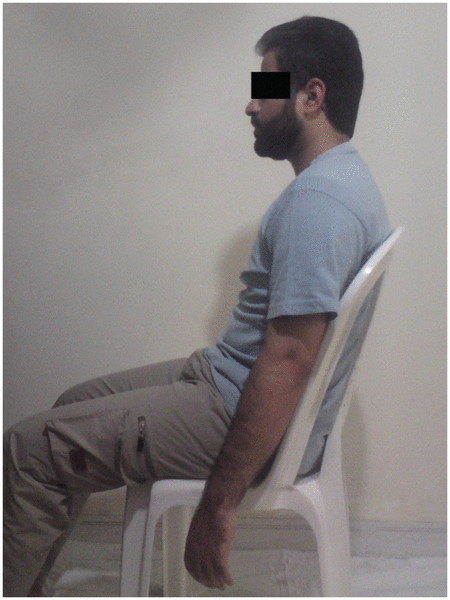
Figure 1 The patients were asked to lean on the chair back-rest in a relaxed position with their hands hanging from their sides.
Younes Jahangiri Noudeh , MD 1,*, Nasibeh Vatankhah , MD 1, Hamid R. Baradaran , MD, PhD 2
1 Faculty of Medicine, Tehran University of Medical Sciences, Tehran
2 Department of Epidemiology, Faculty of Medicine, Tehran University of Medical Sciences, Tehran, Iran
Background
Migraine headache significantly impacts the health of individuals and of society. The application of simple physical nonpharmacological techniques could greatly reduce the therapeutic costs and side effects in acute onset of such headaches.
Methods
Ten male patients (mean age was 32.0 ± 10.59 years) with acute onset of a migraine headache according to IHS-2004 diagnostic criteria were enrolled in the study. Neck and upper thoracic spine massage and manipulation technique was performed. Headache pain intensity was assessed before and after the intervention by means of a verbal analog scale.
Results
Following treatment, headache pain intensity was significantly reduced compared to the pretreatment values (1.85 ± 1.11 vs. 5.80 ± 2.25, p = .005). As a percentage, this represents a mean pain reduction of 68.77% ± 18.56. No side effects were observed, and all of the patients reported satisfaction with the intervention.
Conclusion
Our results show that the applied cervical and upper thoracic massage and manipulation technique could reduce the headache attack pain intensity in patients with migraine headaches, though further testing, including study designs that make use of control groups, is needed.
KEYWORDS: migraine , neck massage , cervical spine manipulation , abortive treatment
Migraine is one of the most common disorders in general and in neurological practice. The one-year prevalence is approximately 10% and varies little worldwide(1). Societal costs associated with migraine are high, with recent estimates of €27 billion in Europe(2) and $13 billion to $17 billion in the United States annually(3). Acute migraine attacks can be treated with simple or combination analgesics or triptans(4). However, not all attacks respond to acute treatment. Some patients with migraine have contraindications to triptans such as vascular diseases(5) or pregnancy(6), and triptans are not effective or approved during the aura phase of a migraine attack(7). On the other hand, of the total annual cost associated with migraine and its treatment, roughly one tenth ($1.5 billion) goes to medication, with triptans accounting for the majority of this amount ($1.18 billion)(3).
International Headache Society (IHS) has recently defined the term medication overuse headache (MOH) to describe daily or near daily (chronic) headache that occurs after the regular intake (overuse) of any kind of antiheadache or antimigraine drug. This is a growing problem worldwide(8). A retrospective study analyzed MOH in an US headache center over a period of 15 years(9). Interestingly, the proportion of patients with a MOH remained fairly stable over time (1990: 64% of all cases; 2005: 59.3% of all cases). However, the profile of the overused medications changed drastically. In 1990, triptans were not used in migraine therapy at all. Fifteen years later, the relative frequency of probable triptan overuse headache had increased from 0% to 21.6%. Additionally, the relative frequency increased for simple analgesics (from 8.8% to 31.8%) and combinations of acute medications (from 9.8% to 22.7%). In contrast, a significant decrease in the relative frequency could be observed for ergotamine overuse headache (from 18.6% to 0%). This retrospective study supported that MOH remains an important medical problem, although the medication profile changed over the years. The treatment of choice for MOH is abrupt drug withdrawal, and most patients improve after discontinuing regular drug intake(8). Consequently, nonpharmacological treatments with lower costs and safer effects are needed to manage migraine headaches.
The efficacy of massage and manual therapy in prevention of migraine headaches has already been demonstrated in some studies(10,11). However, there is no evidence supporting or refuting the use of spinal manipulative treatment (SMT) as an abortive treatment for headaches(12). Piovesan et al.(13) reported a case of migraine-attack pain reduction in response to massage over the greater occipital nerve territory. Another study demonstrated that the inclusion of manual techniques like osteopathic manipulative treatment (OMT) in a treatment regimen for patients with migraine headache may lower the cost of the treatment regimen(14).
