Research
The Effectiveness of Traction Massage Combined with Herbal Compress for Relieving Menstrual Cramps: A Randomized Controlled Trial
Aumpol Bunpean, Phd, M. Thai Traditional Medicine, Grad. Thai Traditional Medicine,1* Patama Chantarapon, M. Thai Traditional Medicine, Grad. Thai Traditional Medicine,2 Nianeefa Salaeh, Grad. Thai Traditional Medicine,3 Nurfatin E-tae, Grad. Thai Traditional Medicine4
1Faculty of Public Health and Allied Health Sciences, Praboromarajchanok Institute, Ministry of Public Health, Nonthaburi, Thailand,
2Songkhla Provincial Public Health Office, Songkhla, Thailand,
3Srisakhorn Hospital, Narathiwat, Thailand,
4Kanchanabhishek Institute of Medical and Public Health Technology, Nonthaburi, Thailand
Background and objective
Menstrual cramps are a common gynecological symptom affecting up to 90% of women worldwide. They constitute one of the most prevalent causes of absenteeism from school, work, and social activities. The aim of the study is to assess the effectiveness of traction massage combined with herbal compress on menstrual cramps.
Method
This research used an experimental design using a two-group pretest and posttest approach. A sample of 30 female students with menstrual cramps was randomly assigned to either the massage or control group. The experimental group (n = 15) received traction massage for 10 min, herbal compresses to the lower back, stomach, and anterior muscles of the legs for 15 min, and health-care advice in the week leading up to menstruation. The control group (n = 15) received healthcare advice only.
Results
The intensity of menstrual cramps significantly decreased in the experimental group (p = 0.001). Additionally, the intervention led to a reduction in associated menstrual symptoms such as fatigue, diarrhea, dizziness, headache, irritability, nausea, vomiting, lower back pain, and general fatigue.
Discussion
This study demonstrated that traction massage and herbal compresses significantly reduced the intensity of menstrual cramps in the experimental group. Although we did not measure muscle relaxation or blood flow, the results align with existing literature suggesting that massage therapy can alleviate menstrual discomfort. Additionally, the intervention led to a decrease in associated side effects, enhancing overall well-being during menstruation. Future studies should include physiological measurements to further explore these interventions’ effects. Overall, incorporating traction massage and herbal compresses may improve the management of menstrual cramps effectively.
Conclusion
The combination of traction massage and herbal compresses can serve as an effective option for relieving menstrual cramps and associated side effects when compared to receiving counseling alone.
KEYWORDS: Traction massage; herbal compress; menstrual cramps
INTRODUCTION
Menstrual cramps are a common gynecological symptom experienced by up to 90% of women worldwide(1); it is also known as dysmenorrhea. The symptoms of menstrual cramping or dysmenorrhea include a painful or cramping sensation in the lower abdomen that is frequently accompanied by other biological symptoms like exhaustion, perspiration, headaches, nausea, vomiting, and diarrhea.(2) It is one of the most common causes of absence from school, work, and social activities. It has an impact on women’s daily quality of life.(3)
Menstrual cramps, medically termed dysmenorrhea, are a common occurrence among menstruating individuals and are primarily caused by hormonal imbalances within the body.(4) These imbalances trigger a cascade of physiological responses that lead to the characteristic pain experienced during menstruation. When the menstrual period begins, the body releases prostaglandins, hormone-like substances that stimulate uterine contractions to shed the uterine lining. These contractions help expel menstrual blood from the uterus. However, an excess of prostaglandins can lead to stronger, more painful uterine contractions. These contractions cause the blood vessels in the uterine lining to constrict, reducing blood flow to the uterus. This reduction in blood flow results in a temporary oxygen deficiency in the uterine muscles, triggering pain receptors and leading to cramping sensations.(5,6) Arachidonic acid undergoes two metabolic pathways: the cyclooxygenase and 5-lipoxygenase pathways. Cyclooxygenase produces prostaglandins (PGF2α and PGE2), prostacyclins, and thromboxane, while the 5-lipoxygenase pathway generates leukotrienes.(5) Both prostacyclins and leukotrienes contribute to vasoconstriction, uterine smooth muscle contraction, and ischemia, ultimately lowering the pain threshold.(6) Modern medical treatments for menstrual cramps involve the use of drugs or hormones, and these treatments can come with side effects resulting from the use of synthetic drugs.(7) The most frequently used remedies for relief from menstrual cramps include drinking warm beverages (62%), taking medicine (57%), or sleeping (45%).(8)
