all variables at the 5% significance level, which means that the intervention and control groups came from the same population and were appropriate for the comparison of results of the participants in the two arms of this study. This determines whether participants in the self-massage intervention therapy arm had improved pain level, diminution of joint stiffness, improved physical functioning, and improved ROM at the conclusion of the study period.
Table 1
Self-Massage Therapy Study Baseline Demographics of Evaluable Participants in the Intervention Group Compared to the Control Group
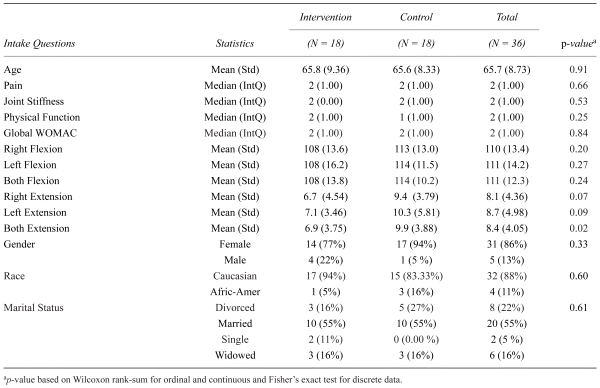
The average age of the participants was 66. Participants resided in the South Jersey area within a 20-mile radius of Collingswood, NJ. The majority of these participants were female (86%) and Caucasian (89%). The scores for pain level, joint stiffness, and physical functioning of the knees at baseline were moderate. The average range of motion at baseline for right flexion and left flexion was 108°. The average ROM at baseline for right extension was 6.7° and left extension was 7.1°.
Summary of Findings
The post-treatment outcome measures of the differences between control and intervention groups in the data from the self-reported measures of pain, stiffness, function, and total mean of WOMAC scores were statistically significant; the lower scores in the figures indicate improvement of symptoms. There was no difference between the groups in knee ROM. Specifically, the significant differences between control and experimental groups on pain, stiffness, physical function, and total mean WOMAC mean scores are outlined in the following paragraphs.
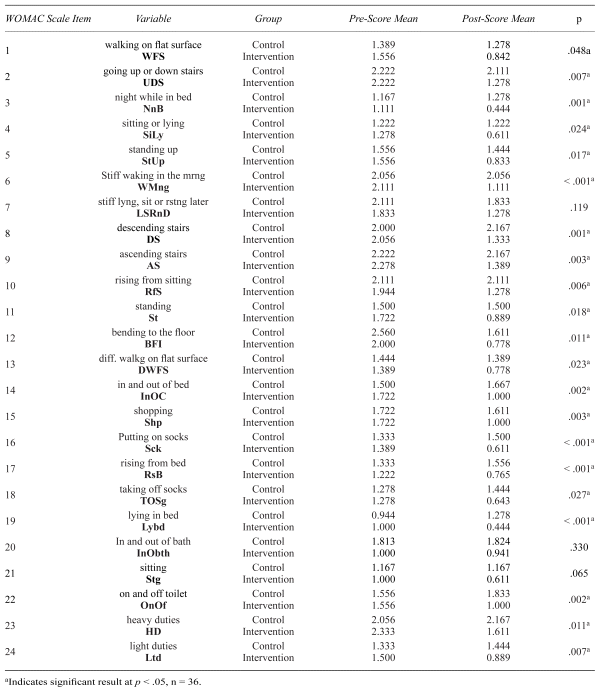
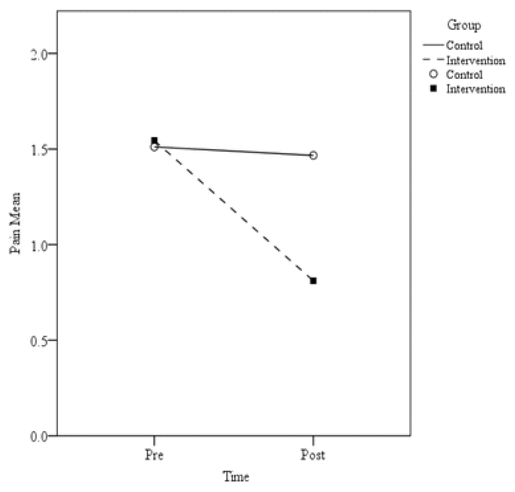
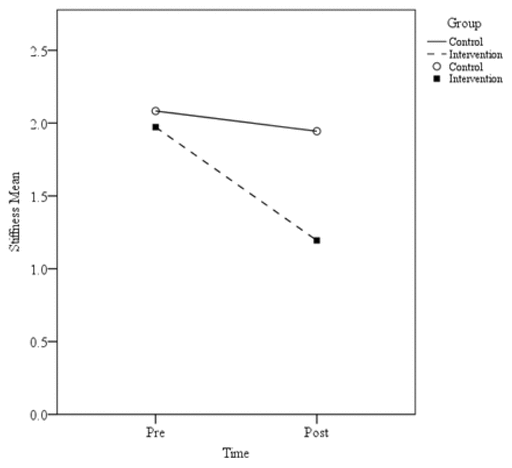
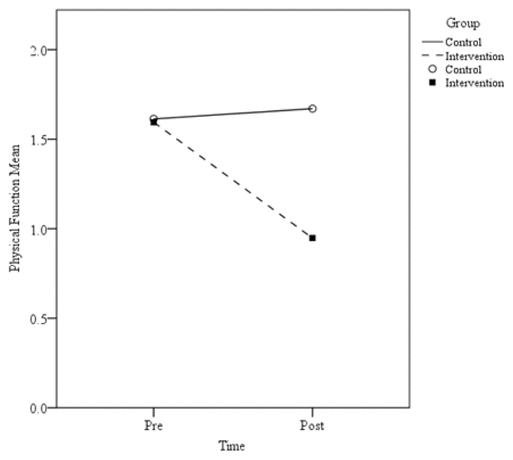
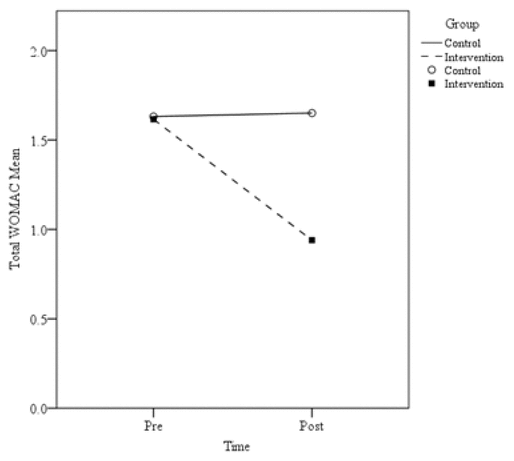
The measures of pain showed significant differences between control and intervention groups in postscore walking on flat surface, postscore ascending or descending stairs, postscore at night while in bed, postscore sitting or lying, and postscore standing up (Table 2, Figure 2). For stiffness, significant differences between groups were observed for postscore first waking in the morning and postscore lying, sitting, or resting later in the day (Table 2, Figure 3). The results showed significant differences in physical function, including highly significant results for postscore descending stairs, ascending stairs, rising from sitting, getting in and out of bed, going shopping, putting on socks, rising from bed, lying in bed, getting on and off toilet, and light domestic duties (Table 2, Figure 4). WOMAC total mean score improved significantly in post-treatment compared to control (Table 2, Figure 5).
Table 2
Summary of Pre-Post–WOMAC ANCOVA Analyses Comparing Intervention and Control Groups