It has been suggested that SMT may activate the diffuse descending pain inhibitory system, whose neurons are located in the periaqueductal grey matter(15). On the other hand, modest but significant elevations in plasma beta-endorphin levels have been found 5 minutes after cervical SMT. The disruption of pain–spasm–pain cycle is another proposed mechanism through which SMT could improve headache acute pain(16).
Vascular, neuronal, and neurovascular hypotheses have been put forth as the basic mechanism for migraines. The first two hypotheses propose a pure vascular or neuronal basis of migraine headaches(17). However, in 20th century, Moskowitz(18) unified these hypotheses into one neurovascular hypothesis that involves the role of trigeminovascular system of the brain in the basic mechanism of migraine headaches. This hypothesis could also explain the migraines aura phase and its symptoms. Whatever the basic etiology of migraine headaches, the crucial role of the periaqueductal grey matter in the inhibition of nociceptive sensations of head and face has been established(19). Therefore, it seems that spinal manipulative therapy could inhibit painful sensation during a migraine headache attack through multiple mechanisms.
The objective of our study is to evaluate the efficacy of a simple neck massage plus manipulation technique in the reduction of pain intensity in acute migraine attacks.
The study population consisted of a census of all 18–65 years of old subjects referred to our clinic with the complaint of a migraine headache attack. We excluded persons with a high probability of secondary cause for the headache at the initial evaluation, persons with any chronic systemic involvement, persons unwilling or unable to undergo the cervical and thoracic spinal manipulations because of any skeletal disorder, and persons who would have had difficulty giving reliable data because of a mental disorder. Finally, we included 10 male subjects with an episode of migraine headache in our study. Their mean age was 32.0 ± 10.59 years. Seven subjects were referred for migraine without aura attack, while the other three were referred for an episode of migraine with aura.
One headache specialist accomplished the diagnosis of present headache onset for each subject using International Criteria for Diagnosis of Headaches (ICHD-IIR1)(20). The diagnostic criteria for migraines according to ICHD-IIR1 are as follows:
Migraine Without Aura (MWO):
At least five attacks fulfilling criteria B–D.
Headache attacks lasting 4–72 hours (untreated or unsuccessfully treated)
Headache has at least two of the following characteristics:
Unilateral location
Pulsating quality
Moderate or severe pain intensity
Aggravation by or causing avoidance of routine physical activity (eg, walking or climbing stairs)
During headache at least one of the following:
Nausea and/or vomiting
Photophobia and phonophobia
Not attributed to another disorder
Migraine With Aura (MWA):
At least 2 attacks fulfilling criterion B
Migraine aura fulfilling criteria B and C for one of the subforms 1.2.1–1.2.6
Not attributed to another disorder
Comment: the aura is the complex of neurological symptoms that occurs just before or at the onset of migraine headache.
The pain intensity of the current headache episode for each subject was assessed at the time of referral just prior to the therapeutic intervention. We used a verbal analog scale to score current headache pain intensity based on a 0 to 10 point scale, where 0 is “no headache pain” and 10 is “the worst possible and excruciating headache that could be imagined”. All subjects assessed in a uniform manner.
Subjects sat and leaned on the backrest of a chair in a relaxed position with their hands hanged from the sides (Figure 1). The chair’s backrest extended to the upper thorax. The therapist was then standing posterior to the chair with his hands over the patient’s shoulder. It took a maximum of 5 minutes to complete the massage and manipulation session. A single general physician who had been trained and approved by the Iranian Association of Yumeiho Therapy performed all interventions.
|
|
||
|
Figure 1 The patients were asked to lean on the chair back-rest in a relaxed position with their hands hanging from their sides. |