Historically, practitioners of Thai traditional medicine have utilized acupressure massage combined with herbal compresses to alleviate menstrual cramps in women. This treatment is typically administered 7 days before menstruation to prevent cramps.(9) However, some patients may experience discomfort during the acupressure massage due to the applied pressure.(10) Thai traction massage offers an alternative to acupressure. This method involves twisting, pulling, and bending various body parts to stretch the muscles, which helps relieve muscle tension and stimulate blood circulation throughout the body.(11) The traction massage technique provides several advantages over acupressure such as minimal discomfort from pressure and a shorter treatment time. Nevertheless, it has limitations, including potential discomfort from stretching. To address these issues, herbal compresses are often used in conjunction with traction massage to relax the muscles and enhance the overall effectiveness of the treatment.(12)
This study aims to explore the benefits of combining the physical manipulation and stretching provided by traction massage and the soothing, anti-inflammatory effects of herbal compresses. This integrated approach not only facilitates immediate muscle relaxation and pain relief but also improves circulation, reduces inflammation, and supports long-term recovery.(13) Previous studies have clearly demonstrated that combining massage with herbal compresses is more effective for muscle pain relief than massage alone.(14) Evaluating these interventions together offers a more holistic treatment approach, reflecting traditional Thai practices where multiple therapies are integrated to maximize therapeutic outcomes. Additionally, this combined approach aligns with traditional Thai medicine practices and may lead to better clinical results in practical settings.(15) However, there is a lack of supporting literature proving its efficacy in reducing menstrual cramps.
MATERIALS AND METHODS
This research used an experimental design using a two-group pretest and posttest approach. Female students were monitored throughout two menstrual cycles. The initial menstrual cycle served as the baseline for menstrual cramps, and before the second menstrual cycle the interventions were administered.
Inclusion Criteria, Recruitment, and Sample
Participants were recruited via the Public Health Center Thai Traditional Medicine Clinic using purposive sampling through posters placed around the clinic. The inclusion criteria for participants were as follows: (i) The sample group consisted of university students from a specific institution, aged between 18 and 25 years old, (ii) those with regular menstrual cycle (a regular 21- to 35-day cycle, with approximately the same number of days in each cycle), (iii) those who had been diagnosed with menstrual cramps by the licensed practitioners of traditional Thai medicine, (iv) those who had pain intensity on a numeric rating scale (NRS, ranging from 0 to 10, with 0 = no pain, 10 = worst pain imaginable) between 4 and 7 (a score of 4 or higher is considered moderate pain and requires pain management, while a score of 7 or higher indicates severe pain and necessitates the use of pain relief medication(16)) on the second day of menstrual cycle as this period typically marks the peak intensity of pain),(17) (v) those who did not receive any alternative treatments for menstrual cramps within 7 days prior to participation, (vi) those who were not pregnant or potentially pregnant, (vii) those who had no contraindications for massage or compression (see Box 1), and (viii) those who provided written informed consent. They were screened by the licensed practitioners of traditional Thai medicine.
Box 1. Contraindications for Massage or Compression
Conditions that are contraindicated for massage include severe asthma attacks, acute bronchitis, status epilepticus, and acute osteomyelitis.
Symptoms that are contraindications for massage include fever exceeding 38.5°C, high blood pressure (160/100 mmHg) with symptoms such as dizziness, palpitations, headaches, or nausea and vomiting.
Pathological conditions in the spine or abdomen that are contraindicated for massage include fractures, dislocations, unstable fractures, and cancers.
Open wounds, chronic wounds, or contagious skin diseases that can be transmitted, injuries within 24 h to the spine or abdomen, and surgeries within 1 month leading to septicemia.
The criteria for withdrawal or termination during the experiment included the inability to attend follow-up assessments or failure to adhere to at least 80% of the research recommendations.
Sample Size
The sample size was calculated using the G*Power program (version 3.1) based on an estimated effect size of 1.25 as determined by a previous study(18) using a significance level of 0.05, and a power of 0.95. A 30-student sample size (15 in each group) was determined for the study, excluding any participants who were later excluded.
