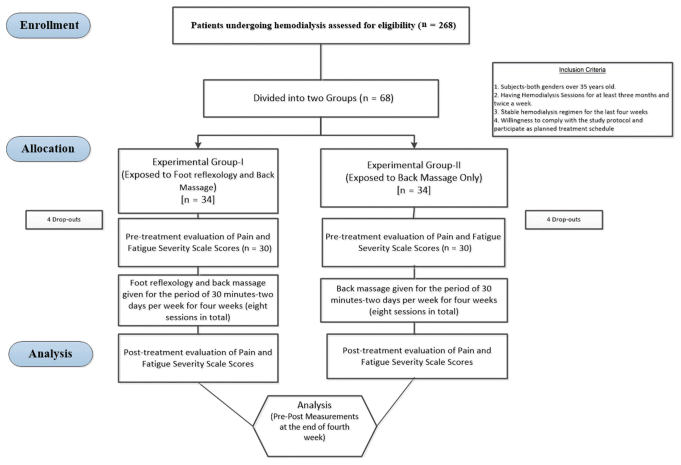
Figure 1 Randomization flow chart showing subjects’ involvement in the study.
Sivakumar Chinnusamy, PhD (PT),1 Arun Vijay Subbarayalu, PhD (PT),2* Pradeepa Mani, PhD (PT),1 Vinosh Kumar Purushothaman, MPT,3 Rajkumar Krishnan Vasanthi, MPT,3 Chittode Krishnasamy Muralidharan, PhD (PT),4 Prabhakaradoss Devadoss, PhD (PT),5 Balachandran Ganapathy Surulisubbiah, MPT6
1PPG College of Physiotherapy, Affiliated to the Tamil Nadu Dr. MGR Medical University, Coimbatore, Tamil Nadu, India,
2Department of Physical Therapy, Deanship of Quality and Academic Accreditation, Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia,
3Faculty of Health & Life Sciences, INTI International University, Nilai, Negeri Sembilan, Malaysia,
4Nandha College of Physiotherapy, Affiliated to the Tamil Nadu Dr. MGR Medical University, Erode, Tamil Nadu, India,
5Vinayaka Mission’s College of Physiotherapy, Vinayaka Mission Research Foundation (DU), Salem, Tamil Nadu, India,
6Physiotherapy Department, Ganga Medical Centre and Hospitals Private Limited, Coimbatore, Tamil Nadu, India
Background
Multiple treatment modalities have been used to treat complications such as pain and fatigue in patients undergoing hemodialysis. However, the combined effectiveness of reflexology and back massage (BM) in relieving pain and fatigue in patients undergoing hemodialysis is limited and this study aims to fill this research gap.
Materials and methods
A pre- and post-test experimental study design was adopted in which 60 patients (n = 60) undergoing dialysis were randomized into two groups of 30 each using a simple randomization technique. The subjects of experimental group I received foot reflexology (FR) and BM, while experimental group II received only BM. The intervention lasted 2 days per week for 4 weeks. To examine the effectiveness of the treatment both before the intervention and at the end of the fourth week, two variables were evaluated: (i) pain intensity, which was measured using the visual analogue scale (VAS) and (ii) fatigue experienced by patients, which was measured using the Fatigue Severity Scale (FSS).
Results
Subjects treated with FR and BM showed better reduction in VAS (mean difference: 1.06, 95% confidence interval (CI): 0.299–1.834, p < 0.05) and FSS (mean difference: 6.61, 95% CI: 0.230–11.90, p < 0.05) than the subjects exposed to BM only, with a significance level of 0.05.
Conclusion
The combination of FR and BM has been found to be significantly more effective than BM alone in managing the health risks of pain and fatigue in hemodialysis patients.