| |
|
|
|
Figure 2
Knee pain mean pre- and postscores. Lower scores indicate perceived improvement in pain.
|
| |
|
|
|
Figure 3
Knee stiffness mean pre- and postscores.
|
| |
|
|
|
Figure 4
Physical function mean pre- and postscores.
|
| |
|
|
|
Figure 5
Total mean WOMAC pre- and postscores.
|
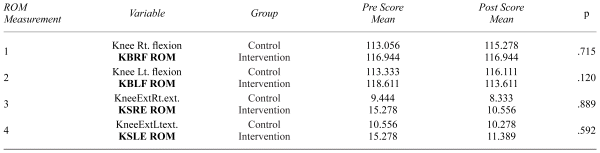
In knee ROM, the study found no significant difference in postscore knee bent right and left flexion and extension, with
p
> .05 in all cases (Table 3, Figures 6 and 7).
Table 3
Summary of Pre-Post–ROM ANCOVA Analyses Comparing Intervention and Control Groups
| |
|
|
|
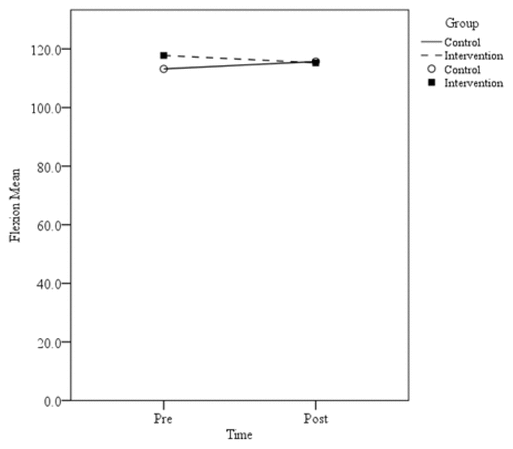
Figure 6
Mean knee ROM flexion scores.
|
| |
|
|
|
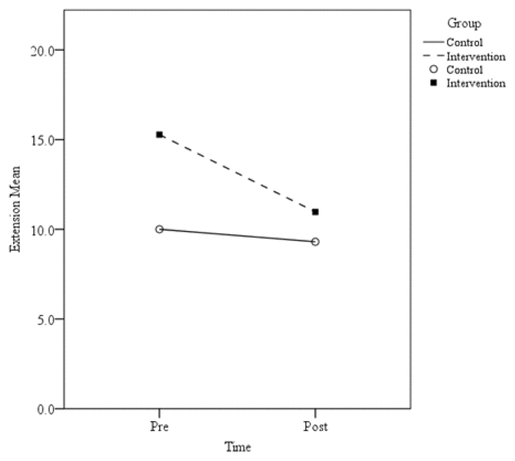
Figure 7
Mean knee ROM extension scores.
|
DISCUSSION
This is the first randomized, controlled trial on the effects of a self-massage protocol applied to the quadriceps muscle on adults with knee OA. The results of the study indicated that at intake, median WOMAC measurements of three subscales (pain, stiffness, and physical function) did not differ between intervention and control groups (Table 1). Intervention and control groups did, however, differ on mean intake levels of ROM extension (Table 1). The ANCOVA analyses were used to test for differences in postscores between the control and experimental groups after controlling for preexisting factors. The results revealed a significant difference in mean postscores between the control and experimental groups in 21 out of 24 WOMAC subscales (Table 2). Thus, the null hypothesis was rejected. The symptoms in the WOMAC subscales most significantly improved by the between-group analysis (
p
= .001) were pain at night while in bed; stiffness when waking in the morning; and physical functions of descending stairs, putting on socks, rising from bed, and lying in bed. On the other hand in Table 2, self-massage results in the between-group analysis showed no significant results in stiffness while lying, sitting, or resting later in the day; getting in and out of the bath; or difficulty in sitting.
The ANCOVA analysis of the null hypothesis measurements 1–4 revealed no difference in post-ROM scores between control and experimental groups after controlling for pre-ROM (Table 3). ROM scores among the control group were slightly lower than those for the intervention group. Knee bent right flexion remained static among the intervention group and went up slightly for the control group. While knee bent left flexion increased slightly for controls, it went down slightly for those in the intervention group; however, this change in scores was not large enough to be significant. Both knee straight right extension and knee straight left extension decreased for both groups, but no significant difference in change was found.