Randomization
Participants who met the eligibility criteria were randomized into two groups using block randomization to ensure that both groups have similar levels of pain. This randomization process aims to achieve the closest possible match in average pain scores between the two groups, as determined by statistical principles. Subsequently, the researchers randomly assigned each participant to either the experimental group or the control group. Blinding of participants and the individuals responsible for performing massages was not possible in this study due to the distinctive nature of the two interventions. Consequently, participants and the massage practitioners were aware of which intervention they were receiving or providing.
Interventions
The experimental group (traction massage plus herbal compress plus health-care advice) received a 5-min traction massage per side, incorporating three postures referred to as the “Nang-ann-lew-lom” (2 min; see Figure 1), “Suea-wien-fouw-tum” (2 min; see Figure 2), and traction lower back (1 min; see Figure 3). Following the massage, a herbal compress ball (consisting of phlai 30 g, turmeric 20 g, lemongrass 20 g, kaffir lime skin 10 g, tamarind leaves 30 g, Som poi leaves 10 g, pandan leaves 10 g, salt 10 g, camphor 5 g) was placed in a steamer for 10 min (45–60°C) and then applied to the lower back (2.5 min per side), stomach (2.5 min per side), and anterior muscle of the leg (2.5 min per side) for 15 min. Subsequently, participants received health-care advice on behavioral modifications to alleviate menstrual cramps from a traditional Thai medicine practitioner. This standard advice for all individuals seeking treatment for menstrual cramps included the following: (i) keeping the genitals clean,(19) (ii) using sanitary pads correctly, (iii) getting enough sleep, (iv) refraining from sexual activity during menstruation for cleanliness and hygiene, (v) exercising regularly, and (vi) dealing with stress by managing it appropriately, such as by addressing underlying issues, practicing meditation, and engaging in relaxing activities. All of these activities were performed 7 days before the expected onset of menstruation based on a regular cycle.
|

| |
|
Figure 1 Nang-ann-lew-lom.
Preparatory posture: The patient sits and meditates in an upright posture, interlocks the fingers of both hands, and places them at the nape of the neck. The shoulders are kept out, and elbows spread on both sides. The therapist stands with knees to the patient’s left side and faces toward their left.
Bending and pulling massage pose: The therapist uses the left hand in front of the patient to detour through the back of the patient’s head. Then the therapist inserts the hand into the patient’s right arm, holding it close to the upper arm on the right side. The therapist lifts the left knee in front of the patient and places it on the patient’s thigh near the therapist’s side (left side), without applying weight. Afterward, the therapist pulls the patient’s right arm, bringing it toward the therapist’s side. The patient’s elbow on the right side should approach the floor, tilting toward the patient’s left elbow until both elbows are almost vertically perpendicular to the floor. |
|

| |
|
Figure 2 Suea-wien-fouw-tum.
Preparatory posture: The patient sits and meditates in an upright posture, raising both hands with fingers interlocked at the chest level, palms facing sideways. The elbows and forearms are kept parallel to the floor. The therapist stands with the knees behind the patient, facing their back.
Bending and pulling massage pose: The therapist uses both the hands to hold the patient’s elbows. Instruct the patient to turn their palms outward, then stretch their arms forward until fully extended, keeping them parallel to the floor. Next, raise the arms above the head and exert pressure to bring the patient’s elbows closer together. To maximize the stretch on the side of the torso, the therapist leans slightly backward, pulling the patient’s torso back and holding for a count of 1–10 before slowly releasing. Repeat the bending massage, pulling the other side using the same method. |
|

| |
|
Figure 3 Traction lower back.
Preparatory posture: The patient sits and meditates in an upright posture, interlocking the fingers of both the hands and placing them at the nape of the neck. The shoulders are kept out on both sides with the elbows spread. The therapist kneels on the patient’s back.