KEYWORDS: Foot reflexology; back massage; hemodialysis; pain; fatigue
End-stage renal disease (ESRD) is the point where the kidneys are unable to carry out their vital tasks. It substantially affects those patients’ general health and quality of life and requires lifelong care, such as hemodialysis.(1) Hemodialysis is a life-sustaining treatment for patients with kidney or renal failure, where blood is removed from the patient, filtered through an artificial kidney called a dialyzer, and then returned to the patient.(2) This process involves the extracorporeal removal of waste products and excess fluids that accumulate due to the kidneys’ inability to perform their excretory functions.(3) It is a lifelong therapy for patients with ESRD with a frequency of 2–3 times per week for 4–5 h per session. Prolonged dialysis can cause stress and various psychological and social problems and lead to psychological disorders. Fatigue is a common feeling experienced by 60–97% of hemodialysis patients.(4) In addition to other complications, hemodialysis patients are more likely to experience pain during catheter insertion due to painful procedures, acute complications of hemodialysis, and painful syndromes such as neuropathic and musculoskeletal syndromes.(5) Complications such as tip misplacement and puncture of the mediastinum can also contribute to catheter insertional pain.(6) In addition, pain in hemodialysis patients is linked to poor treatment compliance, sleep issues, repeated hospital stays, a lower standard of living, and high death rates.(7) Besides these, fatigue is a common symptom among hemodialysis patients and is mediated by several physiological processes. Indolamine-2,3-dioxygenase activity is one such mechanism that is linked to fatigue and alterations in muscle mass and function—a recent study found that 54% of maintenance hemodialysis patients experienced increased fatigue owing to dialysis, suggesting that hemodialysis may contribute to the incidence of fatigue in these patients.(8) Several other studies also highlighted the prevalence of fatigue in patients undergoing hemodialysis, which is associated with lower quality of life, depression, and poor sleep quality.(9) Several treatment methods have been used to manage pain caused by catheter insertion during hemodialysis treatment. These methods include cooling sprays,(10) lidocaine sprays,(5) and EMLA cream.(11) Physical therapy also plays a significant role in managing catheter insertion pain. In particular, aerobic exercises such as walking, cycling, and swimming have been shown to reduce pain and improve physical function in hemodialysis patients.(12,13) Likewise, resistance exercises, including weightlifting and resistance band exercises, can help improve muscle strength and reduce pain in hemodialysis patients.(5) Other physical therapy treatments such as tai-chi, stretching exercises, reflexology, acupressure, aromatherapy, massage, and yoga show potential benefits in reducing fatigue and improving quality of life in hemodialysis patients.(14–16)
Reflexology is a complementary medicine practice that involves applying pressure to certain points on the feet to stimulate the body’s organs and systems. It can reduce fatigue and increase daily living activities in hemodialysis patients.(17,18) Furthermore, it has been found that reflexology techniques, specifically, foot reflexology (FR), help hemodialysis patients manage their pain.(19,20) Similar findings from past research indicate that back massages (BMs) are a useful non-pharmacological treatment for pain and fatigue in hemodialysis patients.(4,21) Despite the existence of these treatment approaches, the combined effectiveness of FR and BM in relieving pain and fatigue in patients undergoing hemodialysis is limited. This research examined the efficacy of FR and BM in reducing pain and fatigue in hemodialysis patients, in an effort to add to the body of literature.
This study was a prospective, single-blinded, randomized trial. Accordingly, the investigators chose a pre-test, post-test experimental group design with two different intervention groups in which intervention group I received FR and BM and intervention group II received BM alone to determine the combined effectiveness of FR and BM on pain and fatigue in patients undergoing hemodialysis.