||
The massage and manipulation sessions consisted of two main steps: the massage and softening step, and the manipulation step. Six successive actions were done through these two main steps. These actions included the massage of the trapezius and the supraspinatus muscles, the massage of the posterior and the lateral neck muscles, the manipulation of the cervical spine, and the manipulation of the upper thoracic spine, respectively.
This step involved a simple massage of the trapezius and supraspinatus fibers and the massage and relaxation of the posterior and lateral neck muscles. The therapist used his thumbs to rub gently on and soften the trapezius and supraspinatus fibers. He performed this in a down–upward direction between T3 and C7 vertebrae levels three to five times. In this position, the four fingers of each hand were spread over the patient’s shoulder with no pressure (Figure 2).
|
|
||
|
Figure 2 The therapist massaged the trapezius and the supraspinatus fibers in a down–upward and lateral direction between T3 and C7 vertebrae levels three to five times. |
||
For massage and relaxation of the posterior and lateral neck muscles, the therapist stood to the patient’s side, put his appropriate hand over the subject’s forehead and asked him to rest his head against the therapist’s hand (Figure 3A). This position released the neck muscles from active contraction and reduced their functional tonus. Then, the therapist drew a dash-line with the thumb of his other hand to apply pressure from the neck base to C7 level on 4 to 5 points just adjacent to the vertebral spinous processes (Figure 3B). This action was done three to five times, as well. The therapist continued the cervical relaxation phase with a similar but horizontal stepping on the same side from lateral neck to the spinous processes on 4 to 5 respective points downward (Figure 3C). The therapist moved to the other side and took the reverse position to perform the same massages for the other side muscle groups. The therapist’s hand was used to massage the contralateral side of the patients’ neck. For example, the therapist worked on the right side of a patient’s neck with his left hand.
|
|
||
|
Figure 3 Massage and relaxation of the neck muscles: (A) the method of holding the patient’s head by the therapist, (B) longitudinal, and (C) horizontal. The position of holding the patient’s head by the therapist is of extreme importance (please refer to the text). |
||
Manipulation step consisted of the adjustment of the cervical and upper thoracic intervertebral joints. This method of adjustment is very similar to chiropractic technique but with some differences in patients’ and therapist positions relative to each other. To manipulate the cervical spine, we asked the patient to hang the arms freely from the sides leaning relaxed on the chair. Then the therapist took the head in his hands from the back, rotating one hand (eg, left one) upward to put his thumb on the lateral side of the C7 vertebra. The other four fingers were spread upward to the patient’s face. The other hand palm covered the patient’s temporomaxillary process at the pre-auricular region. The therapist came down to a semisitting position and attached his chest to the chair back. Then the therapist asked the patient to leave his head relaxed. With this positioning, the patient’s head had an extreme support and the therapist could rotate the patient’s head dorsolaterally with some compression with his hand on his temporoparietal region. With rotating the head to its maximal active movement limit and then exerting some quick gentle force to pass from this limit, ‘popping’ sounds of variable loudness were able to be detected from the patient’s neck corresponding to the adjustment of the cervical intervertebral joints (Figure 4). The reverse hand positions were applied to manipulate the contralateral intervertebral joints, as well.
|
|
||
|
Figure 4 Manipulation of the cervical spine; note the head rotation manoeuvre. Putting the head in its maximum movement limit makes a resistance point such that going beyond this limit produces a popping sound from the spinal joints. |
||