Bending and pulling massage pose: The therapist inserts both the hands into the gap of the arm, interlocking it at the nape of the patient’s neck. After that, gently press the patient’s head down and apply a controlled rocking force to the far-left side for 5 s (you may hear cracking sounds from the bones). Repeat the bending massage, pulling the other side using the same method. |
The control group (health-care advice only): This group received health-care advice 7 days before the expected onset of menstruation based on a regular cycle, covering the same six points mentioned above. The health-care advice covered dietary advice as certain foods can worsen menstrual cramping such as high-sugar foods which eaten in excess can promote inflammation, worsening cramps, caffeine which can increase uterine contractions and intensify pain, high trans fat foods which can worsen inflammation and discomfort, salty foods which can lead to bloating and increased discomfort, alcohol which can lead to dehydration and inflammation and can worsen cramps, and processed foods in which the additives and preservatives may increase inflammation. A balanced diet with fresh fruits, vegetables, and lean proteins can help alleviate menstrual discomfort.(20)
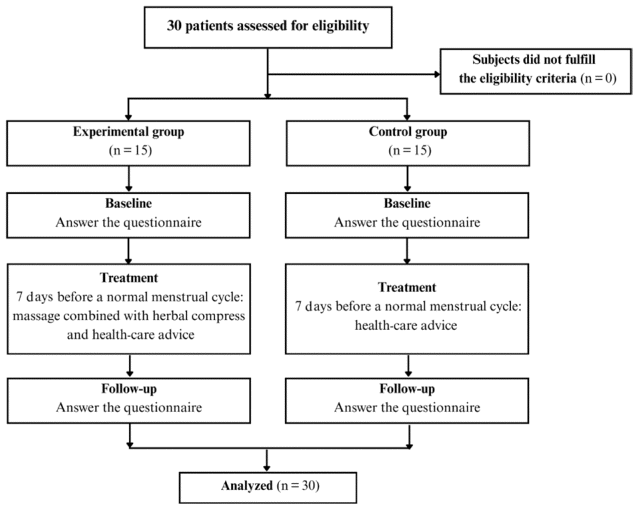
All research participants (both experimental and control groups) will be asked about their adherence to the six recommendations mentioned above. If any participant does not follow the given recommendations, as assessed by their self-report of adhering to all six recommendations at a rate exceeding 80%, they will be excluded from the study (Figure 4).
|
| |
|
Figure 4 Flow chart of participant recruitment, allocation, and follow-up. |
In this study, there was one individual responsible for performing massages. This person underwent short-term training encompassing both theoretical and practical aspects of massage techniques according to the model outlined in this study, provided by the researchers. The individual was trained until each step was accurately executed before proceeding with the massages to collect research data.
Ethical issues
The protocol received approval from the Ethical Committee of the Kanchanabhishek Institute of Medical and Public Health Technology, with the license number KMPHT-65020042. Signed informed consent was obtained from all participants.
Data collection
Participants were asked to complete a sociodemographic questionnaire, including their age, menstrual cramp score, and somatic symptoms.
Outcome measures
The outcome measures used in the study were NRS (reliability 0.99), which was used for assessing menstrual pain, and a questionnaire of menstrual cramps side effects (reliability 0.88), which the researcher adapted from the study by Kamalashiran and Lekskulchai (2012).(21) The tool’s validity was reviewed by three experts in Thai traditional medicine (validity 1.00). The NRS and menstrual cramp questionnaire were administered twice: at baseline which was day 2 of the first menstrual cycle in the study and post-treatment which was day 2 of the second menstrual cycle in the study.
Statistical analysis
Statistical analysis was conducted to determine the characteristics of the participants and to assess the effectiveness of the intervention. Descriptive statistics were used to summarize the demographic information and baseline characteristics of the study sample. To evaluate the difference in outcomes before and after the intervention, an independent t-test was employed. This statistical test compared the mean scores of the outcome variable between the pre-intervention and post-intervention periods. A p-value of less than 0.05 was considered statistically significant. Furthermore, a dependent t-test was utilized to compare the outcomes between the experimental and control groups. This statistical test assessed whether there was a significant difference in the mean scores of the outcome variable within each group before and after the intervention. Again, a significance level of 0.01 was used to determine statistical significance.
RESULTS
Table 1 shows the age, menstrual pain score, and somatic symptom in this study. A third of participants in the experimental group were 21 years old (33.33%). The majority had a menstrual cramp level of 6 on the NRS scale (66.67%). The symptom most commonly present was being easily irritated (90.00%).