This study focused on patients undergoing dialysis in selected private hospitals in Coimbatore city, India. The study was conducted between October 15, 2023 and June 1, 2023, and all patients undergoing dialysis in four selected tertiary care hospitals in Coimbatore city were included in this study after obtaining formal approval from these hospitals. It was carried out in accordance with the principles of the Declaration of Helsinki and all participants signed written informed consent before the planned therapeutic intervention. Formal ethical approval was granted by the study settings for conducting this study (study setting name hidden for blinded review purposes) (clinical ethical committee approval number AH-ECA-5-2023). The required number of samples was calculated as 34 per group based on the assumption of 80% power using a two-tailed test with a significance level of 0.05 and an expected dropout rate of 10%.(22) Subsequently, 68 participants were selected using a criterion-based simple random sampling method (Figure 1). The following criteria were used to screen the subjects and include them in the sampling frame: (i) both genders over 35 years of age; (ii) hemodialysis for at least 3 months and twice a week; (iii) stable hemodialysis regimen for the last 4 weeks, with no expected changes during the study period; (iv) ability to give informed consent or have a legally authorized representative to give consent; and (v) willingness to comply with the study protocol and participate as planned treatment schedule. Excluded from the study were patients with skin lesions, open foot wounds, malignancies, thrombosis, bleeding disorders, cognitive impairments, or psychiatric disorders that could affect their ability to participate or provide reliable feedback. Based on those subjects meeting the inclusion criteria, a sampling frame was developed using a computer-generated random table and 68 participants were randomized into two groups of 34 each using a simple random sampling approach. Furthermore, to avoid selection bias, a random sample across multiple hospitals is ensured, with standardized recruitment protocols in the form of strict inclusion criteria, and the randomization process is managed by a blinded independent coordinator who ensures that participant characteristics (e.g., age, gender, type/stage of renal disease, and general health status) are balanced between groups and helps enhance generalizability and fairness in treatment comparisons, thus overcoming these confounding factors.
|
| ||
|
Figure 1 Randomization flow chart showing subjects’ involvement in the study. | ||
Prior to being exposed to the selected treatment procedures, all of the subjects were randomized into two groups of 34 each using a simple randomization technique. However, eight test subjects were unable to complete the study period and dropped out. While subjects in experimental group I (EG-I) received both FR and BM, those in experimental group II (EG-II) only received BM. According to the study protocol, the interventions were delivered by two licensed physical therapists who are part of a research team with 10–15 years of clinical experience in manual and manipulative therapy techniques and who have acquired formal training in massage therapy in addition to their formal postgraduate master’s degree in physical therapy. All subjects were subjected to pre-measurement of outcome parameters before proceeding to dialysis, i.e., pain and fatigue level. All subjects received common instructions to follow throughout the study period. Before patients were taken to hemodialysis, FR and BM were performed. First, the subjects received a 30-min BM while lying on their side, which gave them the most comfort. Following this, FR was given, which lasted 30 min, with 15 min for each foot. The FR and BM interventions lasted 2 days per week for 4 weeks (eight sessions in total). Two variables were used to assess the effectiveness of the treatment technique: (i) pain intensity, which was measured using the visual analogue scale (VAS) and (ii) fatigue experienced by patients, which was measured using the Fatigue Severity Scale (FSS). The FSS measures changes in fatigue severity and includes items related to motivation, physical activity, work, family, and social life. FSS has nine items, and each item is rated on a 7-point scale, where 1 means the patient strongly disagrees with the statement and 7 means the patient strongly agrees with the statement. Therefore, 9 is the minimum score and 63 is the maximum score. If the patient’s total score is 36 or higher, they are considered fatigued and may require further evaluation by a physician.(23) FSS is internally consistent, has good test–retest reliability, and correlates well with visual analogue measurements.(24) It has been used in multiple studies to assess fatigue severity in hemodialysis patients.(25) Measurements were taken on the first day (day 1), before patients were exposed to pre-intervention, and at the end of each treatment session. However, to determine the effectiveness of the treatment, this study uses a post-intervention measurement with similar VAS and FSS tools, conducted at the end of the fourth week of intervention, immediately after the last treatment session. Blinding of both the treating physiotherapist and the participating subjects was practically not possible and therefore the treating physiotherapist was not blinded due to the regulations of the study setting. However, blinding occurred at the level of measurement of the outcome variables and data collection because the physiotherapists involved in the randomization were neither involved in the implementation of the therapeutic intervention nor in the data collection process. Two independent physical therapists, not involved in the randomization or application of the interventions, were involved in recording the outcome measures using a standard VAS and FSS tool to ensure consistent recording of the data. To facilitate this, an orientation session was offered to both physical therapists by the principal investigator prior to the start of this study. To overcome/minimize the impact of inherent biases in study design, researchers also took several steps, including strict adherence to proper random assignment to treatment groups, maintaining single blinding so that participants do not know which treatment they are receiving, and uniform intervention procedures were used across all hospitals involved in this study to prevent differences in treatment protocol execution, and standard forms were used to document treatment details and follow-up. As such, two well-trained physical therapists delivered interventions consistently and avoided unintentional bias in treatment application.