This is a completely painless process. But it should be noted that a loud popping sound of the cervical joints may frighten the patient or be supposed that there may be an injury to the neck. For this reason, before the beginning of the session, the therapist explained to the patients the quality of sounds that may be heard from the neck, and indicated that the sounds are not a sign of neck injury. We performed also a range-of-motion examination of head and neck (flexion, extension, and rotation movements) before and after the manipulation, and assessed for any kind of pain or disturbances after manipulation.
The last step of our intervention is more facilitated and simple. This step included the manipulation of the upper thoracic spinal joints. In this part of the intervention, we asked the patient to maintain the sitting position and to put both hands on the occipitoparietal part of the head with the fingers interlaced. In this position, a triangle is made up of the patient’s head and neck, his forearm and arm in each side. The therapist brought his hands from behind to the patient’s front side as if attempting to embrace the subject from behind, but with the subject still seated. Then the therapist crossed his hands through the above-mentioned triangular space in each side and placed them over the patients’ hands. The therapist asked the subject to remain relaxed, then pulled the chest in a backward and upward (posterosuperior) direction imposing a concomitant pressure on back of the head in an opposite direction. This caused the patient’s upper thoracic vertebrae from T1 to almost T4 to release in the pedicular joints with a concomitant ‘popping’ sound (Figure 5). Finally, the patient was asked to lower the hands, and the therapist gave a gentle massage to the neck, shoulder, and upper arms bilaterally for about 10 to 15 seconds. Although it is not necessary to hear a popping sound during any of the manipulations, this was observed to a greater or lesser degree for all of our subjects.
|
|
||
|
Figure 5 Manipulation of the upper thoracic spine: the therapist has to pass his hands from the triangular space forward (A) and put them on the patient’s interlaced hands (B). |
||
Just after the completion of the session, we assessed the subjects’ pain by means of the verbal analog scale. Subjects were also asked about any side effects such as neck pain or the aggravation of their headache pain after the therapeutic session. We also calculated percent pain score reduction (PPSR ) for each subject using the following formula: (Pre score –post score)/Pre score. We also asked the subjects to scale their level of satisfaction about our physical intervention (massage and manipulation) according to a 7-point scale with these ratings: “terrible”, “very bad”, “bad”, “indifferent”, “good”, “very good” and “excellent”.
We requested the subjects to remain in our clinic for one hour after manipulation so that we could observe them and make sure that a remission would not occur in this period; we could also provide standard analgesic therapeutic interventions, if necessary. Finally, after completion of this period, we discharged them. We could not follow two subjects because of sleep deficiency that caused their migraine episode arousal, such that they did not agree to stay in clinic after improvement of their pain, and instead preferred to go home and sleep.
We performed a brief explanation of the therapeutic procedure to each patient and took an informed consent from the patients before including them in the procedure. After the completion of the therapeutic session, the patients were given appropriate analgesic therapeutic care according to the IHS guidelines based upon their demand and their residual painful status. Our study was approved by the Ethical Review Board of Iran University of Medical Sciences (ERBIUMS).
We used the nonparametric Mann-Whitney U test to compare patients’ mean pain scores before and after the intervention. We compared achieved scores between different migraine types, patient groups referring with or without nausea, and unilateral or bilateral headache episode. Wilcoxon signed rank test was also used to compare mean pain scores in independent groups. To compare mean pain scores in three successive measurements, we performed repeated measures Analysis of Variances (ANOVA) with Greenhouse-Geisser correction for degrees of freedom. Such an adjustment has been done because of small sample size of our study ( p = .022, Mauchly’s test of sphericity for the ANOVA test). We used Statistical Package for Social Studies (SPSS) version 17.0 (Aug 23, 2008) (SPSS Inc., Chicago, IL) to analyze our data. Tolerance for Type one error was 0.05 for all analyses.