Table 1 Demographics and Characteristics
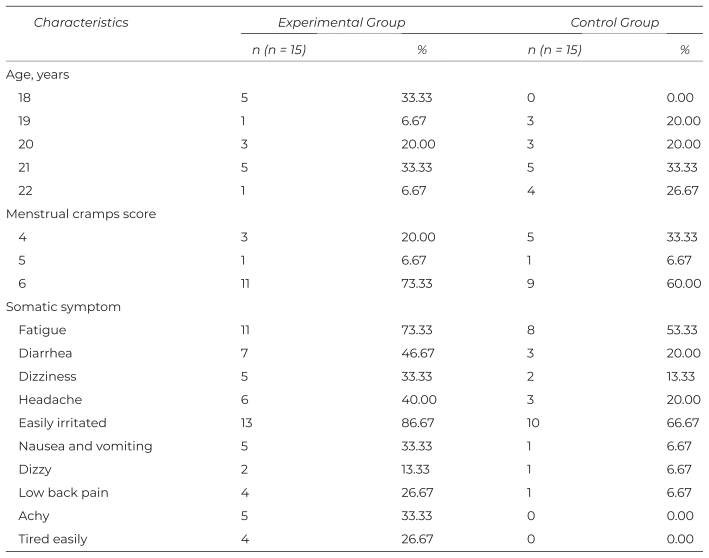
Table 2 shows no significant difference between the experimental and control groups in baseline. The experimental group had a menstrual pain score of 5.53 after receiving traction massage and herbal compresses 7 days before menstruation. The pain score during menstruation was 2.73. When compared using an independent t-test, there was a statistically significant difference at the 0.01 level. As for the control group, their menstrual pain score before the experiment was 5.26, which decreased to 5.06 after the intervention. However, when compared using an independent t-test, no statistically significant difference was found. Furthermore, when comparing the difference between the two groups using a dependent t-test, it was found that there was no significant difference in pain levels before the experiment. However, after the intervention, there was a significant difference at the 0.01 level. This indicates that the intervention effectively reduced menstrual pain compared to the control group.
Table 2 Pain Assessment
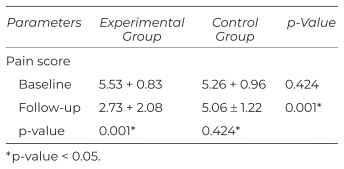
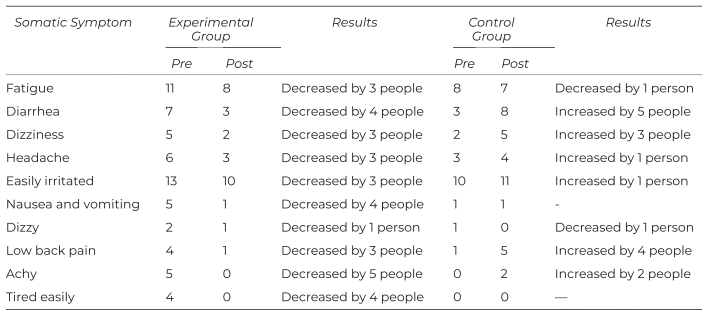
Table 3 shows the side effects from the disease in this study. The experimental group had decreased side effects from the disease such as fatigue, diarrhea, dizziness, headache, getting easily irritated, nausea and vomiting, dizziness, low back pain, and feeling achy and tired easily. The control group had increased side effects from the disease such as fatigue, diarrhea, dizziness, headache, getting easily irritated, low back pain, and feeling achy but with decreased achiness.
Table 3 Somatic Symptom Assessment
DISCUSSION
The study demonstrated that the application of Thai massage therapy in conjunction with herbal compresses led to a statistically significant reduction in menstrual pain compared to the control condition, which involved standard health-care advice only, indicating the potential utility of integrative therapies in the management of dysmenorrhea. The combined application of Thai massage and herbal compresses is a pairing that has not been extensively explored in previous trials. Previous research has investigated the individual and combined effects of massage and herbal compresses on menstrual pain(22) and they found that Thai royal massage applied to the legs, back, and abdomen for 30 min, followed by a 15-min hot compress, significantly reduced menstrual pain compared to pre-treatment levels. While our study findings indicated that the combination of Thai massage therapy and herbal compresses was shown to be more effective in reducing pain than health-care advice, a notable limitation of this study is the inability to isolate the individual contributions of traction massage and herbal compresses to the overall treatment effect. While both modalities have independently shown efficacy in prior studies,(23–26) the precise interaction between the two remains unclear. Some evidence suggests that the combination of massage and hot compresses may produce additive or synergistic effects, although findings have varied depending on the outcomes measured, such as prostaglandin F2α levels. These mixed results underscore the need for future comparative research to delineate the relative and combined efficacy of these modalities.