There are various factors that may contribute to this study’s difference in ROM between group results. First, the study population consisted of participants with varying symptoms of pain and stiffness of the knee in one or both knees(22), possibly affecting their ROM. Second, the intra-and interrater reliability of the knee ROM measurements were not tested, possibly creating a bias with measurements(18). Finally, previously mentioned research on the effects of massage for knee OA used knee ROM as a secondary outcome measure and observed the groups ROM did change in a positive direction though not significant(12). The relationship between the slight decrease in both knees extension indicates some improvement, according to researchers in
Measurement of Joint Motion: A Guide to Goniometry
(18,p.42): “extension limitations greater than 5° in adults may be considered as knee flexion contractures.” Additionally, researchers found in a study measuring the knee ROM among nursing home residents that 33% of the subjects had bilateral knee extension limitations of 5° and 42% had greater than 10° of extension limitations causing flexion contractures that may affect mobility(18). As was previously stated in the present study, researchers have found correlations between the role of the quadriceps muscle and the role of its weakness to increased pain and altered walking patterns. In conclusion, insignificant ROM results may have some beneficial effect on knee extension and affect mobility. Future research with larger samples may consider looking at what effect self-massage has on knee ROM and mobility.
Self-massage provides a self-administered, on-demand massage therapy that may meet an ongoing need for symptom relief. The significant results of this randomized self-massage study may be attributed to the administering of the twice weekly study in a supervised group setting, ensuring proper technique and compliance. Additionally, the expectation of its benefits may also contribute to its nonspecific effects. Second, the sequences were narrated and demonstrated by certified research therapists who observed participants throughout the first series of eight-week sessions and thus ensured adherence. Lastly, following each session, the WOMAC questionnaire and ROM measurement were completed, allowing participants to experience the immediate sensation of self-touch and its possible effects on ambulation.
The underlying mechanism of the action of massage is not well understood(23)—early research reviewed physiological benefits to include increasing blood flow(24); however, more recent studies using Doppler ultrasound techniques have found the use of massage had no effect on venous or arterial blood flow(25). Following this further, theories that support massage therapy’s influence on lymph drainage to remove waste and reduce edema are reflected in