Headaches were unilateral in five subjects, and the remaining five persons complained of a bilateral headache episode. Nausea was present in three patients. No other accompanying symptoms were reported by any subject. The mean primary pain score at subjects’ referral was 5.80 ± 2.25 that dropped to a mean of 1.85 ± 1.11 ( p = .005, Z =−2.805, Wilcoxon signed rank test) just after our therapeutic intervention, and to 0.56 ± 0.56 one hour after the intervention ( p < .0001, F = 44.956, ANOVA) (Figure 6). The average percent pain score reduction immediately following treatment was 68.10 ± 18.56%, and the mean pain score change was 3.95 ± 1.67 just after intervention. Eight patients out of 10 had at least 50% reduction in their headache pain scores just after intervention as described by the patients themselves.
|
|
||
|
Figure 6 The reduction in the headache pain score was statistically significant after treatment (p=.005 for comparison of before and just after manipulation average pain scores; and p<.0001 for comparison of three successive measurements of average pain scores). |
||
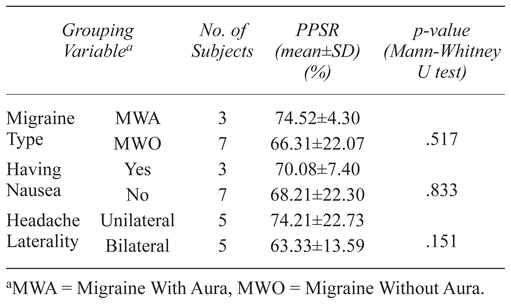
Percent pain score reduction (PPSR) was not correlated with the subjects’ age (correlation coefficient = 0.113, p = .756). The mean PPSR was 66.31 ± 22.07% for migraine without aura (MWO) vs. 74.52 ± 4.30% for migraine with aura (MWA) groups. This difference was not statistically significant ( p = .517, Mann-Whitney U test). The mean PPSR after the therapy was 70.08 ± 7.40% in patients referred with nausea vs. 68.21 ± 22.30% without nausea ( p = .833, Mann-Whitney U test). The mean PPSR after intervention was 74.21 ± 22.73% in subjects referred with a unilateral headache pain vs. 63.33 ± 13.59% with a bilateral episode ( p = .151, Mann-Whitney U test). Table 1 demonstrates a summary of these comparisons.
Table 1
Percent Pain Score Reduction After Manipulation
After one hour of follow-up, there was no recurrence of headache pain for any subject. Three patients requested an oral analgesic drug (one tablet of Iboprofen 400 mg), and one patient with an episode of migraine without aura and pain score of 10 underwent IV fluid therapy with 500 cc of dextrose 5% and a cocktail of dexamethasone 8 mg and methoclopramide 10 mg infused, in addition to 50 mg of promethazine injected intramuscularly in the gluteal region.
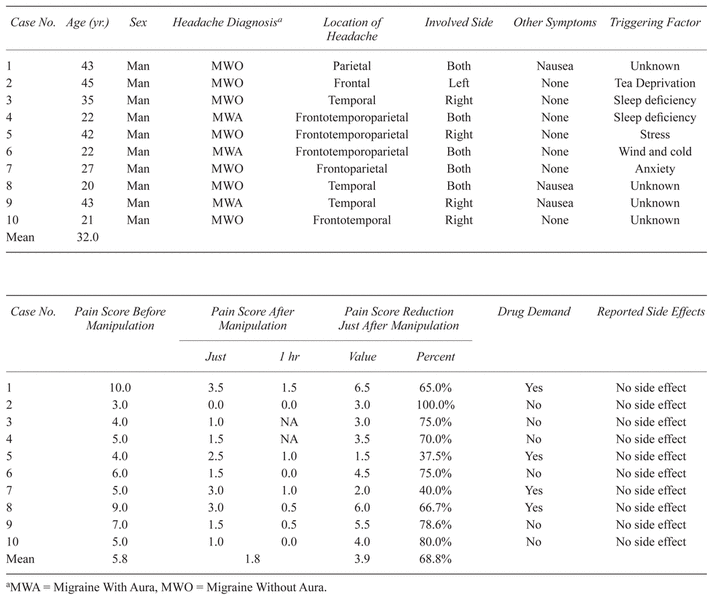
There was no reduction in flexion, extension, or rotation of the neck. Also, none of the patients complained from any side effects including neck pain or aggravation of the headache pain, and all of them mentioned experiencing a relaxed, comfortable state after the therapeutic session. Four subjects rated the massage and manipulation intervention as “good”, and three rated it as “very good”. The remaining three persons rated it as “excellent”. These data and other subject details are summarized in Table 2.
Table 2
Summary of Characteristics of Study Subjects
The application of massage therapy has already been studied with some promising results as the prophylactic treatment for migraine headaches(10). Several clinical trials indicate that spinal manipulation therapy may help in the treatment of migraine headaches. In one study of people with migraines, 22% of those who received chiropractic manipulation reported more than 90% reduction of attacks and 49% reported a significant reduction of the intensity of their migraine headaches(21). Harris(22) reported a case of severe migraine with aura that had begun after the patient was involved in an automobile accident 17 years prior. After 12 weeks of chiropractic treatment, the duration, frequency, and intensity of migraines decreased. In another study, cervical spine manipulation showed similar efficacy as amitriptyline in reducing the migraine intensity in the long term. However, the evidence is weak in this area(23,24).