The effectiveness of herbal compresses is well documented. Research indicates that hot compresses applied at 40–46°C for 20 min, refreshed every 10 min, significantly reduce menstrual pain(27) and herbal compresses have been found to be more effective than hot compresses alone in relieving pain.(28) This timing may influence the preventive or palliative effects of the intervention. The capacity to intervene prior to the onset of menstruation may be important, as reducing pain before the menstrual cycle begins may be more effective than managing symptoms after they have already manifested.(29,30) Additionally, feeling like impending menstrual pain is more manageable might significantly empower women to seek help as research shows that patients who internalize the idea that severe menstrual pain is normal are less likely to seek help.(31–33)
This study contributes to the growing evidence supporting non-pharmacological management strategies for menstrual pain. Increasing the evidence for menstrual pain is important as research on pain phenotypes demonstrates that menstrual pain, specifically primary dysmenorrhea, is a complex experience potentially involving nociceptive and neuropathic components,(34,35) as well as neuroplastic changes in the brain,(36) depending on the underlying cause. Thus, different pain reduction methods are needed to support individuals with different dominant pain phenotype presentations and/or combined pain phenotypes as treatment is not a one-size-fits-all solution. Thai massage combined with herbal compresses may offer a valuable option for individuals seeking alternatives to pharmacological treatments. Continued research in this area is necessary to confirm these findings, determine optimal treatment parameters, and establish long-term efficacy.
Limitations
A potential limitation of this study is the lack of a long-term follow-up period and the absence of blinding for both participants and the individuals responsible for the intervention, which could affect the reliability of the results.
CONCLUSION
This study provides evidence that Thai massage therapy combined with herbal compresses is more effective in reducing menstrual pain than standard healthcare advice alone. The findings support the potential of this integrative, non-pharmacological approach as an option for managing dysmenorrhea. Given the benefit of premenstrual application, which may enhance pain prevention, further research is warranted to explore the underlying mechanisms and to compare the efficacy of individual components within the combined intervention.
ACKNOWLEDGMENTS
Thanks to the participants of the study for generously providing their time and for making themselves physically available so this study could be completed.
CONFLICT OF INTEREST NOTIFICATION
This study was conducted by Aumpol Bunpean as the principal investigator, with Patama Chantarapon, Nianeefa Salaeh, and Nurfatin E-tae serving as co-investigators. The authors declare that there are no conflicts of interest regarding the conduct and publication of this research. The study was carried out independently, without any financial or personal relationships that could inappropriately influence the outcomes.
FUNDING
No sources of funding were used in this study.
REFERENCES
1. Ju H, Jones M, Mishra G. The prevalence and risk factors of dysmenorrhea. Epidemiol Rev. 2014;36:104–113. https://doi.org/10.1093/epirev/mxt009
Crossref
2. Bahrami A, Sadeghnia H, Avan A, Mirmousavi SJ, Moslem A, Eslami S, et al. Neuropsychological function in relation to dysmenorrhea in adolescents. Eur J Obstet Gynecol Reprod Biol. 2017;215:224–229. https://doi.org/10.1016/j.ejogrb.2017.06.030
Crossref PubMed
3. Wal P, Gupta D, Wal A, Pandey SS, Krishnan K. A wholistic approach to non-pharmacological intervention for primary dysmenorrhea. Curr Womens Health Rev. 2024;20(1):21–34. https://doi.org/10.2174/1573404819666230109105829
4. Maybin JA, Critchley HOD. Progesterone: a pivotal hormone at menstruation. Ann N Y Acad Sci. 2021;1221:88–97. https://doi.org/10.1111/j.1749-6632.2011.05953.x
Crossref
5. Rapkin AJ. Pelvic pain and dysmenorrhea. In: Berek JS, ed. Berek & Novak’s Gynecology. 16th ed. Wolters Kluwer Health, Inc.; 2020. 256–283.
