
Alison Fraser, RMT1*
1West Coast College of Massage Therapy, Victoria, British Columbia, Canada
Introduction
Dissociation is a transdiagnostic phenomenon common among trauma survivors. Key characteristics include depersonalization, derealization, absorption, and amnesia. Chronic dissociation is correlated with autonomic nervous system hypoarousal and other neurophysiological adaptations that impact survivors’ ability to make gains in conventional psychotherapy. Therapeutic massage has demonstrated stimulatory effects on cortical regions that exhibit functional dysregulation in dissociation and post-traumatic stress disorder (PTSD). This case study explored whether therapeutic massage and homecare could reduce persistent dissociation in a client with PTSD.
Case presentation
The study participant was a 35-year-old Indigenous female who was diagnosed with PTSD at age 18. Intake assessment via the Dissociative Experiences Scale-II (DES-II) confirmed pathological levels of dissociation consistent with PTSD. Intervention comprised 10 sessions conducted by a massage therapy student over a period of 12 weeks. Each session included an initial interview, therapeutic massage, homecare prescription, and closing interview. Manual techniques were selected to promote parasympathetic tone while providing tactile stimuli; homecare techniques were selected to promote conscious proprioception. Dissociative progress was evaluated using four discrete DES-II samples, while somatic awareness was assessed during structured, 15-min massage periods in each session. Both tracked indicators showed improvement with intervention, with DES-II scores decreasing by 53.7% from initial baseline, and real-time awareness of somatic stimuli improving by 78%. These improvements were consistent with the participant’s subjective reports of increased somatosensory awareness.
Discussion
As a low-risk intervention, therapeutic massage shows promise as an adjunct therapy in PTSD recovery. While the participant demonstrated improvements in tracked indicators, further research is needed to isolate the effects of massage from those of homecare exercises and the data collection process itself. Collaboration with psychiatry would enhance future study rigor by incorporating diagnostic assessments beyond the scope of massage therapy.
KEYWORDS: Massage therapy; stress disorders, post-traumatic; dissociative disorders; complementary therapies; psychophysiologic disorders; PTSD
Post-traumatic stress disorder (PTSD) affects approximately 3.9% of citizens globally, with few patients receiving specialized treatment.(1) Diagnostic features of PTSD include hyperarousal and alterations in mood and cognition.(2) Dissociation, a disruption in memory, perception, identity, and consciousness,(2) is pervasively comorbid, affecting up to 48% of individuals with PTSD.(3) Dissociation ranges from mild detachment to intense amnesia, depersonalization (the feeling of observing oneself from outside the body), and derealization (feeling that surroundings are unreal).(2)
Effective treatment for PTSD remains elusive. Non-pharmacological interventions center on cognitive-based psychotherapies,(4,5) which rely on survivors’ capacity for learning, memory formation, and emotional regulation. Simultaneously, neuroimaging studies of PTSD have identified structural and functional alterations in the prefrontal cortex, hippocampus, and amygdala,(6,7) regions which are crucial to learning, memory formation, and sensory and emotional processing.
As stand-alone interventions for PTSD, cognitive therapies yield poor results: only one-third of patients achieve remission with initial treatment, and most relapse within 1 year.(8) As a predictor for non-response in psychotherapy, dissociation further complicates recovery(9–11); it is often among clinical trials’ exclusion criteria,(4) creating systematic bias and underrepresentation in current literature. Dissociation remains under-researched, with minimal targeted interventions.
Though further research is needed, studies suggest dissociation may reflect central nervous system hypoarousal.(12) Therapeutic massage is a promising adjunct, promoting neuroplastic changes(13) and increasing cortical activity in regions involved in sensory integration,(8) collectively helping temper limbic system activity.(9)
This prospective case study examines the effects of massage therapy on dissociation in a 35-year-old female with PTSD.
This study was conducted in accordance with the Second Edition of the Tri-Council Policy Statement: Ethical Conduct for Research Involving Humans.(14) This report was prepared in accordance with CARE guidelines, adapted for therapeutic massage.(15)
Participants with a formal diagnosis of PTSD with concurrent dissociation were recruited through advertisement. Exclusion criteria included multifactorial or unstable psychiatric conditions, contraindications for massage therapy, and impaired capacity to provide informed consent. Written consent was obtained from the selected participant prior to the study commencing.
The client was a 35-year-old Indigenous female, generally in good health, who had completed post-graduate studies. She identified as an intergenerational survivor of the Canadian residential school system. She described a positive relationship with her spouse and preschool-aged child, alongside stable housing and employment.