The authors adopted the FR protocol from previous studies.(26) Therefore, the first steps in FR are relaxation exercises involving rubbing, patting, and squeezing motions with the thumb, finger, and hand lasting for 30 min, with 15 min for each foot. The therapist applies FR in a top-down fashion. First, the big toe points corresponding to the pituitary gland, hypothalamus, brain, and pineal body are softly massaged. Following this, the area from the big toe to the middle of the back side of the heel is massaged along the medulla spinalis body point. Finally, reflexology is applied to all areas of the foot corresponding to the nerve projections after applying pressure to the solar plexus. The FR session ends with the application of the same relaxation techniques discussed previously.
The subjects were given a 30-min BM by the investigators while they were lying on the side that provided them with the most comfort. The massage was applied before each patient’s hemodialysis session for a period of 4 weeks.(27) Three to five drops of baby oil were used to lessen friction during the massage. The massage techniques, which include friction, petrissage, and effleurage, were applied in a standard room temperature setting. Specific movements, such as rotations beneath the upper cervical region, are used in the slow stroke BM. Slow strokes are applied along the spinal column during the entire session. Light taps are applied to various areas of the patient’s back to produce a therapeutic effect. This massage technique uses slow, rhythmic, and soft strokes to enhance the patient’s sensory awareness and promote relaxation.
Data were analyzed using SPSS (Statistical Package for Social Sciences) for Windows, version 23.0 (IBM Corp., Armonk, NY, USA). For each outcome parameter, a paired t-test was used to determine whether there was a significant difference between the pre- and post-treatment scores. The effectiveness of treatment between the two intervention groups was also evaluated using an unpaired t-test on two outcome measures. The extent of change in the mean of an outcome measure from one time point to another was also determined by calculating the effect size (r) (Cohen’s d).(28,29) Furthermore, the standard deviation approach, a distribution-based method, was used for calculating the minimal clinically important difference (MCID) in pain (VAS), and the FSS after the application of FR and BM in patients undergoing hemodialysis.(30)
Taking into account those who dropped out of the study (n = 8), 30 subjects continued until the end of the intervention period—data from all participants (n = 30) were subjected to statistical treatment with a significance level of 0.05. It was observed that patients undergoing hemodialysis and subjected to BM showed a significant reduction in VAS (mean difference: 1.87, 95% confidence interval (CI): 1.49–2.24, p < 0.05) and FSS (mean difference: 3.03, 95% CI: 2.35–3.72, p < 0.05) between the pre- and post-intervention periods at a significance level of 0.05 with a large effect size (Table 1).
Table 1 Analysis of Pain and Fatigue Severity Scale in Hemodialysis Patients After the Application of Back Massage
Similarly, patients undergoing hemodialysis who were exposed to the treatment combinations of FR and BM showed a significant reduction in pain intensity (mean difference: 2.73, 95% CI: 2.24–3.23, p < 0.05) and FSS (mean difference: 8.74, 95% CI: 6.84–9.56, p < 0.05) between the pre-intervention and post-intervention periods at 0.05 level of significance with a large effect size (Table 2).