anecdotal accounts and empirical evidence, and conclusive research is needed(26). On the other hand, massage therapy has been shown to relieve musculoskeletal pain. In a meta-analysis on the effects of massage therapy, 37 studies yielded a number of theories; one which may be applicable here was in the multiple-dose effects category. Weeks after massage treatments ended, pain levels averaged lower on assessment, perhaps indicating the potential on-going benefits after a series of massage sessions(27). Finally, self-massage research is in its early stages; thus, there is little research to support its therapeutic value. However, two studies on the benefit of massage for hand arthritis(28) and carpal tunnel(29) have incorporated the use of self-massage in the studies. Even though its exact mechanism of action is unknown, our findings indicate self-massage applied to the quadriceps muscle resulted in significant WOMAC improvements in knee pain, stiffness, and physical function in the intervention group in all subsets. This on-demand, natural, economical self-help therapy may be examined in future massage therapy research. Potentially, the 4.3 million people in the USA with knee OA may benefit from this model as an option for self-managing arthritic knee symptoms.
In this paper we have examined the effects of a single intervention self-massage applied to the quadriceps muscle, evaluated by the WOMAC questionnaire and knee ROM. The WOMAC index is a widely used disease specific evaluation of the important changes in health status that occurs as a result of an intervention. The potential benefits of the self-massage intervention were further supported in this study when the WOMAC total scores demonstrated highly significant improvement from baseline as compared to the control group. The observed improvements are most likely attributed to the knee self-massage intervention, study design, random assignment to groups, and lack of improvement in the control group. In addition, the benefits of the intervention were achieved in 12 weeks. It is easy to see these findings may have important implications for self-management and preventative options for those with knee OA.
The limitations of the study’s design were the following issues. First, trials with blinded participants, researchers, or research therapists were not possible in a group-setting intervention. Second, research assistants’ attention in and concern for the study participants could have stimulated nonspecific effects and general optimism (i.e., the Hawthorne effect(30)). Third, given that the WOMAC self-report was administered after each intervention, response bias may have occurred when participants responded to the same survey questions repeatedly. Finally, the study included a three-week at home follow-up period in which the participants were encouraged to continue the intervention. In this situation it was difficult to ensure compliance in the study.