The client was diagnosed with PTSD at age 18, with a history of episodic depression, most recently 8 years prior to this study. Ongoing symptoms included hypervigilance, anxiety, and brain fog. She reported persistent dissociation, describing herself as a “floating head” with minimal somatosensory awareness below the neck.
The client described a history of developmental, medical, childbirth, and assault-related traumas, noting an incremental increase in PTSD symptoms with each event. Significant traumas included emergency appendectomy, strangulation and sexual assault, and birthing complications.
Since her PTSD diagnosis, the client had been under the care of two psychiatrists, expressing high regard for both. She had declined pharmaceutical treatment. She was discharged from her last psychiatrist’s care when his practice closed 2 months prior to this study. Despite 17 years of psychiatric care, she continued to struggle with daily symptoms of PTSD.
Sensory testing was conducted pursuant to the protocols detailed by Rattray & Ludwig,(16) to rule out peripheral nerve lesions and impairment in cutaneous receptors and spinothalamic and posterior column–medial lemniscus pathways. The client correctly identified all stimuli detailed in Table 1.
Table 1 Functional Assessment of Cutaneous Receptors and Ascending Spinal Tracts
Two-point discrimination was assessed along select dermatomes to screen for tactile agnosia despite intact afferent pathways. The client could not distinguish between single and two-point contact with a handheld tool calibrated to 2 cm. Upon recalibration to 3 cm, she correctly identified only 2 of 30, two-point stimuli (6.7%) but correctly identified all 30 single-point stimuli. This test was repeated immediately before the final treatment session to assess progress.
Dissociative markers were tracked using the Dissociative Experiences Scale-II (DESII), a psychometric instrument with high validity and reliability (test–retest = 0.79 < r < 0.84, and Cronbach’s α = 0.95),(17) alongside “high convergent validity with other dissociation measures” (mean Cohen’s d = 1.82; N = 5916).(18) Effective treatment of dissociation is expected to decrease DES-II mean scores.(17)
The DES-II was administered four times in total: 10 days prior to the study commencing; immediately prior to session 6; immediately following the 10th and final session; and finally 1 month after the study’s conclusion. The client remained blinded to calculated scores on the DES-II throughout.
The client was provided with a handheld tally counter to be used during the first 15 min of each treatment session. She was instructed to activate the counter whenever she perceived a difference in sensation, such as touch or pressure, without interpreting or analyzing these sensations. She was instructed to focus on how various regions might experience the same stimuli differently or respond uniquely to directional variations of techniques. Care was taken to avoid implying expected outcomes.
During each 15-min sample period, tactile contrast was introduced through variations in pressure, depth, rate, and direction (e.g., caudal versus cephalad) of manual technique application. Efforts were made to provide a consistent degree of tactile contrast across sessions. The client remained blinded to the tally counts throughout the study.
Ten 75-min sessions were conducted over a 12-week intervention period in the intern clinic of an accredited registered massage therapy (RMT) college. Sessions were conducted by a massage therapy student in their fourth term of study.
Each session began with an interview regarding the client’s physical state during the preceding week. The client was encouraged to share her observations on the previous treatment session and homecare. Physical complaints were assessed to ensure safe, therapeutic treatment. Massage techniques were then selected to alleviate regions of discomfort and promote parasympathetic tone and somatic awareness,(19) as detailed in Tables 2 and 3. Techniques were performed slowly and rhythmically to further encourage parasympathetic tone.(16) Verbal informed consent was obtained prior to assessment and treatment in each session.
Table 2 Treatment Administered: First 25a Min of Each Treatment
Table 3 Treatment Administered: Final 20–35a Min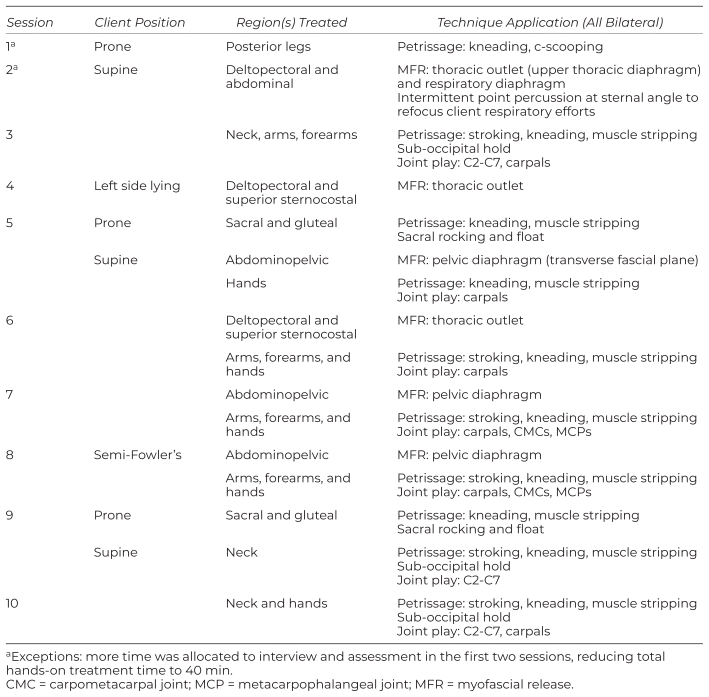
The first 25a min of treatment targeted the posterior thorax and shoulders in prone (Table 2). Thereafter, varying regions were treated to address identified areas of discomfort (Table 3); petrissage pressure varied from light to moderate per local tissue presentation.