Table 2 Analysis of Pain and Fatigue Severity Scale in Hemodialysis Patients After the Application of Reflexology and Back Massage
Additionally, a clinically significant difference with a medium effect size was observed in the post-intervention mean scores of FSS and VAS between the two experimental groups at the end of the fourth week of therapeutic intervention. More specifically, EG-I, which received both FR and BM, showed better improvement than EG-II, which only received BM, in both FSS (mean difference: 6.61, 95% CI: 0.230–11.90, p < 0.05) and VAS scores (mean difference: 1.06, 95% CI: 0.299–1.834, p < 0.05) with a significance level of 0.05 (Table 3).
Table 3 Analysis of Pain and Fatigue Severity Scale in Hemodialysis Patients After the Application of Therapeutic Interventions in Both Experimental Groups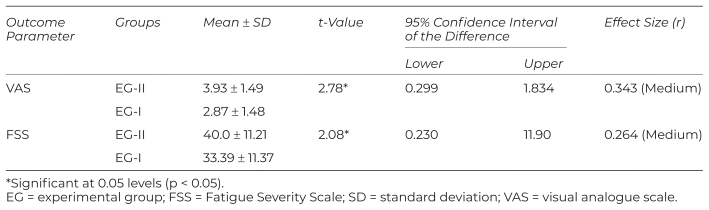
The aim of this study was to compare the effectiveness of FR and BM over a period of 4 weeks in patients undergoing hemodialysis with the expectation of reducing their pain and fatigue associated with catheter insertion.
After 4 weeks of intervention (two sessions per week), subjects undergoing hemodialysis showed statistically and clinically significant improvements in pain and FSS following the application of FR and BM (Table 1). Besides, this study found that the calculated MCID (threshold) for pain (VAS) and FSS after applying FR and BM was 0.66 and 1.82 points, respectively. In addition, it was found that 100% of subjects met the MCID threshold for pain and fatigue severity after the application of FR and BM. Likewise, the MCID values determined for pain and fatigue severity in the subjects who received BM were 0.50 and 0.92, respectively. Furthermore, all subjects in this particular group met the MCID threshold for both pain and fatigue severity. The MCID concept is essential for evaluating patient-reported outcomes in hemodialysis patients, such as the degree of pain and fatigue,(31) and it represents the smallest change in scores that patients perceive as meaningful.(32) In the context of hemodialysis, understanding MCID scores for pain and fatigue severity can be helpful in interpreting treatment effectiveness and patient satisfaction.(33)
Our results show that subjects treated with FR and BM showed a significant reduction in pain intensity according to VAS. Consistent with these results, a previous study also demonstrated that reflexology and massage can help reduce symptoms that hemodialysis patients frequently experience, such as anxiety, fatigue, restless leg syndrome, and poor quality sleep.(19) While massage encourages relaxation, enhances blood circulation, and releases endorphins—which are the body’s natural analgesics—reflexology techniques target specific reflex points and lessen the experience of pain.(4,19) Therefore, the benefits of BM and reflexology for pain management in hemodialysis patients underscore the value of complementary therapies in improving their overall health and quality of life.(34)
Similarly, this study also showed a significant reduction in pain in the group that received BM where a mean difference of 1.87 (95% CI: 1.49–2.24, p < 0.05) was observed between its pre- and post-intervention time intervals (Table 1). A previous study also showed that BM can significantly improve comfort levels by treating muscle cramps, back pain, and other ailments associated with hemodialysis.(35) Several mechanisms are behind the efficacy of massage on pain reduction. One main mechanism involves stimulating the release of endorphins, which are the body’s natural analgesics and reduce pain perception while elevating feelings of well-being.(34) Furthermore, massage therapy can enhance blood circulation, which lessens the commonly felt ischemia-induced pain during hemodialysis and relieves muscle cramps.(36) The results of this study also indicate that there is a significant reduction in fatigue severity following massage therapy. This could be due to the fact that there is improved blood circulation after massage, which helps to remove metabolic waste products that accumulate during dialysis, thereby reducing the feeling of fatigue.(37) In addition, BM stimulates the parasympathetic nervous system, promoting relaxation and reducing stress levels, which contribute significantly to fatigue in hemodialysis patients.(38)