Despite the limitations discussed above, the strengths of the study included the use of reliable and validated outcome instruments, the WOMAC and goniometer; the randomization of the study participants; and control group adherence. Equally important, the opportunity that the participants had to select the session in which they chose to participate—afternoon or evening—may have affected attendance and participation in a positive way. Finally, these strengths resulted in strong statistical support that a simple intervention, as described here and administered in a group setting, is something that with relative minimal training and efficient use of practitioner time, can provide effective increases in important quality of life measures for persons with osteoarthritis of the knee.
CONCLUSION
While this is the first evidence-based research on self-massage therapy for knee OA, there appears to be a relationship between self-massage interventions on the quadriceps muscle performed twice a week over 12 weeks and the statistically significant improvement in the condition in the intervention group over baseline. This study contributes to the emerging evidence-based massage research into self-massage. This category of massage is patient-centered, benefiting patients who are seeking active solutions for chronic symptoms related to knee OA.
Our research study provides a contribution which may have important implications for future research, particularly in terms of managing knee pain, stiffness, and physical function in knee OA.
Future research with a larger cohort is needed to determine the efficacy and effectiveness of self-massage in the general population. The results here also suggest the need for further studies which might look at the value of the intervention over a longer period of time to determine whether there are any lasting benefits and whether continuing the intervention affects long-term outcomes. Finally, long-term follow-up studies of self-massage for knee OA to assess adherence, use of medication, and disease progression are also warranted.
CONFLICT OF INTEREST NOTIFICATION
The authors declare there are no conflicts of interest.
APPENDICES
Self-massage Sequence
Appendix A
(View the PowerPoint presentation, uploaded to the website as Supplementary Materials.)
REFERENCES
1 Dillon CF, Rasch EK, Gu Q, et al. Prevalence of knee osteoarthritis in the United States: arthritis data from the Third National Health and Nutrition Examination Survey, 1991–94. J Rheumatol. 2006;33(11):2271–2279.
2 McAlindon T. The knee. Bailliere Clin Rheumatol. 1999; 13(2):333.
3 Lawrence R, Felson DT, Helmick CG, et al. Estimates of the prevalence of arthritis and other rheumatic conditions in the United States. Part II. Arthritis Rheum. 2008;58(1):26–35.