The use of spinal manipulation as a treatment for headaches is predicated upon the cervical spine being a contributing factor in the etiology of headaches. The theoretical mechanism is based on the convergence of two peripheral systems of nociception: the trigeminal system and the cervical spinal nerves, particularly C1 to C3(12). The spinal trigeminal nucleus, especially Spinal trigeminal nucleus (Sp5C), is an essential component in the transmission and processing of pain and thermal sensations from the head and face(25). So far, sensory nerves innervating cerebral vessels clearly terminate in a region extending from the caudal portion of the spinal trigeminal nucleus (Sp5C) in the medulla to the lower end of the C2 spinal dorsal horn, a region referred to as the trigeminocervical complex(26). Bovim et al.(27) demonstrated in an experimental study that structures in addition to the zygapophyseal joints, which are innervated by the first three cervical nerves, might contribute to or cause headaches. Another possible connection between the cervical spine and headache is an anatomic connection between cervical spine musculature and the spinal dura. A dense connective tissue bridge connects the rectus capitus posterior minor (RCPM) with the spinal dura at the level of the atlanto-occipital junction. The connective tissue fibers are oriented perpendicular to the dura, which is a pain sensitive structure known to be a source of headache pain. It is hypothesized that mechanical dysfunction of the atlanto-occipital junction and/or hypertonicity of the RCPM may exert a traction force on the dura through the connective tissue bridge and thereby produce headache pain(12). These pathophysiologic approaches may be the common ground of migraine with the cervicogenic headache. This is because nerve-vessel compression on the C2 root, where the ventral ramus crosses the upper cervical segment of the vertebral artery, and ipsilateral C2-C3 nerve or nerve root involvement and possible secondary central somatosensory dysfunction both were hypothesized as causes for cervicogenic headache(28).
Since abortive therapy of headaches accounts for a main part of the therapeutic costs in migraine treatment(3), the application of drug-free physical treatment modalities could potentially reduce the costs of treating migraine headaches. Our results may also emphasize that stratified care should include nonpharmacologic and other nonspecific treatment modalities for milder headaches with a stronger pharmacotherapy program being used when appropriate(29). In addition, the continued pain reduction and absence of headache recurrence in the hour following treatment could be explained by an increase in the plasma beta-endorphin concentrations, which has been proposed in previous studies(16).
It is worth mentioning the long-standing concern regarding the potential for serious complications including vascular injury and overall safety of cervical spine manipulation. None of the patients in our study reported any side effects like cervical pain or headache aggravation following the cervical manipulation. Further, the state of relaxation and the expression of no pain or disturbance while performing the manipulations made it so acceptable for the patients. While this may be true in the majority of studies, cervical spinal manipulation may have a very small potential risk of serious adverse events following treatment, which must be considered in the formation of clinical guidelines(30,31). It has been reported that chiropractic manipulation increases the risk of vertebral artery dissection and stroke or transient ischemic attack approximately six-fold(32). Wada et al.(33) reported a case of internal jugular vein thrombosis following to the shiatsu massage of the neck in a 35-year-old man. In the present study, all manipulations were performed by a trained physician (Y. J.). Although the applied techniques were from Yumeiho therapy—a newly arisen Japanese manipulative therapy—they were not substantially different from chiropractic manipulations.
We do not know whether the neck massage, manipulation, or the combination of these modalities improved the painful status of the subjects. Determination of this issue needs future comparative studies. The absence of a control group and a low number of subjects severely limits the value of our findings. However, in the absence of similar reports of the application of this technique, it can be a good basis as a preliminary novel idea for future large scale studies.
We demonstrated in this preliminary study that cervical spinal massage and manipulation could significantly reduce the headache pain intensity in acute migraine attacks. However, future controlled studies with larger sample sizes are necessary to confirm the findings of the present study.
1
Stovner L, Hagen K, Jensen R, et al. The global burden of headache: a documentation of headache prevalence and disability worldwide.
Cephalalgia
. 2007;27(3):193–210.