This study also reports that the subjects treated with FR and BM showed a significant reduction in pain and fatigue severity after 4 weeks of intervention. Consistent with our findings, previous studies also confirmed that FR can significantly reduce fatigue and improve activities of daily living,( 17) and BMs have been associated with a decrease in fatigue scores in hemodialysis patients after the procedure.(4) FR is believed to stimulate specific reflex points corresponding to various organs and systems in the body, promoting relaxation and improving blood circulation, which can relieve fatigue by improving oxygen and nutrient delivery to tissues and removing metabolic waste products more efficiently.( 4,17) It also triggers the release of endorphins, which are natural painkillers and mood enhancers, reducing feelings of fatigue and improving overall well-being.(16) In addition, both reflexology and foot massage can modulate the autonomic nervous system by reducing sympathetic activity and increasing parasympathetic activity, resulting in a state of relaxation and reduced stress levels, which are crucial for managing fatigue.(16)
Because there is no control group, it is difficult to confirm observed changes, and the short-term intervention did not examine long-term effects. In addition, the subjects’ everyday activities were not observed, which could have influenced the outcome of the study. Future research should increase the sample size to generalize the results. In addition, there are some confounding factors such as age and frequency and duration of hemodialysis that might have influenced the study’s outcomes and the investigators formulated specific inclusion criteria to recruit samples within a particular age range and those patients who are on hemodialysis for at least 3 months and the frequency of hemodialysis is twice a week as well as having patients who have a stable hemodialysis regimen for the last 4 weeks, with no expected changes during the study period. Despite these strategies, it is recommended to conduct a longitudinal study in the future to overcome these factors.
The present study concluded that FR and BM were found to have short-term effects on pain and fatigue severity scores of subjects undergoing hemodialysis. Also, the study confirms that, clinically, the protocol consisting of FR and massage therapy with two sessions per week for 4 weeks is effective enough to reduce catheter insertional pain and fatigue severity experienced by the patients undergoing hemodialysis. However, future studies can be conducted with a larger sample size, and the duration of the treatment protocol could be extended for a longer period of time to determine the long-term effectiveness of the improvement achieved.
No sources of funding were used in this study.
The authors declare there are no conflicts of interest.
1. Powathil GG, Kr A. The experience of living with a chronic illness: a qualitative study among end-stage renal disease patients. J Soc Work End Life Palliat Care. 2023;19(3):190–208.
Crossref PubMed
2. Rajasekaran T, Preetha KG, Sneha D, Priyadharshini P. Smart portable kidney dialysis control and monitoring system. Int J Adv Res Innov Ideas Educ. 2020;6:219–224.
3. Williams A. Hemodialysis and peritoneal dialysis. In: Godbole PP, Koyle MA, Wilcox DT, eds. Pediatric Urology: Surgical Complications and Management. Wiley-Blackwell; 2015:305–314.
Crossref
4. Khamid A, Rakhmawati A. The influence of feet reflexology and back massage on hemodialysis patients’ fatigue. KnE Life Sci. 2022;7(2):677–686.
5. Gerogianni G. Factors affecting pain in hemodialysis and non-pharmacological management. Cureus. 2023;15(2):e35448.
PubMed PMC
6. Desai A, Bennikal M, Bangari G, Janaky M, Manjunath R. Malpositioned dialysis catheters: a case series. Ukr J Nephrol Dial. 2022;4(76):10–15.
Crossref
7. Moore I, Byrne P, Ilic N, Chen JHC, Lambert K. The prevalence and lived experience of pain in people undertaking dialysis. Kidney Dial. 2023;3(1):24–35.
Crossref
8. Zheng XY, Zhang ZH, Cheng YM, Yang Q, Xu B, Lai BC, et al. Factors associated with subgroups of fatigue in maintenance hemodialysis patients: a cross-sectional study. Ren Fail. 2023;45(1):2221129.