During intake, the client expressed concern about unexpected touch provoking anxiety. To address this, the therapist and client agreed on a verbal cue of “hands coming on” to be provided before each initiation of contact.
The client was periodically prompted to focus on the area being treated, compare sensations, or visualize the distance between contact points while practicing diaphragmatic breathing. Each session concluded with a brief exit interview to obtain the client’s immediate observations and provide homecare recommendations.
Homecare was structured to progressively enhance proprioceptive awareness across body regions, leveraging the client’s background in yoga and meditation. Since she identified her cervical region as a transition point where awareness declined, initial exercises targeted this area to reinforce conscious proprioception before expanding distally. Each activity built sequentially upon the previous one.
Instruction emphasized slow, comfortable mid-range movements with attention to sensations of stretch, crepitus, or asymmetry. The client was advised to discontinue any activity provoking pain or distress, and was observed demonstrating each exercise to ensure safe biomechanics. Activity details and rationale are provided in Table 4.
Table 4 Homecare Prescription by Session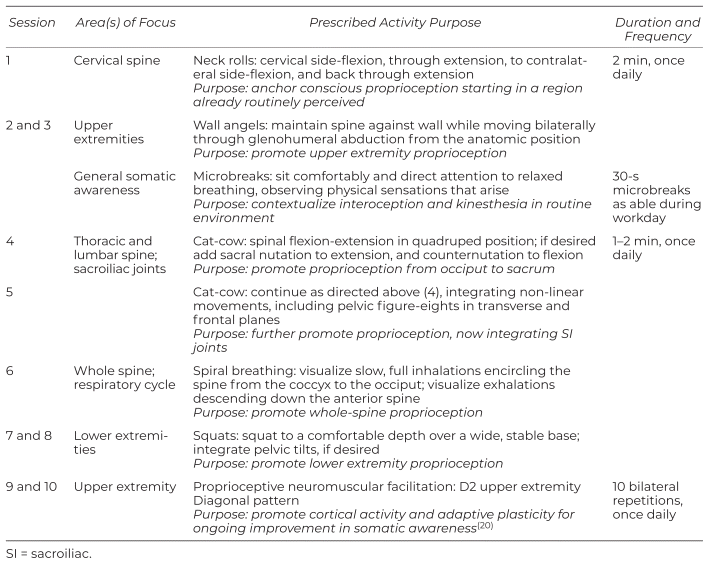
Specific duration and frequency were recommended for each activity, but rigidity was dispensed with from session 5 onward. To better promote somatic awareness, the client was encouraged to observe for signs of mental or physical fatigue in lieu of adhering to prescribed intervals. The client performed homecare as directed, with only minor deviations in duration and frequency.
Starting in session 3, the client reported a “somatic breakthrough,” whereby she experienced increasing awareness of sensations in her upper thoracic region, both anterior and posterior. This awareness continued to increase throughout the study. By the study’s conclusion, the client reported sustained improvements in general well-being, somatic awareness, and “brain fog.” She felt progressively safer and “more grounded” in her daily life, and reported increased patience when parenting. She also reported increased emotional and physical fatigue, potentially signaling a depressive relapse, which she attributed to stress both at home and at work.
On initial testing of two-point discrimination, the client was able to correctly identify only 2 of 30 stimuli; at the 10th session, she correctly identified 14 out of 34, two-point stimuli, for a 34.5% improvement in accuracy.
Baseline scoring on the DES-II was 34.11, consistent with PTSD and “high levels of dissociation.”(17) At the final session (week 12), scoring decreased to 17.15; at 1-month follow-up, scoring further decreased to 15.79, for an overall improvement of 53.7% from baseline.