2
Andlin-Sobocki P, Jonsson B, Wittchen HU, et al. Cost of disorders of the brain in Europe.
Eur J Neurol
. 2005;12(Suppl 1):1–27.

3
Goldberg LD. The cost of migraine and its treatment.
Am J Manag Care
. 2005;11(2 Suppl):S62–S67.
4
Evers S, Afra J, Frese A, et al. EFNS guideline on the drug treatment of migraine –revised report of an EFNS task force.
Eur J Neurol
. 2009;16(9):968–981.

5
Dodick DW, Martin VT, Smith T, et al. Cardiovascular tolerability and safety of triptans: a review of clinical data.
Headache
. 2004;44(Suppl 1):S20–S30.

6
Cunnington M, Ephross S, Churchill P. The safety of sumatriptan and naratriptan in pregnancy: what have we learned?
Headache
. 2009;49(10):1414–1422.

7
Olesen J, Diener HC, Schoenen J, et al. No effect of eletriptan administration during the aura phase of migraine.
Eur J Neurol
. 2004;11(10):671–677.

8
Katsarava Z, Holle D, Diener HC. Medication overuse headache.
Curr Neurol Neurosci Rep
. 2009;9(2):115–119.

9
Meskunas CA, Tepper SJ, Rapoport AM, et al. Medications associated with probable medication overuse headache reported in a tertiary care headache center over a 15-year period.
Headache
. 2006;46(5):766–772.

10
Lawler SP, Cameron LD. A randomized, controlled trial of massage therapy as a treatment for migraine.
Ann Behav Med
. 2006;32(1):50–59.

11
Lipton SA. Prevention of classic migraine headache by digital massage of the superficial temporal arteries during visual aura.
Ann Neurol
. 1986;19(5):515–516.

12 Gay RE, Nelson CF. Clinical efficacy of chiropractic treatment. In: Wainapel SF, Fast A, ed. Alternative Medicine and Rehabilitation: A Guide for Practitioners . New York: Demos Medical Publishing; 2003. p.67–71.
13
Piovesan EJ, Di Stani F, Kowacs PA, et al. Massaging over the greater occipital nerve reduces the intensity of migraine attacks: evidence for inhibitory trigemino-cervical convergence mechanisms.
Arq Neuropsiquiatr
. 2007;65(3A):599–604.