6. Guimaraes I. Primary dysmenorrhea: assessment and treatment. Rev Bras Ginecol Obstet. 2020;42(8):501–507. https://doi.org/10.1055/s-0040-1712131
Crossref PubMed PMC
7. Thiantongin P, Pisaipan R, Deelurd K, Inthasoi P. Thai medicinal plants used in the treatment of dysmenorrhea. J Health Res Dev Nakhon Ratchasima Public Health Prov Off. 2021;7(2):5–18.
8. Chia CF, Lai JHY, Cheung PK, Kwong LT, Lau FPM, Leung KH, et al. Dysmenorrhoea among Hong Kong university students: prevalence, impact, and management. Hong Kong Med J. 2013;19(3):222–228. https://doi.org/10.12809/hkmj133807
PubMed
9. Tantipidok Y. Thai Massage Textbook. 5th ed. Bangkok, Thailand: Public Health Foundation and Development; 2020.
10. Moraska AF, Stenerson L, Butryn N, Krutsch JP, Schmiege SJ, Mann JD. Myofascial trigger point-focused head and neck massage for recurrent tension-type headache: a randomized, placebo-controlled clinical trial. Clin J Pain. 2015;31(2):159–168. https://doi.org/10.1097/AJP.0000000000000091
Crossref PMC
11. Public Health and Development Foundation. Thai Massage Therapy Textbook 2 and 3. 2nd ed. Bangkok, Thailand: Moh-Chao-Ban Publishing House; 2018.
12. Usayapunt N, Santamit S. Effects of deep and superficial heating with joint mobilization therapy on range of motion and visual analog scale in patients with frozen shoulder. Region 11 Med J. 2017;31(2):305–315.
13. Somsak N. Guideline for Physical Diagnosis and Treatment by Method of Applied Thai Traditional Medicine. Bangkok, Thailand: D.A. Printing; 2012.
14. Cheteh N, Panoh A. Effectiveness of Thai royal massage therapy combined with herbal compress in office syndrome patients with neck pain, Kapho Hospital, Pattani Province. TUH J Online. 2024;9(1):62–67.
15. Tavee L, Uepong J, Phathanee T. Applied Thai Traditional Medicine and Sustainable Development of Thai Traditional Medicine. Bangkok, Thailand: Supawanish Printing; 2011.
16. Thai Association for the Study of Pain. Guidelines for Developing Acute Pain Relief. Bangkok: Amarin Printing & Publishing; 2009.
17. Harlow SD, Park M. A longitudinal study of risk factors for the occurrence, duration and severity of menstrual cramps in a cohort of college women. Br J Obstet Gynaecol. 1996;103(11):1134–1142. https://doi.org/10.1111/j.1471-0528.1996.tb09597.x
Crossref PubMed
18. Shetty GB, Shetty B, Mooventhan A. Efficacy of acupuncture in the management of primary dysmenorrhea: a randomized controlled trial. J Acupunct Meridian Stud. 2018;11(4):153–158. https://doi.org/10.1016/j.jams.2018.04.001
Crossref PubMed
19. Charoensook J. The role of nurses in solving the problem of menstrual cramps. Nurs Sci J Thail. 2006;24(3):9–20.
20. Airaodion AI, Adejumo PR, Njoku OC, Ogbuagu EO, Ogbuagu U. Implication of sugar intake in haemorrhoid and menstruation. Int J Res Rep Hematol. 2019;2(1):56–64.
21. Kamalashiran C, Lekskulchai O. The comparative study of the efficacy and side effect of Prasaplai extract versus mefenamic acid on relieving primary dysmenorrhea: a clinical phase II trial. Thammasat Med J. 2012;12(4):749–756.
22. Limapanth M, Poontananivattanakul B, Putti N, Mohamad K. The effectiveness of Thai royal massage combined with hot water bag compress in relieving menstrual pain. J Thai Tradit Altern Med. 2016;14(2):8.