Three elements of the DES-II were identified as having strong misfit, with marked deviations from Rasch model expectations(21); exclusion of these elements improves reliability and measurement invariance. Accordingly, scoring was recalculated, producing adjusted scores of 34.20 at baseline, 16.61 at week 12, and 14.48 at 1-month follow-up (Figure 1).
|
| ||
|
Figure 1 DES-II mean scores. | ||
High variance was observed in response ranges among DES-II elements. Four-factor analysis was performed,(22) revealing maximal improvement in absorption for both raw and adjusted datasets (Figure 2).
|
| ||
|
Figure 2 DES-II mean ranges by factor. | ||
During the first session’s sample period, the client activated the tally counter 40 times, primarily during upper thoracic treatment. By session 5, she was activating the counter with greater frequency and uniformity during the sample period. Tally counts peaked at 71 in the final session, representing a 78% improvement from baseline (Figure 3).
|
| ||
|
Figure 3 Somatosensory cognizane over time. | ||
In the week preceding session 5, the client and her community were deeply impacted by the discovery of mass graves at a former residential school site; this event had a lasting impact on her emotional state through the remainder of the study.
Improvement in the client’s DES-II scores suggested a clinically significant reduction in dissociation.(17) Real-time somatic awareness and two-point discrimination suggested improved somatosensory integration. Subjective client reports should be considered alongside codified data in evaluating mental health interventions. The client described increased somatosensory awareness but also reported heightened symptoms she associated with a potential depressive relapse.
Dissociation inherently involves non-awareness, and the data collection methods and homecare prescribed in this study promoted mindfulness and introspection, practices shown to modulate limbic activity in patients with PTSD.(23) As such, it is impossible to isolate dissociative improvements owing to therapeutic massage from gains attributable to homecare and/or the data collection process itself, warranting cautious interpretation.
Efforts were made to optimize reliability and validity; systematic bias was minimized via blinding the client to quantitative results throughout. Algebraic analyses of limited datasets risk introducing bias; ordinal analysis with referential comparisons may be more suitable. Given n = 1 herein, inferential conclusions are inappropriate.
Given recorded improvements across all tracked indicators, further studies on therapeutic massage for dissociation appear both safe and feasible. To more accurately determine the efficacy of therapeutic massage, future studies should exclude homecare.
Despite the low-risk profile of therapeutic massage as an adjunct intervention, structured collaborations with psychiatry would improve study safety via concurrent monitoring of PTSD while strengthening research rigor through diagnostic assessments beyond the scope of massage therapy.
No acknowledgments are included as this study was conducted independently, and the case subject remains anonymous to protect privacy.
The author declares there are no conflicts of interest.
This study received no external funding.
1. Koenen KC, Ratanatharathorn A, Ng L, McLaughlin KA, Bromet EJ, Stein DJ, et al. Posttraumatic stress disorder in the World Mental Health Surveys. Psychol Med. 2017;47(13):2260–2274. https://doi.org/10.1017/S0033291717000708
Crossref PubMed PMC
2. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. American Psychiatric Association; 2013. https://doi.org/10.1176/appi.books.9780890425596
3. White WF, Burgess A, Dalgleish T, Halligan S, Hiller R, Oxley A, et al. Prevalence of the dissociative subtype of post-traumatic stress disorder: a systematic review and meta-analysis. Psychol Med. 2022;52(9):1629–1644. https://doi.org/10.1017/S0033291722001647
Crossref PubMed
4. Katzman MA, Bleau P, Blier P, Chokka P, Kjernisted K, Van Ameringen M, et al. Canadian clinical practice guidelines for the management of anxiety, posttraumatic stress and obsessive-compulsive disorders. BMC Psychiatry. 2014;14(Suppl 1):S1. https://doi.org/10.1186/1471-244X-14-S1-S1