Crossref PubMed PMC
9. Li H, Yin J, Dong Y, Tian Z. Factors predicting post-dialysis fatigue of maintenance hemodialysis patients. Ren Replace Ther. 2023;9(1):30.
Crossref
10. Khosravi Pour A, Hejazi S, Kameli A, Hoseini Azizi T, Armat MR, Eshghi M. Cooling spray or lidocaine spray and needle insertion pain in hemodialysis patients: an open-label cross-over randomized clinical trial. BMC Anesthesiol. 2023;23(1):69.
Crossref PubMed PMC
11. Babamohamadi H, Ameri Z, Asadi I, Asgari MR. Comparison of the effect of EMLA™ cream and the Valsalva maneuver on pain severity during vascular needle insertion in hemodialysis patients: a controlled, randomized, clinical trial. Evid Based Complement Alternat Med. 2022;2022(1):8383021.
Crossref
12. Smart NA, Williams AD, Levinger I, Selig S, Howden E, Coombes JS, et al. Exercise & Sports Science Australia (ESSA) position statement on exercise and chronic kidney disease. J Sci Med Sport. 2013;16(5):406–411.
Crossref PubMed
13. Heiwe S, Jacobson SH. Exercise training for adults with chronic kidney disease. Cochrane Database Syst Rev. 2011;(10):CD003236.
PubMed PMC
14. Salahshour VN, Noodeh FA, Ghoobi FB, Sajadi M. Taichi versus stretching exercises to manage fatigue in patients receiving hemodialysis: a randomized clinical trial. J Emerg Nurs Manag. 2023;2(2):1–6.
15. Ramai P, Diana L. Supportive therapy for fatigue in hemodialysis patients. Int J Heal Sci Res. 2021;11(7):367–373.
Crossref
16. Bayülgen MY, Gün M. Effect of complementary and integrative treatments on fatigue symptoms in hemodialysis patients: a systematic review. Holist Nurs Pract. 2022;36(1):17–27.
Crossref
17. Kalani L, Kheirandish V, Shamloo MBB, Zanganeh M, Valiani M, Mojab F, et al. Comparing the effect of geranium aromatherapy and foot reflexology on fatigue and daily activities of patients undergoing hemodialysis: a randomized controlled trial. Trends Med Sci. 2023;2(4):e136136.
Crossref
18. Bayülgen MY, Gün M. The effect of Reiki on fatigue and comfort in hemodialysis patients. Explore. 2023;19(4):553–560.
Crossref
19. Ghanbari A, Shahrbabaki PM, Dehghan M, Mardanparvar H, Abadi EKD, Emami A, et al. Comparison of the effect of reflexology and Swedish massage on restless legs syndrome and sleep quality in patients undergoing hemodialysis: a randomized clinical trial. Int J Ther Massage Bodywork. 2022;15(2):1–13.
PubMed PMC
20. Abu Maloh HIA, Soh KL, Chong SC, Ismail SIF, Soh KG, Abu Maloh DI, et al. The effectiveness of Benson’s relaxation technique on pain and perceived stress among patients undergoing Hemodialysis: a double-blind, cluster-randomized, active control clinical trial. Clin Nurs Res. 2023;32(2): 288–297.
Crossref
21. Komariah A, Rochmawati E. Complementary and integrative interventions for improving fatigue and quality of life in adults receiving hemodialysis: a review. Jurnal Aisyah: Jurnal Ilmu Kesehatan. 2022;7(S2):1–8.
22. Chow SC, Shao J, Wang H, Lokhnygina Y. Sample Size Calculations in Clinical Research. Chapman and Hall/CRC; 2017.
Crossref
23. Artom M, Moss-Morris R, Caskey F, Chilcot J. Fatigue in advanced kidney disease. Kidney Int. 2014;86(3):497–505.
Crossref PubMed
24. Rosti-Otajärvi E, Hämäläinen P, Wiksten A, Hakkarainen T, Ruutiainen J. Validity and reliability of the Fatigue Severity Scale in Finnish multiple sclerosis patients. Brain Behav. 2017;7(7):e00743.