23. Wamontree P, Chairat N, Taksin R, Phasinam K. A comparison of the effects of court-type traditional Thai massage and Prasaplai in reducing primary dysmenorrhea. J ReAttach Ther Dev Divers. 2023;6(1s):53–58. https://doi.org/10.52783/jrtdd.v6i1s.215
24. Rejeki S, Pratama FY, Ernawati E, Yanto A, Soesanto E, Pranata S. Abdominal stretching as a therapy for dysmenorrhea. Open Access Maced J Med Sci. 2021;9(G):180–183. https://doi.org/10.3889/oamjms.2021.6711
Crossref
25. Wijaya F, Kushartanti W, Ambardini RL, Delano EH, Manihuruk FF, Murnianah. Effectiveness of manipulative therapy and heat therapy on pain reduction, increased range of motion and motion function in cases of low back pain. Int J Phys Educ Sports Health. 2023;10(3):76–79. https://doi.org/10.22271/kheljournal.2023.v10.i3b.2925
Crossref
26. Veena M, Rajan JK. Dysmenorrhea and perceived stress in the adolescent girls: potential role of relaxation techniques. Int J Obstet Gynaecol Nurs. 2020;4(2):79–84. https://doi.org/10.33545/26642298.2022.v4.i2b.107
27. Fitri D, Isnaini M, Qurniasih N, Wulandari LA, Retno SN. The effect of warm compresses on dysmenorrhea in female students at SMK Darul Fikri Sumanda Tanggamus Regency. Int J Matern Midwifery Sci. 2023;1(1):21–26.
28. Udi SM, Salamah U. Efektivitas pemberian hot herbal compress untuk meredakan dismenore pada remaja putri di SMK Kesehatan Prima Indonesia. J Ilm Kebidanan Imelda. 2023;9(1):60–65. https://doi.org/10.52943/jikebi.v9i1.1200
29. Chaichanadee S, Suthisisang C, Suwannapong N. Effects of herbal compresses on primary dysmenorrhea among Thai university students. J Tradit Complement Med. 2019;9(3):212–217.
30. Tangchai N, Jindadamrongwech S, Suthipinittharm P. The efficacy of Thai massage combined with hot compress for reducing dysmenorrhea: a randomized controlled trial. Complement Ther Med. 2021;58:102686. https://doi.org/10.1016/j.ctim.2021.102686
31. Denny E. “I never know from one day to another how I will feel”: pain and uncertainty in women with endometriosis. Qual Health Res. 2009;19(7):985–995. https://doi.org/10.1177/1049732309338725
Crossref PubMed
32. Wright K. “You have endometriosis”: making menstruation-related pain legitimate in a biomedical world. Health Commun. 2018;34(8):912–915. https://doi.org/10.1080/10410236.2018.1440504
Crossref PubMed
33. Seear K. The etiquette of endometriosis: stigmatisation, menstrual concealment and the diagnostic delay. Soc Sci Med. 2009;69(8):1220–1227. https://doi.org/10.1016/j.socscimed.2009.07.023
Crossref PubMed
34. Coxon L, Wiech K, Vincent K. Is there a neuropathiclike component to endometriosis-associated pain? Results from a large cohort questionnaire study. Front Pain Res (Lausanne). 2021;4(2):743812. https://doi.org/10.3389/fpain.2021.743812
Crossref
35. Oladosu FA, Tu FF, Farhan S, Garrison EF, Steiner ND, Roth GE, et al. Abdominal skeletal muscle activity precedes spontaneous menstrual cramping pain in primary dysmenorrhea. Am J Obstet Gynecol. 2018;219(1):91.e1–91.e7. https://doi.org/10.1016/j.ajog.2018.04.050
Crossref PubMed PMC
36. Tu CH, Niddam DM, Yeh TC, Lirng JF, Cheng CM, Chou CC, et al. Menstrual pain is associated with rapid structural alterations in the brain. Pain. 2013;154(9):1718–1724. https://doi.org/10.1016/j.pain.2013.05.022
Crossref PubMed
Corresponding author: Aumpol Bunpean, Faculty of Public Health and Allied Health Sciences, Praboromarajchanok Institute, Ministry of Public Health, Nonthaburi, Thailand 11000, E-mail: aumpol@kmpht.ac.th
(Return to Top)
COPYRIGHT
Published under the CreativeCommons Attribution-NonCommercial-NoDerivs 3.0 License.
International Journal of Therapeutic Massage and Bodywork, Volume 18, Number 4, December 2025