14
Schabert E, Crow WT. Impact of osteopathic manipulative treatment on cost of care for patients with migraine headache: a retrospective review of patient records.
J Am Osteopath Assoc
. 2009;109(8):403–407.
15
Vicenzino B, Collins D, Benson H, et al. An investigation of the interrelationship between manipulative therapy-induced hypoalgesia and sympathoexcitation.
J Manipulative Physiol Ther
. 1998;21(7):448–453.
16
Maigne JY, Vautravers P. Mechanism of action of spinal manipulative therapy.
Joint Bone Spine
. 2003;70(5):336–341.

17
Dodick DW. Examining the essence of migraine–is it the blood vessel or the brain? A debate.
Headache
. 2008;48(4):661–667.

18
Moskowitz MA. The visceral organ brain: implications for the pathophysiology of vascular head pain.
Neurology
. 1991;41(2(Pt 1)):182–186.
19
Knight YE, Goadsby PJ. The periaqueductal grey matter modulates trigeminovascular input: a role in migraine?
Neuroscience
. 2001;106(4):793–800.

20 International Headache Society. The International Classification of Headache Disorders, 2nd Edition. 1st Revision. Headache Classification Subcommittee of the International Headache Society. Oxford, UK: Blackwell Publishing; 2005.
21
Tuchin PJ, Pollard H, Bonello R. A randomized controlled trial of chiropractic spinal manipulative therapy for migraine.
J Manipulative Physiol Ther
. 2000;23(2):91–95.

22
Harris SP. Chiropractic management of a patient with migraine headache.
J Chiropr Med
. 2005;4(1):25–31.

23
Biondi DM. Physical treatments for headache: a structured review.
Headache
. 2005;45(6):738–746.

24
Bronfort G, Assendelft WJ, Evans R, et al. Efficacy of spinal manipulation for chronic headache: a systematic review.
J Manipulative Physiol Ther
. 2001;24(7):457–466.
25
Dubner R, Bennett GJ. Spinal and trigeminal mechanisms of nociception.
Annu Rev Neurosci
. 1983;6:381–418.

26
Goadsby PJ, Classey JD. Glutamatergic transmission in the trigeminal nucleus assessed with local blood flow.
Brain Res
. 2000;875(1–2):119–124.

27
Bovim G, Sand T. Cervicogenic headache, migraine without aura and tension-type headache. Diagnostic blockade of greater occipital and supra-orbital nerves.
Pain
. 1992;51(1):43–48.

28 Inan N, Ates Y. Cervicogenic headache: pathophysiology, diagnostic criteria and treatment. Agri . 2005;17(4):23–30.
29
Weintraub JR. Treatment of acute migraine attacks.
J Am Osteopath Assoc
. 2000;100(9 Suppl):S1–S7.
30
Carnes D, Mars TS, Mullinger B, et al. Adverse events and manual therapy: a systematic review.
Man Ther
. 2010;15(4):355–363.

31
Ernst E. Adverse effects of spinal manipulation: a systematic review.
J R Soc Med
. 2007;100(7):330–338.


32
Smith WS, Johnston SC, Skalabrin EJ, et al. Spinal manipulative therapy is an independent risk factor for vertebral artery dissection.
Neurology
. 2003;60(9):1424–1428.
33
Wada Y, Yanagihara C, Nishimura Y. Internal jugular vein thrombosis associated with shiatsu massage of the neck [letter].
J Neurol Neurosurg Psychiatry
. 2005;76(1):142–143.
Published under the CreativeCommons Attribution NonCommercial-NoDerivs 3.0 License.
CONFLICT OF INTEREST NOTIFICATION
The authors declare that there are no conflicts of interest. ( Return to Text )
INTERNATIONAL JOURNAL OF THERAPEUTIC MASSAGE AND BODYWORK , VOLUME 5 , NUMBER 1 , MARCH 2012