Crossref PubMed PMC
5. Schrader C, Ross A. A review of PTSD and current treatment strategies. Mo Med. 2021;118(6): 546–551.
PubMed PMC
6. Harnett NG, Goodman AM, Knight DC. PTSD-related neuroimaging abnormalities in brain function, structure, and biochemistry. Exp Neurol. 2020;330:113331. https://doi.org/10.1016/j.expneurol.2020.113331
Crossref PubMed
7. Deppermann S, Storchak H, Fallgatter AJ, Ehlis AC. Stress-induced neuroplasticity: (mal)adaptation to adverse life events in patients with PTSD – a critical overview. Neuroscience. 2014;283:166–177. https://doi.org/10.1016/j.neuroscience.2014.08.037
Crossref PubMed
8. Rapaport MH, Schettler PJ, Larson ER, Carroll D, Sharenko M, Nettles J, et al. Massage therapy for psychiatric disorders. Focus (Am Psychiatr Publ). 2018;16(1):24–31. https://doi.org/10.1176/appi.focus.20170043
PubMed PMC
9. Bae H, Kim D, Park YC. Dissociation predicts treatment response in eye-movement desensitization and reprocessing for posttraumatic stress disorder. J Trauma Dissociation. 2016;17(1):112–130. https://doi.org/10.1080/15299732.2015.1037039
Crossref
10. Kleindienst N, Limberger MF, Ebner-Priemer UW, Keibel-Mauchnik J, Dyer A, Berger M, et al. Dissociation predicts poor response to dialectial behavioral therapy in female patients with borderline personality disorder. J Pers Disord. 2011;25(4):432–447. https://doi.org/10.1521/pedi.2011.25.4.432
Crossref PubMed
11. Kleindienst N, Priebe K, Görg N, Dyer A, Steil R, Lyssenko L, et al. State dissociation moderates response to dialectical behavior therapy for posttraumatic stress disorder in women with and without borderline personality disorder. Eur J Psychotraumatol. 2016;7:30375. https://doi.org/10.3402/ejpt.v7.30375
Crossref PubMed PMC
12. Beutler S, Mertens YL, Ladner L, Schellong J, Croy I, Daniels JK. Trauma-related dissociation and the autonomic nervous system: a systematic literature review of psychophysiological correlates of dissociative experiencing in PTSD patients. Eur J Psychotraumatol. 2022;13(2):2132599. https://doi.org/10.1080/20008066.2022.2132599
Crossref PubMed PMC
13. Xing XX, Zheng MX, Hua XY, Ma SJ, Ma ZZ, Xu JG. Brain plasticity after peripheral nerve injury treatment with massage therapy based on resting-state functional magnetic resonance imaging. Neural Regen Res. 2021;16(2):388–393. https://doi.org/10.4103/1673-5374.290912
Crossref PMC
14. Tri-council Policy Statement: Ethical Conduct for Research Involving Humans – TCPS 2 (2022). Ethics.gc.ca; 2023. Accessed November 25, 2024. Available from: https://ethics.gc.ca/eng/policy-politique_tcps2-eptc2_2022.html.
15. Munk N, Boulanger K. Adaptation of the CARE guidelines for therapeutic massage and bodywork publications: efforts to improve the impact of case reports. Int J Ther Massage Bodywork. 2014;7(3): 32–40. https://doi.org/10.3822/ijtmb.v7i3.251
PubMed PMC
16. Rattray F, Ludwig L. Sensory testing. In: Clinical Massage Therapy: Understanding, Assessing and Treating Over 70 Conditions. Talus Inc; 2000: 1124–1126.
17. Carlson EB, Putnam FW. An update on the dissociative experiences scale. Dissociation. 1993;6(1): 16–27.
18. Lyssenko L, Schmahl C, Bockhacker L, Vonderlin R, Bohus M, Kleindienst N. Dissociation in psychiatric disorders: a meta-analysis of studies using the dissociative experiences scale. Am J Psychiatry. 2018;175(1):37–46. https://doi.org/10.1176/appi.ajp.2017.17010025
Crossref
19. Andrade CK. Outcome-Based Massage: Putting Evidence into Practice. 3rd ed. Lippincott Williams and Wilkins; 2013.
20. Moreira R, Lial L, Teles Monteiro MG, Aragão A, Santos David L, Coertjens M, et al. Diagonal movement of the upper limb produces greater adaptive plasticity than sagittal plane flexion in the shoulder. Neurosci Lett. 2017;643:8–15. https://doi.org/10.1016/j.neulet.2017.02.022
Crossref PubMed
21. Saggino A, Molinengo G, Rogier G, Garofalo C, Loera B, Tommasi M, et al. Improving the psychometric properties of the dissociative experiences scale (DES-II): a Rasch validation study. BMC Psychiatry. 2020;20(1):8. https://doi.org/10.1186/s12888-019-2417-8
Crossref PubMed PMC
22. Espírito Santo H, Abreu JL. Portuguese validation of the Dissociative Experiences Scale (DES). J Trauma Dissociation. 2009;10(1):69–82. https://doi.org/10.1080/15299730802485177
Crossref PubMed
23. Boyd JE, Lanius RA, McKinnon MC. Mindfulness-based treatments for posttraumatic stress disorder: a review of the treatment literature and neurobiological evidence. J Psychiatry Neurosci. 2018;43(1):7–25. https://doi.org/10.1503/jpn.170021
Crossref PMC
Corresponding author: Alison Fraser, RMT, West Coast College of Massage Therapy, Victoria, British Columbia, Canada, E-mail: alison@alisonfraser.ca
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
International Journal of Therapeutic Massage and Bodywork, Volume 18, Number 3, September 2025