4 Bennell KL, Hunt MA, Lim BW, et al. Role of muscle in the genesis and management of knee osteoarthritis. Rheum Dis Clin North Am. 2008;34(3):731–754.

5 Hurley MV. The role of muscle weakness in the pathogenesis of osteoarthritis. Rheum Dis Clin of North Am. 1999;25(2):283–298.

6 Sharma L, Dunlap D, Cahue S, et al. Quadriceps strength and osteoarthritis: progression in malaligned and lax knees. Ann Intern Med. 2003;138(8):613–619.
7 Hunter D, Felson D. Osteoarthritis. BMJ. 2006;332:639.


8 Katz, WA. Themed Review: Nonpharmacologic approaches to osteoarthritis. Am J Lifestyle Med. 2007;1(4):249–255.

9 Deyle G, Allison SC, Matekel RL, et al. Physical therapy treatment effectiveness for osteoarthritis of the knee: a randomized comparison of supervised clinical exercise and manual therapy procedures versus a home exercise program. Phys Ther. 2005;85(12):1301–1307.
10 Brandt KD. Non-surgical treatment of osteoarthritis: a half century of “advances.” Ann Rheum Dis. 2004;63(2):117–122.

11 Perlman A, Sabina A, Williams AL, et al. Massage therapy for osteoarthritis of the knee. Arch Int Med. 2006;166(22):2533–1538.

12 Perlman A, Ali A, Njike Y, et al. Massage therapy for osteoarthritis of the knee: a randomized dose-finding trial. PLoS One. 2012;7(2):1–8.

13 Cassar MP. The Handbook of Clinical Massage: a Complete Guide for Students and Professionals New York, NY: Churchill Livingstone; 1999.
14 Furlan AD, Brosseau L, Imamura M, et al. Massage for low-back pain: a systematic review within the framework of the Cochrane Collaboration Back Review Group. Spine. 2002;27(17):1896–1910.

15 Van Barr M, Dekker J, Oostendorph R, et al. Effectiveness of exercise in patients with osteoarthritis of hip or knee: nine months’ follow up. Ann Rheum Dis. 2001;60(12):1123–1130.

16 Hochberg M, Altman R, Brandt K, et al. Guidelines for the medical management of osteoarthritis: Part II. Osteoarthritis of the knee. Arthritis Rheum. 1995;38(11):1541–1546.

17 Bellamy N, Buchanan WW, Goldsmith C, et al. Validation study of WOMAC: a health status instrument of measuring clinically important patient relevant outcomes to antirheumatic drug therapy in patients with osteoarthritis of the hip or knee. J Rheumantol. 1988;15(12):1833–1840.
18 Norkin C, White DJ. Measurement of Joint Motion: a Guide to Goniometry, 3rd ed. Philadelphia, PA: F. A. Davis Company; 2003.
19 Tabachnick BG, Fidell LS. Using Multivariate Statistics, 5th ed. Boston, MA: Pearson; 2007.
20 Bellamy, N. WOMAC Osteoarthritis Index User Guide. London, Ontario, Canada: 1995.
21 Clay CJH, Pounds DM. Basic Massage Therapy: Integrating Anatomy and Treatment. New York, NY: Lippincott Williams and Wilkins; 2003.
22 Holla J, van der Leeden M, Roorda L, et al. Diagnostic accuracy of range of motion measurements in early symptomatic hip and/ or knee osteoarthritis. Arthritis Care & Res. 2012:64(1):59–65.

23 Field T, Hernandez-Reif M, Diego M, et al. Cortisol decreases and serotonin and dopamine increase following massage therapy. Int J Neurosci. 2005;115(10):1397–1413.

24 Goats G. Massage – the scientific basis of an ancient art: part 2. Physiological and therapeutic effects. Br J Sports Med. 1994;28(3):153–156.

25 Robertson A, Watt JM, Galloway SD. Effects of leg massage on recovery from high intensity cycling exercise. Br J Sports Med. 2004;38(2):173–176.

26 Tidus P. A review of human massage therapy: assessing effectiveness primarily from empirical data in the human species. AAEP Proceedings. AAEP. 2000;46:302–305.
27 Moyer C, Rounds M, Hannum JW, et al. A meta-analysis of massage therapy research. Psychol Bull. 2004:130(1):3–18.

28 Field T, Diego M, Hernandez-Reif M, et al. Hand arthritis pain is reduced by massage therapy. J Bodyw Mov Ther. 2007;11(1):21–24.

29 Field T, Diego M, Cullen C, et al. Carpal tunnel syndrome symptoms are lessened following massage therapy. J Bodyw Mov Ther. 2004;8(1):9–14.

30 McCarney R, Warner J, Iliffe S, et al. The Hawthorne effect: a randomized, controlled trial. BMC Med Res Methodol. 2007;7(1):1–8.

Corresponding author: Dorothea V. Atkins, ThD, RN, Holos University Graduate Seminary, 20 Sussex Ave., Voorhees, NJ 08043, USA, E-mail: dmassage1@comcast.net
(Return to Top)
COPYRIGHT
Published under the CreativeCommons Attribution NonCommercial-NoDerivs 3.0 License. (
Return to Text
)
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK
, VOLUME
6
, NUMBER
1
,
March 2013