Crossref PubMed PMC
25. Mistik S, Ünalan D, Aslaner H, Tokgöz B. Evaluation of fatigue’s effect and severity in hemodialysis patients. Eurasian J Fam Med. 2022;11(2):136–142.
Crossref
26. Unal KS, Akpinar RB. The effect of foot reflexology and back massage on hemodialysis patients’ fatigue and sleep quality. Complement Ther Clin Pract. 2016;24:139–144.
Crossref PubMed
27. Ahmadidarrehsima S, Mohammadpourhodki R, Ebrahimi H, Keramati M, Dianatinasab M. Effect of foot reflexology and slow stroke back massage on the severity of fatigue in patients undergoing hemodialysis: a semi-experimental study. J Complement Integr Med. 2018;15(4):20170183.
Crossref
28. Cohen J. Statistical Power Analysis for the Behavioral Sciences. Routledge; 2013.
Crossref
29. Goulet-Pelletier JC, Cousineau D. A review of effect sizes and their confidence intervals, Part I: the Cohen’sd family. Quant Method Psychol. 2018;14(4):242–265.
Crossref
30. Sutton RM, McDonald EL, Shakked RJ, Fuchs D, Raikin SM. Determination of minimum clinically important difference (MCID) in visual analog scale (VAS) pain and foot and ankle ability measure (FAAM) scores after hallux valgus surgery. Foot Ankle Int. 2019;40(6):687–693.
Crossref PubMed
31. Rossi MJ, Brand JC, Lubowitz JH. Minimally clinically important difference (MCID) is a low bar. Arthroscopy. 2023;39(2):139–141.
Crossref PubMed
32. Mishra B, Sudheer P, Agarwal A, Srivastava MVP, Vishnu VY. Minimal clinically important difference (MCID) in patient-reported outcome measures for neurological conditions: review of concept and methods. Ann Indian Acad Neurol. 2023;26(4): 334–343.
Crossref PubMed PMC
33. Jørgsholm J, Wejnold Jørgensen R. The minimal clinically important difference of the Southampton Dupuytren’s Scoring Scheme. J Plast Surg Hand Surg. 2023;57(1–6):539–544.
Crossref
34. Malekshahi F, Aryamanesh F, Fallahi S. The effects of massage therapy on sleep quality of patients with end-stage renal disease undergoing hemodialysis. Sleep Hypn. 2018;20:91–95.
35. Tabiee S, Momeni A, Saadatjoo SA. The effects of comfort-based interventions (back massage and patient and family education) on the level of comfort among hemodialysis patients. Modern Care Journal. 2017;14(3):e64687.
Crossref
36. Yaghoubi M, Amini K, Fathi M, Ahamadi FA, Mohammadi ISA, Salehnezhad GH. Effects of massage on pain due to cramp muscle during hemodialysis. J Ilam Uni Med Sci. 2009;17(1):39–46.
37. Lazarus ER, Deva Amirtharaj A, Jacob D, Chandrababu R, Isac C. The effects of an olive-oil massage on hemodialysis patients suffering from fatigue at a hemodialysis unit in southern India–a randomized controlled trial. J Complement Integr Med. 2020;18(2):397–403.
Crossref
38. Padehban V, Mohammadpourhodki R, Bazghale M, Moghadasi A, Sargolzaei M. Comparing palm reflexology and slow-stroke massage on fatigue in hemodialysis patients. Prensa Med Argent. 2018;104(5):3–6.
Crossref
Corresponding author: Arun Vijay Subbarayalu, Department of Physical Therapy, Deanship of Quality and Academic Accreditation, Imam Abdulrahman Bin Faisal University, P.O. Box 1982, Dammam 31441, Saudi Arabia, E-mail: ausubbarayalu@iau.edu.sa, Tel: +966-13-3332503; Mobile: +966- 535071285
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
International Journal of Therapeutic Massage and Bodywork, Volume 18, Number 2, June 2025